Norwegian patients with colon cancer start their adjuvant therapy too late
National recommendations for treatment of colorectal cancer have existed in Norway since the early 1990s. According to these national guidelines, patients with colon cancer with a high risk of relapse must receive adjuvant chemotherapy (1). Such treatment is normally provided over a period of six months to patients under 75 years, and the guidelines stipulate that it should start within 4 – 6 weeks (28 – 42 days) after surgery.
The optimal time for initiation of adjuvant chemotherapy after surgery for colon cancer has not been established by randomised clinical trials. There is nevertheless an international clinical consensus that treatment ought to start within 4 – 8 weeks after surgery, and that providing this treatment after three months is not appropriate, since the objective is to eliminate any circulating malignant cells (2). Even though the national guidelines in this area have a low level of evidence (Level D), this is no reason for every hospital trust to follow its own practice. If so, this should be justified in every individual case. A meta-analysis from 2011 indicates that relative survival is reduced by 14 % for each week adjuvant therapy is delayed (3). An analysis from the Danish colorectal cancer registry shows a reduction in the total survival rate if the chemotherapy is initiated more than 55 days after surgery (4).
We wished to investigate whether the national guidelines with regard to the time of initiation of adjuvant therapy were followed up in Norwegian hospital trusts, and to see whether the type of surgery was related to any differences in the time that elapsed before initiation of adjuvant therapy.
Material and method
This study is part of the research project «Analyses of patient pathways», which has obtained a licence from the Norwegian Data Protection Authority and has been exempted from the duty of confidentiality by the Regional Committee for Medical and Health Research Ethics. The licence grants access to personally identifiable data from the Norwegian Patient Register, which has provided information on patients treated in Norwegian hospitals in the period 2008 – 2013.
Encrypted patient serial numbers permit descriptions of patient pathways that involve multiple hospitals over several years. In addition to selected patient information, such as place of residence and gender, the licence grants access to certain administrative and medical data, including institutions, treatment level and diagnosis codes (ICD-10), as well as procedural codes (Norwegian classification of medical procedures (NCMP) and the Nordic classification of surgical procedures (NCSP)).
Study population
The sample for our study includes patients who have undergone surgery for colon cancer in the period 2008 – 2013, defined through the diagnosis code for colon cancer (C18) and codes for surgical procedures that indicate removal of parts or the whole of the large intestine.
Open surgery is defined by the procedural codes JFB20, JFB30, JFB33, JFB40, JFB43, JFB46, JFB50, JFB60, JFB63, JFB96, JFH00, JFH10 and JFH96. Laparoscopic surgery is defined by the procedural codes JFB21, JFB31, JFB34, JFB41, JFB44, JFB47, JFB51, JFB61, JFB64, JFB97, JFH01 and JFH11.
The date of admission to hospital for surgery plus two days was set as the date of the surgery, since we did not have access to the actual date of the intervention.
Patients who had undergone relevant surgery to the colon and during the same hospitalisation period had been diagnosed with «carcinoma in situ» (D01) or «neoplasms of uncertain or unknown behaviour» (D37) were included if a cancer diagnosis (C18) was established within 120 days of the estimated date of surgery, or if a follow-up examination for a malignant neoplasm (Z08) was undertaken within 200 days (12 356 patients).
Patients who had undergone surgery for colon cancer and were not coded for secondary neoplasms (C77.0, C77.1, C77.3, C78* or C79*) within 90 days after the estimated date of surgery were assumed to have a limited illness requiring therapy with a curative intention, and thus to be available for adjuvant therapy (10 377 patients).
To ensure a sufficiently long follow-up period to be able to assess whether chemotherapy had been administered for six months after the primary surgical treatment, we included only patients with an estimated date of surgery earlier than ten months before the end of the data set (i.e. admission date before 1 March 2013) in our patient sample. Patients older than 75 years are normally not considered for adjuvant therapy for colon cancer and were excluded (Figure 1). Patients who were not coded with C18 as a diagnosis in the period while the adjuvant chemotherapy was provided or had codes for secondary neoplasms (main or secondary diagnoses) for this period, or did not receive adjuvant therapy, were also excluded. A total of 9 245 patients were excluded.
