More cost-efficient and holistic patient pathways are a goal for Norwegian and international health policy (1, 2). Priority is given to providing better help quickly to those who need it in the municipality (2, 3). It is seen as desirable to provide health services close to the patient’s home, and one of the instruments for this is to ensure that all municipalities can undertake emergency hospitalisations (EH) to reduce the number of hospitalisations in the specialist health services (3). The Health and Care Services Act (4) requires all municipalities to establish such a service. From 1 January 2016 all municipalities will be obligated to provide this service.
The new Act on municipal health and care services does not identify particular groups of patients for whom municipal service provision will be appropriate, but the guidelines issued by the Directorate of Health state that this applies to patients who are frequently hospitalised (3).
Previous studies (5) – (7) have mainly focused on experience from emergency hospitalisation in small municipalities that engage in inter-municipal collaboration.
The objective of this study is to develop knowledge on experience with this service gained by medium-sized municipalities that are not engaged in inter-municipal collaboration. Some municipalities started as early as January 2012. The municipalities organise their service provision in various ways, and it is essential to obtain knowledge of experience gained from different models (8). This knowledge can be used by politicians, health workers and others who have responsibility for planning and implementation of the service.
We formulated the following research questions:
What experience have health workers in medium-sized municipalities gained from the establishment of emergency hospitalisation?
To what extent are the inpatient beds being utilised?
Material and method
In this study we have used qualitative as well as quantitative data (mixed methods) (9), since we wished to obtain information on the experience of the health personnel, in addition to statistics on the hospital bed utilisation in each municipality.
A total of six focus-group interviews (10, 11) were conducted with health personnel in positions with co-responsibility for the scheme. The interviews were conducted from November 2013 to March 2014 in six small and medium-sized municipalities in Western Norway (Figure 1) (12). Data on the utilisation of the emergency hospitalisation beds were subsequently retrieved from the same municipalities.
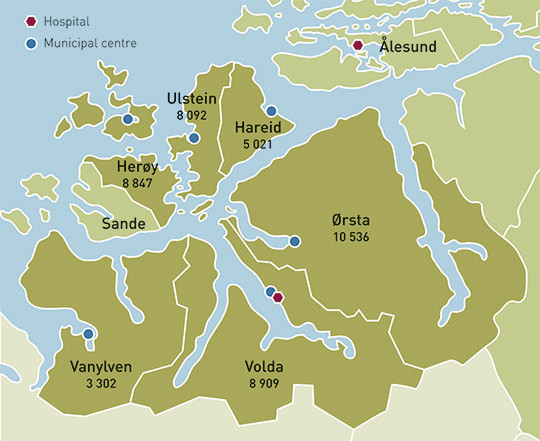
Participating municipalities
The participating municipalities are members of an inter-municipal, inter-professional collaboration between seven municipalities that meet at regular intervals (known as «the seven-pointed star»). All these six municipalities had chosen to operate the service without any inter-municipal collaboration, which sets it apart from most other services in Møre og Romsdal county.
One of the municipalities was not included in the study, since it had not yet established an option for emergency hospitalisation.
Participants
The informants were selected strategically (10). They were recruited because they were in charge of, and had experience from, operating an emergency hospitalisation service in the municipality. We wished to include informants from a variety of professions. We asked GPs, heads of care services, heads of departments for short-term/overnight services, doctors in nursing homes, chief medical officers and an experienced nurse to participate in the interviews. Not all of the municipalities were organised in such a manner that all these positions existed. The participants were contacted by the head of care services and were provided with written information on the project in advance.
Altogether 25 persons were interviewed, out of 30 who were requested. Ten of the participants were doctors, 14 were nurses and one had a background from social services. At the time of the interviews, the municipalities had experience ranging from approximately six months to two years.
Data collection
The focus-group interviews were conducted in the municipal administration building or other municipal institutions. An interview guide was prepared (10) on the basis of national documents (3). The questions addressed five topics: experience from an early start, quality, patient co-determination, competence and patient pathways.
The last author acted as group moderator for the interviews (10, 13). In addition, one or two co-researchers were present, taking notes about the group dynamics during the interviews (14). The co-researcher gave a final summary of what had been reported, and the participants were given an opportunity to supplement or correct the summary. The interviews lasted 60 – 90 minutes. They were recorded on an audio device and transcribed verbatim. The text was adjusted for written presentation. Data on the utilisation of emergency hospitalisation were retrieved from the operational statistics for each municipality.
