It is well known that substance abuse, including alcohol abuse, leads to increased risk of mortality (1, 2). In Norway, more than 650 people die each year from substance-related disorders, including 140 from alcohol-related liver disease. Many others die as a result of drug-related accidents and injuries. Around 5 200 people, one third of whom are female, are admitted to general hospitals for alcohol-related diseases annually. Many others are admitted following accidents and injuries sustained after other forms of substance abuse (3).
Responsibility for the treatment of substance abusers used to lie largely with specialist centres, but from the 1980s funds were earmarked for the treatment of substance abuse in outpatient clinics (youth mental health teams and adult substance abuse teams). From 2004, two reforms of the care provision for substance abusers were introduced in Norway. In the first reform («Rusreform I») (4), responsibility for the provision of specialist health services for substance abusers was transferred from the Social Services Act to the Specialist Health Services Act. The regional health authorities assumed responsibility for interdisciplinary specialised addiction treatment – detoxification, medical examinations and treatment programmes for substance abusers (5). With the second reform («Rusreform II») (6), the municipalities assumed responsibility for provision of social services to substance abusers.
The GP reform, which was introduced in 2002, gave all residents in Norway the right to a GP. The GP has primary responsibility for examination, treatment and referrals (7). S/he is also responsible for prescribing addictive medications and narcotics during medication-assisted rehabilitation (MAR) (8).
In Norway, there have been two studies of somatic disease in patients undergoing MAR treatment (9, 10). In both, there were considerably fewer cases of acute substance-related illness while patients were undergoing treatment compared to when they were not. A London-based study with both inpatients and outpatients, mostly heroin addicts, found that roughly three out of four had at least one somatic problem and roughly half had at least two problems (11). In 2005, a study of 315 alcoholics undergoing treatment in six European cities found that 79 % had at least one somatic problem and 59 % had at least two (12). Beyond this, to our knowledge, there has been little clinical research on the somatic health of patients in the outpatient clinics for substance abuse provided by the specialist health service.
Treatment in these outpatient clinics is often lengthy, but does not normally include investigation and treatment of somatic illness. In our experience, patients frequently complain about a lack of contact with their GPs, and referral documents often contain scant information on somatic health. We wished to examine these issues more closely.
Material and method
Enrolment
From September 2009, all new patients at the outpatient clinic for substance abuse at Levanger Hospital (hereafter «the outpatient clinic») were given the opportunity to participate in the project by their regular clinicians (psychologists, social workers, nurses and doctors). There were no exclusion criteria. The offer was made verbally and in writing, and those who wished to take part signed a consent form. Before the start of the project, a target of 150 patients was set as the number that might reasonably be expected to participate in the course of one year.
Clinicians were periodically reminded about the project and that patients must not be selected on the basis of health status. Some patients left before they were offered the chance to participate, some did not receive an offer, and others did not wish to take part. All enrolled patients were examined by one doctor (ED), the last in November 2012.
Anamnesis
Interviews with patients were used to obtain information on family history, medical history, name of GP and quality of GP-patient relationship, bodily functions, regular prescription medications and tobacco use. Substance abuse was inquired about in depth; any uncertainties were checked against information in the referral documents and, if applicable, earlier records at the outpatient clinic, and were often discussed with the patient and their regular clinician. Patients were not asked systematically about intravenous drug use.
Tobacco use was divided into «not daily use», «daily smoking of tobacco or cigarettes» and «daily use of «snus»». Occasional use of tobacco products was categorised as «not daily use».
Patients were asked «Do you have good contact with your GP?», followed by additional questions if appropriate. Contact was categorised as good, acceptable, poor or none, declined to answer or have just changed GP. Patients were informed that the results would be shared with their GP. Missing responses were therefore interpreted as poor contact.
Clinical examination and laboratory tests
The clinical examination covered general health, organ health, and reflex and sensibility testing (on the legs). With regard to general health, the following were examined: walking, skin, standardised blood pressure (measured three times on the upper arm while seated, the average of the last two measurements was used), height and weight. Laboratory tests were conducted for haemoglobin, erythrocyte sedimentation rate, electrolytes (sodium, potassium), liver function (ALT, LDH, GT), renal function (creatinine, eGFR and urine dipsticks), infections (CRP, hepatitis B and hepatitis C virus, HIV), lipids (total cholesterol, HDL cholesterol, LDL cholesterol and triglycerides), ferritin, troponin I, NT-proBPN and carbohydrate-deficient transferrin (CDT). Not all samples were analysed even though orders were placed, and some patients did not attend for a re-test.
