Assessing alcohol use and smoking among patients admitted to the medical ward
Smoking and harmful alcohol use cause a considerable loss of healthy life-years (1). Smoking has attracted a lot of attention, and in contacts with the health services patients are routinely inquired about their use of tobacco, frequently with subsequent advice to cut down their consumption and/or quit (2).
Harmful alcohol use is considered to be one of the main causes of poor health and the third most important cause of loss of healthy life-years (3). Annual alcohol consumption in Norway is well below the European average (7.8 litres versus 12.2 litres of pure alcohol per person per year), but it is increasing (4, 5). In addition, we can see a more liberal attitude with regard to alcohol among the country’s decision makers.
Alcohol is a contributory factor to more than 60 different known diseases (4, 6). Accidents associated with its use are additional to these. For many common diagnoses in patients in medical wards, alcohol may be a contributory factor to the hospitalisation. According to a report to the Storting, however, it remains a challenge to persuade the staff of various services to ask about and discuss the use of substances in consultations and admissions (7). In accordance with expert advice (8), the report recommends that systematic measures should be introduced to detect harmful use of alcohol and ensure that findings are followed up by further examinations, tailored counselling and referral to interdisciplinary, specialised addiction treatment, if relevant. The health enterprises are now obligated to report whether such measures have been implemented.
In this study we have also wanted to capture those who were drinking alcohol at-risk, meaning people who are at risk of developing a harmful consumption pattern (9). Such alcohol consumption is classified according to two criteria – consumption in excess of a recommended upper weekly limit or an excessively high consumption of alcohol on single occasions (termed heavy episodic drinking or binge drinking) (9).
The Nordic countries assume that a standard unit of alcohol (UA) is equivalent to 13 grams of pure alcohol. Although there are no official Norwegian guidelines, a weekly consumption of more than 14 UA for men and nine UA for women is considered at-risk drinking (9). A weekly consumption of more than 21 UA for men and 14 UA for women is denoted as harmful. People over the age of 67 years should adhere to the limits recommended for women (10).
Heavy episodic drinking is defined as ≥ 5 UA for men and ≥ 4 UA for women per drinking episode (11). This is mainly associated with alcohol-related injuries and accidents, but regularly occurring heavy drinking episodes also result in an elevated risk of a number of diseases whose onset may be delayed by many years (12). There is no specific low-risk threshold for the frequency of heavy episodic drinking (9). A recent Norwegian study showed elevated mortality in both genders and elevated cardiovascular mortality in men who are binge drinking as rarely as 1 – 4 times per month (13).
The objective of this study was first to investigate the incidence of risky alcohol use in patients admitted to medical wards and establish associated factors, and second, to determine whether there were any differences in the assessments made by health personnel of smoking and alcohol use, as well as whether alcohol users with a risky consumption level were provided with health promotion advice to the same extent as smokers.
Material and method
The study was undertaken in collaboration between four medical wards and the Addiction Unit at Sørlandet Hospital. The data collection lasted from 1 October to 20 December 2013. Patients over 18 years who had been electively or non-electively hospitalised on the medical wards on weekdays were considered for inclusion in the study. Those who were deemed too ill to be able to complete the questionnaire or undergo an interview, or were unable to understand the information provided (for example because of language problems or cognitive impairment), were excluded. In addition, some could not be included for administrative reasons (previously included or too short a hospitalisation period).
Three research nurses undertook the data collection. Once the admission interview had been undertaken and the case history had been recorded during the first-day visit to the ward, written consent was collected from the patients. They subsequently completed the questionnaire as described below. Those who were incapable of completing the questionnaire themselves were offered to complete it as an interview.
The study had been approved by the regional committee of medical and health research ethics (no. 2013/1252)
The questionnaire
The participants reported their demographic data (age, gender, residential situation, main income and education). Smoking and alcohol habits were identified with the aid of questions about the average number of daily cigarettes and alcohol consumption over the last week (number of UA). In addition, the Alcohol Use Disorder Identification Test-4 (AUDIT-4) was used, a shortened version of AUDIT (14). AUDIT-4 is scored for the last year and provides information including average consumption figures (Figure 1). A score of ≥ 7 for men and ≥ 5 for women was used as the threshold value for risky use of alcohol (14).
