Chronic obstructive pulmonary disease (COPD) is defined as a disease characterised by airflow limitation that is not fully reversible, that is progressive and associated with a pathological inflammatory response to exposure to noxious particles and gases (1). Work-related COPD is caused or exacerbated by exposure to particles and gases in the workplace (2).
The main known risk factors for COPD are cigarette smoking, workplace exposure, air pollution, fumes from the burning of biomass fuels, recurrent respiratory infections, low socioeconomic status and chronic airflow limitation resulting from asthma (3). In Norway it has recently been shown that several parts of the country have a higher incidence of COPD than the prevalence of smoking in those areas would suggest (4).
Studies from other countries show that 25 % of patients with COPD have never smoked (3, 5). Although exposure to fumes from the burning of biomass fuels is the main non-tobacco related cause of COPD globally (3), occupational exposure is considered to be among the main causes in Norway. It is known that 15 – 20 % of all COPD cases in Europe and the USA are work-related (2, 6, 7), and that there is an additive effect from smoking and occupational exposure (7, 8). Calculations show that 3 000 new cases will occur each year in Norway, and approximately 200 persons will die as a result of work-related COPD (9).
What types of occupational exposure can cause COPD? A recent review study, to which one of the authors of this article (TOBAA) contributed, assessed studies published in the period 2003 – 09 (10). The authors included 25 population studies and 34 industry or sector-oriented studies, and concluded that a sufficient correlation has been demonstrated between a number of types of occupational exposure and COPD. Occupations and industries that were associated with an increased risk in this study are shown in Table 1 (10, 11).
Table 1
Exposure associated with increased risk of development of COPD¹
| Industry/work task |
Exposure |
| Combined exposure |
|
| Asphalting |
Bitumen, polycyclic aromatic hydrocarbons |
| Glass and ceramic production |
Particles and gases from furnaces, paints and pigments |
| Mining, building and construction |
Silica, combination of particles and gases |
| Transport |
Diesel exhaust |
| Paper production |
Wood dust, peak exposure of ozone, ClO₂, SO₂ |
| Petroleum production and refinement |
Particles and gases from production, cleaning |
| Tunnelling |
Silica, oil vapour, mixture of gases and particles |
| Metals |
|
| Cadmium processing |
Cadmium |
| Welding |
Welding fumes |
| Vanadium extraction and processing |
Vanadium |
| Chemicals |
|
| Bleaching, disinfection |
Chlorine, ammonia |
| Cleaning, various production processes |
Ammonia, ammonia compounds |
| Isocyanate production, spray painting |
Diisocyanates |
| Weed control |
Pesticides |
| Minerals |
|
| Coke oven workers |
Coke |
| Miners |
Coal, silica |
| Quartz extraction, oven workers |
Silica |
| Insulation work |
Man made mineral fibres (MMMF) |
| Organic particles and gases |
|
| Cotton production |
Particles from cotton spinning |
| Agriculture |
Animal husbandry, handling of animals, endotoxin |
| Animal feed production |
Particles and gases from production, endotoxin |
| Grain milling, bakeries |
Grain dust |
| Rubber production |
Particles and gases from production |
| Jute processing |
Particles and gases from production, jute batching oil |
| Wood product and furniture industry |
Wood dust |
| [i] | |
[i] ¹ Based on findings from a Nordic systematic review study (10) and information from studies registered in Haz-Map, US National Library of Medicine (11), chapter on work-related COPD
Several studies on work-related COPD have been published since 2009, and the purpose of this article is to present recent findings. We also review diagnostic and prognostic considerations and opportunities for improving the prevention of work-related COPD.
Method
We conducted searches in Medline and Embase (May 2009 – July 2014) based on searches from a previous review study (10), restricted to human studies in Danish, English, Norwegian, German and Swedish with the following search terms (MeSH terms): pulmonary disease, chronic obstructive; (chronic obstructive pulmonary disease, OR chronic airflow obstruction copd OR coad OR chronic obstructive lung disease); chronic bronchitis. The combination: 1 OR 2 OR 3 were linked together (AND) with occupational diseases OR agricultural workers’ diseases OR pneumoconiosis, OR bagasosis, OR miner lung coal OR anthracosis, OR asbestosis OR berylliosis OR byssinosis OR siderosis OR silicosis OR occupational exposure OR work related OR workplace OR work location. In addition, single terms were truncated and included as text words. The authors also added three relevant articles which were assessed in the same manner as the others.
