The goal of public health work is to promote health and to mitigate the effects of social inequalities in the population. Health surveillance is a necessary part of this work to allow prioritisation and targeted interventions (1). According to current law, municipalities must monitor their population’s health and the factors affecting it, as well as facilitate research. Ever since they were established, child health centres and the school health services have collected data of relevance to health surveillance and epidemiological research, but this information has largely been recorded as free text. For reporting, collation and analysis of data, more structured information is required (2).
Since 2008, Bergen municipality has collaborated with researchers at the Norwegian Medical Birth Registry, University of Bergen, Department of Paediatrics, Haukeland University Hospital, Bergen University College and Uni Research Health to develop the medical records system «Health Profile 0 – 20 years» (or «Health Profile»). Within this system, basic health information in electronic patient records from child health centres and the school health services, including height, weight, breastfeeding, nutrition, dental health, sleep, development/behaviour, social interaction/bonding and language, is used for statutory health surveillance and research. «Health Profile» can provide information on service provision, quality and professional development as well as the effects of interventions, and can form the basis for studies of living conditions. The system meets stringent requirements with regard to privacy and data security and was adopted in Bergen in January 2010.
Research shows that breastfeeding has health benefits for mother and child, both in the short and long term (3, 4). Exclusive breastfeeding until six months of age, as opposed to exclusive breastfeeding for 3 – 4 months followed by partial breastfeeding, can lead to fewer intestinal infections for the infant and weight loss and lactational amenorrhoea in the mother. Exclusive breastfeeding is defined as breastmilk alone during the last 24 hours, without any other liquids or solids (3). In low-income countries, it is particularly important that all infants are exclusively breastfed for six months and that breastfeeding is maintained until the infant is at least one year of age (3) – (5).
There is no evidence that exclusive breastfeeding has long-term protective effects with regard to allergy development, growth, obesity, dental health, cognitive skills or behaviour in children. In Norway, there was a goal to increase the proportion of infants exclusively breastfed at six months of age from 7 % to 20 % over the course of 2007 – 11 (6).
Recent studies suggest that children in countries such as Norway may experience health benefits from being introduced to solid foods before they are six months old, such as protection against anaemia, allergies and coeliac disease (7, 8), but this is still uncertain (9). Because breastmilk provides immunological protection, it is recommended that breastfeeding be continued after the introduction of solid foods (4, 10). The Nordic Nutrition Recommendations from 2012 advise that breastmilk should be part of the diet until 12 months of age, with partial breastfeeding thereafter for as long as suits mother and infant (9). According to the World Health Organization (WHO), breastmilk continues to be an important energy and nutrient source for children aged 6 – 23 months (5).
Previous Norwegian and Swedish studies have shown that the proportion of mothers who breastfeed is highest among those with higher education who are over 24 years of age, married/cohabiting, and who already have children. The proportion is lower among smokers and mothers of infants with low birth weight (11) – (13). The duration of maternity ward stays has decreased in recent times, and women often return home two or three days after giving birth, before breastfeeding is well established.
All forms of additional support, whether from health professionals or others (fathers, friends and parents), increase the proportion of mothers who breastfeed and the duration of breastfeeding (14). The National Competence Centre for breastfeeding at Oslo University Hospital has, in collaboration with the Norwegian Nurses Association, drawn up a set of best practices for breastfeeding guidance (15), and child health centres that work in accordance with best practice are certified as specialist breastfeeding centres.
The purpose of this study was to use «Health Profile» in combination with the Medical Birth Registry to survey breastfeeding and the factors affecting it in the infant’s first six months, including maternal age and smoking habits as well as infant birth weight. We have not come across any studies that examine potential advantages of specialist breastfeeding centres, and therefore wished to compare the course of breastfeeding in mothers attending standard health centres and those attending specialist centres.
Material and method
Sample
The study includes all infants born in the period 1 January 2010 to 31 December 2011 who were monitored by child health centres in Bergen and had consultations registered in «Health Profile» at both six weeks and six months of age. A total of 7 115 infants were born who had links to child health centres in Bergen, and data from both consultations were available for 6 093 (85.6 %).
The infants were distributed among 21 health centres. Of these, five were certified as specialist breastfeeding centres – two in 2009 (1 099 infants) and three in 2011 (385 infants). A survey of living conditions in Bergen has shown that these specialist breastfeeding centres are used by broad sections of the population. Two of them are in districts with a high prevalence of factors negatively associated with health, such as low parental educational levels and a high proportion of families with low incomes, income support and contact with the child welfare services (16).