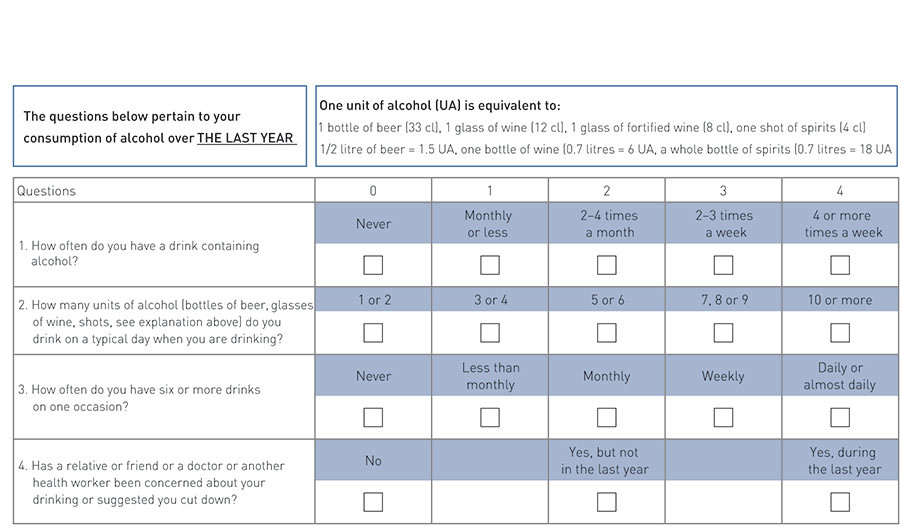
Furthermore, the patients were asked about their attitudes – «During your hospitalisation, what is your attitude to being asked about alcohol use?» – and correspondingly for smoking. Responses were given on a seven-point ordinal scale, with the extremes «I am very critical of it» (score 1) and «it’s completely OK to be asked about it» (score 7). At the end of the questionnaire, the participants were asked whether they had been questioned about smoking or alcohol use during their hospitalisation period (yes/no/don’t know – don’t remember). They were also asked whether they had been advised to cut down/quit smoking/alcohol use during their hospitalisation period (yes/no/don’t know – don’t remember).
The main diagnosis for the admission in question was retrieved from each participant’s patient records.
Definitions/coding
In this study, a risky use of alcohol was defined as an AUDIT-4 score above the threshold value and/or a weekly consumption in excess of the recommended upper limit – a consumption of > 14 UA for men and > 9 UA for women and for those ≥ 67 years is considered at-risk drinking (9, 15).
In the regression analysis (below) age was entered as a continuous variable. Education was scored on a five-point ordinal scale ranging from «not completed primary/lower secondary» to «completed > 3 years of university/university college». Residential situation was dichotomised into whether the respondent lived alone or not. Main income was not included in the regression analysis, since we knew in advance that a large proportion of the sample would be older than 67 years and no longer in the workforce. Smoking was included to reveal any co-variation with alcohol-related problems. All those who responded that they smoked ≥ 1 cigarette per day were coded as smokers.
Statistics
Differences in identification and counselling of smokers versus alcohol users were investigated with the aid of chi-square testing. Logistic regression analysis was used to determine which variables were associated with having a risky alcohol consumption. After bivariate analyses, variables that had a p-value < 0.20 were included in a multivariate logistic regression analysis using the standard method (the «enter» method) (16). The final model presents variables that are statistically significant at the 5 % level. Data were analysed using IBM SPSS, version 21.0.
Results
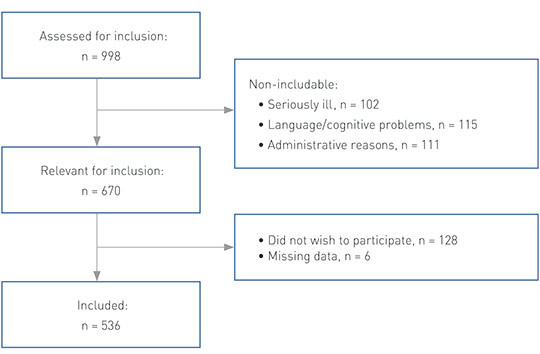
The inclusion of patients is shown in a flowchart (Figure 2). Altogether 536 patients (54 %) were included in the analysis. There were no differences between those included and those non-included in terms of gender, but the non-included were three years older on average (68 years). A description of the included patients is provided in Table 1.
