Along with the Emergency Medical Communication Centres (EMCCs) and the ambulance service, the out-of-hours primary health care system comprises the emergency medical services outside hospitals (1, 2). According to the Norwegian Index for Medical Emergencies – a decision support tool used by the EMCCs and local emergency medical communication centres (LEMCs) – the ambulance and the out-of-hours doctor must be alerted about all patients in the out-of-hours district who are assigned the acute (red) response – the highest priority of the index. The red response is assigned to patients defined as those who are in or who may quickly enter into a life-threatening state and those whose vital functions are threatened or disrupted (1, 3). Two studies have shown that the ambulance was alerted on the health radio network about almost all the red responses, while the out-of-hours doctor was only alerted in almost half the cases (4, 5). On the basis of the initial notification, it is up to the out-of-hours doctor to decide whether it is necessary to respond with a call-out. In one study the out-of-hours doctor who was notified of a red response turned out in 42 % of the cases (4). In another study the degree of involvement from the out-of-hours doctor (telephone call or call-out) was between 13 % and 50 % in different districts, although the study does not describe how often the doctor was alerted and was therefore able to reach a decision as to whether or not to respond with a call-out (6).
During the daytime the population’s need for emergency care is met by their regular GPs. Outside ordinary working hours this need is met by the out-of-hours emergency service, organised either in the municipality or as an inter-municipal collaboration. Inter-municipal collaboration reduces the workload for the duty doctors, although at the same time it leads to a greater area of coverage, more patients and longer travelling distances between the doctor and patient. In the largest urban authorities the out-of-hours service also provides emergency care during the day. Basically, participation in the out-of-hours primary healthcare system is a compulsory part of the GPs’ work: 53 % of GPs took part in this work in 2008, handling 47 % of the patient contacts at the out-of-hours services (7). The remainder of the work was performed by other doctors such as foundation doctors (with secondary on-call duty), full-time out-of hours doctors, hospital doctors and doctors employed by universities (8).
Some studies have investigated which doctors participate in out-of-hours emergency primary health care, how often they are alerted about red responses and how often they respond with a call-out (4) – (6, 9, 10). However, little is known about why out-of-hours doctors choose to turn out or not for the incidents they are alerted about. The objective of this study was to investigate the grounds for the out-of-hours doctors’ decisions about whether or not to respond with a call-out in actual situations.
Material and method
We conducted a prospective observational study with retrospective, structured interviews of out-of-hours doctors who were alerted about red responses by the Bergen EMCC during their duty shift. Eight of the out-of-hours districts covered by this communication centre were included in the study – a total of 20 local authorities with 152,340 inhabitants altogether (11). Bergen municipality was excluded because alarms are never sent to the out-of-hours emergency service in this city.
The interview period was 9 July to 24 October 2012 (108 days). After excluding weekends (Friday 16:00 to Sunday 16:00) and days with inadequate information from the Bergen EMCC, a total of 70 days were included. Weekends were excluded because the interviews were to be held within 24 hours. One out-of-hours district was included from 3 September 2012. The organisation of emergency care during the day made it difficult to trace doctors who responded to alarm calls, and even more difficult to trace doctors who did not respond with a call-out. We therefore excluded alarm calls between 07:00 and 16:00.
Those responsible for the emergency services in all the out-of-hours districts involved were contacted before the start-up of the study. They approved participation in the study and informed the LEMCs about participation. In addition, emails with information on the research project were sent to all the out-of-hours doctors and LEMCs.
The Bergen EMCC informed us daily about the number of alarm calls sent to the out-of-hours doctors included in the relevant districts. The LEMC was then contacted to obtain the telephone number of the doctor who had been on duty and had received the alarm calls. Each doctor was initially contacted by a text message that gave a brief description of the research project and invited participation. The doctors who agreed to participate were then interviewed on the phone, one interview for each alarm call, and the doctors who declined to participate were not contacted again. The time of the interview and the doctor’s name were not noted out of consideration for privacy protection.
