Residents in nursing homes have a higher risk of developing infections that require antibiotic treatment than elderly people living at home (1). Antibiotics are also used to prevent infections, for example UTIs and surgical site infections. Antibiotics can cause adverse effects, and elderly people are particularly susceptible to this (2). Increased and incorrect antibiotic use may contribute to the development of antibiotic resistance (3), making it more difficult to prevent and treat infections.
In order to prevent the development of antibiotic resistance, avoid adverse effects and achieve the desired therapeutic effect in the patient, it is essential to avoid unnecessary use of antibiotics as well as to select the right drug at the correct dosage. Recommendations for the use of antibiotics in nursing homes are contained in the National Guidelines for the Use of Antibiotics in Primary Care (4).
Approximately 6 % of prescriptions for antibiotics in Norway are issued in nursing homes (5). There are significant differences in prescribing practice between different nursing homes – with no obvious medical explanation (5). The objective of the Norwegian Ministry of Health and Care Services’ action plan against antibiotic resistance in the health services is to reduce antibiotic use in the health services, including in Norwegian nursing homes, by 30 % by the end of 2020 compared with 2012 (6). It is particularly important to reduce the use of the most resistance-inducing drugs, especially quinolones and macrolides.
UTI is one of the most frequently recorded types of infection among nursing home residents (7). Several studies indicate significant overdiagnosis and overtreatment of UTIs in nursing homes, including through treatment of asymptomatic bacteriuria (8, 9). Many different drugs are also used to prevent recurrent UTIs, including both antibiotics and other substances/drugs (10, 11). Where renal function is normal, methenamine may prevent UTI, at least when used as a short-term prophylaxis (11). Methenamine appears only to be effective in acidic urine and is considered ineffective in patients with a permanent catheter (4, 11).
UTI is often caused by E. coli (12, 13). Results from the Norwegian Surveillance System for Antimicrobial Drug Resistance showed that 34 % of E. coli strains in urine samples were resistant to ampicillin, 23 % were resistant to trimethoprim, 21 % to trimethoprim-sulfamethoxazole, 7 % to ciprofloxacin, 5 % to mecillinam and 1 % to nitrofurantoin in 2015 (3).
Since May 2015 it has been mandatory for nursing homes in Norway to participate in two point prevalence surveys per year. These surveys record the prevalence of healthcare-associated infections and use of systemic antibiotics. Healthcare-associated infections are infections that are associated with periods spent or treatment in healthcare institutions, in addition to surgical site infections.
The purpose of the survey was to describe the prevalence of healthcare-associated UTIs and use of antibiotics for this indication in Norwegian nursing homes in the spring of 2016, as well as to assess whether the use of antibiotics was in accordance with the National Guidelines for the Use of Antibiotics in Primary Care (4).
Material and method
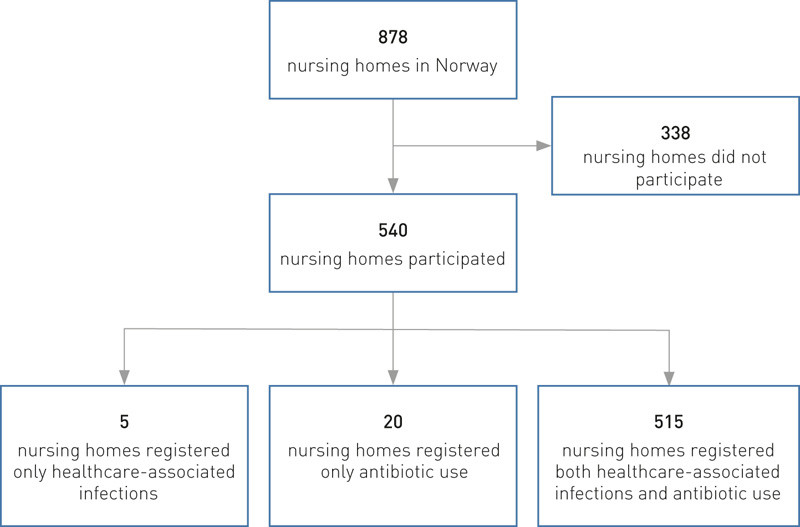
In the spring of 2015, the Norwegian Institute of Public Health requested all municipalities in Norway to report which nursing homes were located within their boundaries. As of July 2015, a total of 878 nursing homes were registered, of which 540 took part in the point prevalence survey in the spring of 2016, conducted in week 19 (9 – 13 May), on a day when the nursing home doctor was in attendance. None of the nursing homes applied for exemption. The Institute of Public Health sent a reminder prior to the survey, and the county medical officers subsequently received a list of the nursing homes that had participated in their county.
