Urinary incontinence, anal incontinence and pelvic organ prolapse are together referred to as pelvic floor dysfunction. The International Continence Society has established a standardised terminology for these conditions, which is now in widespread use among researchers (1). Their prevalence is primarily studied in high-income countries (Table 1) (2). There is a significant degree of overlap between these conditions (2, 3), but the risk factors vary.
Table 1
Prevalence of symptoms of pelvic floor dysfunction among women (2)
| Symptom |
Prevalence (%) |
| Urinary incontinence |
25 – 45 |
| Anal incontinence¹ |
11 – 15 |
| Pelvic organ prolapse |
5 – 10 |
| [i] | |
[i] ¹ Anal incontinence encompasses leakage of gas or liquid or solid faeces
It is commonly assumed that pelvic floor dysfunction is partly attributable to injury associated with vaginal delivery. The proportion of caesarean sections has increased significantly in high-income countries in recent years (4), and in Norway from just under 2 % in 1967 to 17 % in 2010 (5). However, there are large variations between countries. For example, in 2011 the proportion of caesarean sections was 24 % in the UK and 14 % in the Netherlands (6). At two of our largest maternity institutions, Oslo University Hospital, Ullevål, and Haukeland University Hospital, caesarean sections represented 18.3 % and 13.6 % of the deliveries in 2013, respectively, whereas the national average was 16.4 % (5). Such differences indicate that the proportion of caesarean sections is not dictated solely by objective medical factors – there must also be cultural differences between the institutions and in society at large (7).
We have reviewed the literature on vaginal delivery as a risk factor for pelvic floor dysfunction compared to caesarean section.
Material and method
We conducted a search in PubMed of literature in English, last updated in January 2014 (Fig. 1). Since we wanted to investigate the risk following caesarean section under comparable conditions, we did not include articles containing material from low- and middle-income countries with conditions and frameworks for obstetrics that differ from those in high-income countries. Articles based on selected populations were excluded. Where there were articles based on the same material (duplications), these were also excluded.
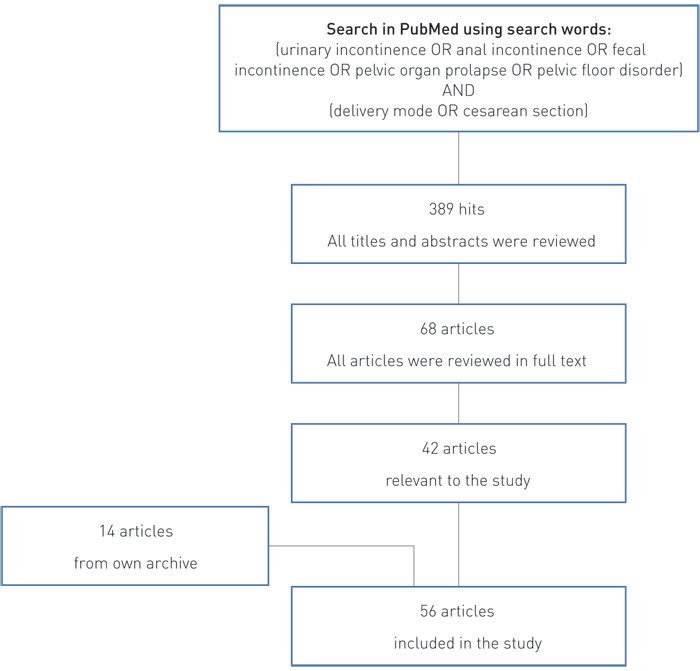
We did not search primarily for systematic review articles and meta-analyses but we emphasise findings from seven such articles in our analysis, since in these types of studies underlying studies have been quality assessed and relevant outcomes are summarised from larger populations. Studies that are not included in articles of this type are rendered in summary form, taking into account whether they support or refute the findings from the meta-analyses and the systematic review articles. In some cases these studies have been published after the review article, while other studies are included here because they provide supplementary information with a reasonable degree of methodological quality.
