Hearing loss caused by noise in the workplace reduces the quality of life of those affected and increases the risk of occupational injuries, since it may reduce the employee’s alertness (1, 2). It has been estimated that in the EU, approximately 13 million employees suffer from hearing loss because of exposure to noise in the workplace (3). The Nord-Trøndelag Health Study (HUNT) showed a moderate association between hearing loss and exposure to noise in occupations such as construction, carpentering and mining (4).
In the Oslo Health Study (HUBRO), altogether 28 % of the gainfully employed 30-, 40- and 50-year-olds with a self-reported hearing loss believed that it may have been caused by the conditions at their workplace (5). In Statistics Norway’s living conditions survey from 2009, a total of 14 % of all gainfully employed men and 7 % of all gainfully employed women reported that they were exposed to loud noise for one-quarter of their working hours or more (6). Loud noise was defined as noise that made it necessary to stand very close and shout in order to be heard.
In Norway, there are two compensation schemes for occupational injury or disease. One is a governmental scheme under the national insurance system and is administered by the Norwegian Labour and Welfare Agency (NAV). The other is based on the enterprises’ mandatory insurance of its employees and is administered by private insurance companies. The private insurance covers also future loss of income and will therefore tend to pay out a larger amount than the national insurance system, and the criteria for approval of a case as an occupational injury/disease are somewhat less restrictive.
NAV no longer publishes figures on the number of occupational injuries and diseases that they approve. According to secondary sources, in the period 2004 – 07 they approved on average 347 cases per year of «diseases of the ear and mastoid process» (ICD-10 H60-H95), whereof 11 cases pertained to women (7). These are primarily cases of noise-induced hearing loss. Each year, compensation for permanent injury (0.07 G annually), which assumes a disability degree of at least 15 %, is granted to approximately 50 people. A bilateral loss of 40 dB with a well-adapted hearing aid will be equivalent to a disability degree of only 10 % in NAV’s disability table according to the regulations for compensation for permanent injury after an occupational accident.
According to Finance Norway, altogether 117 cases of hearing loss with a claim for compensation were reported in the period 2002 – 2009. A total of NOK 41.9 million was paid in compensation for these cases (8). The real number of employees who suffer from reduced quality of life as a result of hearing loss is likely to be far higher than indicated by the figures from NAV and Finance Norway, as is the case for other occupational diseases (9, 10). There is also a lack of awareness among employees and doctors with regard to the fact that claims to occupational injury benefit and private insurance must be put forward by the employees themselves (9, 10).
According to Section 5-3 of the Working Environment Act, doctors must report to the Labour Inspection Authority all cases of hearing loss that they believe to have been caused by exposure to noise at work. This obligation to report applies to all diseases that may have been caused by working conditions, and in practice provides an opportunity to inform the inspectorate about patients whose working conditions are harmful. The report provides information on risks attributed to the working environment and serves as basis for sentinel surveillance (11).
When the permissible noise levels in the working environment were defined in 1978, the experts believed that the upper limit had to be 80 dB in order to prevent hearing loss. For economic reasons, however, the limit was set at 85 dB (12). Hearing tests should be undertaken to detect early signs of hearing loss in those exposed to hazardous noise levels ranging from 80 dB to 85 dB. In other words, the objective of such tests in the enterprises is to provide a basis for secondary prevention, for example by relocating vulnerable individuals. At the same time, in enterprises where there is a need for hearing tests of the employees, systematic efforts must be made in terms of primary prevention in the form of a reduction in the noise levels or the period of employee exposure to noise (Regulations on action and threshold values).
The objective of this study was to describe the doctors’ reports to the Labour Inspection Authority concerning noise-induced hearing loss and to assess the quality of the information that this reporting system provides to the inspectorate.
Material and method
This study is based on data that includes the registrations of doctors’ reports in the Labour Inspection Authority’s incident-based registry of work-related related diseases (RAS). The registry shall be used for purposes of prevention of work-related health problems and has been described in more detail in another article (11).
