Comparison of data from the Cause of Death Registry and the Norwegian Patient Register
The data quality in the Cause of Death Registry has been questioned (1). Many death certificates include logical or content errors (2, 3), and the Cause of Death Registry has been criticised for containing a large proportion of non-specific codes or codes that cannot represent the underlying cause of death (4). This is important, since a high quality of the data in the Cause of Death Registry is a precondition for reliable statistics on causes of death, health analyses and research.
The Cause of Death Registry receives all death notifications (5), and the information they contain is coded in accordance with international guidelines (6). In addition to the routine linkage to the National Registry, further medical and forensic autopsy and toxicology reports are retrieved, and checks are made against the Cancer Registry of Norway and the Medical Birth Registry (6). The Cause of Death Registry then determines the underlying cause of death, defined as the disease or injury that initiated the chain of illnesses that caused death to occur, or as the circumstances around the accident/external event that caused the lethal injury (6). The underlying cause of death serves as the basis for statistics on causes of death.
The Norwegian Patient Register retrieves patient data from all parts of the specialist health services (7), including demographic and medical information. These are routinely linked to the National Registry to check the information on the patient’s place of residence and retrieve information on deaths.
The Cause of Death Registry and the Norwegian Patient Register both use the International Classification of Diseases, version 10 (ICD-10) coding standard for coding of causes of death and diagnoses respectively (8).
The Cancer Registry of Norway uses data from the Norwegian Patient Register to request information from hospitals regarding patients who are registered with cancer in the Norwegian Patient Register, but not in the Cancer Registry. The objective of this study was to investigate whether data from the Norwegian Patient Register can be used to advantage by the Cause of Death Registry, especially in cases where non-specific codes for causes of death are used due to incomplete death notifications. We have linked information from the Cause of Death Registry for all deaths that occurred during the period 2009 – 2011 to information for the final year of life reported by somatic hospitals and psychiatric institutions to the Norwegian Patient Register.
Material and method
The study has been carried out in conformity with the Cause of Death Registry regulations (5) and the Norwegian Patient Register regulations (7).
We retrieved information on all persons who died during the period 2009 – 2011 (N = 124 098) from the Cause of Death Registry, and information on all hospitalisations and outpatient consultations during the last year of life from the Norwegian Patient Register. We included a total of 899 265 registrations from somatic hospitals and 51 933 registrations from psychiatric institutions. Information from the Norwegian Patient Register was retrieved with the aid of national identity numbers submitted by the Cause of Death Registry. The national identity numbers were first encrypted and then replaced by study allocation numbers generated by the Cause of Death Registry. The analysis files did not at any time contain identifiable national identity numbers.
Deaths in hospital were defined as having occurred when the patient’s last contact (hospitalisation or outpatient consultation) was registered with «deceased» as the condition at discharge.
We grouped the underlying causes of death in accordance with the European shortlist (6). This list is used in international cause of death statistics and includes 17 main groups and 48 sub-groups. In our presentation we have included all of the main groups, with the exception of «complications of pregnancy, childbirth, and the puerperium» and «certain conditions originating in the perinatal period». These two groups accounted for 267 persons only. In addition, we have carried out analyses for the ten largest sub-groups of the European shortlist, as well as the sub-group «dementia and Alzheimer’s disease», which is used in Norwegian cause of death statistics. In total, 11 sub-groups were included. The ICD-10 codes for the groupings are presented in Tables 1 and 2.
