In the vernacular, overweight is often synonymous with both overweight and obesity, two conditions that differ in terms of their aetiology, prognosis and treatment. Clinicians tend to use the WHO classification of body mass on the basis of the body mass index (BMI) and distinguish between overweight and varying degrees of obesity (1). In encounters with patients, finding a precise term may represent a challenge, and it is conceivable that the choice of terms may have an effect on the climate of cooperation and treatment outcome.
Many people who are overweight or obese realise that they are at risk of disease. Some of them nevertheless find it difficult to change their lifestyle. Since 66 % of the population see their doctor each year, the GPs can play a key role (2). An American study shows that patients with a high body mass index more often cancel the appointment with their doctor if they are to be weighed (3). As regards the doctor, co-morbidity rather than body mass index will decide whether an issue will be made of the patient’s weight (4) – (6). There could be a negative association between the patient’s body mass index and the doctor’s use of time for the consultation (7). In sum, this may indicate that both the patient and the doctor tend to evade the topic of overweight, and overweight will be addressed only when complications occur.
How one’s own body size is perceived varies from one person to the next. In addition, this perception will vary according to life stage, gender (8, 9) and age (10). Moreover, there is a general tendency to underreport bodyweight (11). An increasing prevalence of overweight nowadays may help normalise this condition and cause fewer people to regard themselves as overweight.
In addition, the conversation between the doctor and the patient may be complicated by the fact that various vernacular expressions for overweight and obesity may be perceived as pejorative. Making the body an issue impinges on individual self-esteem; this is further highlighted by the prevalence of depression among people with manifest obesity (12). In general, society harbours negative attitudes to overweight, including in the health services (13). Although clinicians differ in their opinions regarding how overweight should be referred to in relation to patients (14, 15), there is little empirical knowledge in this area. Two American studies have studied patients’ sensitivity to various expressions, but differences in language and culture render the findings not immediately transferable to Norwegian conditions. No Norwegian studies have been made in this field.
In this study we have investigated the way in which Norwegian patients perceived various expressions for obesity. This is referred to as sensitivity to expressions, here understood as how appropriate or inappropriate the various designations were perceived to be.
We seek to answer the following questions:
To what extent have morbidly obese patients experienced that their obesity has been made an issue by their GP?
How inappropriate did patients with obesity deem the use of various expressions?
Is the sensitivity to expressions related to background variables such as gender, age, education, marital status, mental health, assessment of one’s own weight and/or the stage in life when overweight first developed?
Material and method
Participants
The analysis of sensitivity to expressions was a secondary end point of a five-year study of patients who originally had been referred to St Olavs Hospital for treatment of morbid obesity. Out of 206 participants altogether 157 completed the questionnaire (response rate 76 %). The questionnaire was distributed prior to the one-year examination with a request to return it on attendance, whereupon complete information was obtained for 142 patients from Central Norway. Because of the successive inclusion procedure, the study extended from 2005 to 2013. In a previous article we have described the treatment provided to these patients and its health effects (18). All the patients fulfilled the criteria for morbid obesity and had a BMI > 35 kg/m² at the time of inclusion.
The study was approved by the Central Norway Regional Committee for Medical and Health Research Ethics (REK).
Data
The following variables were included in the analysis of sensitivity to expressions: gender, age (continuous variable), level of education (primary/lower secondary/vocational or upper secondary/higher education), marital status (living alone or with a partner), time of onset of overweight (childhood/adolescence or adulthood) and satisfaction with the weight loss achieved after treatment (satisfied or dissatisfied).
Furthermore, we included the dimension of social functioning from the SF-36, on the basis of the questions referring to whether the respondents’ physical health or emotional problems have had an effect on social contacts. The SF-36 is a generic instrument for measuring quality of life and contains 36 questions that permit construction of eight separate dimensions of experiences (19).
We used symptom intensity for anxiety measured with the aid of HADS (Hospital Anxiety and Depression Scale) (20). Both the SF-36 and HADS (the anxiety dimension) were included in the analysis as continuous variables. The regression analysis included only the anxiety dimension from HADS, because of multicollinearity between this dimension and depression.