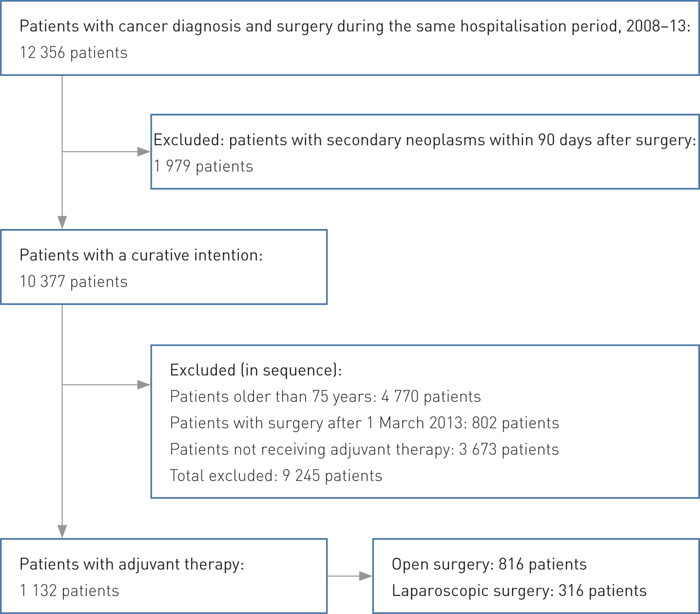
Chemotherapy was identified by the diagnosis code Z51.1*, reimbursement code H05a and/or the procedural codes WBOC05, WBOC08 and WBOC20. Patients were defined as recipients of adjuvant chemotherapy if this had been initiated within 90 days after the estimated date of surgery and one of two treatment patterns were discovered (1 132 patients):
Up to 12 treatments received over a period of 210 days, with a minimum interval of two weeks between each treatment (5-fluorouracil and calcium folinate combined with oxaliplatin).
Up to eight treatments received over a period of 210 days, starting every three weeks (capecitabine/oxaliplatin)
Patients who had suffered complications or had undergone reoperations were identified with a diagnosis code for complications (T81.0 – 81.9, T88.8, Y83.2) or a procedure code for reoperation (JW*) during the same hospitalisation period as the primary surgery or within 30 days after the estimated date of the surgical procedure. A total of 158 patients were identified as having suffered complications.
Statistical method
The analyses were undertaken in the statistics software application SAS (SAS Institute, Cary, N.C.). These analyses include the entire population, not merely a sample, and no p-values are therefore reported for differences between groups and categories. Regression analysis was used to analyse the associations between the number of days elapsing between surgery and the initiation of adjuvant therapy, hospitalisation period and age.
Results
Altogether 1 132 patients (Figure 1) received adjuvant chemotherapy, 52 % of whom were women. The average age was 62.7 years, with only a minor difference in average age between men and women. Nor were there any major differences in the average age of persons who had undergone open surgery and laparoscopic surgery respectively. Altogether 14 % of the patients had sustained complications or undergone reoperations. There were only minor differences between men and women with regard to the proportion of complications. The proportion of complications among those who had undergone open surgery was more than double compared to patients who had undergone laparoscopic surgery (Table 1). The average hospitalisation period amounted to 9.5 days, and was relatively similar for men and women. Patients whose surgery had been undertaken with the open technique had significantly longer hospitalisation periods than patients who had been operated on with the laparoscopic technique (Table 1).
Table 1
Patients who have received adjuvant chemotherapy for colon cancer. Number of patients, age, proportion with complications, hospitalisation periods and time before initiation of adjuvant therapy by type of surgery and gender, Norway 2008 – 2013. Number (%), average (SD) or proportion (number)
| Total |
Men |
Women |
||||
| Number (%) |
1 132 |
(100 %) |
541 |
(48 %) |
591 |
(52 %) |
| Laparoscopy |
316 |
(28 %) |
156 |
(14 %) |
160 |
(14 %) |
| Open surgery |
816 |
(72 %) |
385 |
(34 %) |
431 |
(38 %) |
| Age (years), average (SD) |
62.7 |
(9.5) |
62.5 |
(9.4) |
62.9 |
(9.6) |
| Laparoscopy |
61.8 |
(9.9) |
62.1 |
(9.5) |
61.6 |
(10.3) |
| Open surgery |
63.0 |
(9.3) |
62.7 |
(9.4) |
63.3 |
(9.3) |
| Complications, percentage (number) |
14.0 |
(158) |
14.6 |
(79) |
13.4 |
(79) |
| Laparoscopy |
7.6 |
(24) |
9.6 |
(15) |
5.6 |
(9) |
| Open surgery |
16.4 |
(134) |
16.6 |
(64) |
16.2 |
(70) |
| Hospitalisation period (days), average (SD) |
9.5 |
(6.8) |
9.6 |
(7.2) |
9.4 |
(6.5) |
| Laparoscopy |
6.5 |
(4.2) |
6.6 |
(5.3) |
6.5 |
(2.9) |
| Open surgery |
10.7 |
(7.3) |
10.8 |
(7.5) |
10.6 |
(7.0) |
| Days until adjuvant therapy, average (SD) |
44.7 |
(11.9) |
44.7 |
(11.4) |
44.7 |
(12.3) |
| Laparoscopy |
44.1 |
(11.0) |
45.2 |
(10.5) |
43.1 |
(11.5) |
| Open surgery |
44.9 |
(12.2) |
44.5 |
(11.8) |
45.3 |
(12.6) |
There were no significant differences between the hospital trusts with regard to the patients» age at the time of surgery, hospitalisation period and complications, but there were differences between the hospital trusts in terms of the time that elapsed before the initiation of adjuvant chemotherapy (Figure 2).