This registry contains information on diagnoses, relevant exposure factors, period of exposure and on whether the patient is still working in the enterprise where the exposure occurred. Moreover, there is information on the patient’s age, gender and occupation and the professional designation of the reporting doctor (occupational health physician, hospital doctor, general practitioner etc.). The diagnosis and occupation are coded by the Labour Inspection Authority in accordance with the information that the doctor has provided in the report. Diagnoses are coded according to ICD-10, while occupations are coded according to the Norwegian Standard Classification of Occupations (STYRK). The registry includes the name and address of the enterprise as provided in the doctor’s report. The organisation number and industry code are retrieved from the Central Coordinating Register for Legal Entities. The industry code follows the Norwegian Standard Industrial Classification (NACE).
Our study population includes all reports submitted in the period 2005 – 2009 with the ICD-10 diagnoses H 83.3 (noise effects on inner ear) and H 93.1 (tinnitus) in employees in land-based enterprises. The reporting incidence (reports per 100 000 employees) was estimated with the aid of employment data retrieved from Statistics Norway.
For example, the reporting incidence in the construction industry was estimated on the basis of the average annual number of reports over the five-year period (n = 303) and the average annual number of employees in the industry during the same period (n = 175 701) in the following manner:
303 · 100 000/175 701 = 172
The Agency for National Surveillance of Working Environment and Occupational Health (NOA) provided data on self-reported hearing loss in employees based on Statistics Norway’s living conditions survey from 2009. Statistical analyses were performed in Microsoft Excel 2007.
Results
In the five-year period 2005 – 2009, the Labour Inspection Authority received a total of 7 888 reports on hearing loss (ICD-10 H 83.3 and H 93.1).Tinnitus (ICD-10 H 93.1) was the main diagnosis in 2 % of these reports (n = 158) . The average annual number of reports was 1 577, ranging from 1 453 to 1 697. Altogether 96 % of the reports concerned men, and 52 % concerned patients who were no longer working in the enterprise where they may have been inflicted with this hearing loss. Occupational health physicians accounted for the majority of the reports (85 %). In a few instances the report had been submitted by a hospital doctor (7 %) or other doctors, such as municipal medical officers and general practitioners (8 %). The total reporting incidence was 66 per 100 000 employees per year in this period; six and 120 for women and men respectively.
Figure 1 shows the reporting incidence by age groups. The reporting incidence (occurrence of new report per 100 000 employees per year) was highest in the age group 55 – 74 years, while the majority of the reports (n = 689) concerned the age group 40 – 54 years. For the age groups 16 – 24 years, 25 – 39 years and 55 – 74 years, there were 31, 234 and 624 reports respectively.
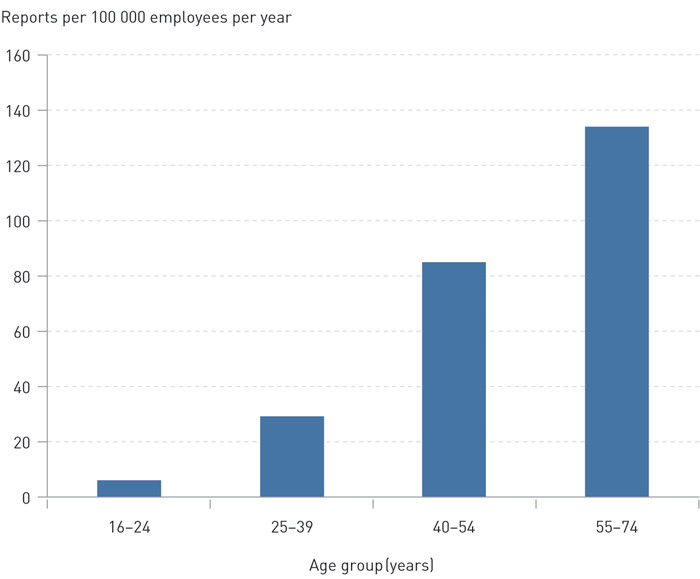
Table 1 shows the distribution of reports by industry. If we exclude mining and extraction and electricity, gas, steam and hot-water supply because the incidence has been estimated on the basis of only very few reports, the highest reporting incidence was found in the manufacturing and construction industries, with 223 and 172 per 100 000 employees respectively. These two industries also accounted for the highest number of reports.