The choice of variables for the analysis was based on what we hypothetically assumed to play a role. The availability of variables was also determined by the framework defined by the original data in the five-year (main) study from which the investigation of expressions emerged, since this part of the study was added after the initiation of the main study.
Sensitivity to expressions
The questions pertaining to sensitivity to expressions were inspired by an American study (16). The questionnaire was developed especially for this study, and a test-retest analysis of 33 persons found a high correlation.
In the questionnaire, the patients were asked to imagine the following situation: «You are seeing your GP for a regular check-up. This happened before you were referred to the hospital for treatment of overweight. On his/her own initiative, the doctor wants to talk to you about your overweight and the consequences it may have for your health. You have not previously talked to your GP about your overweight.»
This was followed by 14 different terms for overweight or obesity that were assumed to have been used by the doctor. Each term was scored by the patient in terms of their sensitivity on a five-point scale, with response alternatives ranging from very inappropriate (– 2) to very appropriate (+ 2). The terms were collected from the Overweight Patients’ Association, which had been requested to provide designations that could be perceived as either positively or negatively charged. Expressions that are primarily used as terms of abuse were excluded.
The following terms were included in the questionnaire, in this order: «overweight, «weight problem», «BMI», «high BMI», «obesity», «morbid obesity», «obesitas», «excess weight», «too heavy», «obese», «fat», «big», «stout» and «weight».
The questionnaire also contained the following questions (with the response alternatives yes/no/don’t know): Whether the doctor’s choice of term would have had an impact on the doctor-patient relationship, whether it would be appropriate for the doctor to initiate a conversation about obesity, and whether the patients had actually encountered such an initiative on the part of their doctor.
Statistical analyses
The sensitivity to expressions could be rendered in five categories. We used Friedman’s ANOVA followed by Wilcoxson’s signed-rank test to assess differences between the terms. Because of a high number of paired tests (n = 91), the significance level was adjusted to 0.001. The three terms that were given the highest total of negative scores were merged to a single variable, permitting an investigation of the phenomenon of sensitivity to expressions, rather than to each individual term. Such a collective variable will also reduce the risk of random measurement errors.
Using multiple linear regression we then investigated whether sensitivity to expressions was associated with background factors (significance level 0.05). Because of the limited sample size we drew repeated random samples («bootstrapping»), a technique that produces confidence intervals estimated by the real distribution in the material, not based on an assumption of a normal distribution. Statistical estimates were undertaken in PASW Statistics 18 (SPSS Inc., 2009, Chicago, IL).
Results
The study is based on 157 persons (76.2 %) who completed the questionnaire on sensitivity to expressions. At the time of testing (one year into the study), the participants’ average body mass index (SD) had fallen from 45.2 kg/m² (5.7 kg/m²) to 37.6 kg/m² (7.3 kg/m²).
Table 1 shows sociodemographic and anthropometric data for the sample.
Table 1
Sociodemographic and anthropometric data for the 157 included patients, all of whom had undergone weight-loss treatment one year previously
| Age (years) – average ± SD |
42.6 ± 9.2 |
| Women – number (%) |
119 (75.8) |
| Men – number (%) |
38 (24.2) |
| Co-habiting/married – number (%) |
96 (57.0) |
| Education equivalent to a bachelor’s degree or higher – number (%) |
54 (35.7) |
| Onset of overweight in childhood/adolescence – number (%) |
108 (71.5) |
| BMI (kg/m²) – average initial value ± SD |
45.2 ± 5.7 |
| BMI (kg/m²) – average one year after treatment ± SD |
37.6 ± 7.3 |
The patients’ experiences from doctors raising the issue of overweight and obesity
Altogether 124 patients (80 %) were of the opinion that the doctor’s ability to express him-/herself had an effect on the collaborative relationship, and 145 patients (92 %) deemed it appropriate for the doctor to initiate a conversation about obesity and its health consequences. Altogether 52 patients (33 %) reported to have encountered such an initiative on the part of their doctor.