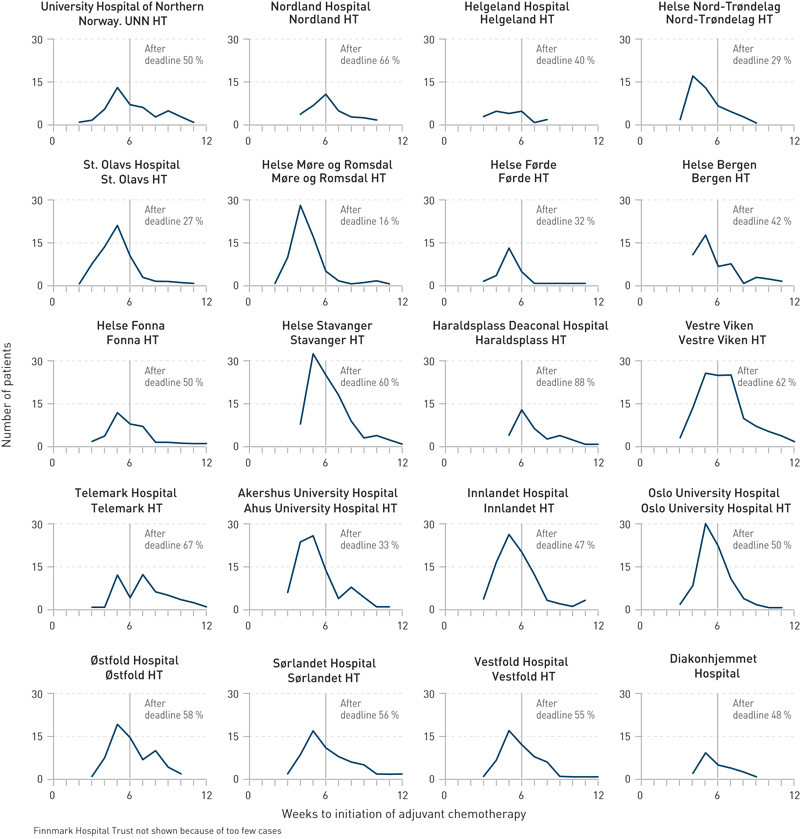
On average, 44.7 days (median 42 days) elapsed between the surgical procedure and the start of adjuvant therapy. Altogether 49 % of the patients failed to start their adjuvant therapy before the final deadline stipulated in the national guidelines (42 days), and 14.5 % of the patients started their adjuvant therapy later than 55 days after surgery.
Patients who had undergone laparoscopic surgery started their adjuvant therapy 0.8 days earlier than patients who had undergone open surgery (44.1 days and 44.9 days respectively). Patients with complications/reoperations started their adjuvant chemotherapy 5.0 days later on average than patients who had had no complications/reoperations during their treatment sequence (49.0 days and 44.0 days respectively).
There was a positive association between the time elapsing between the surgical procedure and initiation of adjuvant chemotherapy on the one hand and hospitalisation period and age on the other. One extra hospitalisation day caused the initiation of the adjuvant therapy to be delayed by half a day. The same result was found for all patients, irrespective of whether they had undergone open or laparoscopic surgery. Older patients started their adjuvant therapy later than others. On average, the time elapsing before initiation of adjuvant therapy increased by 0.13 days for every additional year of age. Even this finding was irrespective of the type of surgery. The age-adjusted time elapsing before the initiation of adjuvant therapy amounted to 44.2 days and 44.9 days for patients who had undergone laparoscopic and open surgery respectively. In other words, adjustment for age has only a marginal effect.
Discussion
In Norway, it is recommended that adjuvant chemotherapy be started within 28 – 42 days after the surgical procedure. This study shows that on average, 44.7 days (median value 42 days) elapse from the estimated date of surgery to the initiation of adjuvant therapy. The deadline imposed by the guidelines was exceeded for 49 % of the patients. Thus, the therapy is significantly delayed not only in a few cases; there were many who got off to a late start.
Patients who have been operated on with the laparoscopic technique have shorter hospitalisation periods and fewer complications, but nevertheless fail to start their adjuvant chemotherapy significantly sooner than patients who have been operated on with open-surgery methods.
