Patients with personality disorders constitute a large proportion of patients treated by the psychiatric specialist health service (1). Psychosocial treatment, including psychotherapy, is the primary treatment for personality disorder, and patients with moderate and severe personality disorders present the greatest challenge with regard to therapy. They have a low functional level, complex problems and need help in many areas of life. They tend to be young adults with a broad range of symptoms, self-destructive behaviour, relational problems and difficulty in functioning in studies and work.
A number of international studies, including Norwegian ones, have demonstrated that many patients with personality disorders benefit from outpatient individual psychotherapy (2, 3). Such studies have mostly investigated treatment offered by public outpatient departments or university clinics. Specialists in private practice with a contract with the regional health authorities are an important part of the overall services offered by the psychiatric specialist health service, but we do not know enough about the treatment of patients with more severe personality pathology in such private specialist practice.
The Ullevål Personality Project (UPP) is a randomised study investigating the efficacy of a specialised hospital-based treatment programme for patients with moderate and severe personality disorders compared with outpatient individual therapy.
There were no differences in outcome between the treatment groups after eight and 18 months. After three years the group that had been referred for outpatient individual therapy had a significantly higher level of psychosocial functioning, while after six years there were once again no significant differences between the groups (4, 5). There was considerable improvement in both groups.
This was an unexpected finding, as the original hypothesis was that the hospital-based programme would yield the greatest clinical change. 85 % of the patients who were randomised to outpatient individual therapy were referred to specialists in private practice. The findings aroused curiosity regarding how the private practitioners and patients experienced this treatment.
In this study, we focus on treatment provided in private practice up to the three-year follow-up. The aim is to describe the characteristic features of the therapy, the therapists’ experiences and the patients’ satisfaction with the therapy.
Material and method
The Ullevål Personality Project is a prospective longitudinal study conducted by the Section for Personality Psychiatry, Oslo University Hospital. The study was approved by the Regional Committee of Medical Research Ethics and by the Norwegian Data Protection Authority.
Prior to therapy, all patients underwent an evaluation carried out by the department’s clinical staff, including structured diagnostic interviews and self-reported symptoms (4). Psychosocial functioning was measured using the observer-based instrument Global Assessment of Functioning (GAF) (6) on the basis of an interview that was designed for the project.
After three years, the patients took part in a follow-up evaluation conducted by a research assistant. GAF assessments were performed blinded for treatment condition. The reliability of diagnoses and GAF scoring were found to be satisfactory (4). At the three-year follow-up, the patients answered a question regarding how satisfied they were with the therapy. The responses were graded on a scale from 1 (very dissatisfied) to 5 (very satisfied). Information about other treatment in the three-year period is based on patient interviews at three follow-up investigations (8 months: n = 40; 18 months: n = 32; 3 years: n = 31).
Recruitment of specialists in private practice
The specialists were recruited by means of a written enquiry to all psychiatrists and psychologists with a contract for practice in Oslo in 2003/2004. They were asked whether they would like to take part in a randomised treatment study and could choose themselves whether they wanted to be therapists in the hospital-based treatment programme or participate as therapists for patients randomised to outpatient individual therapy.
The private practitioners who took part in the outpatient treatment described here were instructed to treat the patients in the way they would normally do, whether they were taking part in the project or not. They were not given instructions about the length, frequency of appointments or contents of the treatment. The therapists could also use their clinical judgement to refer patients to another type of therapy if they considered it desirable. The reason was that the treatment was supposed to reflect the usual treatment given in a private specialist practice, rather than a special type of psychotherapy, and as such represent a realistic alternative to the hospital-based treatment programme.
Procedures
The private practitioners stated how many project patients they wanted and when they could receive a patient. After randomisation, they were allocated patients according to a list, with instructions to contact the patients themselves. The therapists were sent the results of the patients’ assessment by the department. The patients, for their part, were given the name of the therapist to whom they had been allocated.
On inclusion in the project, the specialists filled in a questionnaire about their training and experience and degree of satisfaction in their work as psychotherapists. When patients ended their treatment, the therapist completed a form about the duration and frequency of the treatment, reason for termination, complications and how the therapist concerned had themselves experienced the therapy. For those patients who had not ended the therapy at the time of the three-year follow-up, the therapists completed a preliminary treatment form.
Two therapists, treating three patients in all did not submit the termination form. One of them was deceased, the other could not be traced.
The specialists in private practice
The study included 26 specialists (Table 1). They had many years of experience as psychotherapists and reported a high degree of satisfaction with their work. On a scale from 0 (not at all) to 5 (very much), the median score on the question of satisfaction was 4 (range 3 – 5). The therapists treated 1 – 3 project patients each.