We identified three population studies and five prospective industry or sector-oriented studies (original articles), published in the period from May 2009 to July 2014. We supplemented these with three prospective studies on lung function and occupational exposure that were not indexed with the MeSH search terms used for obstructive pulmonary disease. These are discussed at the end of this article. For reasons of space and because the correlation between exposure and findings is less well-defined in cross-sectional studies, the latter have not been included. Studies that did not include measurements of pulmonary function or refer to occupational exposure were excluded.
Figure 1 shows inclusion and exclusion of articles and Table 2 (12) – (22) summarises the included studies.
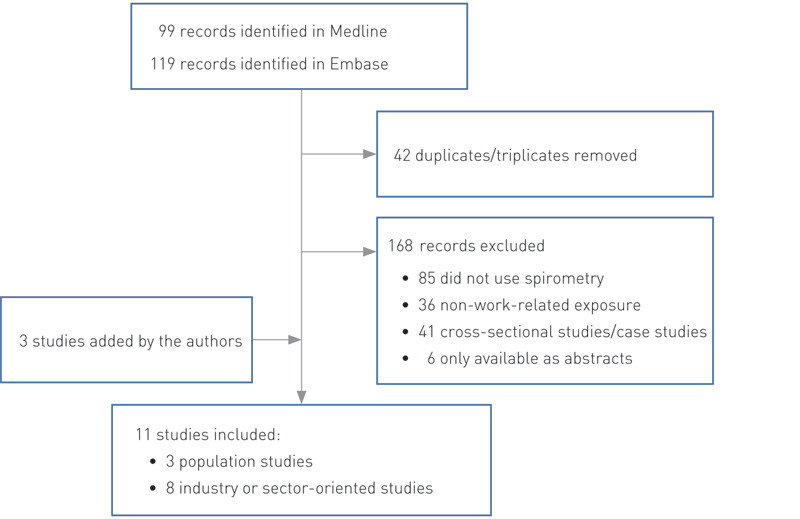
Table 2
Studies identified through an updated literature search on work-related COPD. All studies are adjusted for age and smoking, and all confidence intervals (CI) are 95 %. GOLD: Global Initiative for Chronic Obstructive Disease, FVC: forced vital capacity, FEV₁: forced expiratory volume after one second, IRR: adjusted incidence rate ratio. LLN: lower limit of normal, which corresponds to the 5th percentile in a healthy, non-smoking population, GM: geometric median
| First author, year (reference) |
Exposure |
Design |
Population |
Outcome |
Association |
| Metha, 2012 (12) |
Job-exposure matrix based on occupational codes |
Population study: 10 – 12 years |
N = 4 267 (18 – 62 years) |
COPD GOLD Stage II+ |
All exposure: COPD II+: IRR 2.1 (1.1 – 4.0) Biological dust: 2.6 (1.3 – 5.4) Mineral dust: 2.3 (1.1 – 5.0) Gas/fumes: 2.1 (1.1 – 4.2) |
| Mirabelli, 2012 (13) |
Job-exposure matrix based on occupational codes |
Population study: 3 years |
N = 8 967 (45 – 64 years) |
RR – symptoms compared to non-exposed, FEV₁ < LLN, FEV₁/FVC < LLN |
Mechanical work/maintenance: cough: RR 1.8 (1,0 – 3,2), sputum: 2.1 (1.2 – 3.6) Cleaning/maintenance of buildings: cough: 1.9 (1.0 – 3.4), sputum: 2.3 (1.3 – 4.1) FEV₁, FEV₁/FVC: no reduction |
| De Jong, 2014 (14) |
Job-exposure matrix based on occupational codes |
Population study: 25 years |
N = 2 527 (30 – 80 years) |
FEV₁-reduction per year |
Pesticides: FEV₁: –6.9 ml/year (–10.2 – –3.7) |
| Möhner, 2012 (15) |
Mining industry Job-exposure matrix Quartz: 1 mg/m³ over 220 eight-hour shifts/year |
Case-control study: 8 years |
N = 233, reference group: 1 N=115 (born 1954 – 56) |
COPD stage I+/II+ |
COPD I+: OR 1.8 (1.3 – 2.6) COPD II+: 1.4 (0.9 – 2.2) |
| Shi, 2010 (16) |
Textile industry Endotoxin: median 2 086 – 1 289 EU/m³ in 1981 – 92, 98 EU/m³ in 1996 |
Case-control study: 25 years |
N = 447, reference group: 572 (27 – 47 years at time of inclusion) |
FEV₁-reduction/year |
Previous exposure endotoxin: FEV₁: workers < 5 years before baseline: 93 (19 – 205), workers ≥ 5 years: 30 (43 – 104), > 10 years: 39 (50 – 129) |
| Webber, 2011 (17) |
Participation in fire and rescue work at the World Trade Center (day 0 – 14) |
Case-control study: 7 – 9 years |
N = 9 715, reference group: 1228 (18 – 64+) |
FEV₁/FVC in relation to medically diagnosed obstructive pulmonary disease |
Lowest quintile of FEV₁/FVC: 0.5 % COPD, 9.2 % chronic bronchitis, 9.4 % reported asthma – against 0.3 %, 1.1 % and 4.2 % respectively in the reference group |
| Aldrich, 2013 (18) |
General fire and rescue work |
Case-control study: 5 years |
N = 940, reference group: 97 (25 – 44 years) |
FEV₁/FVC-reduction/year |
Firefighters: FEV₁/FVC: 45 (42 – 48) ml/year. Reference group: 45 (35 – 54) |