Analysis
The analysis was inspired by the hermeneutic circle (15). All authors were supplied with the transcribed interviews for review. Data were initially coded wherever we found significant units of meaning with regard to three areas: initiation, assessment of the service provided to the patients and consequences for the professional community. Thereafter the analysis brought forth a topic that illustrated the underlying patterns in their experience from each area (10). These topics are used as headings in the section on results.
The analysis was inductive as well as deductive. We started from the raw data to identify main topics, before returning to the raw data to see how the various main topics were corroborated by the material (14). A shared document was established to permit all authors to participate in and monitor the presentation of the findings, thus working towards dialogical intersubjectivity (11). The topics grew out of an analytical process that alternated between working with the parts and the whole, and between pre-understanding and understanding (15).
The authors held different positions, providing them with different entry points to understanding the studied phenomena. One of the researchers is head of division in a health enterprise, one is research advisor in the same health enterprise, and one is professor of nursing at a university college. The fourth researcher was employed as coordinator of the collaboration between the seven municipalities in the Sunnmøre district. Because of their different positions and their interdisciplinary background, the authors could read the material from a variety of perspectives. Data on interaction within the group were used in the analysis of the transcribed interviews (16).
Ethical considerations
An application was submitted to the Regional Committee on Medical and Health Research Ethics (REK Central Norway 2013/1943) to ascertain whether the study was subject to submission for approval. The committee found that this was not the case. The project was undertaken according to research ethics guidelines, and written consent was obtained from all participants at the start of the interviews (10).
Results
The findings elucidate the experience from emergency hospitalisation in six municipalities. Three topics were identified by the analysis: emergency hospitalisation in the home municipality to strengthen the nursing homes; patient-centred and flexible service provision; and competence enhancement.
There was considerable enthusiasm in the focus-group interviews and few tensions between representatives of different professions.
Emergency hospitalisation in the home municipality to strengthen the nursing homes
The health personnel reported that before they started, they had benefited greatly from the inter-municipal, inter-professional collaboration in the seven municipalities. They had developed a shared understanding of how they wanted to operate the service in their home municipality, both in order to help develop the professional community and because it was an advantage for the patients to be provided with services close to their homes.
The municipalities reported that the members of «the seven-pointed star» had shared knowledge of the patient groups to which the service would apply, knowledge about the types of drugs and equipment that were needed and other experience associated with starting to provide emergency hospitalisation. Some municipalities had been granted support by the Directorate of Health, others had politicians who had obtained extra grants for positions for doctors and nurses. It was reported that competence was regarded as a crucial factor for launching the service. The importance of specialist nurses was emphasised in particular.
A patient-centred and flexible service
It was stated that emergency hospitalisation in the municipality is a patient-centred and flexible service.
One of the doctors expressed this as follows: «We believe fairly strongly that there are major advantages to having this in each municipality. Because we provide the service locally, the patients do not need to travel out of the municipality, it’s easier for the next of kin to come and visit, it’s easier to obtain information from the GP and the home nursing services, easier to establish appropriate services after discharge and easier to find out what the patient needs once the EH stage is over.»
The value of providing the service locally, thus better to understand the patient’s life situation and to plan holistic patient pathways based on the patient’s values, was emphasised. In some of the groups, however, it was also stated that the scheme might entail more transfers and more split patient pathways than previously. This would especially be the case when patients were admitted with an undetermined diagnosis.
In the interviews it was also reported that in the participants’ experience, the health enterprise and the municipalities had different ideas about patient pathways. One of the doctors put it like this: «The health enterprise may well establish pathways for difficult and demanding groups of patients, such as those with COPD. We cannot establish patient pathways to the same extent at the diagnostic level. We need to establish patient pathways that capture a larger proportion of the population. We are generalists, they are specialists.»
It was stated that helping to ensure holistic and coordinated patient pathways was essential. Rehabilitation and palliation were cited as examples of such areas that had been developed in the municipalities.
It was emphasised that co-determination is easier to achieve when the patient is treated in the local community. The groups referred to close cooperation with the next of kin to safeguard the patient’s interests. The participants stated that they were well familiar with the ideas about patient co-determination reflected in health-policy documents.
One of the doctors emphasised the need for good information to achieve appropriate patient pathways: «It’s important to specify at the outset what will happen and what the entire patient pathway will look like.»
It was reported that the beds were used flexibly, for example when a patient was transferred from a bed in the EH service to a short-term place without having to move from one municipality or nursing home to another, since the municipalities had chosen to locate these beds in the nursing homes – most of them in a short-term or rehabilitation ward. Others had established separate wards that were not linked to any department. It was stated that some younger patients could react negatively to being admitted to a nursing home. Providing more information to the population was deemed important in all the municipalities.