The patients’ assessments of terms and expressions
The test of the total variation between the terms was statistically significant: χ²(13) = 857.8; p < 0.001. Figure 1 shows the details in sensitivity to expressions. Among the terms, «weight» scored highest, with an average score (SD) of 1.51 (± 0.7) – this was significantly different (p < 0.001) from the other terms. This was followed by «overweight» with a score of 1.17 (± 1.0); «weight problem» with 0.98 (± 1.1); «BMI» with 0.69 (± 1.1); «too heavy» with 0.68 (± 1.2); «high BMI» with 0.27 (± 1.2) and «too stout» with 0.24 (± 1.2).
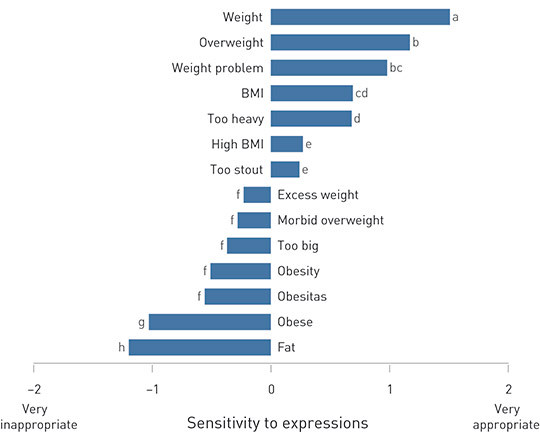
«Fat» (NO: «feit») was deemed the most inappropriate term with an average score of –1.20 (± 1.2). Moreover, «fat» differed significantly from «obese» (NO: «fet»), which scored –1.03 (± 1.2). The next five scores were not significantly different: «obesitas» – 0.56 (± 1.2); «obesity» – 0.51 (± 1.4); «too big» – 0.37 (± 1.3); «morbidly obese» – 028 (± 1.4) and «excess weight» – 0.23 (± 1.3).
The highest sensitivity to expressions was found among women, those who developed overweight in early life and those who were dissatisfied with their weight (Table 2). Age, marital status, anxiety symptoms and social functioning status did not achieve significance in the model. The regression is based on those 142 participants for whom we had complete data.
Table 2
Who were the most sensitive to the least favoured terms for obesity? Multiple linear regression with sensitivity to expressions predicted by various patient characteristics in 142¹ patients who had undergone weight-loss treatment. 95 % confidence interval
|
|
B² |
95 % CI of B |
| Education (0³ = primary/lower secondary/vocational; 1 = upper secondary) |
–1.92 |
–2.92 — –0.90 |
| Onset of obesity (0 = childhood/adolescence; 1 = adulthood) |
1.59 |
0.29 — 2.82 |
| Gender (0 = woman; 1 = man) |
1.58 |
0.39 — 2.86 |
| Self-assessment of weight (0 = dissatisfied; 1 = satisfied) |
1.24 |
0.27 — 2.23 |
| Social functioning (SF-36) |
–0.06 |
–0.11 — 0.01 |
| Anxiety symptoms (HADS) |
–0.11 |
–0.22 — 0.01 |
| Marital status (0 = single; 1 = living with partner) |
0.55 |
–0.32 — 1.52 |
| Age (years) |
–0.00 |
–0.06 — 0.06 |
| [i] | ||
[i] ¹ Complete data for the regression analysis only for 142 participants.
² Beta is a regression weight and denotes the difference in sensitivity to expressions when the variable changes by one unit while all other variables remain constant. Positive values indicate less sensitivity while negative values indicate increased sensitivity to expressions.
³ For dichotomous variables 0 is the reference category. Example: Persons with upper secondary education (or higher) are on average two score points more averse to the expressions than those who have only primary/lower secondary/vocational education when all other factors remain the same.