Randomised studies are scarce, since it is not ethically defensible to treat vaginal delivery and caesarean section as equivalent methods in the great majority of cases. Other indicators of quality that we highlighted were size of the study population, use of validated instruments to measure outcomes, classification of degree of severity of the different conditions, and information on and possible adjustment for relevant confounding factors.
Results
The search results are described in Fig. 1. There was a large degree of heterogeneity in the studies, and therefore we did not find it appropriate to reanalyse the raw data.
Urinary incontinence
In a systematic review article in which the underlying figures were reanalysed, it was estimated that the prevalence of urinary incontinence three months postpartum is on average 30 % in women with spontaneous vaginal delivery, while for women who were delivered by caesarean section the corresponding figure is 15 % (8). This is supported by other studies (9, 10).
How does this look following the postpartum period? In a review article the prevalence of stress incontinence is estimated to be 23 % for those who give birth vaginally, compared to 10 % in the caesarean section group more than one year after the birth (11). A number of single research studies support these findings (12) – (30). A study of 4,200 women conducted six years after the delivery showed that those who had only given birth vaginally and those who had given birth both vaginally and by caesarean section had an approximately equal prevalence of urinary leakage (26 % and 28 % respectively) (14). However, the prevalence among those who had only given birth by caesarean section was 14 %. Correspondingly in 15,300 Norwegian women we found a prevalence for urinary leakage of 24 % in the group that had only given birth vaginally and of 16 % in the caesarean section group (15).
Several studies report differences between the groups, but these do not have the statistical power to determine an effect due to the inclusion of an insufficient number of participants or too great an age span between the participants (31) – (36). The Term Breech Trial is the only randomised controlled study of mode of delivery (8). In this article we treat this as an observational study due to significant overlap between the randomised groups. Two years after delivery there was no significant difference between the groups with regard to urinary leakage when they were analysed as they were randomised (intention to treat), but the difference between the groups that the women actually ended up in was as much as 9 % (26 % incontinent in the vaginal delivery group and 17 % in the caesarean section group) (37).
With respect to degree of severity, it was reported in one of the systematic review articles that the prevalence of severe stress incontinence did not vary significantly between the groups (2.0 % in the vaginal delivery group versus 1.7 % in the caesarean section group) (11). In one Swedish study, however, it was found that vaginal delivery gave a hazard ratio of 3.1 (95 % CI 2.5 – 3.8) for subsequent surgery for stress incontinence compared to caesarean section (38).
Several factors can weaken or strengthen the correlation between mode of delivery and urinary incontinence. As mentioned above, an important factor is women’s age at the time of investigation. In the EPINCONT study we found that women aged over 50 years no longer had any protective effect from having delivered by caesarean section for each of their births (15). This was also true for moderate and severe incontinence. These findings have since been confirmed by others (12, 39).
Other factors that may have a negative influence are older age at first birth (40) and primiparity (41). It appears that a woman must give birth to all her children by caesarean section in order to achieve protection against long-term incontinence (14, 23). Incontinence in pregnancy increases the risk of later incontinence, both postpartum and later in life (9, 18, 21, 42), but this is nevertheless not a predictor of benefit from giving birth by caesarean section to protect against urine leakage (9, 43).
Anal incontinence
The results are less clear for anal incontinence. Meta-analyses are difficult to conduct because of large differences between studies with regard to prevalence of anal incontinence and data collection methodology (44).
The short-term effects of mode of delivery in the first year after birth were investigated in a meta-analysis (45), which found a significant odds ratio for anal incontinence of 1.3 (95 % CI 1.04 – 1.7) for spontaneous delivery compared to caesarean section. A single research study supports this conclusion (29). However, several other single research studies found no differences between the two groups in the postpartum period (33, 46, 47).