Table 1
Information from the Norwegian Patient Register on contacts with somatic hospitals and psychiatric institutions during the last year of life for persons who died in the period 2009 – 2011, by main group of causes of death
| Somatic hospital |
Psychiatric institution |
|||||||
| Main group¹ (ICD-10 codes²) |
N |
Death in hospitals (%) |
Admission and/or outpatient (%) |
Outpatient only (%) |
Deaths in institutions (%) |
Admission and/or outpatient (%) |
Outpatient only (%) |
|
| Total |
124 098 |
34.9 |
80.9 |
8.5 |
0.2 |
5.4 |
3.4 |
|
| Infectious diseases (A00 – B99) |
2 846 |
53.7 |
85.3 |
4.2 |
0.1 |
4.8 |
3.1 |
|
| Neoplasms (C00 – D48) |
33 087 |
43.8 |
97.4 |
2.2 |
0.0 |
3.7 |
2.7 |
|
| Diseases of the blood and blood-forming organs) and certain disorders involving the immune mechanism (D50 – D89) |
420 |
43.6 |
88.1 |
3.6 |
0.0 |
5.2 |
3.1 |
|
| Endocrine, nutritional and metabolic diseases (E00 – E90) |
3 037 |
20.6 |
74.7 |
10.5 |
0.2 |
6.2 |
3.8 |
|
| Mental and behavioural disorders (F00 – F99) |
5 897 |
5.1 |
50.3 |
11.7 |
0.2 |
8.5 |
5.3 |
|
| Diseases of the nervous system and the sense organs (G00 – H95) |
4 860 |
16.4 |
62.7 |
10.9 |
0.1 |
8.5 |
5.6 |
|
| Diseases of the circulatory system (I00 – I99) |
39 594 |
35.3 |
78.3 |
8.1 |
0.1 |
3.6 |
2.4 |
|
| Diseases of the respiratory system (J00 – J99) |
12 032 |
38.9 |
81.6 |
6.6 |
0.1 |
4.8 |
3.1 |
|
| Diseases of the digestive system (K00 – K93) |
3 839 |
61.7 |
90.5 |
2.8 |
0.1 |
5.5 |
3.6 |
|
| Diseases of the skin and subcutaneous tissue (L00 – L99) |
269 |
33.1 |
81.8 |
7.1 |
0.0 |
6.7 |
4.5 |
|
| Diseases of the musculoskeletal system/connective tissue (M00 – M99) |
772 |
41.6 |
86.7 |
6.2 |
0.1 |
4.7 |
3.5 |
|
| Diseases of the genitourinary system (N00 – N99) |
2 770 |
36.9 |
85.7 |
5.2 |
0.0 |
4.0 |
2.5 |
|
| Congenital malformations (Q00 – Q99) |
386 |
41.2 |
71.8 |
4.7 |
0.3 |
10.1 |
9.3 |
|
| Symptoms, signs and abnormal clinical and laboratory findings (R00 – R99) |
6 317 |
6.5 |
55.1 |
14.2 |
0.1 |
4.4 |
2.6 |
|
| Violent deaths (V01 – Y89) |
7 705 |
28.6 |
73.4 |
11.0 |
1.3 |
20.4 |
8.8 |
|
| [i] | ||||||||
[i] ¹ According to the European shortlist (5). The groups «Complications of pregnancy, childbirth, and the puerperium», and «Certain conditions originating in the perinatal period» (267 persons in total) have been excluded.
² International Classification of Diseases, version 10
Table 2
Information from the Norwegian Patient Register on contacts with somatic hospitals during the last year of life for persons who died during 2009 – 2011, by selected sub-groups of causes of death
| Sub-group¹ (ICD-10 codes²) |
N |
Deaths in hospitals (%) |
Admission and/or outpatient (%) |
Outpatient only (%) |
Equivalent diagnostic code registered in a somatic hospital during the last year of life (%) |
| Total |
124 098 |
34,9 |
80,9 |
8,5 |
– |
| Cancer of the colon and rectum (C18 – C21) |
4 689 |
40,0 |
97,0 |
3,0 |
86,3 |
| Cancer of the pancreas (C25) |
1 940 |
44,2 |
99,2 |
0,8 |
89,7 |
| Lung cancer (C32 – C34) |
6 521 |
50,7 |
99,1 |
0,9 |
91,1 |
| Breast cancer (C50) |
1 965 |
41,4 |
94,7 |
5,3 |
85,6 |
| Prostate cancer (C61) |
3 143 |
31,1 |
95,5 |
4,5 |
87,1 |
| Cancer of lymphatic, haematopoietic and related tissue (C81 – C96) |
2 605 |
59,1 |
97,7 |
2,3 |
90,9 |
| Dementia and Alzheimer’s disease (F00 – F03, G30 – G31) |
7 368 |
3,9 |
48,3 |
11,8 |
26,8 |
| Ischaemic heart disease (I20 – I25) |
15 554 |
37,7 |
78,5 |
21,5 |
50,8 |
| Other cardiovascular diseases (excl. rheumatic and mitral valve disorders (I30 – I33, I39 – I52) |
8 467 |
24,4 |
76,0 |
24,0 |
55,1 |
| Cerebrovascular diseases (I60 – I69) |
9 733 |
36,1 |
77,5 |
22,5 |
56,6 |
| Unknown, unspecified (R96 – R99) |
4 735 |
7,3 |
57,1 |
42,9 |
1,1 |
| Suicide (X60 – X84, Y87.0) |
1 721 |
8,4 |
29,6 |
16,2 |
7,7 |
| [i] | |||||
[i] ¹ According to the European shortlist (5)
² International Classification of Diseases, version 10
The study is descriptive. Data linkages and analyses were carried out with the aid of the Stata statistics software package.