Table 1
Work-related hearing loss reported to the Labour Inspection Authority in the period 2005 – 09. Average number per year and reporting incidence per 100 000 employees per year in the ten industries that had the highest number of reports during the period
| Industry |
Average number per year (%) |
Reporting incidence per 100 000 employees |
|
| Mining and extraction |
31 |
(2) |
710 |
| Manufacturing |
588 |
(37) |
223 |
| Electricity, gas, steam and hot water supply |
32 |
(2) |
215 |
| Construction |
303 |
(19) |
172 |
| Public administration, defence, public benefits administration¹ |
98 |
(6) |
64 |
| Transport and storage |
119 |
(8) |
62 |
| Agriculture, forestry and fishery |
31 |
(2) |
39 |
| Retail trade, automotive repair |
91 |
(6) |
25 |
| Education |
37 |
(2) |
19 |
| Business services |
25 |
(2) |
14 |
| All industries |
1 577 |
(100) |
66 |
| [i] | |||
[i] ¹ Most of the reports came from the Armed Forces
Figure 2 shows the proportion of reports pertaining to employees younger than 40 years in the five industry groups with the highest number of reports. The figure also shows the corresponding proportion of all employees who reported work-related hearing loss in Statistics Norway’s living conditions survey for 2009.
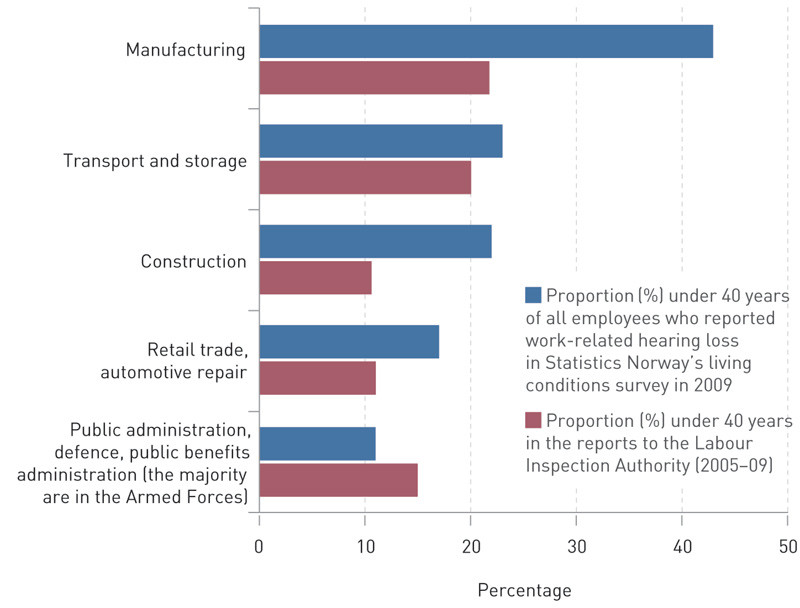
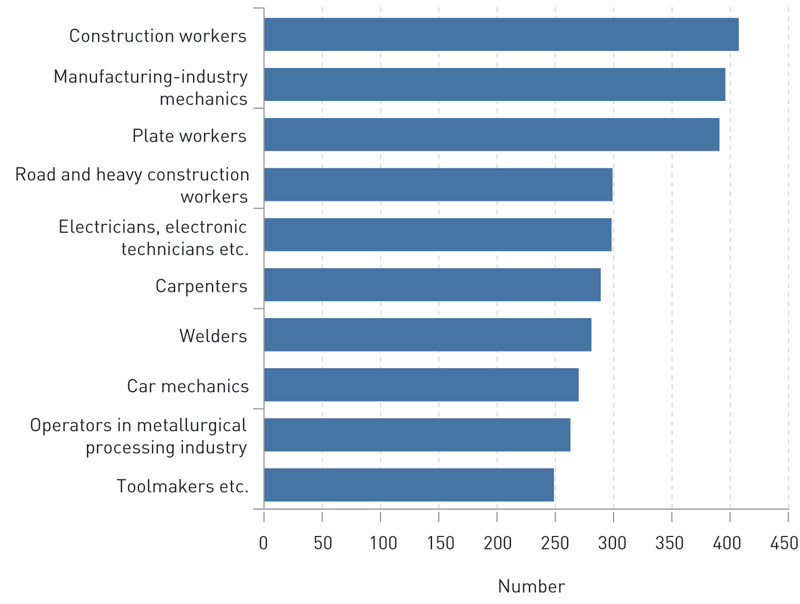
Figure 3 shows the ten occupations that had the highest number of reports.