Registration in «Health Profile»
In traditional electronic patient records for child health centres and the school health services, the topics to be addressed at each consultation are presented in a list. For each topic there is a tick box. By putting a tick in the box the public health nurse or doctor confirms that the topic has been raised, but the result itself is not stated. A «T» in the box refers to a note in a text field elsewhere in the records.
With regard to breastfeeding, notes might state «no problems with breastfeeding», «not breastfeeding», «sore nipples» etc, with text crafted by the registrant. In «Health Profile», data collection is systematic and standardised for each topic. For breastfeeding, the options are «exclusive breastfeeding», «partial breastfeeding» or «no breastfeeding». When «no breastfeeding» is selected, the registrant is prompted to record the time of breastfeeding cessation.
Variables
Data on the mother and the birth were obtained from the Medical Birth Registry, including parity, maternal age and marital status, smoking status at start and end of pregnancy, the infant’s sex, year of birth and weight and whether the infant was transferred to the paediatric unit.
«Health Profile» contained information on whether the mother still smoked (yes or no), child health centre type (standard or specialist breastfeeding centre) and the infant's age (six weeks or six months). The variables social interaction/bonding, family situation and social network, infant development/behaviour and sleep were categorised as «satisfactory» or «uncertain/abnormal». Selection of «uncertain/abnormal» led to presentation of further options to define this more closely.
Statistics
SPSS version 20 was used for chi-square tests and logistic regression. In the regression analysis, «no breastfeeding at six months of age» was used as the outcome variable. In the adjusted analysis, the above-mentioned sociodemographic and clinical variables were controlled for. Statistical significance was set at p ≤ 0.05. Results are presented as odds ratios (OR) with 95 % confidence intervals (CI).
Ethics
This study is a subproject of the research project «Prevention of health problems in infants and schoolchildren». It is approved by the Regional Ethics Committee for Western Norway and is based on the use of anonymous data without the need to obtain consent.
Results
For the 6 093 infants who attended a consultation at both six weeks and six months of age, data on breastfeeding were missing for 13 (0.2 %) at six weeks of age and for 18 at six months (0.3 %). In total, 4 485 (73.6 %) were exclusively breastfed at six weeks of age and 1 150 (18.9 %) at six months. Table 1 shows breastfeeding prevalence in relation to various background variables.
Table 1
Breastfeeding of infants aged six weeks and six months stratified by background characteristics for infants born in Bergen 2010 – 11. The percentage without recorded breastfeeding status (outcome variable) at six weeks and six months is for the most part under 1 % for all independent variables.
| 6 weeks |
6 months |
||||||||||||||||