| Nordby, 2013 (19)¹ |
Cement production Job-exposure matrix Thoracic aerosol: 0.14 – 14 mg/m³ |
Cohort study: 4 – 5 years |
N = 4 998 (17 – 54 years) |
Reduction FEV₁/m² per year and per mg/m³ |
All exposed: FEV₁/m²: 2.9 (2.5 – 3.2) ml/m² · (year · mg/m³) Lowest exposure category: (0.6 – 1.6 mg/m³): 9.7 (7.6 – 12) Highest (5.4 – 14 mg/m³): 19 (15 – 22) |
| Tungu, 2014 (20) |
Cement production Total dust before and after reduction: 10.6 and 5.8 mg/m³ |
Case-control study: 2 years |
N = 120, reference group: 107 (24 – 49 years) |
FEV₁/FVC < 0,7 |
Before dust reduction: FEV₁/FVC < 0.7: 22.6 %, reference group: 5.9 % After dust reduction: 1.9 %, reference group: 4.3 % |
| Hovland, 2013 (21)¹ |
Nitrate fertiliser production Inhalable and thoracic fraction: 1.1 and 0.21 mg/m³ |
Cohort study: 3 years |
N = 383 (38 – 58 years) |
Reduction FEV₁ |
FEV₁: 18 (27 – 10) ml/year |
| Johnsen, 2010 (22)¹ |
Metallurgical smelting industry Job-exposure matrix Highest and lowest tertile for median GM: FeSi/Si metal: 1.1 and 3.2 mg/m³ SiMn/FeMn/FeCr: 0.82 and 1.9 mg/m³ |
Cohort study: 4 – 5 years |
N = 2 620 (20 – 55 years) |
Reduction FEV₁/height² per year |
FeSi/Si metal: FEV₁/m²: 0.42 (0.95 – 0.11) (ml/m²) · (mg/m³) · year SiMn/FeMn/FeCr: 1.1(2.1 – 0.1) |
| [i] | |||||
[i] ¹ Studies added by the authors – these were not indexed with the MeSH search terms for obstructive pulmonary disease that were used
Population studies
The results from a prospective Swiss study show that persons with high levels of occupational exposure had a risk of COPD (GOLD stage II+) that was two to five times higher than for those who were not exposed (12). A total of 4 267 persons were followed up for ten years and job-exposure matrices, which reduce errors based on over-reporting of exposure by those who are ill (23), were used to categorise exposure. The proportion of work-related COPD was 23 % in smokers and 32 – 51 % in non-smokers, depending on which criteria for COPD were used. The study corroborates previous findings (3).
In an American study in which 8 967 persons were followed up for three years, elevated risk was observed for new-onset chronic cough and chronic phlegm for mechanics, repairers, cleaners and building service workers compared with the control group (managerial and administrative support) (13). No elevated risk was observed for COPD, which may be attributable to the short follow-up time and exclusion of persons with respiratory symptoms at the outset. However, the findings may indicate an increased risk of COPD if the exposure is of long duration.
In a large-scale study from the Netherlands, occupational exposure in general, and to pesticides in particular, was linked to elevated risk of COPD (n = 11 851) (14). The authors repeated the study by drawing a new sample (n = 2 364) and were able to confirm the results for this group. However, a correlation with exposure to pesticides still remains to be demonstrated in other studies.
A general problem with population studies is lack of information on exposure and differential diagnostic assessments. In the Swiss and American studies, occupational codes are used instead of more rudimentary categories for exposure, which provide more information on which types of exposure entail increased risk.
Industry or sector-oriented studies
Studies that examine an industry or sector have the advantage that the exposure is often described and categorised. The disadvantage is that the participants may differ from the normal population (selection bias), which can result in an underestimation of risk.