Table 1
Characteristics of specialists in private practice (n = 26). Median (range) unless otherwise specified
| Male therapists (n) |
20 |
|
| Age (years) |
58 |
(47 – 66) |
| Psychiatrists (n) |
15 |
|
| Psychologists (n) |
11 |
|
| Psychotherapeutic training (n) |
||
| Norwegian Psychoanalytical Institute |
4 |
|
| Institute for Psychotherapy |
17 |
|
| Norwegian Institute for Vegetotherapy |
6 |
|
| Institute for Group Analysis (Norway) |
10 |
|
| Specialist training in cognitive therapy |
0 |
|
| Specialist training in family therapy |
8 |
|
| Other |
13 |
|
| No. of years training in individual psychodynamic therapy |
4 |
(1 – 12) |
| No. of years training in group analysis |
5 |
(1 – 6) |
| No. of years training in family therapy |
2 |
(1 – 5) |
| Degree of influence from various theoretical directions in work as therapist (scale 0 – 5) |
||
| Analytical/psychodynamic |
4 |
(2 – 5) |
| Cognitive |
3 |
(1 – 5) |
| Behavioural therapy |
2 |
(0 – 3) |
| No. of years working as psychotherapist |
24 |
(8 – 30) |
| Satisfaction in work as psychotherapist (scale 0 – 5) |
4 |
(3 – 5) |
The patient population
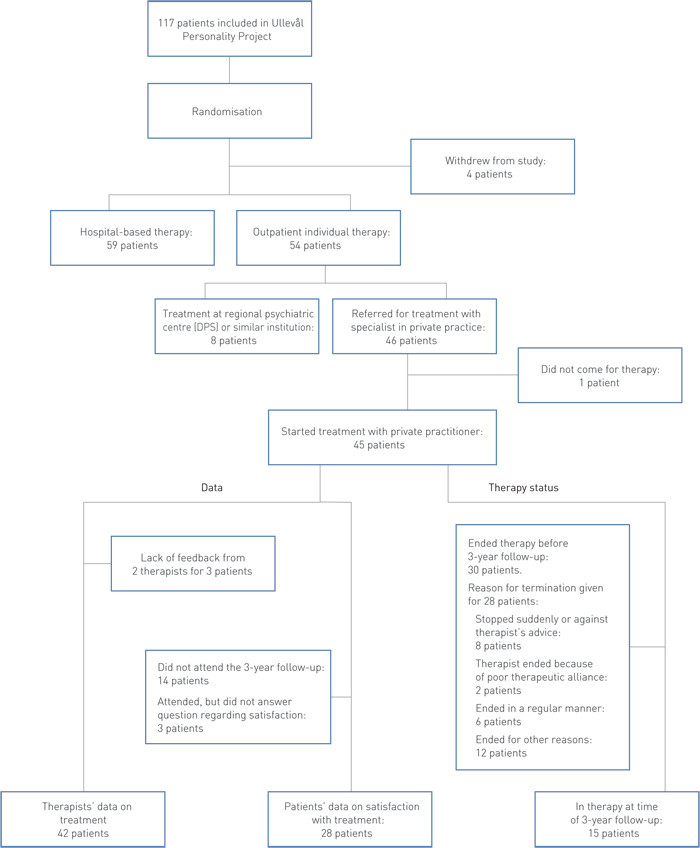
A total of 46 patients were referred to specialists in private practice. Referral to a private practitioner as compared to a therapist at a regional psychiatric centre (DPS) or similar institutions was random (Fig. 1). One patient did not come for therapy and was excluded from the analyses. 31 patients (69 %) took part in the follow-up investigation after three years.
There were no significant differences between those who did not take part and those who took part in the three-year follow-up with respect to sociodemographic characteristics, diagnoses, initial symptom severity or work function, but those who did not participate had a significantly lower GAF score prior to the treatment (mean 45.9 (SD = 3.6), compared with mean 49.3 (SD = 5.0), p = 0.029). The median age at the start of treatment was 29 (range 20 – 53). 31 per cent were women.
The most commonly occurring types of personality disorder were borderline (19 patients), avoidant (17 patients), paranoid (6 patients) and unspecified personality disorder (11 patients). In addition they had depressive disorders (40 patients), anxiety disorders (37 patients) and alcohol or substance abuse (15 patients). In the year preceding inclusion in the trial, 11 of the patients had engaged in self-harm, 38 had had suicidal thoughts and six had attempted suicide.
The median age at the time of the first contact with the health service owing to mental problems was 21 (range 2 – 45 years). 20 patients had had psychotherapy previously and 17 had been inpatients in psychiatric departments. Of the 42 who answered the question about work, 18 stated that they had neither studied nor worked in the year prior to the study. These are thus patients with long-term, complex problems and considerably impaired work function.