The point prevalence survey consisted of two parts, one that recorded healthcare-associated infections, and one that recorded all systemic use of antibiotics. A complete description of the survey can be found in Prevalensundersøkelser av helsetjenesteassosierte infeksjoner og antibiotikabruk i helseinstitusjoner – registreringsmal for sykehjem [Point prevalence surveys of healthcare-associated infections and antibiotic use in healthcare institutions – user guide for nursing homes] (14).
In the section of the survey dealing with infections, the following three types of healthcare-associated infections were registered in accordance with the McGeer criteria (15): symptomatic UTI (in residents with or without a urinary catheter), lower respiratory tract infection and skin infection. In addition, surgical site infection was registered according to the case definition from the European Centre for Disease Prevention and Control (16). Number of residents with healthcare-associated infections and number of residents with a urinary catheter were also registered.
In the section of the survey dealing with antibiotics, all systemic use (not solely use connected with the four types of healthcare-associated infections) was registered. Antibiotics are defined here as antibacterial drugs (including methenamine) and antimycotics, as well as vancomycin, fidaxomicin, metronidazole and rifampicin. The number of residents who were given one or more of these drugs was registered, and for each prescription the product name, dosage, route of administration and indication were recorded.
A total of 24 indications (cf. the user guide) were used, including asymptomatic bacteriuria and lower and upper UTI, but no criteria for the indications were specified. Also registered was whether antibiotics were prescribed for a healthcare-associated or a community-acquired infection, or as prophylaxis. Where methenamine was recorded as being prescribed for treatment (n = 62), this was considered an incorrect registration and included under prophylactic prescribing. In the case of prescription for treatment, we recorded whether a microbiological sample had been taken. Age and gender were only registered for residents who received antibiotics.
The total number of residents on the day of the survey was used to calculate prevalence of healthcare-associated infections and antibiotic use. Point prevalence surveys fall within the regulations concerning the Norwegian Surveillance System for Antibiotic Use and Healthcare-associated Infections. Health information was retrieved in accordance with the regulations. No other approvals were necessary.
The diagrams and estimates were made with the aid of Excel 2013 MSO (Microsoft Corp., Washington, USA).
Results
Participation
Altogether 61 % of Norwegian nursing homes participated in the point prevalence survey in the spring of 2016 (Figure 1). For antibiotic use, 23 752 residents were registered, and 23 503 residents for the survey of healthcare-associated infections. These were distributed among the following department types: 54 % in long-term care departments, 17 % in dementia care units, 17 % in combined short-term and long-term departments, 9 % in short-term departments and 3 % in rehabilitation units.
Healthcare-associated infections
The survey showed that 5.2 % of the residents had one or more healthcare-associated infections. A total of 1 304 of these were registered, of which UTIs accounted for 49 %, lower respiratory tract infection 26 %, skin infections 18 % and postoperative surgical site infections 7 %.
The proportion of nursing home residents who had a UTI was 2.7 %. A total of 1 922 of the residents surveyed (8.2 %) had a urinary catheter. Among the residents with a catheter, the proportion with an infection was 8.2 %, while among those with no catheter it was 2.2 %.
Use of systemic antibiotics
The survey showed that 7.2 % of the residents were given antibiotics on the day of the survey. For 210 of these, no detailed information about the prescriptions was available. Drug and indication was recorded for 1 544 prescriptions. Of these, 63 % had UTI as the indication (including asymptomatic bacteriuria, lower and upper UTI), 18 % lower respiratory tract infection, and 8 % had skin and soft tissue infection as the indication. The remaining prescriptions were distributed among other indications.
Use of systemic antibiotics for urinary tract infections
A total of 966 prescriptions had UTI as the indication – of which 40 % related to treatment and 44 % to prophylaxis. In 16 % of the cases, the classification was «other» or «unknown» (Table 1).