Table 1
Description of included patients in four medical wards, Sørlandet Hospital, autumn 2013 (N = 536, average age 65 years)
| Variable |
Number |
(%) |
| Gender (proportion of women) |
230 |
(43) |
| Age (years), proportion ≥ 67 years |
276 |
(51) |
| Residential situation, is living alone (n = 524) |
177 |
(34) |
| Education (n = 534) |
|
|
| Not completed primary/lower secondary |
4 |
(1) |
| Completed primary/lower secondary |
107 |
(20) |
| Completed upper secondary/vocational training |
271 |
(51) |
| Completed 3-year university college |
92 |
(17) |
| Completed > 3-year university college/university |
60 |
(11) |
| Main source of income |
|
|
| Regular wages/sickness benefit |
131 |
(25) |
| Sickness benefit |
11 |
(2) |
| Social benefits from NLWA |
14 |
(3) |
| Disability pension |
86 |
(16) |
| Retirement pension |
273 |
(51) |
| Other |
21 |
(4) |
Alcohol use
Altogether 211 participants (39 %) reported not to have consumed any alcohol during the last year. Forty-seven patients (8.8 %) scored above the AUDIT-4 thresholds for risky alcohol use. Twelve of these stated on the AUDIT form that they consumed alcohol ≥ 4 times per week, and 18 reported at least one weekly drinking bout (≥ 6 UA) over the last year.
As regards the question about consumption during the week preceding admission, altogether 13 were over the threshold for risky consumption. Seven of these had a harmful level of consumption (> 21 UA), all of whom were men. Three of those who had maintained a risky consumption level over the last week were not captured by the AUDIT scoring. All in all, a total of 50 patients (9.3 %) had a risky level of alcohol consumption as defined in this study. Of these, 12 were ≥ 67 years.
Three patients had been given specifically alcohol-related diagnoses as their main diagnosis for the admission in question (F10.1 Harmful use of alcohol and K70.4 Alcoholic hepatic failure). All of them were captured by the AUDIT scoring.
A multivariate regression analysis showed that younger age, being a man and living alone were significantly associated with having a risky alcohol consumption (Table 2). In this study, there was no significant correlation between smoking and risky consumption levels. The same applied to risky alcohol consumption and education level.
Table 2
Correlations between demographic factors and risky alcohol consumption in four medical wards, Sørlandet Hospital, autumn 2013 (N = 536). Logistic regression
| Variables |
Bivariate analyses OR (95 % CI) |
P-value |
Multivariate analysis¹ OR (95 % CI) |
P-value |
| Gender (male) |
1.67 (0.90 – 3.11) |
0.105 |
3.08 (1.45 – 6.55) |
0.003 |
| Age² |
0.95 (0.94 – 0.97) |
< 0.001 |
0.96 (0.94 – 0.98) |
< 0.001 |
| Residential situation (alone) |
2.06 (1.11 – 3.83) |
0.023 |
2.60 (1.33 – 5.08) |
0.005 |
| Education³ |
0.97 (0.70 – 1.34) |
0.859 |
– |
|
| Smoking (yes) |
2.00 (1.06 – 3.78) |
0.033 |
– |
|
| [i] | ||||
[i] ¹ Variables with a p-value < 0.2 were included in a multivariate analysis. The final model presents variables that were statistically significant (p < 0.05).
² Age is included as a continuous variable.
³ Education is included as a five-point ordinal variable.
Mapping of counselling
A total of 108 patients (20 %) reported that they smoked ≥ 1 cigarette per day, while 88 (16 %) smoked ≥ 5 cigarettes on a daily basis. Altogether 332 respondents (62 %) reported to have been questioned about smoking during their hospitalisation period, while 236 (44 %) could recall having been asked about their alcohol consumption (χ² = 34.5; p < 0.001). Among those who were ≥ 67 years, altogether 42 % had been asked about their alcohol consumption, while 58 % of those who were < 67 years had been asked (χ² = 11.7; p < 0.001).
When asked to state their opinion on being asked about their alcohol and smoking habits, the proportion answering that it was completely OK to be asked about alcohol use (92 %) was equal to the proportion who found it unproblematic to be asked about smoking (93 %), meaning that they had given the most positive answers on the ordinal attitude scale. Two per cent and three per cent were critical to being asked about smoking and alcohol respectively, meaning that they scored at the lower end of the scale.
Of those 50 who had a risky alcohol consumption, there were five (10 %) who reported that they had been recommended during their hospitalisation period to cut down on their consumption or quit drinking. As regards the smokers, there were 31 (29 %) who had been recommended to quit or smoke less. In other words, those who had a risky alcohol consumption had been recommended to reduce their intake and/or quit to a lesser extent than the smokers (χ² = 6.8; p = 0.009).