A positive development was reported, with more extensive bed utilisation, and that for example in the field of palliative care, they were able to provide services that were as good as those in the hospitals. The value of close cooperation with the patient and the next of kin for palliative care was emphasised.
Competence enhancement
The informants reported that the requirement for establishing emergency hospitalisation services had led to competence enhancement and would also require further competence development in the professional community of the nurses and doctors involved.
It was pointed out that locum doctors could be a hindrance to provision of these services in line with its intentions. Access to specialist nurses and nurses with a clinical Master’s degree in nursing was mentioned as a key condition for operating this service. It was reported that systematic efforts in the form of one-day training courses had been undertaken in several municipalities to qualify the personnel for their new functions. It was also noted that the municipalities wished to establish close cooperation with the university colleges with a view to competence enhancement.
One of the most experienced doctors expressed clearly that emergency hospitalisation is a nursing service. «If the patient needs medical attention several times each day, such a patient will not be suitable for municipal EH beds.»
Major emphasis was placed on the necessity of having professionals with relevant competence to handle the challenges involved. The groups reported that positive attitudes and enthusiasm on the part of the staff were preconditions for succeeding in developing an adequate service. Reports by the informants to the fact that the new option has entailed an enhancement of professional competence in the municipal health services as well as many new and interesting work duties featured repeatedly in the interviews.
Reference was also made to the cooperation between the health enterprise and the municipalities. It was noted how the health enterprise had provided valuable guidance, for example with regard to palliation and treatment of severe infections. However, informants also pointed to the need for further clarifications regarding the distribution of responsibilities associated with various stages of the patient pathway. Dialogue between professionals in the health enterprises and the municipal health services was underlined as essential to achieve adequate patient pathways and appropriate transfers between the different administrative levels.
It emerged from the groups that it was essential that bed utilisation had been well thought through and that those involved had a shared understanding of what kind of treatment services the municipalities would provide. The informants also emphasised that the service needed to be adequate and that it was important that a clear diagnosis had been established.
It was also deemed important that the nurses and doctors involved in the provision of this service had trust in each other and were well familiar with each other’s competence. One of the groups maintained that nurses and doctors ought to attend joint training courses. The need for training in topics related to emergency medicine was noted in particular. The value of having shared venues for professionals from the specialist and municipal health services was emphasised.
Use of the service
Five of the municipalities had formally established 1 – 2 beds from 1 October 2012, the sixth on 16 September 2013. Data were collected for the period until 31 August 2014.
A total of 14 admissions and 35 hospitalisation days had been recorded per month, with an average hospitalisation period of 2.5 days (1.8 – 3.1 days in different municipalities) in 2013, and 21 admissions and 60 hospitalisation days per month in 2014, with an average hospitalisation period of 2.9 days (range 2.1 – 3.6 days). Bed utilisation during the observation period increased from the time of establishment of the service in all of the municipalities. Capacity utilisation remained low during the initial year of operation, at 16 % on average, but rose to 20 % in the second year (range 10 – 36 %).
Discussion
The study revealed that the municipalities had cooperated on the establishment of emergency hospitalisation services. They reported to perceive the new service as patient-centred and flexible, and as providing room for greater patient co-determination. In their opinion, the service would also lead to competence enhancement in the municipalities. Bed utilisation has increased from provision of the service started until 31 August 2014 in all six municipalities.
The municipalities included in the study have established a formal collaboration, in relation to which it was made clear that they did not wish for any inter-municipal collaboration on operation of emergency hospitalisation services. They had a shared value base and shared ideological views on the service before development started. This emerged clearly from a number of the interviews.
The main objective of the organisation was to achieve patient-centred and flexible services in the home municipality, where all resources were used to produce seamless service provision. This starting point clearly contrasts with findings from a mapping study conducted in 2013 (5, 6). At that time, more than half of all Norwegian municipalities were in the process of establishing emergency hospitalisation services. Three of four had entered into inter-municipal collaboration, most of which were small municipalities. Most of those that had not entered into inter-municipal collaboration had established such services in association with a nursing home, whereas those who engaged in inter-municipal collaboration had established service provision in association with a casualty clinic. The majority of the small municipalities had no service established in their own local community. This means that for most of them, the service is provided in a neighbouring municipality. The municipalities have chosen to organise and operate the service in varying ways.