The doctor was asked a number of questions depending on whether or not she/he had responded with a call-out. In addition, some general questions were asked. Most of the questions were worded as statements (e.g. «I always respond to alarm calls with a call-out») with response alternatives «Agree» and «Do not agree», while the rest were open questions. Based on the responses collected we created five categories. Responses that contained the words «serious/not serious» or «determined/undetermined» were grouped in the respective categories. Responses that concerned the patient’s condition or situation without including the words «serious» or «undetermined» were grouped in the «Patient» category. Non-medical explanations and need/no need for medical expertise were grouped in the category «Practical» and «Medical expertise» respectively. If the response contained more elements, it was grouped in all relevant categories.
We analysed the data using the SPSS statistics program, version 20 for Mac. The results are presented as frequencies, and statistical testing of differences in call-outs and assessments of necessity were made with the chi-square test where the statistical significance level was set at p < 0.05.
The study was approved by the Regional Ethical Committee for Medical and Health Research (2012/555/REC west) with exemption from the patient consent requirement.
Results
We received information about 280 incidents (Fig. 1). Of these, 28 incidents took place in one out-of-hours district before it was included in the study, which meant that 252 incidents were eligible for interview. We contacted 95 different doctors. Some of them had several duty shifts with alarm calls and were contacted after each shift. When there had been several alarm calls on the same shift, one interview was held for each alarm. The total number of doctors who could have been interviewed is not known since no record was taken of how many times we did not obtain contact information from the out-of-hours district. A total of 49 doctors agreed to be interviewed, and 47 were actually interviewed. Two doctors were not interviewed because too much time had passed since the duty shift or because they did not respond. A total of 72 interviews were conducted. Calculated on the basis of the number of doctors who were invited and interviewed, the response rate was 49 % (47 out of 95). A total of 280 alarm calls were made to the out-of-hours districts in the period concerned (15 hours per day) during 70 days. Based on an assumed even distribution of reported red responses during 24 hours and during the entire week, the red response rate is 15 alarm calls per 1,000 inhabitants per year.
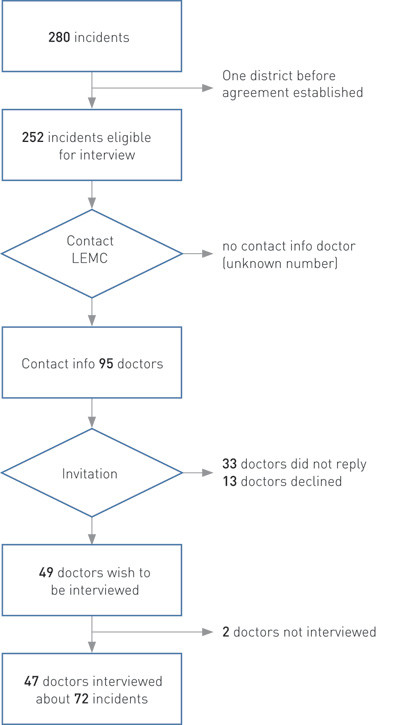
Table 1 shows that there seemed to be some variation in the call-out rate among different groups of out-of-hours doctors. Foundation doctors, locums and out-of-hours doctors with little experience (0 – 2 years) seemed to decide on a call-out more often, but the differences were not statistically significant. Doctors with little experience included 14 interns, ten locums and two GPs.
Table 1
Characteristics of the doctors interviewed¹
| Characteristics |
Number |
(%) |
Proportion responding with call-out (%) |
| Gender |
|||
| Male |
57 |
(79) |
63 |
| Female |
15 |
(21) |
73 |
| Type of doctor² |
|||
| Foundation doctor |
16 |
(22) |
75 |
| Locum |
21 |
(29) |
71 |
| GP |
36 |
(50) |
58 |
| Specialist in general medicine |
13 |
(18) |
46 |
| No. of years’ experience | |||
| 0 – 2 years |
24 |
(33) |
75 |
| 3 – 10 years |
25 |
(35) |
56 |
| > 10 years |
23 |
(32) |
65 |
| No. of out-of-hours duty shifts per month | |||
| 0 – 2 |
12 |
(17) |
42 |
| 3 – 4 |
27 |
(38) |
70 |
| 5 – 10 |
24 |
(33) |
75 |
| > 10 |
5 |
(7) |
60 |
| Short-term locums |
4 |
(6) |
50 |
| [i] | |||
[i] ¹ The same doctor may have been interviewed several times and will thus also be counted several times.