Discussion
In the period 2005 – 2009, the Labour Inspection Authority received a total of 7 888 reports on work-related hearing loss. Altogether 40 % of these reports concerned employees older than 55 years. This is fairly consistent with a corresponding study from the Norwegian continental shelf (petroleum installations), in which 44 % of the reports pertained to employees older than 55 years (13). Hearing loss develops over time, and will not always manifest itself until additional age-related changes develop in parallel. The relative attribution of ageing and occupation to hearing loss is difficult to evaluate (14). Changes in industrial structure, technological development and better primary prevention over the last 20 – 30 years may have reduced the risk of work-related hearing loss.
Only 4 % of the reports concerned women. This corresponds poorly with the gender distribution in terms of exposure to noise in Norwegian working life. Noise exposure and hearing loss in women employees have been described as an underestimated problem also in the EU (15). A Belgian study showed that while the proportion of women who were exposed to noise in the workplace was half that of men, only 1 % of all cases of hearing loss that were recognised as an occupational injury included women (16).
The situation in Norway is identical. According to Statistics Norway’s living conditions survey from 2009, half as many women as men (7 % vs 14 %) were exposed to loud noise at work, and nearly half as many women as men (2 % vs 5 %) reported to suffer from work-related hearing loss. (6). However, no women were granted compensation from NAV for permanent occupational injury because of hearing loss in the period 2004 – 2007 (7). Our study shows that the doctors’ report to the Labour Inspection Authority fails to capture work-related hearing loss in women.
Only 2 % of the reports concerned tinnitus (ICD-10 H 93.1). Similarly, a low proportion of tinnitus was found in a Finnish study where work-related tinnitus was not reported when hearing loss was also present (17). Tinnitus was mentioned in no more than 4 % of the reports on work-related hearing loss, while it was evident in nearly 90 % of the cases (17). For many, tinnitus is a serious consequence of exposure to noise, but the problem largely fails to appear in the reports to the Labour Inspection Authority.
The distribution of the reports by industry largely accords with known facts on exposure to noise and hearing loss in Norwegian working life. Three of the four industries that had the highest reporting incidence for hearing loss in this study (mining, manufacturing and construction) also had the highest proportion of employees who were exposed to noise (20 – 25 %) according to Statistics Norway’s living conditions survey from 2009 (6). In the HUNT studies, the prevalence of age-adjusted hearing loss was highest in occupations that are common in these three industries (4). The ten occupations with the highest number of reports (Figure 3) in our material largely correspond to those occupations in which the highest number of cases of work-related hearing loss was reported in the 2009 living conditions survey, and also to those occupations in which the HUNT studies detected the largest average hearing loss (4, 6).
For the primary industries, however, the proportion and reporting incidence are both low in our material, despite the fact that the exposure to noise may be considerable. In Statistics Norway’s living conditions survey for 2009, altogether 12 % of employees in agriculture and aquaculture reported to suffer from work-related hearing loss, compared to 4 % of all employees (6). The primary industries include agriculture, forestry and fishery, but in our study agriculture accounts for 75 % (n = 155) of the reports. An occupational health service is not mandatory for agriculture, pursuant to the Working Environment Act. A voluntary scheme for this industry (the HSE service for agriculture) covers no more than approximately 12 000 of the total of 50 000 agricultural enterprises. In agriculture, a large proportion of workers are self-employed people who are not automatically included in public occupational injury benefit and insurance schemes. They thus stand to gain no financial benefit from being diagnosed with work-related hearing loss, and this most likely explains the low reporting incidence.
We also compared the age distribution of those reported by industry with the age distribution of self-reported work-related hearing loss in the 2009 living conditions survey (6). Figure 2 shows that the proportion of those under 40 years who report to suffer from work-related hearing loss in the living conditions survey is for the most part higher than the corresponding proportion in the reports submitted to the Labour Inspection Authority. This difference varies by industry. It is smaller in the construction industry (23 % vs 20 %) than in the transport sector (22 % vs 11 %) and retail trade (43 % vs 22 %).
The age distribution of those reported by industry may indicate that the follow-up in the form of hearing tests for younger employees exposed to noise is less effective in the transport sector and retail trade than in the construction industry. A large proportion of the employees in retail trade are women, and only parts of this industry are obligated to provide occupational health services. These are two issues that according to our observations reduce the likelihood of hearing loss being captured by the system of reporting to the Labour Inspection Authority.