Table 1
Number of prescriptions of systemic antibiotics for prevention and treatment of UTIs, distributed by indications, among 535 nursing homes that participated in the Institute of Public Health’s survey in the spring of 2016
| Indication |
Prevention |
Treatment |
Other/unknown classification1 |
Total |
| Lower UTI |
374 |
336 |
118 |
828 |
| Upper UTI |
31 |
43 |
8 |
82 |
| Asymptomatic bacteriuria |
22 |
5 |
29 |
56 |
| Total |
427 |
384 |
155 |
966 |
| [i] | ||||
[i] 1 Classification of whether antibiotics are given for prevention or treatment
Altogether 80 % of the prescriptions were for residents who were 80 years of age or older, 14 % were issued for residents in the age group 70 – 79 years and in 6 % of the cases the prescriptions were for younger age groups or age was not stated. In total 97 % of the antibiotics prescribed for the treatment of UTIs and all antibiotics prescribed for prevention of UTIs were administered perorally.
Treatment of urinary tract infections
Of the prescriptions with lower UTI as the indication, 224 were for women (67 %) and 111 for men (33 %). In the case of one prescription gender was not stated.
Pivmecillinam, trimethoprim and nitrofurantoin (first-line drugs in the national guidelines) accounted for a total of 65 % of the prescriptions with lower UTI as the indication (Table 2). Dosage of first-line drugs was predominantly in accordance with the national recommendations (Table 2), while amoxicillin and ciprofloxacin were administered as a double dosage in 64 % and 73 % of prescriptions, respectively.
Table 2
Prescribing of systemic antibiotics (active pharmaceutical ingredient) for treatment of lower UTIs among 535 nursing homes that participated in the Institute of Public Health’s survey in the spring of 2016, and compliance with the National Guidelines for the Use of Antibiotics in Primary Care (4)
| Prescribed drug |
Recommendation in the guidelines |
Proportion (%) of prescriptions administered in dosages according to the guidelines |
Proportion (%) of prescriptions where a microbiological sample was taken |
| Pivmecillinam n = 1341 Trimethoprim n = 53 Nitrofurantoin n = 30 |
First-line drugs: Pivmecillinam 200 mg × 3 Trimethoprim 160 mg × 2 Nitrofurantoin 50 mg × 3 |
53 77 57 |
57 60 60 |
| Amoxicillin n = 22 Cephalexin n = 2 Ciprofloxacin n = 22 Ofloxacin n = 1 |
After urine culture results available 2 Amoxicillin 250 mg × 3 Cephalexin 250 mg × 3 Ciprofloxacin 250 mg × 2 Ofloxacin 200 mg × 2 |
5 0 9 0 |
59 0 55 0 |
| Trimethoprim-sulfamethoxazole n = 47 Other antibiotics3 n = 25 |
Not specified Not specified |
– – |
49 32 |
| [i] | |||
[i] 1 Mecillinam is not shown together with pivmecillinam which should be administered orally, because mecillinam should be administered intravenously and has a higher recommended dose
2 See National Guidelines for the Use of Antibiotics in Primary Care for further specifications for use
3 With the exception of cephalexin and ofloxacin, antibiotics with fewer than ten prescriptions are included in «Other antibiotics»: phenoxymethylpenicillin, doxycycline, cefotaxime, cefuroxime, mecillinam, dicloxacillin, benzylpenicillin, azithromycin and metronidazole
Of the prescriptions for men, trimethoprim-sulfamethoxazole accounted for 25 %, ciprofloxacin 10 % and amoxicillin 9 % (n = 111), while these three drugs comprised 8 %, 4 % and 5 % of the prescriptions for women, respectively (n = 224). In the case of one prescription for ciprofloxacin, gender was not stated. Microbiological samples were collected with approximately equal frequency when prescribing trimethoprim-sulfamethoxazole, amoxicillin and ciprofloxacin as when prescribing first-line drugs, i.e. around half of the prescriptions (Table 2).
Treatment of upper urinary tract infections
Of the prescriptions where upper UTI was indicated, a total of 20 (47 %) were for women.
Pivmecillinam, trimethoprim-sulfamethoxazole and ciprofloxacin (which together with ofloxacin represent first-line drugs in the national guidelines) in total accounted for 58 % of the prescriptions with upper UTI as the indication (Table 3). Ofloxacin was not prescribed.