| Exclusive breastfeeding |
Partial breastfeeding |
No breastfeeding |
Exclusive breastfeeding |
Partial breastfeeding |
No breastfeeding |
||||||||||||
| Background characteristic |
Number |
(%) |
Number |
(%) |
Number |
(%) |
Number |
(%) |
Number |
(%) |
Number |
(%) |
|||||
| Type of child health centre |
|||||||||||||||||
| Standard child health centre |
3 372 |
(73.2) |
800 |
(17.4) |
426 |
(9.2) |
784 |
(17.0) |
2 555 |
(55.4) |
1 256 |
(27.3) |
|||||
| Specialist breastfeeding centre |
1 113 |
(75.0) |
248 |
(16.7) |
121 |
(8.2) |
366 |
(24.7) |
770 |
(51.9) |
344 |
(23.2) |
|||||
| Total |
4 485 |
(73.6) |
1 048 |
(17.2) |
547 |
(9.0) |
1 150 |
(18.9) |
3 325 |
(54.6) |
1 600 |
(26.3) |
|||||
| Parity |
|||||||||||||||||
| First-time mother |
1 979 |
(70.1) |
545 |
(19.3) |
289 |
(10.2) |
486 |
(17.2) |
1 491 |
(52.8) |
835 |
(29.6) |
|||||
| 1 previous child |
1 642 |
(77.6) |
307 |
(14.5) |
163 |
(7.7) |
412 |
(19.5) |
1 196 |
(56.5) |
501 |
(23.7) |
|||||
| 2 previous children |
684 |
(78.1) |
123 |
(14.0) |
69 |
(7.9) |
196 |
(22.4) |
484 |
(55.3) |
195 |
(22.3) |
|||||
| 3 or more previous children |
180 |
(64.5) |
73 |
(26.2) |
26 |
(9.3) |
56 |
(20.1) |
154 |
(55.2) |
69 |
(24.7) |
|||||
| Parity |
|||||||||||||||||
| First-time mother |
1 979 |
(70.1) |
545 |
(19.3) |
289 |
(10.2) |
486 |
(17.2) |
1 491 |
(52.8) |
835 |
(29.6) |
|||||
| Previous births |
2 506 |
(76.6) |
503 |
(15.4) |
258 |
(7.9) |
664 |
(20.3) |
1 834 |
(56.1) |
765 |
(23.4) |
|||||
| Birth weight (g) |
|||||||||||||||||
| < 1 500 |
14 |
(36.8) |
16 |
(42.1) |
8 |
(21.1) |
5 |
(13.2) |
13 |
(34.2) |
20 |
(52.6) |
|||||
| 1 500 – 1 999 |
23 |
(41.1) |
21 |
(37.5) |
12 |
(21.4) |
5 |
(8.9) |
20 |
(35.7) |
30 |
(53.6) |
|||||
| 2 000 – 2 499 |
74 |
(43.0) |
62 |
(36.0) |
34 |
(19.8) |
21 |
(12.2) |
64 |
(37.2) |
84 |
(48.8) |
|||||
| ≥ 2 500 |
4 734 |
(75.1) |
949 |
(16.3) |
493 |
(8.5) |
1 119 |
(19.2) |
3 228 |
(55.4) |
1 466 |
(25.2) |
|||||
| Maternal age (years) |
|||||||||||||||||
| ≤ 24 |
526 |
(62.3) |
184 |
(21.8) |
132 |
(15.6) |
103 |
(12.2) |
323 |
(38.3) |
413 |
(48.9) |
|||||
| 25 – 29 |
1 402 |
(75.5) |
301 |
(16.2) |
152 |
(8.2) |
350 |
(18.8) |
1 029 |
(55.4) |
475 |
(25.6) |
|||||
| 30 – 34 |
1 631 |
(77.5) |
323 |
(15.4) |
145 |
(6.9) |
423 |
(20.1) |
1 255 |
(59.6) |
418 |
(19.9) |
|||||
| 35 – 39 |
786 |
(72.4) |
205 |
(18.9) |
91 |
(8.4) |
235 |
(21.7) |
606 |
(55.9) |
243 |
(22.4) |
|||||
| ≥ 40 |
140 |
(69.3) |
35 |
(17.3) |
27 |
(13.4) |
39 |
(19.3) |
112 |
(55.4) |
51 |
(25.2) |
|||||
| Marital status |
|||||||||||||||||
| Married/cohabiting |
4 252 |
(74.8) |
950 |
(16.7) |
469 |
(8.3) |
1 088 |
(19.1) |
3 178 |
(55.9) |
1 402 |
(24.7) |
|||||
| Other |
233 |
(56.8) |
98 |
(23.9) |
78 |
(19.0) |
62 |
(15.1) |
147 |
(35.9) |
198 |
(48.3) |
|||||
| Infant transferred to paediatric unit |
|||||||||||||||||
| No |
4 333 |
(74.8) |
954 |
(16.5) |
491 |
(8.5) |
1 099 |
(19.0) |
3 201 |
(55.3) |
1 474 |
(25.5) |
|||||
| Yes |
152 |
(50.0) |
94 |
(30.9) |
56 |
(18.4) |
51 |
(16.8) |
124 |
(40.8) |
126 |
(41.4) |
|||||
| Maternal smoking at pregnancy start¹ |