² Some doctors are included in several categories.
The out-of-hours doctor chose to respond with a call-out in 47 (65 %) of the 72 incidents. Table 2 shows what these doctors stated as the main reason for the decision. The most common responses in the «Patient» category were related to loss of consciousness, chest pains/heart disease and the fact that the patient was young. The patient’s age was never the only reason. «Practical» could be that the doctor had plenty of time, that the travelling distance was short or that the doctor «always turns out for alarm calls».
Table 2
Main reasons to decide on a call-out based on information from the initial notification. 47 situations in total. Several reasons may be given for the same situation
| Reason |
Number |
(%) |
| Patient’s condition¹ |
22 |
(47) |
| Serious condition/situation |
17 |
(36) |
| Undetermined condition/situation |
17 |
(36) |
| Practical aspects |
9 |
(19) |
| Need for medical expertise |
2 |
(4) |
| [i] | ||
[i] ¹ Responses that concerned the patient’s condition or situation without including the words «serious» or «undetermined».
In 30 (64 %) out of 47 situations, the doctors who responded with a call-out regarded the call-out as necessary afterwards. The most important reason was the patient’s need for medical expertise – for example interpreting ECG results and making a diagnosis. Practical reasons, such as saving time or avoiding delays, were mentioned more seldom. In the remaining 17 (36 %) situations where the doctor decided to respond with a call-out, the doctor was afterwards of the view that the call-out had not really been necessary. The most common grounds for this were that the patient turned out to be less ill than the initial report stated, or that her condition had stabilised in the period between the alert and the clinical assessment. Foundation doctors and doctors with little experience were more often than other doctors of the opinion that the call-out had been unnecessary, but the difference was not statistically significant.
The doctor decided not to respond with a call-out for 25 (35 %) of the 72 alarm calls. The main reasons were of a practical nature: the doctor was busy with another patient or on a call-out and the travelling distance was longer for the doctor than for the ambulance, but also that the patient would anyway have to be taken directly to hospital, that another doctor or the air ambulance responded with a call-out or that the doctor could monitor the case on the telephone. In 24 of the 25 (96 %) incidents the doctor maintained afterwards that the decision not to respond with a call-out had been correct.
Discussion
This study shows that the out-of-hours doctors interviewed responded with a call-out in two out of three of the emergency situations they were alerted about. Factors concerning the patient’s condition were the most common reason for the doctor choosing to respond with a call-out. On completion of the call-out the participation was regarded as necessary in two-thirds of the incidents, primarily due to the need for medical expertise. Among those who turned out but who afterwards did not view the call-out as necessary, this was most often related to the patient’s condition. The most important reasons for not responding with a call-out were practical aspects associated with travelling time, time constraints and the like.
The red response rate in this study was 15 alarm calls per 1,000 inhabitants per year, i.e. somewhat lower than the rate identified in other Norwegian studies which is 20 – 31 per 1,000 per year (9, 10). The calculation assumes that the proportion of alarm calls is the same throughout the 24 hours and the whole week. Previous studies have found that a few more incidents occur during the day and at weekends, so that our calculated rate is most likely an underestimate (9, 10).
Incidents that occurred during the day and at weekends are not included in the study. A total of 72 interviews were conducted for 252 relevant alarm calls. Among the doctors invited to participate, 49 % were interviewed. This, plus the fact that some doctors were interviewed several times, may have distorted the results. A frequent reason for the doctor not being interviewed was a lack of contact information, but it is presumably incidental which alarm calls this applied to. In this study the rate of responding with a call-out was 65 % higher than that found in two other studies (4, 6). In contrast to the two other studies, this study investigated rural municipalities where call-outs are traditionally more frequent compared with urban municipalities. Nonetheless we cannot exclude the possibility that doctors who responded with a call-out were more willing to be interviewed, which may cause a distortion of the results. We are of the view that the study makes a major contribution to knowledge about call-outs from out-of-hours primary health care, even though some of the findings are uncertain and cannot necessarily be transferred to all local authorities.