Our results are more in line with those of Grimsmo and Løhre (7). They describe a split between the centre and periphery with regard to views on organisation. Inter-municipal service provision in proximity to a hospital appeared meaningless to doctors in peripheral municipalities, because of the excessive travel distances involved. It was also pointed out that many doctors perceived few differences between inter-municipal and local service provision. The difference pointed out by these authors in terms of how central and peripheral municipalities regard the organisation of this service is a key discussion that will have professional as well as organisational implications.
In these municipalities, emergency hospitalisation is mainly a nursing service that requires a clear diagnosis before admission. This is a clear premise for the organisation, which will differ from other types of organisation where diagnostic services are also provided and where there is better access to medical services. Patient selection and the scope of bed utilisation may differ considerably between such services. They may also have varying potential for a reduction in the number of admissions in the specialist health services based on the design of the admission criteria and the diagnostic services provided. Our study cannot draw any conclusions in this respect.
Access to nursing competence in the municipalities was deemed especially important for the establishment and operation of the service. The flexible organisation of the emergency hospitalisation in nursing homes enabled this competence to be used flexibly for several groups of patients and thus help strengthen the overall competence in the municipalities. The extent to which the university colleges will be able to provide relevant competence to the municipalities by way of their training programmes may prove important for the establishment and development of this service.
In all of the municipalities we can observe increasing bed utilisation over time. However, the rate of utilisation was nevertheless relatively low in relation to capacity even in the second year of operation, varying between 10 % and 36 %. Vanylven municipality, which has the longest experience of operating the service, also has the highest rate of utilisation of bed capacity. This may indicate that the doctors need some time to gain confidence in the service and in how they can make use of it. Bed utilisation in these six municipalities is not significantly different from what emerged in the mapping study in 2013 (5, 6). Our study has no data that can show whether the extent of utilisation of emergency hospitalisation services has reduced the use of inpatient beds in the specialist health services.
The study revealed that the informants wished to establish more patient-centred treatment sequences than are seen in the specialist health services, where these are linked to diagnoses. This corresponds with findings made by Røsstad and collaborators (17) which indicate that a disease-oriented perspective on patient pathways is unsuitable in the municipal health services. A key finding in our study is that the municipalities envisage a need for establishing holistic treatment sequences that capture wider patient groups. Rehabilitation and palliation were examples of areas where such solutions had been established.
One interesting finding is that the informants deemed it easier to achieve co-determination when patients are treated in their local environment. Dialogue on values in the choice of end-of-life treatment was another key finding in our study. Our findings largely correspond to those made by Lappegard and Hjortdahl in Ål municipality, although that service programme is somewhat more comprehensive than the one provided by our municipalities (18). Lappegard and Hjortdahl found that in the patients’ opinion, the local provision of treatment gave a feeling of overview and continuity of care on home ground. It may appear as though emergency hospitalisation is able to respond appropriately to key intentions of the Interaction Reform regarding reinforcement of the right to co-determination for patients and their next of kin.
Limitations
The generally positive attitude to emergency hospitalisation came as something of a surprise to us. It is conceivable that if more of the nurses who are involved in daily operations had been included, more of the problems associated with operating the service would have come to light.
The study is unable to reveal the number of patients that otherwise would have been admitted to hospital, and we have no data regarding the distribution by type of service provided to the patients after discharge from emergency hospitalisation.
Conclusion
Establishment of a patient-centred and flexible service was the key justification for providing an emergency hospitalisation service within the municipality. The health workers reported that this had resulted in competence enhancement in the municipality, while high-level nursing competence was a precondition for establishing adequate service provision to patients.
Utilisation of the service appears to have been low during the initial year of operation, but increased over time afterwards. Appropriate interaction between the different professions involved in provision of the service was deemed important. There is a need for further research that can provide for evidence-based organisation of the service and knowledge about the types of organisation and content that would be appropriate in each municipality, in light of their size, geographical conditions and distances to local hospitals, as well as factors that determine the utilisation and quality of this inpatient service.
MAIN MESSAGE
Inpatient treatment in the local community provided good conditions for patient co-determination and dialogue on value issues.
Good interaction between the professions involved was regarded as a key condition for appropriate development of these services.
- 1.
Together for health: a strategic approach for the EU 2008 – 2013. Brussel: European Commission, 2007.
- 2.
St.meld. nr. 47 (2008 – 2009). Samhandlingsreformen. Rett behandling – på rett sted – til rett tid. www.regjeringen.no/contentassets/d4f0e16ad32e4bbd8d8ab5c21445a5dc/no/pdfs/stm200820090047000dddpdfs.pdf (4.7.2015).
- 3.
Kommunenes plikt til øyeblikkelig hjelp døgnopphold. Veiledningsmateriell. Oslo: Helsedirektoratet, 2014.