|||||||||||||||||
| No |
3 802 |
(76.1) |
818 |
(16.4) |
369 |
(7.4) |
993 |
(19.9) |
2 846 |
(57.0) |
1 143 |
(22.9) |
|||||
| Yes |
609 |
(62.0) |
203 |
(20.7) |
166 |
(16.9) |
136 |
(13.8) |
420 |
(42.7) |
424 |
(43.1) |
|||||
| Maternal smoking at pregnancy end¹ |
|||||||||||||||||
| No |
4 274 |
(75.1) |
952 |
(16.7) |
457 |
(8.0) |
1 096 |
(19.3) |
3 189 |
(56.0) |
1 394 |
(24.5) |
|||||
| Yes |
137 |
(47.9) |
69 |
(24.1) |
78 |
(27.3) |
33 |
(11.5) |
77 |
(26.9) |
173 |
(60.5) |
|||||
| Maternal smoking at 6 weeks |
|||||||||||||||||
| No |
4 374 |
(74.8) |
989 |
(16.9) |
473 |
(8.1) |
1 129 |
(19.3) |
3 263 |
(55.8) |
1 442 |
(24.7) |
|||||
| Yes |
111 |
(45.3) |
59 |
(24.1) |
74 |
(30.2) |
21 |
(8.6) |
62 |
(25.3) |
158 |
(64.5) |
|||||
| Family situation and social network |
|||||||||||||||||
| Satisfactory |
4 183 |
(74.9) |
920 |
(16.5) |
474 |
(8.5) |
1 096 |
(19.6) |
3 065 |
(54.8) |
1 422 |
(25.4) |
|||||
| Uncertain/abnormal² |
238 |
(57.9) |
113 |
(27.5) |
60 |
(14.6) |
42 |
(10.1) |
215 |
(51.8) |
157 |
(37.8) |
|||||
| Infant interaction/bonding |
|||||||||||||||||
| Satisfactory |
4 349 |
(74.1) |
993 |
(16.9) |
520 |
(8.9) |
1 140 |
(18.9) |
3 287 |
(54.6) |
1 575 |
(26.2) |
|||||
| Uncertain/abnormal³ |
129 |
(61.1) |
55 |
(26.1) |
26 |
(12.3) |
5 |
(8.6) |
30 |
(51.7) |
23 |
(39.7) |
|||||
| Infant development/behaviour at 6 weeks |
|||||||||||||||||
| Satisfactory |
3 985 |
(74.1) |
907 |
(16.9) |
475 |
(8.8) |
|||||||||||
| Uncertain/abnormal⁴ |
493 |
(69.9) |
138 |
(19.6) |
72 |
(10.2) |
|||||||||||
| Infant sleep at 6 months |
|||||||||||||||||
| Satisfactory |
883 |
(19.0) |
2 390 |
(51.3) |
1 372 |
(29.4) |
|||||||||||
| Uncertain/abnormal⁵ |
263 |
(18.5) |
930 |
(65.4) |
226 |
(15.9) |
|||||||||||
| [i] | |||||||||||||||||
[i] ¹ Data on maternal smoking habits during pregnancy are based on those mothers who consented to provide this information to the Medical Birth Registry
² Uncertain/abnormal: difficulties in relationship with family, financial or housing problems, problems related to physical environment (noise, overcrowding, interior environment), problems related to social environment, other
³ Uncertain/abnormal at 6 weeks: eye contact, «cooing», smiling, other. Six months: uncertain eye contact, no smiling, does not use voice, poor response to contact, parental concerns, other
⁴ Uncertain/abnormal: restless, frequent crying, frequently awake, limp, frequently asleep, other
⁵ Uncertain/abnormal: bedtime problems, problems with falling asleep, nocturnal awakening, other
Information on maternal smoking habits during pregnancy is based on those mothers who consented to provide these data to the Medical Birth Registry (98 %). All mothers supplied information to the child health centre about their smoking habits after the birth.
Prevalence of breastfeeding and factors that influenced breastfeeding
Fewer of the youngest and oldest mothers breastfed and breastfed exclusively. The highest frequency of breastfeeding was in the age group 30 – 34 years for 6-week-old infants and 35 – 39 years for 6-month-old infants (Table 1, Fig. 1).