Exposure to quartz occurs in several industries, such as building and construction, the steel industry, mining, and during tunnelling and sandblasting. A German study of miners exposed to quartz (n = 1 421) confirms that exposure to quartz (1 mg/m³ over the course of 220 eight-hour shifts per year) may increase the risk of stage I COPD (OR 1.8, 95 % CI 1.3 – 2.6), and it is estimated that exposure to 0.1 mg/m³ (Norwegian threshold value) over a 40 year period will result in reduced pulmonary function (15). The study shows an elevated risk of COPD at current levels of exposure, where new rock-drilling technology (higher rate of revolutions per minute) may conceivably produce a greater number of finer particles. Increased prevalence of COPD has previously been shown in a Norwegian study of tunnel workers from 2001 (10) and in a large-scale Swedish study of construction workers from 2004 (24).
The extent to which textile workers have an elevated risk of COPD is a matter of debate, as the findings from previous studies have been at variance. In a study from 2010, 447 textile workers were followed up for 25 years and it was found that previous exposure to endotoxin (median 2 086 – 1289 EU/m³ for 1981 – 92) was associated with reduced forced expiratory volume after one second (FEV₁), while recent exposure (median 98 EU/m³) was associated with chronic shortness of breath and cough (16). Although the data on smoking were incomplete, the researchers have measured exposure and adjusted for other possible causal factors. There is still a need for further studies, but the results give grounds to suspect an increased risk of COPD in textile workers.
Firefighters are periodically exposed to high-grade exposure, but this has been insufficiently studied. An increased risk of COPD was found in firefighters who were involved in the rescue and recovery work following the terror attacks on the World Trade Center (17). In a later study no such correlation was found for New York firefighters who were exposed for five years, but recruited after 2003 (18). The 9/11 exposure was typically extremely high-grade, complex and consisted of pulverised cement, glass, lead, polycyclic aromatic hydrocarbons, metals and polychlorinated biphenyls, and had a pH of around 12. While it is still unclear whether firefighters in general have an elevated risk of COPD, the 9/11 studies may be relevant for the assessment of exposure to high-grade, complex, alkaline dust.
The effects of another type of alkaline dust have been investigated in a large-scale prospective study of cement production workers from eight European countries (19). In the Norwegian-led study, 4 998 employees were followed up for 4.6 years and a dose-response relationship was found between level of dust and reduced FEV₁/standing height² per mg/m³ and year, with 9.7 (95 % CI 7.6 – 12) for the lowest category of exposure (0.6 – 1.6 mg/m³) and 19 (15) – (22) ml for the highest (5.4 – 14 mg/m³). Job-exposure matrices were used to categorise exposure, and asthmatics were excluded from the analyses. A study of 171 cement workers from 2014 found that a reduction in dust levels (from 10.6 mg/m³ to 5.8 mg/m³ total dust) resulted in a reduced prevalence of COPD (from 22.6 % to 1.9 %) after two years (20), thereby indicating an effect from dust-reducing measures. The results provide sound evidence for an elevated risk of COPD in the cement production industry, and are also considered relevant for employees in the building and construction industry.
A three-year follow-up of Norwegian employees (N = 383) working with nitrate fertiliser production showed reductions in FEV₁ of 18 ml/year (95 % KI 10 – 27) with an exposure of 1.1 mg/m³ and 0.2 mg/m³ for inhalable and thoracic aerosols (21). There was no correlation between reduced pulmonary function and exposure, which indicates that factors other than the measured aerosol fraction are of significance. There is a need for further studies, but the results may give rise to the suspicion that work at the fertiliser factory entails an increased risk of COPD.
In a study from 2010 which followed up 2 620 workers at Norwegian metallurgical smelters for five years and used job-exposure matrices to characterise exposure, FEV₁/standing height² fell with rising dust level (22). Annual reduction in FEV₁/standing height² for a worker (1.80 cm tall) was 5.7 ml/year in smelters that produced silicomanganese, ferromanganese and ferrochrome, whereas it was 6.4 ml/year for a non-smoking worker in a smelter that produced ferrosilicon and silicon metal. FEV₁ was lower for women than for men. In a review article the authors have concluded that there is sound evidence of an increased prevalence of COPD also in non-smokers in the metallurgical smelting industry (25).
Diagnostic assessments
It has been demonstrated that those who have been exposed to particles and gases had more sputum production and dyspnoea than other COPD patients (26). A recent study found that patients with work-related COPD more frequently reported atopy, wheezing and work-related disability than others affected by COPD (27). We recommend the use of short, validated questionnaires and yearly spirometry to screen for COPD in workers who are exposed to particles and gases. Good training should be provided to those conducting spirometry testing to ensure reliable results.