Table 3
Prescribing of systemic antibiotics (active pharmaceutical ingredient) for treatment of upper UTIs among 535 nursing homes that participated in the Institute of Public Health’s survey in the spring of 2016, and compliance with the National Guidelines for the Use of Antibiotics in Primary Care (4)
| Prescribed drug |
Recommendation in the guidelines |
Proportion (%) of prescriptions administered in dosages according to the guidelines |
Proportion (%) of prescriptions where a microbiological sample was taken |
| Pivmecillinam n = 13 Trimethoprim-sulfamethoxazole n = 5 Ciprofloxacin n = 7 Ofloxacin n = 0 |
First-line drugs : Pivmecillinam 400 mg × 3 Trimethoprim-sulfamethoxazole 160 + 800 mg × 2 Ciprofloxacin 500 mg × 2 Ofloxacin 400 mg × 2 |
69 40 100 – |
46 20 71 – |
| Trimethoprim n = 5 Amoxicillin n = 5 Other antibiotics1 n = 8 |
Not specified Not specified Not specified |
– – – |
20 40 63 |
| [i] | |||
[i] 1 Antibiotics with fewer than five prescriptions are included in «Other antibiotics»: cefotaxime, cefuroxime, phenoxymethylpenicillin and nitrofurantoin
Prevention of urinary tract infection
Of the prophylactic prescriptions, a total of 336 (79 %) were for women.
Methenamine accounted for 87 %, trimethoprim 7 %, nitrofurantoin 5 % and other antibiotics 1 % of the prescriptions for prevention of UTIs.
Discussion
The prevalence of UTIs in Norwegian nursing homes was high compared to the prevalence in nursing homes elsewhere in Europe, where overall prevalence was 1.1 % (varying from 0 % to 3.7 % between countries) (7). Number of residents, their age, degree of incontinence and catheter use varied among the countries in the European survey, such that the prevalence was not necessarily comparable (7).
In accordance with previous findings (17) the point prevalence survey in the spring showed that UTI was the most frequently occurring type of healthcare-associated infection in Norwegian nursing homes. The prevalence was higher in residents with urinary catheters than in those without catheters. In order to prevent UTIs and thereby also reduce the use of antibiotics in nursing homes, the national guidelines for the prevention of catheter-associated UTIs should be adhered to (18).
The prevalence of antibiotic use in the survey in the spring was high compared to the prevalence in nursing homes elsewhere in Europe, where overall prevalence was 4.4 % (varying from 2 % to 11 % between countries) (7). The proportion of prophylactic prescriptions for UTIs was considerably higher in Norwegian nursing homes than in nursing homes in most other European countries (7). Methenamine was the drug most commonly prescribed as a prophylactic in Norwegian nursing homes. Although methenamine is not considered to be resistance-inducing and has few adverse effects, unnecessary use of drugs should be avoided due to patient-related and economic costs.
Antibiotics that were recommended as first-line drugs in the national guidelines represented approximately 60 % of the prescriptions for treatment of both lower and upper UTIs. For both indications, pivmecillinam constituted a significantly larger proportion of the prescriptions than the other first-line drugs, even though these are ranked equally in the guidelines. Trimethoprim and trimethoprim-sulfamethoxazole were prescribed with approximately the same frequency for lower and upper UTIs, although trimethoprim is a first-line drug for lower UTIs and trimethoprim-sulfamethoxazole is a first-line drug for upper UTIs.
The guidelines recommend the same antibiotics for women and men. However, trimethoprim-sulfamethoxazole, ciprofloxacin and amoxicillin were prescribed more frequently for men than for women with lower UTIs. In a study from Vestfold county, significant gender differences were found in nursing homes with regard to urinary tract pathogens and patterns of resistance (12), which raises questions as to whether the guidelines should be changed with respect to first-line drugs.
Dosages of amoxicillin and ciprofloxacin prescribed for treatment of lower UTIs conformed to a large extent with the guidelines regarding upper UTI. The higher dosage of amoxicillin, together with the fact that this was the most frequently prescribed drug for the treatment of lower respiratory tract infections, gives reason to believe that this drug was prescribed in cases where it was difficult to know whether the resident had a UTI, a lower respiratory tract infection or both.
Although ciprofloxacin is a first-line drug for treatment of upper UTIs, the guidelines specify that for treatment of lower UTI, ciprofloxacin and amoxicillin should only be used after the urine culture results are available. However, the proportion of prescriptions for lower UTIs where a microbiological sample was taken was no higher when prescribing these drugs than when prescribing first-line drugs. The survey only provides answers to whether a microbiological sample has been taken, not whether the treatment is based on test results. Nor does it provide answers to whether there was a clinical suspicion of infection when the sample was taken, as there should be according to the guidelines. Given that 15 – 50 % of nursing home residents have asymptomatic bacteriuria, a positive sample result is not necessarily tantamount to a UTI (19).