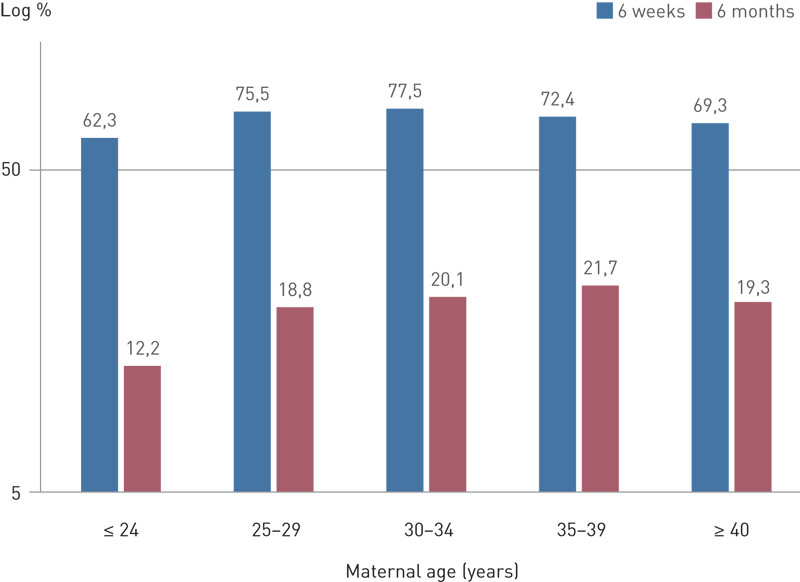
At both six weeks and six months, previous births were associated with higher rates of both partial and exclusive breastfeeding. A satisfactory family situation and social network, and cohabitation with a partner or spouse, were also associated with higher breastfeeding prevalence. Smoking during and after pregnancy was negatively associated with breastfeeding (Table 1, Fig. 2).
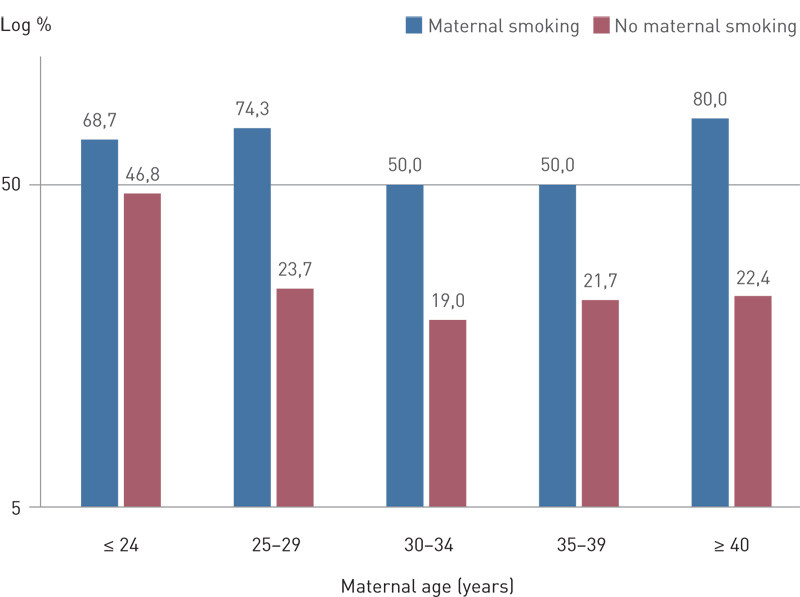
At six weeks of age, approximately 40 % of infants with birth weight under 2 500 g were exclusively breastfed, versus 75.1 % of those with birth weight over 2 500 g. By six months of age, the corresponding figures were 11 % and 19.2 % (Fig. 3). The proportion of infants who were breastfed at six months was lower among those who were transferred to the paediatric unit shortly after birth (57.6 %) than among those who were not (74.3 %). A higher proportion of infants whose sleep pattern was recorded as «uncertain/abnormal» at six months were breastfed than those whose sleep was recorded as «satisfactory» (83.9 % versus 70.3 % respectively).
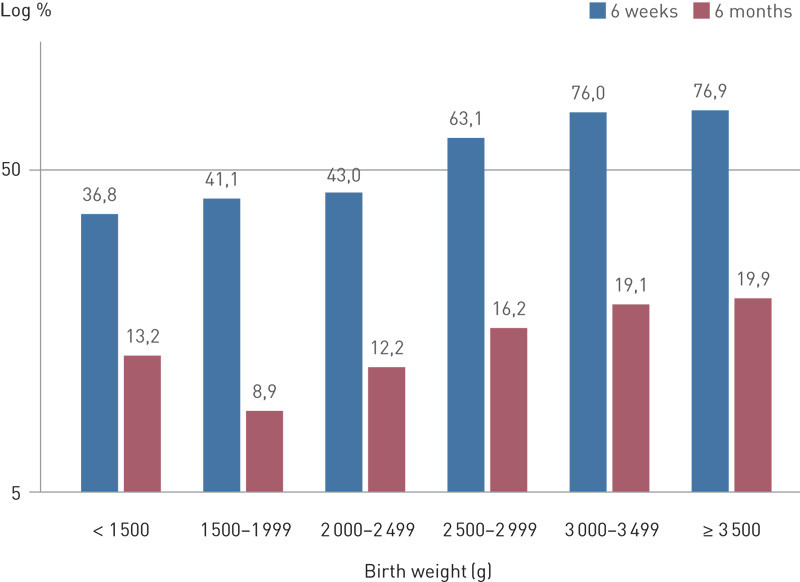
Six months after the birth, the proportion of mothers breastfeeding exclusively was higher among those with links to a specialist breastfeeding centre (24.7 %) than among those linked to a standard health centre (17.0 %). There was no significant difference between the two types of centre six weeks after the birth.
