At the end of 2012, more than 7 000 patients were undergoing opioid maintenance treatment (OMT) in Norway (1). This number has increased consistently over recent years. Since OMT was introduced as a nationwide option for opioid-addicted persons in 1998, more than 9 000 patients have participated (2). A significant part of the treatment is provided by GPs in cooperation with the specialist health services and the social services (3).
A number of patient evaluations were undertaken by way of annual status surveys during the period 2004 – 11 (2, 4). The main impression from these studies is that approximately two-thirds of those who start their treatment continue in a long-term perspective, while approximately one-third terminate the treatment.
In addition to the annual status surveys, a number of research projects have investigated the outcomes of the Norwegian OMT programme (5) – (8). The studies show that with regard to outcomes such as death, criminality and somatic morbidity, prevalence/risk is reduced to approximately half in the period when the patients are undergoing OMT compared to the time before onset of treatment. Even though we have considerable knowledge about the benefits of OMT such as it is practised in the Norwegian model, we still know little about those who discontinue their treatment for various reasons.
In 2004 the reform of the care system for substance users was introduced, and with it patients in this category gained patients’ rights. At the same time, a basis was laid for inter-disciplinary addiction treatment. Before 2004, patients could be discharged from the OMT programme if they failed to attend observed intakes of medication, if their behaviour included consistent substance use, if they attempted to sell OMT medication, behaved violently towards staff or fellow patients or attempted to cheat with their urine samples. After the reform, which included harm reduction as a legitimate treatment goal, «sustained substance use» became less relevant as a reason for discharge from OMT. Today, in accordance with new guidelines (9) and established knowledge (10), such involuntary discharge occurs only in exceptional cases.
Our clinical experience indicates that most of those who terminate their treatment do so voluntarily, by requesting to be discharged or by failing to report for treatment. Findings based on studies of registry data indicate that outcomes such as crime and mortality are exacerbated in the «post-OMT period» for the entire group which terminates the treatment sequence (8, 11, 12). On the other hand, we have little knowledge of whether those who discontinue treatment constitute a homogenous group, whether their «post-OMT existence» is stable, or whether their treatment status changes over time.
According to a report from 2004 by SERAF, altogether 90 % of those who underwent OMT did so for the first time, whereas 10 % had experience from previous treatment attempts (13). These observations will soon be ten years old, and there has been progress in the provision of OMT in Norway.
In this article we describe the characteristics and treatment status of persons who discontinued their OMT at the Addiction Unit at Sørlandet Hospital.
Material and method
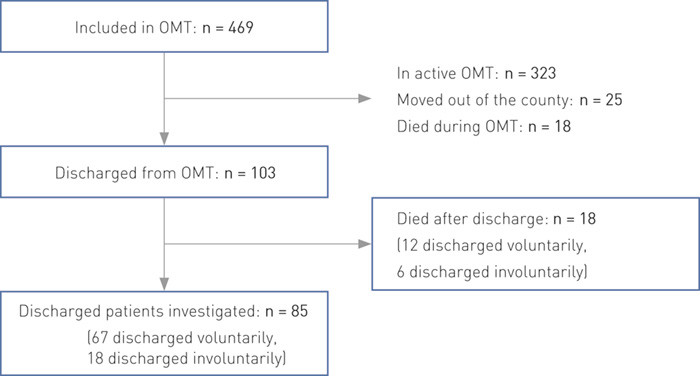
This is a descriptive study. Data were collected in a retrospective review of patient records at Sørlandet Hospital. In the autumn of 2011, a review was undertaken of annual status reports and records of all patients who were or had been admitted for OMT in Vest-Agder county from the start of the programme in the autumn of 1998 through 2009 (469 patients) (Figure 1). As of 31 December 2009, altogether 103 had been discharged. The situational status of these was recorded on two occasions: 31 December 2009 and 30 June 2011. The median observation time from discharge to the two control dates was 1 034 days as of 31 December 2009 and 1 571 days as of 30 June 2011.
The data, which were entered in a spreadsheet, included age, gender, date of initiation of the treatment, number of days in treatment, type of OMT medication, the date of termination of the treatment and the reason for such termination, if any, as well as information recorded on death. Information on situational status was retrieved from the patient records and registered for the two dates 31 December 2009 and 30 June 2011 (a period of 18 months). In some cases, the situational status was based on therapists’ local knowledge .