Because some workers do not attend screening examinations, doctors are encouraged to provide information about risks and protective measures in workplaces where there is exposure to particles and gases. This may help to ensure that more workers attend and fewer fear the consequences of possible findings.
Spirometry monitoring programmes may be considered in order to identify those who are about to develop COPD (28). Reduced pulmonary function, but also changes over time for those who have values within normal ranges, should result in further assessment and measures to be taken in the working environment.
In cases of familial aggregation or early onset of COPD, measurement of serum levels of alpha-1 antitrypsin is recommended. HRCT (high resolution computed tomography) examination and supplementary respiratory physiology examinations (diffusing capacity for carbon monoxide (DLCO), TLC and RV testing) are recommended to determine and assess emphysema. A low threshold should be required for referral to a department of occupational medicine and/or respiratory medicine, since assessment is time-consuming and the legislation for approval of occupational injury claims is complex.
Prognosis, measures and prevention
Primary prevention in the workplace can be achieved through reduction in exposure with the use of both technical and organisational measures. It is also important to ensure the use of adequate protective equipment when other measures are not possible. Every doctor who suspects work-related illness has a duty to report this to the Norwegian Labour Inspection Authority (form 154b). The report draws attention to new agents and working methods that entail an increased risk of COPD. The Norwegian Labour Inspection Authority can follow up with a workplace visit and an order to implement measures so that new cases can be prevented. Encouragement of smoking cessation should continue.
What next when the diagnosis of work-related COPD has been made? What advice should be given? Can the patient continue to work? Persons with work-related COPD may have a reduced ability to work and lower quality of life than other COPD patients (26, 29). However, doctors should be cautious with regard to recommending that patients give up their job, as experience shows that many have difficulties in returning to employment. The aim should be to cooperate with the occupational health service to make necessary adjustments in the workplace, and with departments of occupational medicine and respiratory medicine which have particular competence with regard to substances and work tasks that should be avoided.
Characteristics of the individual such as smoking habits, age and gender can have a bearing on the risk of work-related COPD. A study from 2008 showed that female (but not male) employees who were exposed to wood dust experienced a dust-related drop in FEV₁ of 25 ml/year (30). By comparison, smoking results in an average drop of 10 ml/year (31). Sunyer et al. (32) have previously demonstrated a greater fall in FEV₁ in women who are exposed to high levels of biological and mineral dust. One of the explanations suggested was that the size of women’s airways is smaller than that of men.
Because there will be vulnerable individuals in all groups, however, the objective should be to reduce the level of exposure for all workers, irrespective of individual vulnerability factors.
Conclusion
Recent studies show an increased risk of COPD where there is exposure to quartz at current levels of exposure and for employees in the cement production and metallurgical smelting industries, whereas the correlation is less certain for firefighters and workers in the nitrate fertiliser production industry. Moreover, findings from previous review studies are confirmed, which conclude that there is sufficient knowledge to state that a series of organic and inorganic exposures at work may cause COPD. All patients in whom work-related COPD is suspected should be referred for an occupational health assessment.
MAIN MESSAGE
Recent studies detect a correlation between occupational exposure and an increased risk of COPD in the construction, metallurgical smelting, cement production and textile industries.
There should be a low threshold for enquiring about exposure in the workplace in cases of suspected or established COPD, and for referral to occupational health assessment.
Where work-related COPD is suspected, this should be reported to the Norwegian Labour Inspection Authority.
- 1.
Global Strategy for the Diagnosis, Management and Prevention of COPD, Global Initiative for Chronic Obstructive Lung Disease. 2013. www.goldcopd.org/Guidelines/guidelines-resources.html (21.10.2014).
- 9.
Leira HL. Kols – ikke bare hos røykere. Tidsskr Nor Legeforen 2011; 131: 1756 – 7. [PubMed]
- 11.
Haz-Map. Information on hazardous chemicals and occupational diseases. www.hazmap.nlm.nih.gov (21.10.2014).
- 18.
Aldrich TK, Ye F, Webber MP et al. Longitudinal pulmonary function in newly hired, non-World Trade Center-exposed fire department City of New York firefighters: the first 5 years. Chest 2013; 143: 791 – 7. www.ncbi.nlm.nih.gov/pubmed/23188136
- 19.
Nordby KC. Prospective monitoring of exposure and lung function among cement production workers – an international study. Occup Environ Med 2013; 70 (suppl 1): A141. [CrossRef]
- 28.
Hznido E, Yan T, Hakobyan A et al. Longitudinal data analysis software for analysis of spirometry data in workplace prevention or COPD Treatment. Open Med Inform J 2004: 94 – 102.