Adjusted analyses
In the adjusted analyses at six months (Table 2), the strongest predictor for absence of breastfeeding was maternal smoking (OR 3.9; 95 % CI 2.9 – 5.2). Other predictors were low birth weight, possible uncertain/abnormal infant development/behaviour, and status as a young, single mother. Links to a health centre without status as a specialist breastfeeding centre also predicted absence of breastfeeding at six months. Uncertain/abnormal sleep in the infant was associated with higher breastfeeding prevalence.
Table 2
Odds ratio (OR) for absence of breastfeeding at 6 months of age stratified by background characteristics for infants born in Bergen 2010 – 2011
| Unadjusted values (n = 6 093) |
Adjusted values (n = 6 093) |
||||
| Background characteristics |
OR |
(95 % CI) |
OR¹ |
(95 % CI) |
|
| Type of health centre |
|||||
| Standard (reference) |
1.0 |
1.0 |
|||
| Specialist breastfeeding centre |
0.8 |
(0.7 – 0.9) |
0.7 |
(0.6 – 0.9) |
|
| Parity |
|||||
| Previous births (reference) |
1.0 |
1.0 |
|||
| First-time mother |
1.4 |
(1.2 – 1.5) |
1.1 |
(0.9 – 1.2) |
|
| Birth weight (g) |
|||||
| ≥ 2 500 (reference) |
1.0 |
1.0 |
|||
| 2 000 – 2 499 |
2.8 |
(2.0 – 3.6) |
2.4 |
(1.8 – 3.4) |
|
| 1 500 – 1 999 |
3.4 |
(2.0 – 5.8) |
2.4 |
(1.3 – 4.3) |
|
| < 1 500 |
3.3 |
(1.7 – 6.3) |
2.6 |
(1.3 – 5.4) |
|
| Maternal age (years) |
|||||
| 30 – 34 (reference) |
1.0 |
1.0 |
|||
| ≤ 24 |
3.9 |
(3.3 – 4.6) |
3.2 |
(2.7 – 3.9) |
|
| 25 – 29 |
1.4 |
(1.2 – 1.6) |
1.4 |
(1.2 – 1.6) |
|
| 35 – 39 |
1.2 |
(1.0 – 1.4) |
1.2 |
(1.0 – 1.4) |
|
| ≥ 40 |
1.4 |
(1.0 – 1.9) |
1.1 |
(0.8 – 1.6) |
|
| Marital status |
|||||
| Married/cohabiting (reference) |
1.0 |
1.0 |
|||
| Other |
2.9 |
(2.3 – 3.5) |
1.8 |
(1.4 – 2.3) |
|
| Infant transferred to paediatric unit |
|||||
| No (reference) |
1.0 |
1.0 |
|||
| Yes |
2.1 |
(1.6 – 2.6) |
1.3 |
(1.0 – 1.8) |
|
| Maternal smoking at 6 weeks |
|||||
| No (reference) |
1.0 |
1.0 |
|||
| Yes |
5.5 |
(4.2 – 7.3) |
3.9 |
(2.9 – 5.2) |
|
| Family situation and social network at 6 months |
|||||
| Satisfactory (reference) |
1.0 |
1.0 |
|||
| Uncertain/abnormal |
1.8 |
(1.5 – 2.2) |
1.4 |
(1.1 – 1.8) |
|
| Infant development/behaviour at 6 weeks |
|||||
| Satisfactory (reference) |
1.0 |
1.0 |
|||
| Uncertain/abnormal |
1.2 |
(1.0 – 1.5) |
1.4 |
(1.1 – 1.6) |
|
| Infant sleep at 6 months |
|||||
| Satisfactory (reference) |
1.0 |
1.0 |
|||
| Uncertain/abnormal |
0.5 |
(0.4 – 0.5) |
0.5 |
(0.4 – 0.5) |
|
| [i] | |||||
[i] ¹ Odds ratio (OR) and 95 % confidence interval (CI) are adjusted for all variables in the table
Discussion
This study demonstrates that routine data from child health centres can be recorded in such a way as to allow evaluation of national health-related targets. The results show that the proportion of mothers in Bergen who exclusively breastfeed their infants at six months (18.6 %) is close to the Norwegian target.