In the construction industry the prevalence of hearing loss in young employees may also be greater than is indicated by the reporting incidence in this study. In a questionnaire survey undertaken by IRIS (International Research Institute of Stavanger) among 456 employees in this industry with an average age of 34 years, altogether 29 % reported reduced hearing because of exposure in the workplace (18). A number of international studies indicate that young employees in exposed industries such as construction have measurable hearing loss that requires early detection and preventive intervention (14, 19).
Primary prevention on the basis of the doctor’s report to the Labour Inspection Authority can be undertaken after the inspectorate has issued an injunction for a mapping of the noise exposure (if there is doubt regarding the risk) or noise reduction (level or time of exposure). The doctor’s hearing loss report may also provide a basis for an injunction for secondary prevention if the employee needs follow-up because of vulnerability to the hazardous effects of noise. For example, a relocation may be necessary.
About 52 % of the reports to the Labour Inspection Authority pertained to previous exposure. Hearing tests undertaken after the employment relationship and exposure have ceased may clarify the individual employee’s claim to compensation from national and private insurance, but provide little information of value to the labour inspectorate. However, if the report states that the enterprise in question continues to have a noise problem, this information may provide grounds for an injunction for primary prevention that will benefit other employees.
The occupational health physicians account for 85 % of all reports concerning hearing loss. Even in industries that are obligated to provide occupational health services, less than half of the enterprises are likely to comply with this obligation, according to figures from inspections undertaken by the Labour Inspection Authority in 2010. Many industries that are not obligated to provide occupational health services may have employees who are exposed to hazardous noise. In addition to the primary industries, this applies also to other industries such as the entertainment business and retail trade. Employers are obligated to ensure that hearing tests are performed, irrespective of their obligation to provide occupational health services (Regulations on performance of work in enterprises with exposure to noise). Judging by the reports submitted to the Labour Inspection Authority, however, hearing tests are very rarely undertaken by doctors other than occupational health physicians.
If the doctors suspects that there is an association between the patient’s tinnitus or hearing loss and noise in the workplace, this constitutes sufficient grounds for reporting. The threshold for reporting ought to be low. The purpose of the reporting system is not to measure «the scope of the problem», as many seem to believe, but to obtain information on possible risk factors and the need for preventive efforts. The criticism that has been raised regarding the lack of specificity in the reporting system clearly disregards this fact (20).
General practitioners could ask about the patient’s occupational history and undertake a simple hearing test such as whispering voice test (Box 1) (21). This is similar to when completing a health certificate for a driving licence (22). Studies have shown that when appropriately applied, the whispering test remains a useful tool for diagnosing hearing loss (23) – (25). A whispering test combined with an occupational history may reveal a need for an examination by a specialist and audiometry, but a report to the Labour Inspection Authority does not require detailed examinations.
Whispered voice test for a simple hearing test (21)
The doctor stands at an arm’s length (0.6 m) behind the seated patient and whispers a combination of numbers and letters (e.g. 4-k-2). The patient is then asked to repeat the sequence.
The doctor should quietly exhale before whispering to ensure as quiet a voice as possible.
If the patient answers correctly, his/her hearing is deemed normal. If the patient gives a wrong answer, the test is repeated with another combination of numbers and letters.
The patient’s hearing is deemed normal if at least three of six possible numbers or letters are repeated correctly.
The doctor must stand behind the patient to prevent lip-reading.
Each ear is tested individually, starting with the ear with better hearing. The patient blocks the other ear by occluding the auditory canal with a finger and rubbing the tragus in a circular motion. The other ear is assessed similarly with a different combination of numbers and letters.
A strength of this study is the authors’ familiarity with internal practices for registration and follow-up in the Labour Inspection Authority and the inspectorate’s internal inspection data at the aggregate level (compliance with the Act on enterprise health services). A weakness is that the information communicated in the reports on noise exposure and work-related hearing loss by age, gender and industry cannot be compared to noise exposure and audiometry data. Available national data are mainly based on self-reported information from surveys (Statistics Norway’s living conditions survey from 2009).