Results
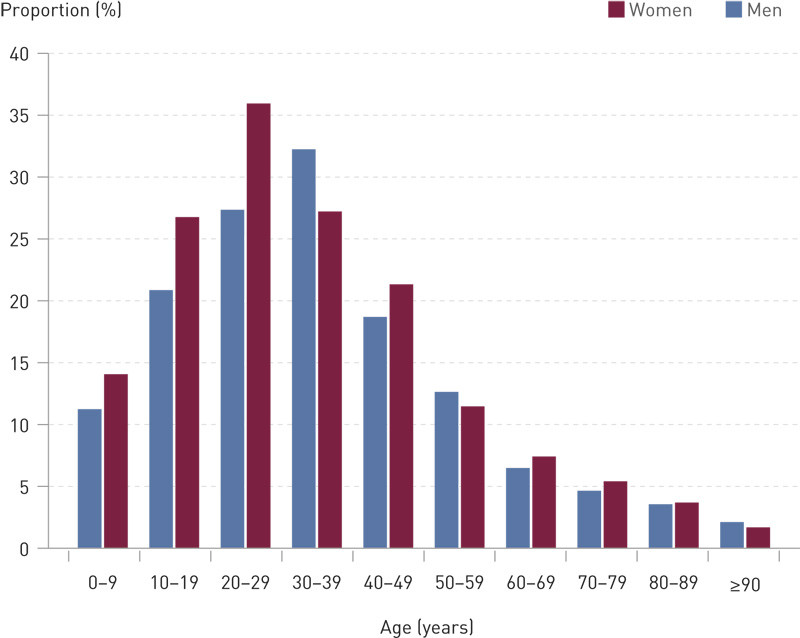
Contact with somatic hospitals and psychiatric institutions during the last year of life by sex and age. In total, 43 250 (34.9 %) of all deceased persons were registered as having died in a somatic hospital (Table 1). There were large variations with regard to sex and age (data not shown). Of the total number of persons who died during the period 2009 – 2011, 100 418 (80.9 %) were registered with at least one admission or outpatient consultation in a somatic hospital during their last year of life (Table 1), with large variations by sex and age (Figure 1). A very small proportion of all deceased (0.2 %) were registered as having died in a psychiatric institution (Table 1). Moreover, the table shows that a total of 6 742 deceased persons (5.4 %) had at least one admission or outpatient consultation in a psychiatric institution during their last year of life. We observed large variations in terms of sex and age (Figure 2).

By main group of causes of death. There were major differences between the main groups of causes of death in terms of the proportion of deaths that had occurred in somatic hospitals (Table 1). The lowest proportion was observed when mental and behavioural disorders had been stated as the cause of death (5.1 %), followed by symptoms and unspecified conditions (6.5 %). We also found major differences with regard to contact with somatic hospitals during the last year of life. The lowest proportion was found among persons with mental and behavioural disorders as their cause of death (Table 1).
The proportion of deaths in psychiatric institutions was low in all main groups, with 1.3 % in the group of violent deaths as the highest value (Table 1). The proportion of persons who had been in contact with a psychiatric institution during their last year of life was highest in the main group of violent deaths (20.4 %) (Table 1).
By sub-group of causes of death. We found further major differences between the subgroups in terms of the proportion of deaths that had occurred in somatic hospitals (Table 2). The proportion was lowest for persons with dementia and Alzheimer’s disease as their cause of death (3.9 %), followed by those with unknown or unspecified conditions (7.3 %). In cancer-related subgroups, we found that nearly all persons involved had been registered in a somatic hospital during their last year of life (94.7 – 99.2 %). The proportion was significantly lower among persons with dementia or Alzheimer’s disease as their cause of death (48.3 %), as well as among persons with unknown or unspecified causes of death (57.1 %). In all sub-groups it was relatively uncommon to have had only outpatient consultations, but no hospitalisation, during the last year of life. An exception is found in the group with unknown/unspecified causes of death, where this applies to 42.9 % of the deceased.
We carried out similar analyses for admissions to psychiatric institutions during the last year of life. In all subgroups, with the exception of suicides, the proportions for outpatient contact alone were relatively similar to the total proportions for contacts with psychiatric institutions (e-Table 3). In the sub-group of suicides, altogether 4.6 % were registered as having died in a psychiatric institution, 41.8 % were registered with an admission and/or outpatient consultation, and 15.2 % were registered with only outpatient contact during the last year of life. In total, 54.6 % of all women and 36.8 % of all men whose cause of death was suicide had been in contact with a psychiatric institution during their last year of life. For women, the proportion was highest in the age group 20 – 49 years (61 % in total), while the proportion among men was highest in the age group 30 – 39 years (46 %).