All patients were offered a referral for echocardiography at the cardiac outpatient clinic.
Diagnoses
The patient-reported medical history and clinical examination were central to all diagnoses, and many disease diagnoses (ICPC2 70 – 99) were made solely on the basis of these, including dental disease, overweight/morbid obesity, refractive errors of the eye, hypertension and peripheral neuropathies. Others were made on the basis of additional information about chronic diseases in hospital records or from the GP, or information about medication use for illness or the results of laboratory pathology tests. Symptom diagnoses (ICPC2 1 – 29) were made where the patient's complaints could not be objectively verified (13, 14). Disease diagnoses from other hospitals or from the radiology department were not included for practical reasons.
Some patients wished to be referred directly to hospital specialists for further investigation and treatment, and these wishes were fulfilled. Others were either referred directly to a specialist to save time, were started on treatment during the examination or were referred directly to the welfare services to enquire about free dental treatment. GPs were asked to follow up the vast majority of these patients.
Somatic information in referral documents and GP responses
For all patients enrolled, information on somatic health in the referral documents to the outpatient clinic was examined, compared with information from the patient-reported medical history and categorised as good, incomplete or none.
When the patient was given an appointment for examination, their GP received a letter asking them to answer questions to provide additional information on the patient’s somatic health. This information was also categorised as above.
Structured questionnaire
Two structured questionnaires were used: the somatic part of the EuropASI (15) and the EQ-5D (Health-related quality of life) (16, 17). EuropASI contains 12 questions on somatic health, including number of hospital admissions, chronic injuries and diseases with an impact on lifestyle, dental health, hepatitis and HIV, regular medication use, medical assistance and/or welfare support in the last six months because of injury or physical illness, and number of days with somatic health problems within the last 30 days.
EQ-5D has two parts: one contains questions about daily problems (difficulties with walking, personal care, everyday activities, pain/discomfort and anxiety/depression); the other consists of a scale from 0 to 100 on health status today.
The questionnaires were completed either together with the regular clinician or during the examination. Responses to the structured questionnaires were not sent to GPs.
Ethical assessment
The study was approved by the Norwegian Regional Committee for Medical and Health Research Ethics, the Norwegian Social Science Data Services and the Biobank registry. Written consent was obtained from patients. Enrolled patients were informed both verbally and in writing of the possibility to withdraw from the study at any time without compromising their treatment.
The study is registered at ClinicalTrials.gov. Unfortunately, this was done after commencement of the study (4 March 2010) as we were unaware of the registration requirement when the study was initiated.
Results
Altogether 365 patients started treatment for substance abuse during the study period. A total of 189 patients expressed a wish to participate in the study, but 34 of these failed to attend appointments despite repeated invitations. In all, 155 (42 %) attended for examination (Fig. 1, Table 1), and none of these later withdrew. A total of 176 patients were either not invited to participate or declined. Clinicians still working at the outpatient clinic revealed that 69 of these patients had not been invited whereas 44 did not wish to take part. Six clinicians left during the study period, thus we do not have corresponding information for the remaining 63 patients.