The fact that choice of drug, dosage and microbiological testing in the treatment of lower UTIs did not always conform to the guidelines, may indicate non-compliance, but may also be attributable to incorrect recording of the indication. We do not know the criteria on which the doctors have based their choice of indication and cannot therefore draw any conclusions on wrong diagnosis and overtreatment of UTIs in Norwegian nursing homes.
The low participation in the point prevalence survey in the spring may be due to the fact that the Norwegian Institute of Public Health’s reminders failed to reach all nursing homes, or that there is a relatively high turnover of personnel in many nursing homes. We do not know the degree to which the participating nursing homes constituted a representative sample.
Point prevalence surveys only provide a snapshot. Consequently, it is more probable that long-term rather than short-term infections and antibiotic use are included. Nevertheless, the findings in the spring survey are supported by findings in the previous point prevalence survey of healthcare-associated infections and antibiotic use in nursing homes (20).
Despite the widespread use of methenamine, UTIs are a relatively frequent occurrence in Norwegian nursing homes. Norwegian nursing home doctors should therefore consider whether their use of this drug is in accordance with national and international recommendations (4, 11). The survey indicates that compliance with the national guidelines for treatment of lower UTIs could be improved with regard to choice of drug, dosage and microbiological testing.
MAIN MESSAGE
Urinary tract infections (UTIs) were the most commonly occurring type of infection in Norwegian nursing homes.
First-line antibiotics accounted for approximately 60 % of the prescriptions for treatment of UTIs
Compliance with the national guidelines could be improved with regard to the treatment of lower UTIs
Use of methenamine for the prevention of UTIs was widespread in Norwegian nursing homes
- 3.
NORM/NORM-VET-årsrapport. 2015. Usage of Antimicrobial Agents and Occurrence of Antimicrobial Resistance in Norway. Oslo/Tromsø: Norsk overvåkningssystem for antibiotikaresistens hos mikrober (NORM), Veterinærinstituttet, Folkehelseinstituttet, 2016. https://unn.no/Documents/Kompetansetjenester,%20-sentre%20og%20fagr%C3%A5d/NORM%20-%20Norsk%20overv%C3%A5kingssystem%20for%20antibiotikaresistens%20hos%20mikrober/Rapporter/NORM_NORM-VET-2015.pdf (1.2.2017).
- 4.
Nasjonale faglige retningslinjer for antibiotikabruk i primærhelsetjenesten. IS-2030.Oslo: Helsedirektoratet, 2012.
- 6.
Handlingsplan mot antibiotikaresistens i helsetjenesten. I-1171 B. Oslo: Helse- og omsorgsdepartementet, 2015.
- 7.
Point prevalence survey of healthcare-associated infections and antimicrobial use in European long-term care facilities, April-May 2013. Stockholm: European Centre for Disease Prevention and Control, 2014.
- 11.
Lee BS, Bhuta T, Simpson JM et al. Methenamine hippurate for preventing urinary tract infections. Cochrane Database Syst Rev 2012; 10: CD003265. [PubMed]
- 14.
Prevalensundersøkelser av helsetjenesteassosierte infeksjoner og antibiotikabruk i helseinstitusjoner – registreringsmal for sykehjem. Folkehelseinstituttet, 2015. https://www.fhi.no/hn/helseregistre-og-registre/nois/sykehjem-nois-piah/(15.12.2016).
- 16.
Surveillance of surgical site infections in European hospitals – HAISSI protocol, version 1.02. Stockholm: European Centre for Disease Prevention and Control, 2012.
- 18.
Fagernes M, Sorknes N, Lingaas E. Forebygging av kateterassosierte urinveisinfeksjoner – nasjonal veileder. Oslo: Folkehelseinstituttet, 2013.
- 20.
Prevalens av helsetjenesteassosierte infeksjoner og antibiotikabruk i sykehjem – høsten 2015. Oslo: Folkehelseinstituttet, 2016. https://www.fhi.no/hn/helseregistre-og-registre/nois/sykehjem-nois-piah/ (16.12.2016).