Discussion
One in every ten patients reported to have a risky alcohol consumption. Male gender, young age and living alone were associated with this. Despite the fact that an overwhelming majority reported to find it completely acceptable to be questioned about their alcohol and smoking habits, the proportion that had been asked about their drinking habits (44 %) was lower than the proportion that had been asked about their smoking habits (62 %). In addition, a lower proportion of those who had a risky alcohol use had been recommended to reduce their intake and/or quit when compared to the smokers – 10 % versus 29 %.
Compared to a German study of incidence rates in medical wards, in which 20 % had an AUDIT score above the recommended threshold value, our study found a lower proportion with a risky alcohol consumption (9.3 %) (17). A mapping study of patients in Western Norway determined that 3.5 % of them had a harmful consumption of alcohol (18). This is higher than our findings (1.3 %).
The participants in the study from Western Norway, which also included patients from surgical wards, were five years younger on average (60 years). One of the reasons for the lower incidence in our study could be the relatively high average age in our sample, since the proportion that has a risky alcohol consumption is lower in older than in younger age groups (19). Nor did our study include patients who had been admitted during weekends or patients admitted only to the emergency ward. As expected, we found a higher proportion of risky consumption among men and in the younger age groups. This is known from other studies as well (18).
The proportion of alcohol users was three times higher than the proportion of smokers (61 % versus 20 %). The findings in this study nevertheless indicate that assessment of alcohol use is less frequent than assessment of smoking. In light of the fact that the use of alcohol may be directly related to the cause of admission and may have implications for prognosis development and health in general, there should be good reason to pay equally close attention to identifying alcohol use.
One can imagine a number of reasons why questions about alcohol fail to be asked – for example that health personnel consider questions about alcohol use to be more sensitive than enquiries about smoking. We could also see that patients over 67 years were asked about drinking habits less frequently than were the younger age groups. One may speculate that health personnel believe that patients above a certain age cannot have a problematic consumption of alcohol, and refrain from asking. The findings show that one in every four of those who had a risky alcohol consumption was ≥ 67 years. Patient records and recording of case histories can thus not be based on such inferences; asking the patient is in fact necessary.
The HUNT studies found that the proportion of older people (> 60 years) who had a problematic consumption of alcohol increased from HUNT2 (1995 – 97) to HUNT3 (2006 – 08). The proportion among older people in the age group 70 – 79 years increased from less than 0.5 % in HUNT2 to 4.5 % in HUNT3, and in the age group 60 – 69 years it increased from 4.4 % to 7.3 % (20). It has been estimated that the number of elderly people will increase by 50 % by 2030, meaning that the number of elderly people with a problematic consumption of alcohol will increase even if the estimates are extrapolated only on the basis of the HUNT3 findings (20).
Those who had a risky alcohol consumption received less counselling than the smokers. Others have made similar findings. A study among gynaecologists revealed a very high rate of counselling for smokers (79 %), while the counselling rate for those with a risky alcohol consumption amounted to only 36 % (21). The most relevant obstacles were stated to be that doctors had little time and also little training in providing advice about alcohol use, and they therefore coped less well with this than with providing advice about smoking (21). They also had less faith in the usefulness of providing advice on alcohol use.
One may ask whether the hectic everyday life of a somatic hospital ward provides room for giving advice and initiating measures with regard to the patients’ use of alcohol. The disease picture associated with alcohol is undeniably more complex than the disease picture for smoking, and implementing advisory services as part of standard practice has proven difficult (22, 23).
The effect of brief counselling interventions in hospital wards has been documented, however (8). Serious illness and hospitalisation can be regarded as a «window of opportunity» to motivate for change, especially if health consequences of the alcohol consumption can be identified (8). A precondition, which is also an underlying premise in this article, is that the assessment should focus on the patients’ alcohol use to the same extent as on their smoking habits. When such assessments are described in a case history, it will also be easier for the patient’s regular general practitioner to follow up this topic at a later stage (24).
Methodological assessments
The strength of the study lies in its comprehensive data material. However, there was a significant proportion that was not included (46 %). Most of these patients were defined as non-includable for administrative reasons or because they were deemed too ill to answer any questions. Altogether 13 % did not want to participate, and a selection bias can thus not be excluded. One may imagine that those who did not want to participate included a larger proportion of patients with risky alcohol consumption. If the weekend patients and those who had been admitted to the emergency ward had also been included, we cannot exclude the possibility that we might have found a higher incidence of risky alcohol consumption.