Table 3
Information from the Norwegian Patient Register on contacts with psychiatric institutions during the last year of life for persons who died during 2009 – 2011, by selected sub-groups of causes of death
| Sub-group¹ (ICD-10 codes²) |
N |
Deaths in institutions (%) |
Admission and/or outpatient (%) |
Outpatient only (%) |
Equivalent diagnostic code registered in a psychiatric institution during the last year of life (%) |
| Total |
124 098 |
0,2 |
5,4 |
3,4 |
– |
| Cancer of the colon and rectum (C18 – C21) |
4 689 |
0.0 |
2.9 |
2.1 |
0.2 |
| Cancer of the pancreas (C25) |
1 940 |
0.0 |
3.2 |
2.4 |
0.3 |
| Lung cancer (C32 – C34) |
6 521 |
0.0 |
4.1 |
2.9 |
0.2 |
| Breast cancer (C50) |
1 965 |
0.0 |
3.5 |
2.9 |
0.1 |
| Prostate cancer (C61) |
3 143 |
0.0 |
2.7 |
1.9 |
0.2 |
| Cancer of lymphatic, haematopoietic and related tissue (C81 – C96) |
2 605 |
0.0 |
3.6 |
2.8 |
0.6 |
| Dementia and Alzheimer’s disease (F00 – F03, G30 – G31) |
7 368 |
0.1 |
3.4 |
2.3 |
0.1 |
| Ischaemic heart disease (I20 – I25) |
15 554 |
0.1 |
3.7 |
2.4 |
0.1 |
| Other cardiovascular diseases (excl. rheumatic and mitral valve disorders (I30 – I33, I39 – I52) |
8 467 |
0.1 |
3.8 |
2.7 |
0.2 |
| Cerebrovascular diseases (I60 – I69) |
9 733 |
0.1 |
5.0 |
2.8 |
0.0 |
| Unknown, unspecified (R96 – R99) |
4 735 |
0.1 |
6.9 |
4.7 |
4.9 |
| Suicide (X60 – X84, Y87.0) |
1 721 |
4.6 |
41.8 |
15.2 |
2.1 |
| [i] | |||||
[i] ¹ According to the European shortlist (5)
² International Classification of Diseases, version 10
Causes of death compared to diagnostic codes
Finally we compared the underlying causes of death with diagnostic codes reported for the final year of life to the Norwegian Patient Register from somatic hospitals (Table 2) and psychiatric institutions (e-Table 3) for the sub-groups of causes of death. With regard to cancer diagnoses, we largely found that codes equivalent to the codes for causes of death had also been registered by somatic hospitals in the Norwegian Patient Register (85.6 – 91.1 %), whereas this was not as often the case for diseases of the circulatory system. Codes belonging to the sub-group of unknown and unspecified causes of death are invalid in the Norwegian Patient Register and are rarely registered there (1.1 % for somatic hospitals).
Discussion
In this descriptive study we have seen that among those who died in the period 2009 – 2011, four out of five had been admitted to and/or had an outpatient consultation in a somatic hospital during their last year of life. The proportion who had been in contact with a psychiatric institution was much lower.
The proportion of deceased persons who had been in contact with a somatic hospital was relatively low among boys/men aged 10 – 29 years. This can most likely be explained by a higher proportion of deaths from violent causes in these age groups.
We found that approximately one in two persons whose underlying cause of death was dementia and Alzheimer’s disease had been admitted and/or had an outpatient consultation during their final year of life, with a very small proportion of deaths in somatic hospitals. This concurs with information from the Cause of Death Registry, showing that the vast majority of persons in this group died in nursing homes (data not shown).
Among persons with unknown or unspecified causes of death, more than half had been in contact with a somatic hospital during their last year of life. However, most of these were registered with outpatient consultations only, which may limit the potential benefits of retrieving data from somatic hospitals to supplement the death certificate in such cases.
For cancers as the underlying cause of death, a relatively large proportion had equivalent diagnostic codes in the Norwegian Patient Register. Since 2010, data from the Norwegian Patient Register have been routinely transferred to the Cancer Registry of Norway (9). The Cancer Registry checks the diagnostic codes in their databases against the Norwegian Patient Register and requests supplementary information from the hospitals if the codes fail to match. Before the decision to introduce routine data transfer, a study was undertaken in which the data on cancer diagnostic codes in the Norwegian Patient Register were collated with data in the Cancer Registry of Norway (10). For all groups of cancers studied, there was good correspondence between the two registries. For some forms of cancer, however, the question will remain as to whether someone has died from or with the cancer. This applies in particular to deaths among elderly men with prostate cancer (11).