Statistical analyses
Figures for frequencies, mean, median and range are given. The relationship between dichotomous variables was tested using chi-squared tests. Relationships between continuous and dichotomous variables were tested with independent t-tests or Mann-Whitney tests, while correlations between continuous variables were measured using Spearman's rho. The numbers in the analyses vary slightly because of missing data.
Results
The psychotherapy and the therapists’ experiences
The most common frequency of therapy sessions was once a week (Table 2). After a while, some of the therapists started to see the patient less frequently, for example every second week, or at intervals of a few months. The median number of therapy sessions at the three-year follow-up was 43 (range 2 – 258 hours). Eight patients had had less than ten sessions, while ten had had more than 80 sessions. 30 of the in all 45 patients had ended their therapy before the three-year follow-up (Fig. 1).
Table 2
Amount of treatment and the specialists’ experience of the treatment (data from 42 submitted therapist forms). Median (range) unless otherwise specified
| No. of therapy sessions in the 3-year period |
43 |
(2 – 258) |
| Patients with less than 10 sessions (n) |
8 |
|
| Patients with more than 80 sessions (n) |
10 |
|
| Frequency of sessions, most typical for the therapy (n) |
||
| More than 1 session per week |
6 |
|
| 1 session per week |
24 |
|
| Less than 1 session per week |
12 |
|
| Therapist's focus in the treatment (scale 0 – 5) |
||
| Self-insight |
3 |
(0 – 5) |
| Support/stabilisation |
4 |
(0 – 5) |
| Problem solving |
4 |
(0 – 5) |
| Therapist’s experience of the treatment (scale 0 – 5) |
||
| Interesting and professionally stimulating |
3 |
(0 – 5) |
| Good therapeutic alliance on the part of patient |
3 |
(0 – 5) |
| Demanding because of serious concern about patient's acting-out behaviour |
2 |
(0 – 5) |
| Demanding because of serious concern about risk of suicide |
1 |
(0 – 5) |
| Demanding because of strong need for cooperation with other institutions |
0 |
(0 – 5) |
| The therapy was complicated by |
||
| Frequent calls from the patient outside the therapy appointments (n) |
2 |
|
| The patient arrived for appointments under the influence of alcohol/drugs/ medication (n) |
4 |
|
| Admission to psychiatric acute department because of risk of suicide (n) |
4 |
|
| The patient became psychotic (n) |
1 |
|
| Other (n) |
21 |
|
| The patient's no-shows or cancellations were a serious problem for the stability of the therapy (n) |
11 |
|
| No. of patients where the therapist found to some extent that the therapy was difficult to combine with private practice because of |
||
| Financial loss due to cancellation of appointments (n) |
12 |
|
| Strong need for cooperation with other institutions (n) |
5 |
The therapists generally found the therapies interesting and professionally stimulating, and a moderately good therapeutic alliance was reported for the group as a whole (Table 2). They reported some concern in connection with acting-out behaviour and suicidality.
There were few complications in the form of telephone calls outside of appointments, patients arriving for appointments under the influence of substances or hospitalisation because of the risk of suicide, but the therapists reported other types of complications for half of the patients. The factors that most frequently complicated therapy were irregular attendance, the patients’ poor functioning, acting-out behaviour, substance abuse or severe mental symptoms. For approximately a quarter of the patients, failure to attend or cancellation of appointments was a problem for treatment stability.
The patients’ satisfaction with the treatment
Of the 28 patients who responded to the question on satisfaction with the treatment, ten were still in therapy while 18 had ended the therapy. The reason for termination was reported for 16 of these patients: four had dropped out, two treatments had been terminated by the therapist because of poor alliance, five patients had ended therapy in a regular way and five had ended it for other reasons.
There were no significant differences in initial function level or symptom severity among the 28 who had answered the question on satisfaction and the remainder of the patient population. 20 patients (71 %) reported that they were moderately to very satisfied with the therapy offered while eight (29 %) were dissatisfied or very dissatisfied.
There were no significant correlations between degree of satisfaction and sociodemographic characteristics, psychosocial functioning or symptom severity before therapy start, nor with type of personality disorder or type of symptom disorder. There was one exception: Patients with a diagnosis of substance abuse (alcohol or drugs) at the start of treatment (8 of 28 patients) were significantly less satisfied than patients without substance abuse (average 2.5 (SD = 0.5) compared with 3.6 (SD = 1.4), p = 0.025, on a scale from 1 (very dissatisfied) to 5 (very satisfied).
The patients’ satisfaction did not correlate with the therapists’ theoretical orientation or focus on self-insight, support/stabilisation or problem solution. There were, however, negative correlations between patient satisfaction and the therapist’s experience of the treatment as demanding because of serious concern about the patient’s acting-out behaviour (rho = – 0.56, p = 0.003), serious concern about risk of suicide (rho = – 0.51, p = 0.01), a major need for cooperation with other health or social services (rho = – 0.45, p = 0.026) and the fact that no-shows/cancellations represented a problem for therapy stability (rho = – 0.47, p = 0.018).