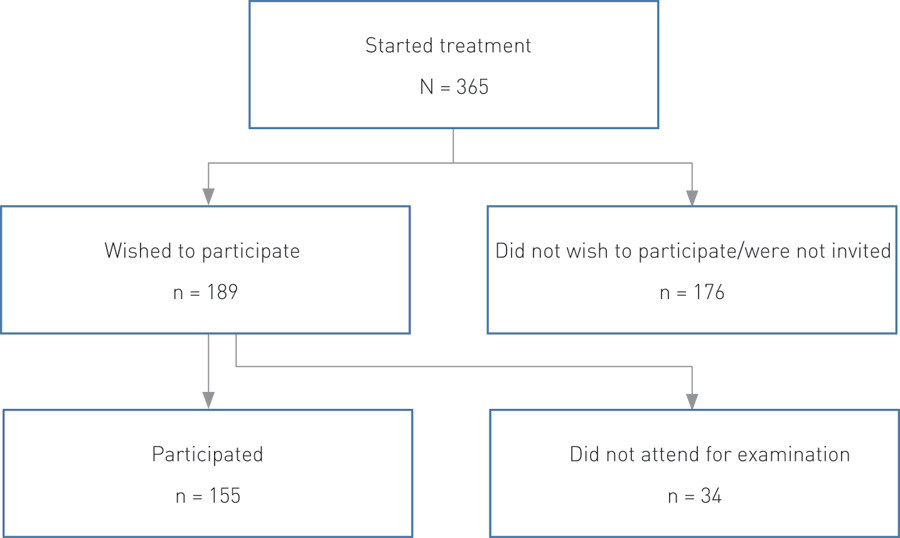
Table 1
Age and sex of patients who started treatment at the outpatient clinic for substance abuse at Levanger Hospital in the period September 2009–November 2012, and of patients enrolled in the study
| Started treatment (N = 365) Number (%) |
Enrolled in study (n = 155) Number (%) |
||||
| Age group (years) |
Male |
Female |
Male |
Female |
|
| < 20 |
15 (6) |
16 (17) |
6 (5) |
5 (14) |
|
| 20 – 29 |
73 (27) |
19 (20) |
22 (19) |
7 (19) |
|
| 30 – 39 |
64 (24) |
13 (13) |
21 (18) |
7 (19) |
|
| 40 – 49 |
57 (21) |
24 (25) |
31 (26) |
8 (22) |
|
| 50 – 59 |
43 (16) |
18 (19) |
26 (22) |
4 (11) |
|
| 60 + |
16 (6) |
7 (7) |
13 (11) |
5 (14) |
|
| Total |
268 (73) |
97 (27) |
119 (77) |
36 (23) |
|
A total of 151 patients attended for blood sampling. For four of these, certain samples were not analysed for various reasons. In all, 220 patients (60 %) who were undergoing treatment at the outpatient clinic, and 109 (70 %) of those included in the study, were referred by their GPs (Table 2).
Table 2
Referral source for patients who started treatment at the outpatient clinic for substance abuse at Levanger Hospital in the period September 2009–November 2012 and for patients enrolled in the study
| Referral source |
Started treatment (N = 365) Per cent |
Enrolled in study (n = 155) Per cent |
| GP |
60 |
70 |
| Psychiatric services |
21 |
14 |
| Welfare services |
9 |
6 |
| Addiction treatment centre |
6 |
5 |
| Somatic medicine |
4 |
5 |
Use of drugs and tobacco
Alcohol was the most commonly used drug (Table 3). Eighty-four patients (54 %) reported that they used only one drug, and 79 of these used alcohol. Of the 71 patients who used two or more drugs, 49 stated that alcohol was one of them; i.e. 128 patients (83 %) reported use of alcohol as either their only drug or as one of multiple drugs. In all, 57 patients used opioids, amphetamines or a mixture of different substances, while 50 patients used cannabinoids alone or in addition to other substances. A number of patients reported use of other drugs sporadically or for short periods, but this usage was excluded.
Table 3
Preferred intoxicant (primary drug) by sex for 155 patients enrolled at the outpatient clinic for substance abuse at Levanger Hospital in the period September 2009 – November 2012
| Drug |
Male (n = 119) Per cent |
Female (n = 36) Per cent |
| Alcohol |
71 |
67 |
| Cannabinoids |
10 |
11 |
| Stimulants |
10 |
11 |
| Opioids |
8 |
3 |
| Benzodiazepines and similar |
1 |
8 |
A total of 128 patients (83 %) reported daily use of tobacco, 107 (69 %) in the form of cigarettes/smoking tobacco and 21 (14 %) in the form of snus. Three of the women (8 %) and 24 of the men (20 %) stated that they did not use tobacco daily.
Diagnoses
An average of 4.2 somatic disease diagnoses were made per patient, with a range from 0 to 12 (Table 4). Four patients stated that they were in good health and this was confirmed by examination. Among the others, the highest disease prevalence was within the digestive system with a total of 118 diagnoses, of which 69 were dental disease, and endocrine/metabolic diseases, also with 118 diagnoses, of which 53 patients were overweight, 37 had morbid obesity and nine had diabetes. We detected hypertension in 56 patients, heart disease (not further specified) in ten, allergy/urticaria in 45, COPD/asthma in 20, and reduced vision/refractive errors in 45 patients. There were an average of 0.8 symptom diagnoses per patient, the majority within the musculoskeletal system.