Conclusion
The doctors’ practice with regard to reporting to the Labour Inspection Authority, as reflected in the reports on work-related hearing loss in the period 2005 – 09, indicates that the inspectorate receives insufficient information on hearing loss in women, young employees (< 40 years) and employees in enterprises with high noise levels but no access to occupational health services. These findings may also indicate that the monitoring in the form of hearing tests of employees who are exposed to noise is less effective in retail trade and the transport sector than in the construction industry. This merits further investigation.
In order for the Labour Inspection Authority’s incident-based monitoring of work-related hearing loss to become an effective tool for reducing noise levels in working life, doctors other than occupational health physicians must also inquire about working conditions when the patient has a hearing impairment, and report to the Labour Inspection Authority if work-related hearing loss is suspected.
Acknowledgements: We wish to thank Liv Astrid Lande, who is in charge of the Labour Inspection Authority’s registry of work-related diseases (RAS), for her efforts with the registration of the doctors’ reports.
MAIN MESSAGE
Doctors can contribute to prevention by reporting patients exposed to hazardous noise at work causing possible work-related hearing loss.
Current reporting practice fails to sufficiently capture work-related hearing loss in women and younger employees, as well as employees in workplaces that have no access to occupational health services.
- 2.
Toppila E, Pyykkö I, Pääkkönen R. Evaluation of the increased accident risk from workplace noise. Int J Occup Saf Ergon 2009; 15: 155 – 62. [PubMed]
- 3.
Reducing the risks from occupational noise. Brussel: EU-kommisjonen, 2005. https://osha.europa.eu/en/publications/reports/6805535 (12.7.2013).
- 6.
Nasjonal overvåking av arbeidsmiljø og helse (NOA). Faktaboka. Oslo: Statens arbeidsmiljøinstitutt, 2011.
- 7.
Norges offentlige utredninger. Yrkessykdommer. Yrkessykdomsutvalgets utredning av hvilke sykdommer som bør kunne godkjennes som yrkessykdom. NOU 2008: 11.
- 8.
DAYSY-rapport. Årsaksstatistikk i yrkesskadeforsikring. Oslo: Finans Norge, 2011. www.fno.no/pagefiles/8420/yrkesskader%20daysy-rapporter/daysy_rapport2011.pdf (1.2.2013).
- 9.
Bratt U, Leira HL. Lov om yrkesskadeforsikring – en forbedring for de skadelidte? Tidsskr Nor Lægeforen 1997; 117: 207 – 11. [PubMed]
- 10.
Leira HL. Astma i norsk arbeidsliv. Tidsskr Nor Legeforen 2008; 128: 2719 – 21. [PubMed]
- 12.
Borchgrevink B. Hearing and hearing prophylaxis. Scand Audiol 1982; 16: 62.
- 13.
Morken T, Bråtveit M, Moen BE. Rapportering av hørselsskader i norsk offshoreindustri 1992 – 2003. Tidsskr Nor Lægeforen 2005; 125: 3272 – 4. [PubMed]
- 15.
New risks and trends in the safety and health of women at work. Bilbao: The European Agency for Safety and Health at Work (EU-OSHA), 2013. https://osha.europa.eu/en/publications/reports/new-risks-and-trends-in-the-safety-and-health-of-women-at-work (12.2.2014).
- 16.
Vogel L. Women and occupational diseases: the case of Belgium. Brussel: European Trade Union Institute (ETUI), 2011.
- 17.
Mrena R. Investigations of noise-related tinnitus. Doktoravhandling. Helsinki: University of Helsinki Medical Faculty, 2011.
- 18.
Kjestveit K, Lund-Ellingsen K, Holte K. Unge arbeidstakere i bygg og anlegg. Fra skole til arbeidsliv. Rapport IRIS – 2010/66. Stavanger: IRIS – International Research Institute of Stavanger, 2010. http://ba.rvofond.no/upload/2012/10/19/rapport-iris-2010_066.pdf (9.3.2014).
- 20.
Lie A, Skogstad M, Johnsen TS. Hørseltap hos jernbaneansatte som ikke har vært yrkesmessig støyeksponert. Ramazzini 2013; 2: 4 – 6.
- 22.
Helsedirektoratet. Retningslinjer for fylkesmennene ved behandling av førerkortsaker. Oslo: Helsedirektoratet, 2013.
- 23.
Eekhof JA, de Bock GH, de Laat JA et al. The whispered voice: the best test for screening for hearing impairment in general practice? Br J Gen Pract 1996; 46: 473 – 4. [PubMed]