On the other hand, there was a positive correlation between patient satisfaction and the therapist’s sense of a good therapeutic alliance on the part of the patient (rho = 0.58, p = 0.003) and between satisfaction and improvement in the GAF score during the three-year period (rho = 0.56, p = 0.002). Even after excluding from the analysis one patient with an unusually high number of sessions (258), there was a significant positive correlation between patient satisfaction and number of therapy sessions (rho = 0.57, p = 0.004).
Other treatment
Six patients had been admitted 1 – 3 times to psychiatric inpatient departments, two had stays with overnighting at a regional psychiatric centre, six had been to the psychiatric emergency ward and six had been referred to a day hospital department other than that at Ullevål. At the three-year follow-up evaluation, ten of the 31 patients (32 %) followed up reported regular use of psychotropic drugs compared with 25 of 43 patients (58 %) at the start.
Discussion
The median number of therapy sessions was 43, and a third of the patients were still in therapy at the time of the three-year follow-up. A significant share of the patients were thus receiving treatment on a level it is difficult to achieve at regional psychiatric clinics. The amount of therapy varied considerably nonetheless, and some had only had a few sessions.
There was a positive correlation between the number of therapy sessions and the patients’ satisfaction with the treatment. The results also showed that the treatment had a certain degree of flexibility in terms of appointment frequency. Some therapies started off as a weekly appointment and then changed to a less intensive phase. The continuity of the therapeutic relationship was thereby preserved.
For many patients with a personality disorder, their relations with caregivers as they grew up were characterised by insecurity or traumatic conditions. Such experiences influence the relational problems the patient has as an adult. Being able to relate to a therapist who is stable and predictable over time may therefore be especially important for these patients, and may enable them to work on core problems within a secure therapeutic relationship.
Patients with personality disorders have a tendency to become involved in negative interactions with others in a manner that reinforces their negative self-image, emotional imbalance and experience of rejection. In this study, several treatments were complicated by irregular attendance, disinhibited behaviour, substance abuse or concern associated with the patient's suicidality, circumstances that therapists may find demanding. Efforts to establish a good therapeutic alliance failed with some patients, and analyses of the patients’ satisfaction indicate that it is precisely those with substance abuse problems, extensive acting-out behaviour or serious suicidality who represent a challenge to therapy that may be difficult to handle in private practice.
Discontented patients displayed weaker functional improvement in the course of the three years. This study does not enable us to draw any conclusions as to whether this reflects inappropriate therapeutic processes in this or subsequent treatments or about other prognostic characteristics of the patients. On the whole, the therapists nonetheless found the treatments interesting and professionally stimulating.
The percentage of patients who dropped out of therapy was not particularly high compared with international studies, where dropout rates of well over 30 % are usual (7, 8). None of those still in therapy after three years will be classified as dropouts, so the final dropout rate will be less than 20 %.
The results must be interpreted with caution. The specialists who took part were self-selected for the study, and it is not certain how representative they were of private practitioners generally. They were probably highly motivated and many of them had extensive experience, although they did not necessarily have any special experience with this patient group. Some therapists treated several patients, so that there is some dependency in the data. The study design precluded the possibility of studying therapist effects.
The patient sample was representative of patients referred for third line service for treatment of personality disorders, but the results cannot necessarily be extended to patients with personality disorders more generally. Some patients were also hospitalised for different types of inpatient treatment or began a different therapy after ending treatment with the project therapist. We do not know whether their experience of other therapy influenced the patients’ reporting of satisfaction with the project treatment.
One main point, however, was that in the event of crises or when the treatment they themselves offered was regarded as insufficient, the specialists in private practice called on other available treatment. This should be possible in many places in Norway with a well developed and reasonably differentiated range of treatments services.
MAIN POINTS
Treatment by a specialist in private practice allows for flexibility in the duration and intensity of therapy for patients with a personality disorder
The majority of the patients are satisfied with the treatment
Irregular attendance, substance abuse, severe symptoms and acting-out behaviour complicate the treatment of a minority
Psychotherapy with a specialist in private practice presupposes access to other health services in the event of symptom exacerbation and complicating substance abuse.
- 4.
Gullestad FS, Wilberg T, Klungsøyr O et al. Is treatment in a day hospital step-down program superior to outpatient individual psychotherapy for patients with personality disorders? 36 months follow-up of a randomized clinical trial comparing different treatment modalities. Psychother Res 2012; 22: 426 – 41. [PubMed] [CrossRef]