Discussion
Our study shows that many patients felt it to be appropriate for the doctor to initiate a conversation on overweight and obesity. At the same time, the patients were sensitive to a number of terms that describe obesity. Many respondents claimed that a wrong choice of words has a negative impact on their relationship to the doctor. As noted above, women had the highest sensitivity to expressions, as well as those who developed overweight early in life, those who had higher education and those who were dissatisfied with their weight.
One in every three patients reported that the doctor had taken the initiative to talk about obesity. Taking the patients’ considerable weight into account, this is a low figure. Another study has shown that weight was a topic in only 17 % of consultations with overweight patients (21). Moreover, notions may vary among patients and doctors as to whether the topic of weight has been raised at all during the consultation. One study found that patients far more rarely than doctors thought that weight had been referred to. The largest discrepancy in opinion was found among patients who had made little effort to lose weight by themselves (22), which emphasises the complexity involved in conversations about this topic.
GPs are reluctant to discuss overweight with their patients because they are apprehensive of causing offence (5, 23). This is especially challenging when the doctor is unfamiliar with the patient (4). In order to succeed with prevention, this topic must be raised at an early stage. Assuming that patients who are overweight, but otherwise healthy, visit their GP more rarely than obese patients with co-morbidity, this means that the conversation on weight must be held with unfamiliar patients. This should also happen in cases where the patients themselves fail to take such an initiative. Findings indicating that co-morbidity rather than body mass index is decisive for the doctor to raise the issue of obesity (4) – (6) highlight the need for prevention. Nine out of ten patients in our study believed that the doctor was correct in taking such an initiative.
The higher sensitivity to expressions among women may be related to gender differences in terms of self-image and bodily awareness. Women tend to be more critical of their own bodies (8, 9), whereas men have a greater tendency to underestimate their own weight (24). It has also been shown that men prefer a more frank language than women do (25).
A contributory factor to the higher sensitivity among people with higher education could be that in contrast to those with less education, they have a lower tendency to underestimate their own weight (24). Therefore, certain expressions may to a greater extent be perceived as confronting. In a sociolinguistic perspective, frank usage may be more prevalent in communities with less education and those with more education may be less hardened to it. A third explanation as to why people with higher education relatively speaking find overweight more stressful could be the perception of falling outside of socially acceptable norms (26).
Somewhat unexpectedly, we found no predictive value of anxiety symptoms measured on the HADS scale. The same applied to the ability to function socially, age and marital status.
There was a clear correlation between having been overweight early in life and being sensitive to expressions. Most likely, this can be traced back to experiences of stigmatisation because of overweight (27), something that thereby may have exerted a decisive influence on identity development. People who develop overweight in adulthood will hardly internalise social norms as strongly.
The data were collected at the one-year follow-up of treatment for obesity. On this occasion the patients reported their degree of satisfaction with their own body/weight loss at that time. Initial weight losses may serve as encouragement and strengthen the patient’s self-image, which may partly explain why those who were dissatisfied with their weight were also more sensitive to expressions.
Traditionally, doctors have actively overseen the development of professional terminology (28), and clinicians tend to seek linguistic precision. Our findings show, however, that expressions which to clinicians ought to clearly denote BMI > 30 kg/m² in fact give rise to negative reactions in patients.
While «overweight» is a precise expression for a body mass index score of 25 – 30 kg/m², it would be correct to use designations such as «obesity/obese/fat», «adipositas/adipose» and «obesitas» for a BMI > 30 kg/m². Most likely, clinicians tend to avoid the expressions «adipositas/obesitas» because they are unknown to people in general. They may also avoid «obesity/obese/fat» because of apprehension about causing offence. They tend to use incorrect terms such as «overweight» and «morbid overweight» including for a BMI > 30 kg/m². Is it correct to let the patients’ perceptions of these terms govern the language usage of health personnel?
This question can be regarded in light of protection motivation theory, in which personal health concerns may be seen as having a positive value (29). A key element of this theory is the individual’s assessment of threat – the perception of a health risk (vulnerability) and the degree of seriousness of the consequences (severity). Health concerns are seen as a resource for changing harmful behaviour. It is conceivable that more specific terms have a greater potential for enhancing such concerns.