With regard to permanent consequences, there are no convincing differences between the two modes of delivery. In a cohort study of almost 4,000 women, no significant difference was found in the prevalence of faecal incontinence based on mode of delivery either six or twelve years after the birth (23, 48). The conclusion is the same in several other studies (13, 22, 24, 37, 49). There are studies that indicate that caesarean section may protect against faecal or anal incontinence beyond the postpartum period, but they are in a minority (20) and frequently have methodological defects such as low statistical power, which meant that the findings were not significant (25, 50, 51).
A key question with regard to anal incontinence is whether this occurs primarily in the subgroup with anal sphincter rupture. In a Norwegian study of women with anal sphincter rupture postpartum, the prevalence of anal incontinence was 38 % (52). A crucial problem both in research terms and clinically is that diagnosis and recording of anal sphincter rupture can vary in quality.
A systematic review article concluded that third or fourth grade perineal tear (i.e. anal sphincter rupture) was the only aetiological factor in delivery that was clearly associated with anal incontinence (53). In a study investigating faecal incontinence, the prevalence was the same in the caesarean section group and in the group that had delivered vaginally without clinically diagnosed anal sphincter rupture (8 % in both groups) (33). However, the prevalence was significantly higher in a group of women with anal sphincter rupture following vaginal delivery (17 %). Other studies also indicate that vaginal delivery in itself is not a risk factor for anal incontinence if the anal sphincter is undamaged (54) – (56).
Obstetric factors may be significant for the correlation between mode of delivery and anal incontinence. It is considered that episiotomy should not be performed routinely (54, 57) – (60). Operative vaginal delivery using forceps or vacuum extraction increases the risk of anal sphincter rupture (54, 61) – (64) and thereby the risk of anal incontinence (54, 65). A Norwegian study shows that anal sphincter injury during the first delivery provides an odds ratio of 4.3 (95 % CI 3.8 – 4.8) for repeated anal sphincter injury at the next delivery (66).
Pelvic organ prolapse
Most of the studies indicate that caesarean section protects against prolapse, both in the short (67, 68) and long term (20, 24, 35, 38, 69) – (72), but in a Danish registry-based study no difference was found (73).
A large multi-centre study reported significantly less anatomical prolapse (measured using standardised methods of gynaecological examination) in women who had only delivered by caesarean section compared to those who had only delivered vaginally (odds ratio 0.11; 95 % CI 0.03 – 0.38) (71). When it came to reported symptoms of prolapse there was the same tendency, but the findings here were not significant (odds ratio 0.84; 95 % CI 0.69 – 1.02) (71). These findings are supported by others (24, 38, 69). Several studies point to a dose-response effect of vaginal delivery for the risk of prolapse (38, 69) – (71, 74). The effect does not appear to decrease in older age groups (38).
Discussion
Overall the research indicates that caesarean section may protect against urinary incontinence in women of fertile age, but the effect does not persist when the women become older and the prevalence of incontinence is highest. For anal incontinence, anal sphincter rupture is of primary significance and not vaginal delivery per se. Strategies to prevent such ruptures are far more important than using caesarean section to avoid anal incontinence. The risk of pelvic organ prolapse following vaginal delivery is well documented, and here we also see a dose-response effect for number of children.
Knowledge of how pelvic floor dysfunction occurs is useful for the development of preventive strategies and treatment. Caesarean section in itself cannot be called a good prevention strategy since this procedure still has many negative consequences for mother and child (37, 75). However, pelvic floor training is well documented for preventing urine leakage and also appears to have an effect on prolapse symptoms, and the financial and medical costs of this treatment are low (76, 77).
There is an interplay of many factors in the development of pelvic floor dysfunction: symptoms can change over time and vary with lifestyle factors and other diseases. This complex interaction is instructively demonstrated by DeLancey and colleagues (Fig. 2, Fig. 3) (78).