- 4.
Lov om kommunale helse- og omsorgstjenester m.m. (helse- og omsorgstjenesteloven). https://lovdata.no/dokument/NL/lov/2011-06-24-30 (4.7.2015).
- 5.
Undersøkelse om bruken av øyeblikkelig hjelp døgnopphold i kommunene. Oslo: Deloitte, Helsedirektoratet, 2014.
- 6.
Spørreundersøkelse om øyeblikkelig hjelp døgnopphold i kommunene. Oslo: Deloitte, Helsedirektoratet, 2014.
- 7.
Grimsmo A, Løhre A. Erfaringer med etablering av kommunalt øyeblikkelig hjelp døgntilbud. Utposten 2014; 43: 14 – 7.
- 8.
Kommunalt øyeblikkelig hjelp døgntilbud. Rapport fra Den norske legeforening og KS. Oslo: Den norske legeforening, 2014.
- 9.
Creswell JW. Research design: qualitative, quantitative, and mixed methods approaches. Los Angeles, CA: Sage, 2014.
- 10.
Malterud K. Fokusgrupper som forskningsmetode for medisin og helsefag. Oslo: Universitetsforlaget, 2012.
- 11.
Kvale S, Brinkmann S, Anderssen TM et al. Det kvalitative forskningsintervju. Oslo: Gyldendal Akademisk, 2009.
- 12.
Statistikkbanken. Oslo: Statistisk sentralbyrå, 2014. www.ssb.no/statistikkbanken (4.7.2015)
- 15.
Gadamer H-G, Holm-Hansen L. Sannhet og metode: grunntrekk i en filosofisk hermeneutikk. Oslo: Pax, 2010.
- 16.
Liamputtong P. Qualitative research methods. South Melbourne: Oxford University Press, 2013.
Takk for en interessant artikkel om øyeblikkelig hjelp-døgnopphold (ØHD) i Tidsskriftet nr. 17 2015 (1). Det er interessant med kommuner som går «mot strømmen» og etablerer tilbud i egen kommune. Noe av formålet med ØHD-plassene var jo å etablere et tilbud nærmere pasientens bosted og nærmiljø. Det er ikke alltid tilfelle i interkommunale ordninger. I Hamarområdet må mange av pasientene faktisk reise forbi sykehuset for å komme til de lokale ØHD-sengene.
Pasienter som legges inn i ØHD skal være pasienter som ellers ville blitt lagt inn i sykehus. Dette spørsmålet er lite berørt i artikkelen. Mitt spørsmål er om det tilbudet disse kommunene har etablert er «ordentlige» ØHD-senger, eller om det mer er et slags forsterket sykehjem. Nysgjerrigheten på dette ble vakt da jeg i artikkelen leste sitatet fra den erfarne legen som uttalte at ØHD-senger er et sykepleiefaglig tilbud, og at dersom pasienten hadde behov for legetilsyn flere ganger i døgnet, var ikke ØHD rette plassen (1). Et annet sted står det at studien ikke kan si noe om hvor mange av pasientene som ville blitt lagt inn i sykehus dersom ØHD ikke fantes.
Spørsmålet jeg sitter igjen med blir derfor om denne artikkelen i bunn og grunn handler om ØHD-senger, eller om den handler om et annet (fint) tilbud disse kommunene har etablert?
Litteratur
1. Hole T, Barstad J, Teigen S et al. Øyeblikkeleg hjelp-døgnopphald i seks kommunar på Sunnmøre. Tidsskr Nor Legeforen 2015; 135:1553 – 7
Forfattarane svarar:
Takk for ein svært relevant merknad til vår artikkel. Dette er ei hovudproblemstilling for desse ØHD-sengene. Tilbodet skal vere eit alternativ til innlegging i sjukehus, og med minst like god kvalitet (for pasienten). Sitatet frå legen må ikkje trekkast for langt; det er faktisk diagnostisk tilbod i sengene slik vi erfarer det, og styrka legeteneste slik at fast lege er tilgjengeleg på dagtid med beredskap ettermidddag for dei fleste tilboda, og tilgang legevakt helg/natt. Men svært overvakingskrevjande pasientar, som krev hyppige legetilsyn gjennom heile døgnet, vil ikkje vere eigna for dette tilbodet. Kriteriene for innlegging i desse kommunane er at problemstillinga i hovudsak er avklart før innlegging. Vi vonar at vi i løpet av nokre få år kan ha gode data som også kan gje svar på denne svært viktige problemstillinga.