However, this theory rests on an important assumption: One should at the same time guide and support new behaviour. Thus, the theory does not legitimise uncritical use of terms when the therapeutic relationship is about to cease or otherwise does not emphasise any change in health-related behaviour. In isolation, offensive terms may produce the reverse of their intended effect (30). At the same time, there are studies showing that obesity patients perceive frank expressions as more motivating than euphemisms for promoting change (31, 32). In this way, it may be more appropriate to use a more frank, perhaps even confrontational, language to patients, at least as far as men are concerned.
Seen in isolation, the choice of terms will hardly have a direct impact on the degree of weight loss, although they may help influence mental processes that are helpful in bringing about changes in behaviour. Hearing the doctor say that they are fat may help patients realise the seriousness of the situation. Such notions also accord with what we know about relative risk of disease (33).
We already know that men and young people in general prefer more frank modes of expression (31). Our study confirms the gender difference, but also points to other significant factors. It is difficult to know where to draw a line between what will have a motivational effect and what would only be seen as offensive. If the patients perceive this as stigmatisation, they may react by avoiding consultations or changing their GP. In this way, unfortunate use of terms may at worst have negative health consequences (32).
This study is based on patients suffering from morbid obesity. The findings cannot be directly generalised to the far larger population of overweight people who are not seeking treatment. In addition, we need to take into account that one of the questions was associated with issues somewhat in the past, and this may have had an effect on the responses. The selection of variables for the regression analysis was restricted to data that had been collected before this sub-study was initiated. Other variables that were unavailable to us may possibly have had an effect on the sensitivity to expressions and thus on the results.
In our opinion, the findings are relevant – especially for GPs. They often observe their patients’ weight increase and one of their tasks is prevention. Knowledge about the perception of language usage may lower the threshold for raising the issue of body weight at an early stage, thus increasing the effectiveness of prevention.
The research fund at Unimed Innovation and St. Olavs Hospital have granted financial support for this study.
MAIN MESSAGE
Most of the patients felt that their doctor had acted appropriately in taking the initiative for a conversation about obesity and its consequences for health.
Expressions such as obesitas, obese and fat were perceived as improper, whereas weight and overweight were seen as more appropriate.
Women, people with higher education and those who developed overweight at an early stage in life were especially sensitive to these expressions.
- 1.
Obesity. Preventing and managing the global epidemic. Genève: World Health Organisation, 2000.
- 2.
Nossen JP. Hva foregår på legekontorene? Konsultasjonsstatistikk for 2006. Oslo: Arbeids- og velferdsdirektoratet, 2007.
- 6.
Potter MB, Vu JD, Croughan-Minihane M. Weight management: what patients want from their primary care physicians. J Fam Pract 2001; 50: 513 – 8. [PubMed]
- 10.
Reboussin BA. Correlates of satisfaction with body function and body appearance in middle-and older aged adults: The Activity Counseling Trial (ACT). Psychol Health 2000; 15: 239 – 54. [CrossRef]
- 14.
Guide to authors. The Obesity Society. http://onlinelibrary.wiley.com/journal/10.1002/(ISSN)1930-739X/homepage/ForAuthors.html (14.9.2015).
- 15.
Holmén J. Den som lider av fetma är fet! Läkartidningen 1999; 96: 3081. [PubMed]
- 25.
Kirtley MD, Weaver JB. Exploring the impact of gender role self-perception on communication style. Women's. Stud Commun 1999; 22: 190 – 209.
- 28.
Myking J. Terminologiutvikling – kulturpolitikk og sosialpolitikk. Tidsskr Nor Legeforen 2008; 128: 850.
- 29.
Norman P, Boer H, Seydel ER. Protection motivation theory. I: Conner M, Norman P, red. Predicting health behaviour. New York, NY: McGraw-Hill Education, 2005.
- 30.
Boer H, Seydel ER. Protection motivation theory. I: Conner M, Norman P, red. Predicting health behaviour. New York, NY: McGraw-Hill Education, 2005.