In Sweden it has been shown that inclusion of data from patient records for the last year of life to determine the underlying cause of death resulted in a change for approximately 11 % of all deaths, but only for somewhat less than 5 % of deaths from cancer (12). Another Swedish study based on a review of medical histories for the last hospitalisation before death also showed that the quality of data on causes of death varies considerably with the group of causes, with the best correspondence for cancers (13). Similar findings have been made in France, where cancer could most frequently be identified as the last main diagnosis for persons who had died in hospital (14).
To the best of our knowledge, no equivalent studies of contact with mental healthcare institutions during the last year of life have been made, in Norway or internationally. In our study, we found that among those who had died from violent causes, one in five had been in contact with a psychiatric institution during their final year of life. Among the deceased whose underlying cause of death was mental disorder, the corresponding figure was one in twelve. Even though the total number of persons who died from these causes is low, it might be valuable to collect supplementary information from psychiatric institutions for quality assurance of the causes of death reported to the Cause of Death Registry.
Conclusion
We have shown that four of every five persons who died during the period 2009 – 2011 had been registered with an admission and/or an outpatient consultation in a somatic hospital during their final year of life, while one in every 20 persons had been registered as having had contact with a psychiatric institution. In case of absent or incomplete information in the death certificate, data from the Norwegian Patient Register can be used to identify the hospitals/institutions in which the deceased person was treated during his/her final year of life. This information can subsequently be used to request supplementary information from the hospitals/institutions in question. As yet, however, there is no empirical evidence showing that this would prove valuable. Among deceased persons with an unknown or unspecified cause of death, only few have been treated in a somatic hospital/psychiatric institution during their final year of life. This limits the potential benefits of such data collection to the quality assurance efforts of the Cause of Death Registry.
MAIN MESSAGE
During the last year of life, four out of five deceased people had been hospitalised or attended outpatient consultations at a somatic hospital, while one in 20 had been in contact with a mental healthcare institution.
If the information in the death certificate sent to the Cause of Death Registry is absent or incomplete, data from the Norwegian Patient Register can provide information on where the patient has been treated, thus enabling the Cause of Death Registry to contact the hospitals or institutions in question.
Any benefit from such data in the quality assurance efforts of the Cause of Death Registry is limited by the fact that there is the least range of information in the Norwegian Patient Register for those whose cause of death is unknown or unspecified.
- 1.
Pedersen AG, Ellingsen CL. Datakvaliteten i Dødsårsaksregisteret. Tidsskr Nor Legeforen 2015; 135: 768 – 70. [PubMed]
- 3.
Alfsen GC, Lyckander LG, Lindboe AW et al. Kvalitetssikring ved dødsfall i sykehus. Tidsskr Nor Legeforen 2010; 130: 476 – 9. [PubMed]
- 4.
Mathers CD, Fat DM, Inoue M et al. Counting the dead and what they died from: an assessment of the global status of cause of death data. Bull World Health Organ 2005; 83: 171 – 7. [PubMed]
- 5.
FOR-2001 – 12 – 21 – 1476. Forskrift om innsamling og behandling av helseopplysninger i Dødsårsaksregisteret (Dødsårsaksregisterforskriften). http://lovdata.no/dokument/SF/forskrift/2001-12-21-1476?q=d%C3%B8ds%C3%A5rsaksregister (7.8.2015).
- 6.
Folkehelseinstituttet. Dødelighet og dødsårsaker i Norge gjennom 60 år 1951 – 2010. Oslo: Nasjonalt folkehelseinstitutt, 2012.
- 7.
FOR-2007-12-07-1389. Forskrift om innsamling og behandling av helseopplysninger i Norsk pasientregister (Norsk pasientregisterforskriften). http://lovdata.no/dokument/SF/forskrift/2007-12-07-1389?q=norsk+pasientregisterforskriften (7.8.2015).
- 8.
Helsedirektoratet. ICD-10 Den internasjonale statistiske klassifikasjonen av sykdommer og beslektede helseproblemer. Oslo: Helsedirektoratet, 2011.
- 9.
Cancer in Norway. 2009. Cancer incidence, mortality, survival and prevalence in Norway. Oslo: Kreftregisteret, 2010.