Table 4
Distribution of ICPC diagnoses in 155 patients at the outpatient clinic for substance abuse at Levanger Hospital in the period September 2009–November 2012. Diagnoses were made on the basis of the patient-reported medical history, clinical examination, medication use, laboratory tests and/or GP/medical records
| ICPC diagnoses |
Number of symptom diagnoses (diagnoses 1 – 29) |
Number of disease diagnoses (diagnoses 70 – 99) |
| Digestive system |
23 |
118 |
| Endocrine, metabolic, nutritional conditions |
0 |
118 |
| Cardiovascular system |
5 |
89 |
| Respiratory system |
5 |
76 |
| Musculoskeletal system |
55 |
65 |
| Eye |
5 |
63 |
| Nervous system |
10 |
39 |
| Ear |
8 |
38 |
| Skin |
7 |
36 |
| Urinary tract and genitalia |
6 |
6 |
| General and unspecified |
1 |
2 |
| Blood |
1 |
1 |
| Total |
121 |
648 |
In all, 384 (59 %) disease diagnoses were made on the basis of the patient-reported medical history and clinical examination alone. Dental disease, refractive errors of the eye, hypertension and overweight/morbid obesity accounted for 238 of these (62 %). A further 157 diagnoses (24 %) were made on the basis of information from somatic case records, 46 (7 %) on the basis of medication use, and 36 (6 %) using information from GPs in addition to the patient-reported medical history and clinical examination.
A total of 147 patients were tested for hepatitis B and hepatitis C. None was infectious for hepatitis B, while 11 patients had antibodies after previous illness or immunisation. Eight patients were infectious for hepatitis C (positive for viral RNA in blood), while one had uncertain infection status. In addition to these nine, a further six patients had hepatitis C antibodies in their blood. Seven patients reported in EuropASI that they were hepatitis C positive, but tests showed that they were negative. Two patients were unknowingly positive. Patients were not systematically asked about intravenous drug use. A total of 144 patients were tested for HIV and found to be negative.
Echocardiography was performed in 107 patients by the same cardiologist. Normal functioning of the ventricles and valves was seen in 75 (71 %). Decreased systolic function of the left ventricle with ejection fraction ≤ 45 % was found in six patients; decreased diastolic function was detected in 14 but only two had more than grade 1 dysfunction. Valve leakage was seen in nine patients and valve stenosis in one, but all valve disease was mild. Other pathology of the heart or thoracic aorta was seen in five patients. Previously diagnosed heart disease was confirmed with echocardiography in 22 patients (21 %), and abnormalities were detected in the absence of previously established heart disease in ten (9 %).
Five patients were referred directly to the department of general medicine, six to the surgical department and 26 to other hospital specialists. Fifty-one patients were referred to the welfare services to enquire about their entitlement to free dental care.
Somatic information in referral documents and GP responses
We found good quality information on somatic health in the referral documents for 27 patients (21 from GPs, three from departments of general medicine, two from the psychiatric services and one from an addiction treatment centre), incomplete information for 27, and no such information for 101 patients.
We received responses from the GPs of 60 patients, with good quality information on 46; for 34 of these, the referral documents contained incomplete or no information on somatic health. In all, somatic health information was absent or incomplete for 94 patients (61 %).
GP contact
Ninety-two patients (59 %) reported that they had good or acceptable contact with their GP, 19 (12 %) had little contact, 19 (12 %) declined to say, 15 (10 %) stated that they had no contact and ten (6 %) had just changed GP.
Patients who did not have contact with their GP received a total of 52 disease diagnoses and 12 symptom diagnoses.
Structured questionnaires
EuropASI was completed by 150 patients. Fifty-five (37 %) stated that they been hospitalised because of physical illness in the last two years, 64 (43 %) reported chronic injuries or diseases that affected their lifestyle, and 62 (41 %) had been to see their GP because of physical ailments. Twenty-seven patients with chronic ailments had not seen their GP in the last six months, while 60 patients (40 %) received welfare payments because of such conditions. Seventy-one patients (47 %) reported that their GP asked them to take regular medication because of somatic injury or illness, while 42 (28 %) had experienced physical problems for at least 25 of the last 30 days; 19 of these had not been in contact with a doctor.