The accuracy of identification of risky alcohol consumption depends on the use of recognised tools. The short version of AUDIT used here has been validated (14) and was considered to fit well with the objective of the study. AUDIT-4 captures average consumption over the last year, and we held it to be essential to supplement this with questions on actual consumption during the week preceding admission. We cannot exclude the possibility that those who were captured with the aid of this question, but not by AUDIT, were discovered exactly because of their consumption during the week in question. The question about recent consumption addresses the here-and-now and easier to recall more precisely from memory. We believe that this could constitute an alternative approach to counselling, cf. the threshold values to risky and harmful consumption referred to above, and questions about actual consumption during the last week may thus be a supplement to AUDIT.
Whether self-reported alcohol consumption can be trusted is another matter. Estimates indicate that underreporting in questionnaire-based surveys may be close to 50 % when compared to biological markers (25). However, there are no reliable markers of a relatively low-frequency consumption (26). One therefore needs to rely on available self-reported data, while keeping in mind that these may be minimum figures (18).
The patients were asked whether they could recall having been asked about smoking and alcohol use. The responses do not necessarily reveal whether they were in fact asked – some reservations are necessary regarding the patients’ memory. However, there is little reason to assume that the patients would have forgotten questions about alcohol to a greater extent than questions about smoking, so we may assume that the comparison is valid.
Conclusion
The study shows that the suggestion in Report no. 30 to the Storting that alcohol use is insufficiently identified in somatic wards may be warranted (7). A natural measure could be to increase awareness and renew the appropriate routine of including questions about alcohol and nicotine in the regular recording of case histories.
We wish to thank research nurses Kirsti Kalleberg, Liv Kari Johnson and Lisa Vassmo Andersen, as well as the ward nurses at the Medical Department for their help with the practical implementation of the study.
MAIN MESSAGE
One in every ten patients admitted to the medical ward had a risky or harmful alcohol consumption
Patients were more frequently asked about their smoking habits than about their use of alcohol.
Only 10 % of the patients who had a risky alcohol consumption reported that they had been recommended to cut down or quit drinking alcohol during their hospitalisation period.
More than 90 % of the patients took a positive view of being asked about their smoking and alcohol habits during their hospitalisation period.
- 1.
World Health Organization. Global health risks – mortality and burden of disease attributable to selected major risks. Genève: WHO, 2011.
- 2.
Gallefoss F. Av-og-til-røyking – en helsetrussel? Tidsskr Nor Legeforen 2014; 134: 132. [PubMed]
- 3.
World Health Organization. Global Strategy to reduce the harmful use of alcohol. Genève: WHO, 2010.
- 4.
World Health Organization. Global status report on alcohol and health. Genève: WHO, 2011.
- 5.
World Health Organization. Norway – Recorded adult (15+) alcohol consumption. Genève: WHO, 2011. www.who.int/substance_abuse/publications/global_alcohol_report/profiles/nor.pdf (3.7.2013).
- 7.
Meld. St. 30 (2011 – 2012). Se meg! En helhetlig rusmiddelpolitikk. Alkohol – narkotika – doping. www.regjeringen.no/nb/dokumenter/meld-st-30 – 20112012/id686014/ (26.5.2015).
- 8.
McQueen J, Howe TE, Allan L et al. Brief interventions for heavy alcohol users admitted to general hospital wards. Cochrane Database Syst Rev 2011; 8: CD005191. [PubMed]
- 9.
Skjøtskift S. Alkohol som medvirkende faktor i noen vanlige kliniske situasjoner. Tidsskr Nor Laegeforen 2003; 123: 185 – 7. [PubMed]
- 10.
Crome I, Dar K, Janikiewicz S et al. Our invisible addict: First Report of the Older Persons’ Substance Misuse Working Group of the Royal College of Psychiatrists. London: Royal College of Psychiatrists, 2011.
- 15.
Williams EC, Palfai T, Cheng DM et al. Physical health and drinking among medical inpatients with unhealthy alcohol use: a prospective study. Alcohol Clin Exp Res 2010; 34: 1257 – 65. [PubMed]
- 16.
Altman DG. Practical statistics for medical research. London: Chapman & Hall/CRC, 1991.
- 19.
Krokstad S, Knudtsen MS. Folkehelse i endring – helseundersøkelsen i Nord-Trøndelag (HUNT). Levanger: HUNT, 2011.
- 20.
Støver M, Bratberg G, Nordfjærn T et al. Bruk av alkohol og medikamenter blant eldre (60+) i Norge. Levanger: HUNT, 2012.
- 25.
Bruusgaard D, Rutle O, Aasland OG. Alkoholproblemer i almenpraksis. Tidsskr Nor Lægeforen 1984; 104: 1431 – 5. [PubMed]