Maternal smoking, age and social network, as well as infant birth weight and development/behaviour, were all related to whether and to what extent a mother breastfed. A higher prevalence of breastfeeding was recorded at the six-month consultation for mothers attending specialist breastfeeding centres.
Strengths and limitations
One of the strengths of this study is that it includes a large sample of infants and their mothers, and that it is based on data recorded continuously. Previous studies have shown that mothers report reliably on breastfeeding when data are collected close to the time (17), and that they also subsequently provide reliable information on breastfeeding duration and extent (18).
The linking of health-related data to the Medical Birth Registry is a major strength of this study. The form for reporting information to the Medical Birth Registry has been in use for many years, and the information collected is quality assured. Given that 85.6 % of eligible infants participated in the study, it is reasonable to assume that the study is representative of the population of Bergen. One of the inclusion criteria was that infants were followed up at both six weeks and six months, and the main reason for dropout was probably that families relocated.
Participation rates among this target group have been considerably lower in previous questionnaire-based studies, which may thus be at risk of selection bias. For example, the participation rate in the Norwegian Mother and Child Cohort Study (MoBa) was 42.7 % (19), and in a national study of dietary patterns in 6-month-old infants in 2006 – 2007, it was 67 % (20).
Studies from the school health services have shown that public health nurses find it straightforward to record physical health in medical records (21), but that nursing records can be affected by organisational changes (22). According to guidelines, specialist breastfeeding centres should survey the prevalence of breastfeeding and work to promote it. It is thus conceivable that child health centres that place greater emphasis on breastfeeding may tend to ask more specific questions about it, which may affect the documented prevalence.
Another strength of this study is that fully 98 % of women had indicated whether or not they smoked during pregnancy (Medical Birth Registry) and 100 % had done so upon follow-up at the child health centre after the birth («Health Profile»). The authors of the prospective cohort study «MoBa» concluded, on the basis of data from a subset of participants, that self-reported tobacco use is a valid marker for smoking (23). There is therefore reason to believe that the information in the current study is correct. One limitation of the «Health Profile» data was variability in the data-entry format for breastfeeding cessation date (for example, 3 March, 3/3, 03.03, 0303, etc). This made it difficult to calculate the exact duration of breastfeeding in the study.
Proportion who breastfeed
The Norwegian target for exclusive breastfeeding of 20 % of infants at six months of age (6) was very nearly reached in this sample. The World Health Organization’s general recommendation of six months of exclusive breastfeeding (24) is now under evaluation in Norway, as recent studies suggest that earlier introduction of solid foods may reduce the development of vitamin B12 deficiency (25), iron-deficiency anaemia, food intolerances and coeliac disease in Western countries (7, 8).
From a public health perspective, it is worth noting that the percentage who stopped breastfeeding before the infant was six months old (26 %) was higher in this study using data from child health centres, than in a previous Norwegian study (20 %) (20). In the previous study, however, participation rates were considerably lower, raising the possibility that findings were not representative of the population. On the other hand, the proportion who breastfed exclusively was higher at both six weeks and six months in our study compared with other Norwegian studies (11, 20) and studies from other countries (4, 26).
Relationship between breastfeeding and other variables
Risk factors for early cessation of breastfeeding were consistent with those in other Norwegian and Swedish studies (11) – (13). Approximately half of all mothers of infants with low birth weight had stopped breastfeeding six months after the birth. Others too have reported that fewer children with low birth weight are breastfed for extended periods (20), despite the fact that breastfeeding can be particularly beneficial for this group, both in the short and long term (4). The fact that most mothers who smoked had stopped breastfeeding six months after the birth is also consistent with previous studies (11, 13). These findings indicate that groups with the aforementioned risk factors may need special follow-up at child health centres.