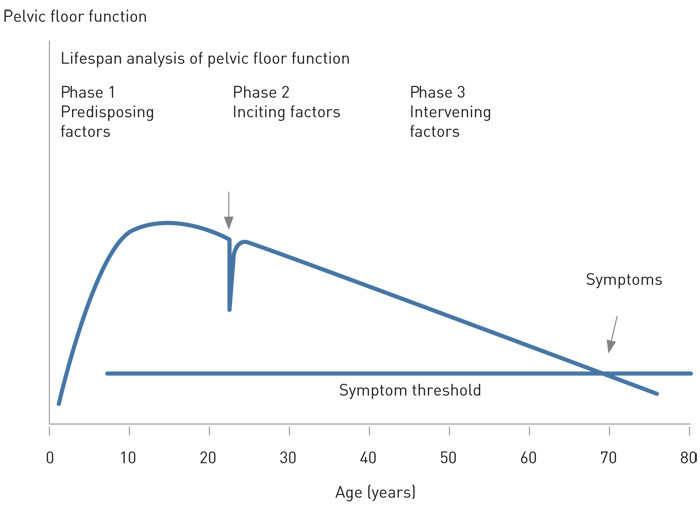
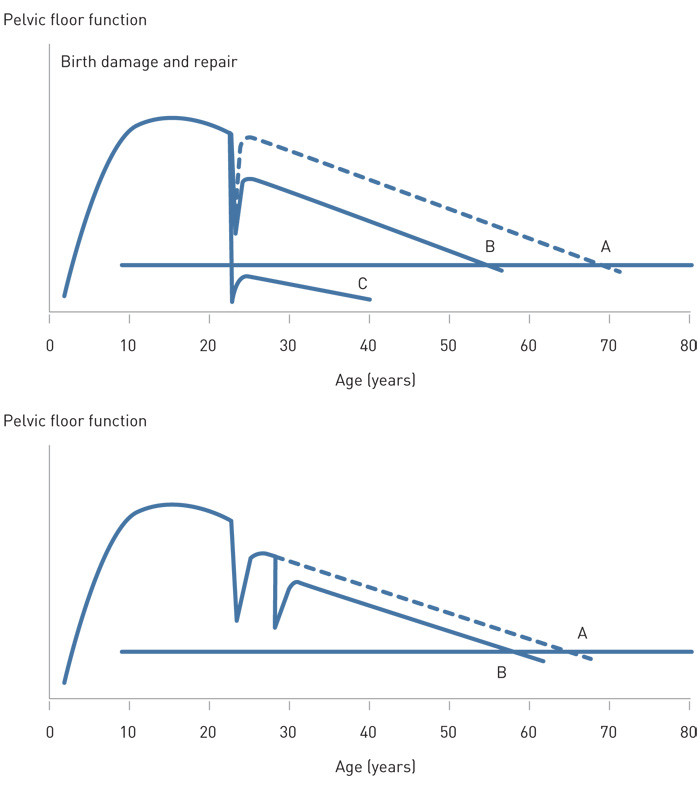
Significant changes have taken place in the indication for caesarean section in the past 30 – 40 years. An increase in obesity (also among pregnant women) and increasing age at first delivery have a bearing on the development of pelvic floor dysfunction. It is not yet clear how mode of delivery has a part to play in this.
It is argued that an optimal caesarean section rate is around 10 – 12 %, based on a balance between risk and benefits for both mother and child (79). In most high-income countries the current rate is above this level and the proportion of caesarean sections is rising. In a global perspective the effort to improve maternal health should be prioritised in countries where access to obstetrics (including necessary caesarean sections) is low. Further development of obstetric methods in high-income countries, for example to prevent anal sphincter ruptures, is a strategy which will also be of benefit to women in low-income countries.
Our search strategy does not conform to the stringent requirements of a systematic review article. We believe nonetheless that the literature in this field is well covered in this review. The main weakness of our study is the variable quality of the underlying data. Although epidemiological studies in this field have greatly improved methodologically in the last decade, there are still a number of challenges – not least in terms of definition and recording of the conditions in question. There is also a significant variation in the degree of severity of the three conditions discussed here. Many studies make a poor distinction between mild symptoms that women can live with and conditions requiring treatment.