Factors that delay the initiation of chemotherapy include post-operative complications or other illness, for which the patient first needs to be examined or treated. However, this factor alone cannot explain why one-half of the patients start their treatment after the expiry of the deadline or that patients with short hospitalisation periods and no post-operative complications are late in starting their therapy. Most likely, this delay can be explained by an absence of appropriate patient pathways and referral routines. The quality registry for colorectal cancer includes quality indicators that emphasise surgical techniques (5). Future measures to improve quality should also include the oncological therapy.
The Danish colorectal cancer group has reported that on average, 43 days passed before the initiation of adjuvant therapy for patients with no anastomotic leak and 59 days for patients with an anastomotic leak (4). The corresponding time periods in Norway amounted to 44 days for patients with no complications and/or reoperations and 49 days for patients with one or both of these factors. The Danish study showed an elevated mortality in those who started their adjuvant therapy after 55 days (4). In our study, 14.5 % of the patients start their adjuvant therapy this late.
In this context, it is interesting to note that relative survival up to five years from the date of diagnosis has remained largely unchanged from the period 2008 – 10 to the period 2011 – 13 (5).
It is important to maintain records and quality assurance of the oncological treatment in the quality registry in the same way as it is undertaken with regard to the surgical intervention. The increased attention generated by the «package processes» for cancer therapy will hopefully have an effect on the total patient pathway, not only until the initiation of treatment. Better knowledge on patient pathways, combined with data from the quality registry, will establish better preconditions for quality-enhancing measures for this group of patients. The weaknesses in the patient pathways needs to be identified and corrective steps taken. This should be implemented in a continuous process.
Methodological considerations
The quality of the coding of colorectal cancer in the Norwegian Patient Register has previously been shown to be satisfactory (6). Experience indicates, however, that the coding of complications is not optimal. Conclusions ought to be drawn with some caution. The Norwegian Colorectal Cancer Registry contains no information on complications in 3 % of all cases (5).
Complications are reported to the quality registry only from the primary hospitalisation, while this study includes all complications occurring within 30 days. Despite a somewhat different definition, there is good correspondence between the proportion of complications reported by the Norwegian Patient Register and the Norwegian Colorectal Cancer Registry (14 % and 17 %). Identification of reoperations by the procedure code JW* does not provide a complete overview, since this code is not invariably used for reoperations. However, it is still regarded as the best identification method. Alternative solutions entail a risk of including procedures that are not reoperations.
Patients with a high risk of complications and reoperations, for example those who suffer from obesity and acute abdominal conditions, will be selected for open surgery by many surgeons. This may explain why this study finds more complications and reoperations in patients who have undergone open surgery. Other comorbidity may also influence the choice of surgical method. However, the selection of patients has no effect on our conclusion – that shorter hospitalisation period s and fewer complications among patients who have been operated on with the laparoscopic technique do not result in a correspondingly faster initiation of necessary adjuvant therapy.
The absence of a specified date of surgery in our data is a possible source of error. Approximately 14 % of the patients are admitted as acute cases and are most likely operated on within 24 hours. The remaining patients are normally operated on within 1 – 3 days after admission. Thus, it seems reasonable to estimate a date of surgery on average two days after admission. The conclusion – that many patients start their adjuvant therapy too late – nevertheless remains unaffected by an error of a couple of days in the estimated date of surgery. The time before initiation of adjuvant therapy will still exceed the recommended 28 – 42 days for a considerable proportion of the patients.
This analysis encompasses the entire Norwegian population of patients with colon cancer in the period 2008 – 2013. We have studied parts of the patient treatment that were not registered in the Norwegian Colorectal Cancer Registry. The study thus illustrates that despite the methodological challenges outlined, the Norwegian Patient Register remains a valuable source of data.
We wish to thank Trygve Deraas at the Centre for Clinical Documentation and Evaluation for his valuable comments on the draft manuscript.
MAIN MESSAGE
One-half of all patients who need adjuvant chemotherapy for colon cancer start their treatment later than is recommended by national guidelines.
Patients who have undergone laparoscopic surgery have shorter hospitalisation periods and fewer complications, but still fail to start their adjuvant therapy correspondingly earlier than those who have undergone open surgery.
- 1.
Nasjonalt handlingsprogram med retningslinjer for diagnostikk, behandling og oppfølging av tykk- og endetarmskreft. Oslo: Helsedirektoratet, 2013.
- 5.
Nasjonalt kvalitetsregister for tykk- og endetarmskreft. Årsrapport 2008 – 2014. Tykktarmskreft 1996 – 2014. Endetarmskreft 2015. Oslo: Norsk gastrointestinal cancergruppe, Kreftregisteret, 2015.
- 6.
Bakken IJ, Gystad SO, Christensen OO et al. Sammenlikning av data fra Norsk pasientregister og Kreftregisteret. Tidsskr Nor Legeforen 2012; 132: 1336 – 40. [PubMed]