For infants aged six months, breastfeeding was associated with higher prevalence of infant sleep problems. It is interesting to compare this finding with results from the large MoBa study, which showed that breastfeeding at six months was associated with nocturnal awakening but did not predict sleep problems one year later. Bed sharing was highlighted as an independent predictor of nocturnal awakening (27). It is conceivable that exclusive breastfeeding leads to more frequent awakening due to hunger as infants grow and their nutritional needs increase.
Another possible explanation is the establishment of a pattern of bedtime problems, difficulty falling asleep, awakening and maternal contact, potentially through bed sharing. It is also feasible that infants with problems being put to bed, difficulty falling asleep or nightly awakening are breastfed to help them fall asleep.
Specialist breastfeeding centres
Significantly more of the mothers who were followed up by specialist breastfeeding centres were still breastfeeding when the infant was six months old. This is consistent with studies from other countries, which show that all forms of additional support in connection with breastfeeding increase its prevalence (14). There was no significant difference at six weeks of age; this is probably due to the very high prevalence of early breastfeeding in Norway irrespective of women’s backgrounds (6, 11, 14).
The high prevalence of early breastfeeding presumably reflects the strong breastfeeding culture and generally close monitoring by maternity wards and then child health centres. It is conceivable that a health centre’s status as having breastfeeding expertise probably has greatest influence after an infant has reached six weeks of age. Fully 91 % of mothers breastfed at six weeks, and there was only a slight tendency for higher rates of breastfeeding among women who were followed up by specialist breastfeeding centres.
Public health nurses at specialist breastfeeding centres have undergone thorough training in how to record breastfeeding. It is conceivable that standard health centres may apply a more liberal definition of «exclusive breastfeeding», and that the true difference in the prevalence of exclusive breastfeeding might have been greater than documented. The specialist breastfeeding centres in this study had been certified for varying lengths of time, and this too may have contributed to the full effects of work to promote breastfeeding not being realised.
Public health work
The «Coordination Reform» emphasises the importance of prevention and early intervention, and of greater cooperation between various stages of the healthcare system (1). According to professional guidelines for the guidance of breastfeeding, child health centres should contribute to establishing a unitary chain of interventions spanning maternity/postnatal/neonatal units and child heath centres.
Specialist breastfeeding centres work to provide uniform, good quality breastfeeding guidance and to survey breastfeeding prevalence (15). This study suggests that a commitment to specialist breastfeeding centres can be beneficial for a large proportion of mothers and their children after the first six weeks of breastfeeding, and that data from child health centres can provide important information as to where efforts should be invested. From a public health perspective, it is therefore important that all Norwegian child health centres are brought up to the same standard.
The results of this study show that with electronic medical record systems such as «Health Profile», it is possible to achieve a near complete record of key healthcare targets. Such usage of data from child health centres is also in line with Norwegian strategies for health-related research and innovation (28).
In Norway, it has not previously been possible to link data from child health centres to other health registries, and information from the child healthcare services has chiefly been recorded as free text. Although this is an isolated population-based study in Bergen municipality and cannot be considered representative of the entire country, it does reveal some important associations and provides a basis for evidence-based interventions. In a survey of living conditions in Bergen in 2011, data from «Health Profile» were used to provide information about the health of the population, as a basis for plans and interventions (16).
Conclusions and implications
This study shows that single, young and first-time mothers, and those with infants of low birth weight, may require increased support and assistance should they wish and have the opportunity to breastfeed. Specialist breastfeeding centres appear to be able to increase the proportion of women who breastfeed beyond the first six weeks.
Tools such as that described here secure access to data from the entire population within the scope of standard practice and can help to identify the need for additional efforts and to evaluate interventions. The development of such medical record systems is dependent on effective collaboration between healthcare professionals with expertise in the services concerned and software providers, in order to ensure appropriate specifications. Collaboration between healthcare services and researchers with knowledge of healthcare registries is essential for development and publication, for ensuring robustness of procedures related to privacy, ethics and statistical methods, and for contributing to research of direct clinical relevance. Finally, there is great value in the knowledge contributed by staff at child health centres.
MAIN MESSAGE
The medical records system «Health Profile» provides reliable information on the proportion of infants who are breastfed and on factors related to infants, mothers and child health centres.
There was a lower prevalence and shorter duration of breastfeeding among mothers who smoked or were young, single, had an unsatisfactory family situation or social network or had an infant with low birth weight.
Specialist breastfeeding centres had a higher proportion of mothers who breastfed six months after the birth.