Conclusion
A normal vaginal delivery causes significant strain on the pelvic floor and can result in some women of fertile age developing urinary incontinence. Vaginal delivery is an even greater risk factor for pelvic organ prolapse. Vaginal delivery without anal sphincter rupture is not thought to increase the risk of anal incontinence.
Caesarean section as a primary method of prevention at population level does not have a beneficial value that is proportional to the effort and the negative consequences it entails. We do not have sufficiently reliable data to be able to identify subgroups at high risk of pelvic floor injuries – those who could benefit from delivery by caesarean section.
MAIN MESSAGE
The prevalence of urinary incontinence and pelvic organ prolapse is lower in women who have only delivered by caesarean section than in those who have delivered vaginally.
There is no basis for identifying sub-groups with a high risk of pelvic floor injury, with the exception of women who have previously had an anal sphincter rupture.
Caesarean section will have a limited primary preventive effect on pelvic floor dysfunction at a population level.
- 2.
Abrams P, Cardozo L, Khoury S et al. Incontinence. Paris: ICI; 2009.
- 4.
D’Souza R, Arulkumaran S. To ‘C’ or not to ‘C’? Caesarean delivery upon maternal request: a review of facts, figures and guidelines. J Perinat Med 2013; 41: 5 – 15. [PubMed]
- 5.
Medisinsk fødselsregister, statistikkbank. Bergen: Folkehelseinstituttet, 2012.
- 6.
Health at a glance 2011: OECD indicators. www.oecd-ilibrary.org/sites/health_glance-2011-en/04/09/index.html;jsessionid=cd2hlkescfjn6.x-oecd-live-01?itemId=/content/chapter/health_glance-2011-37-en&_csp_=c3a4183dfb73fe547b4ee7d62f9a0058 (21.2.2014).
- 7.
Tollånes MC. Økt forekomst av keisersnitt – årsaker og konsekvenser. Tidsskr Nor Legeforen 2009; 129: 1329 – 31. [PubMed]
- 22.
Altman D, Ekstrom A, Forsgren C et al. Symptoms of anal and urinary incontinence following cesarean section or spontaneous vaginal delivery. Am J Obstet Gynecol 2007; 197: 512.e1 – 7.
- 24.
Handa VL, Blomquist JL, Knoepp LR et al. Pelvic floor disorders 5 – 10 years after vaginal or cesarean childbirth. Obstet Gynecol 2011; 118: 777 – 84. [PubMed]
- 38.
Leijonhufvud A, Lundholm C, Cnattingius S et al. Risks of stress urinary incontinence and pelvic organ prolapse surgery in relation to mode of childbirth. Am J Obstet Gynecol 2011; 204: 70.e1 – 7.
- 44.
Nelson RL, Furner SE, Westercamp M et al. Cesarean delivery for the prevention of anal incontinence. Cochrane Database Syst Rev 2010; 2: CD006756. [PubMed]
- 54.
Eason E, Labrecque M, Marcoux S et al. Anal incontinence after childbirth. CMAJ 2002; 166: 326 – 30. [PubMed]
- 60.
Carroli G, Mignini L. Episiotomy for vaginal birth. Cochrane Database Syst Rev 2009; 1: CD000081. [PubMed]
- 69.
Larsson C, Kallen K, Andolf E. Cesarean section and risk of pelvic organ prolapse: a nested case-control study. Am J Obstet Gynecol 2009; 200: 243.e1 – 4.
- 75.
Cesarean delivery on maternal request. Report. Washington D.C.: National Institutes of Health, 2006.
- 77.
Hagen S, Stark D. Conservative prevention and management of pelvic organ prolapse in women. Cochrane Database Syst Rev 2011; 12: CD003882. [PubMed]
- 78.
DeLancey JO, Kane Low L, Miller JM et al. Graphic integration of causal factors of pelvic floor disorders: an integrated life span model. Am J Obstet Gynecol 2008; 199: 610.e1 – 5.