Altogether 146 patients completed the Health-related quality of life questionnaire. Of these, 36 (25 %) reported slight problems with walking, 71 (49 %) with everyday activities (work, studies, housework, family activities etc), 99 (68 %) had some pain/discomfort, and 88 (60 %) had problems with anxiety/depression.On a scale from 0 to 100, the average score for self-reported health was 60.
Discussion
The patients in this dataset had an average of 4.2 disease diagnoses and 0.8 symptom diagnoses. Many had disease in multiple organ systems or multiple diseases in each organ system. Substance abuse, smoking and many of these diagnoses are all significantly associated with reduced health and longevity. The patients in this study seem to have more somatic morbidity than those in two previous studies (11, 12).
The current study did not include a control group. A literature search was therefore conducted to identify findings from previous studies. The proportion of patients with asthma/COPD is 50 % higher in this dataset than in the HUNT 3 dataset (18). A study from Nord-Trøndelag county (19), which performed echocardiography in 1296 individuals (mean age 49 years), found that 30 (2.3 %) had cardiovascular disease that could affect heart function. The frequency of pathology appears to be considerably higher in the current study.
The self-reported health complaints (structured questionnaires) show that many patients put up with diseases, ailments and chronic pain without contacting their GP. In the HUNT 3 study, 83 % of participants said they had consulted their GP in the last year (18), while 62 patients (41 %) in our dataset had contacted their GP because of physical ailments in the last six months.
Eighty-three per cent of our patients used tobacco or snus daily, while in the Nord-Trøndelag Health Study (HUNT 3, 2006 – 08), 16 – 25 % were daily smokers or snus users, with the proportion increasing slightly with age (18).
Twelve per cent of patients stated directly that they had little contact with their GP. A large proportion of those who either declined to answer, had no contact with their GP or who had just changed GP also indicated that they had little contact, but did not want this to be recorded.
Several user surveys have shown a high degree of satisfaction with the GP scheme (20). The substance abusers in this study do not seem to be equally satisfied. There may be several reasons for this, including frequent changes of GP, limited ability to pay fees, poor attendance of appointments, complex presentations that require extensive time to investigate, restriction of access to habit-forming substances by the GP, and fear of stigmatisation.
A number of GPs see substance abusers as troublesome – associating them with disturbances in the waiting room, attendance outside of scheduled appointments and poor compliance with treatment programmes. Before implementation of the GP scheme, and again in 2013, doubts were raised about whether the GP scheme was truly the best option for substance abusers (21, 22). However, from our data we cannot say how many of the patients' illnesses and ailments their GPs were aware of.
Strengths and limitations of the study
One of the strengths of this study is that data on enrolled patients were obtained from multiple sources: the patient-reported medical history, clinical examination, additional examinations, review of somatic hospital records, information from GPs upon referral and/or supplementary information, and structured questionnaires. The fact that examinations were performed by a single doctor was also an advantage as it meant that diagnoses were consistent.
Caution is required with regard to generalising these findings given that only 42 % of patients identified actually took part. Any diagnoses made by the radiology department or other hospitals were not included among the disease diagnoses for practical reasons. This might have led to the proportion of symptom diagnoses being somewhat higher and that of disease diagnoses somewhat lower than in reality. Diagnoses were mostly made in accordance with ICPC2 but were not confirmed with follow-up studies. Follow-up of patients was entrusted to GPs. Chronic diagnoses made by the hospital or by GPs were discussed and assessed during the patient-reported medical history and clinical examination.
Patients were not asked systematically about intravenous drug use, but the low prevalence of hepatitis C suggests that it was not widespread in this cohort.
Interpretation
Treatment can be lengthy at outpatient clinics for substance abuse – it can often last for many months or perhaps several years, and occurs largely in the absence of somatic health information on patients and without them undergoing either a physical examination or treatment.
Given that patients in this study have multiple somatic diagnoses on average, while a number report little or no contact with their GP, we believe there is reason to question whether the requirements of the specialist health service and the primary health service are being met regarding the provision of adequate health care for this patient group.
Registration number in clinicaltrials.gov: NCT01081197
MAIN MESSAGE
Substance abusers in our study had onaverage more than four somatic diagnoses
12 % stated directly that they had little contact with their GP
It is possible that outpatient clinics for substance abuse are not fulfilling the requirements of the specialist health service in terms of adequate healthcare provision for their patients