There was a non-significant tendency for doctors with little experience to respond with a call-out more often and to assess the call-out as unnecessary afterwards compared with doctors with more experience. This may be because doctors with little experience are not as good at assessing the information in the initial notification, or that they nonetheless decide to turn out to gain experience. It could also be the case that doctors with less experience are not as willing to be interviewed about the times they have not responded with a call-out.
When the doctor deemed it necessary to have been present, the most common reason was clearly that she/he contributed significant medical expertise. However, we cannot rule out the possibility that the ambulance staff would have been of the view that they could have handled the situation themselves. A previous study showed that ambulance staff for the most part handle diagnostic and treatment challenges, and mainly contact the out-of-hours doctor when it is a question of whether or not the patient can stay at home (6). At the same time the doctor’s presence is still important in situations where there is no standardised pre-hospital treatment procedure or where there are more complicated differential diagnostic challenges (12).
When the doctors afterwards regarded their presence as unnecessary, the most common reason was that the patient was less injured than presumed or that her condition had stabilised. It can be debated whether there are grounds to assess the doctor’s presence as unnecessary. It is not possible beforehand to predict how a situation will develop, and if a doctor waits, then it may be too late (13). Several of the doctors in our study justified their presence by the fact that they could calm down the situation. Another doctor may perhaps have assessed the same call-out as unnecessary.
The initial notification from the EMCC presumably has considerable importance for the doctor’s decision on whether or not to respond with a call-out. The quality of the notification is therefore vital, and efforts should be made to ensure that it is of good quality and contains sufficient and relevant information to provide the doctor with an appropriate platform to make a decision on a possible call-out. However, this decision is based on an overall assessment of the patient’s condition, on what is practically possible for the doctor and on what is best for the patient and the doctor’s other patients.
The article is based on a student assignment carried out during medical studies at the University of Bergen.
MAIN MESSAGE
The initial information on the patient’s condition from the Emergency Medical Communication Centre played a major role in the decision to respond with a call-out.
The main reason for assessing a call-out as necessary was the need for medical expertise at the patient’s location.
The doctor’s most important reason for not responding with a call-out was the practical aspects of the duty shift.
- 1.
FOR-2005 – 03 – 18 – 252. Forskrift om akuttmedisinske tjenester utenfor sykehus. https://lovdata.no/dokument/SF/forskrift/2005-03-18-252 (16.1.2015).
- 2.
LOV-2011 – 06 – 24 – 30. Lov om kommunale helse- og omsorgstjenester m.m. Kap. 3. https://lovdata.no/dokument/NL/lov/2011-06-24-30?q=Helse-+og+omsorgstjenesteloven (16.1.2015).
- 3.
Den norske legeforening. Norsk indeks for medisinsk nødhjelp. 3. utg. Stavanger: Laerdal Medical, 2009.
- 5.
Blinkenberg J, Jensen Å, Press K. Lege/ambulansealarm i helseradionettet – bruk, tilgjengelighet og respons. Bergen: Nasjonalt kompetansesenter for legevaktmedisin, Nasjonalt kompetansesenter for helsetjenestens kommunikasjonsberedskap, 2008. www.kokom.no/kokomsoek/publikasjonar/Rapportar/Lege_ambulansealarm_2008.pdf (16.1.2015).
- 6.
Kindt PG, Momyr M, Sundland E et al. Prehospital akuttmedisin uten legevaktlege? Tidsskr Nor Legeforen 2013; 133: 1176 – 7. [PubMed]
- 7.
Sandvik H, Hunskår S, Diaz E. Hvilke fastleger deltar i legevakt? Tidsskr Nor Legeforen 2012; 132: 2277 – 80. [PubMed]
- 8.
Sandvik H, Hunskår S. Årsstatistikk fra legevakt 2011. Rapport nr. 5/2012. Bergen: Nasjonalt kompetansesenter for legevaktmedisin, Uni Helse, Uni Research, 2012.
- 11.
Statistisk sentralbyrå. Befolkningsendringer i kommunene, 1951 – 2013. www.ssb.no/folkendrhist (20.2.2014).
- 12.
Rørtveit S, Hunskår S. Akuttmedisinsk handsaming i ein utkantkommune. Tidsskr Nor Legeforen 2009; 129: 735 – 7. [PubMed]