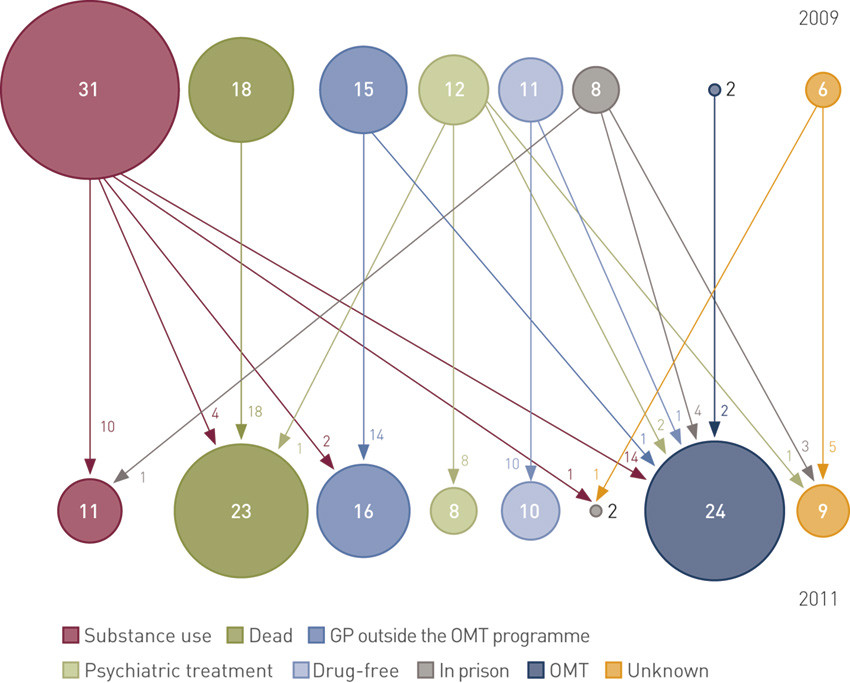
The categories in Figure 2 are mutually exclusive. First it was established whether the patient in question was undergoing various forms of treatment or was institutionalised, and he or she was then categorised under the relevant treatment. It is possible for a person to be in treatment/serving a prison sentence and use substances at the same time, but that person will in this case be categorised as undergoing treatment/institutionalised. Only those who were not undergoing treatment or admitted to a known institution and were known to use substances were included in the «using substances» category.
The project was submitted for assessment by the South-Eastern Norway Regional Committee of Health Research Ethics (REK), which deemed it to be outside the scope of the Health Research Act and thus could be implemented without any need for approval. The project was approved by the Norwegian Social Science Data Services (NSD). The project uses descriptive statistics with medians and averages and concurrent measures of variation. All data were de-personalised.
Results
Characteristics of the entire OMT cohort
In total, 469 patients had been admitted to OMT in Vest-Agder county during the period 1998 – 2009. As of 31 December 2009, altogether 323 (69 %) were still undergoing OMT, while 103 patients (22 %) had been discharged from the treatment (Figure 1).
Of the 323 active OMT patients 72 % were men, and the median age at the start of the treatment was 35 years (range 21 – 62 years). Median time spent in treatment was 1 463 days (range 15 – 4 144 days) (Table 1). Of the OMT patients who were undergoing treatment, 99 (30 %) reported to have been drug-free during the last year (in 2009).
Table 1
Characteristics of patients in medication-assisted rehabilitation opioid maintenance treatment (OMT) at Sørlandet Hospital and those who had been discharged from OMT as of 31 December 2009
| Characteristic |
Patients in OMT |
Discharged from OMT |
| Number |
323 |
103 |
| Age (years) at the start of the treatment, median (range) |
35.0 (21 – 62) |
35.6 (22 – 51) |
| Number of days in treatment, first period, median (range) |
1 463 (15 – 4 144) |
435 (6 – 3 800) |
| Proportion men (%) |
72 |
69 |
| Proportion using methadone (%) |
– |
53 |
| Proportion using buprenorphine (%) |
– |
26 |
| Proportion using both methadone and buprenorphine (%) |
– |
21 |
| Proportion voluntarily discharged (%) |
– |
77 |
| Proportion to later restart OMT (%) |
– |
28 |
Characteristics of 103 patients who terminated their OMT
Those who had been discharged were comparable in terms of age and gender distribution to the patients who were in treatment, but had on average spent a shorter period in OMT (435 days compared to 1 601 days) (Table 1). Of the 103 patients discharged, 28 % had completed more than one period of OMT as of 31 December 2009.
Reason for terminated treatment and discharge
Of those who had been discharged from OMT as of 31 December 2009, one-half (n = 52) had been discharged because they did not want to continue the treatment or failed to report for treatment (discontinued their medication independently). Other causes (mutually exclusive categories) for discharge included that the patients considered themselves drug-free and saw no need for further treatment (n = 19), wanted another form of treatment to be administered by their GP (n = 11) or had reverted to considerable substance use (n = 21).
Altogether 23 % were defined as involuntarily discharged (Figure 1). The proportion of involuntary discharges before and after the reform of the care system for substance users on 1 January 2004 amounts to 44 % and 8 % respectively.
A total of 21 persons had been discharged for reasons of substance use, of which 16 had been discharged before the reform of 2004. Altogether 15 had been discharged involuntarily. After the reform, five persons had been discharged for reasons of substance use, of which four on an involuntary basis.
Status of discharged patients as of 31 December 2009 and 30 June 2011
Of the 103 patients discharged as of 31 December 2009, altogether 18 had died. For the remaining 85 we were able to find information on 79 individuals (Figure 2).
In 2009, there were 31 who had an uncontrolled use of substances and eight were in prison – i.e. 39 of the 79 were outside of regular addiction treatment. Another 29 were in some form of medical care (addiction or psychiatry), whereas 11 persons were described as drug-free, seven of whom had ceased to use substances after a planned gradual cessation of OMT medication.
In the observation made 18 months later (30 June 2011) a change of situational status had occurred in 36 of the persons who had been discharged in 2009 and were still alive (Figure 2). Fewer had an uncontrolled use of substances at that time (n = 11), whereas more of the patients were undergoing OMT or received maintenance medication from their GP (n = 40). The largest group for whom the situational status had changed had reverted from uncontrolled substance use in 2009 and back into OMT (n = 14), whereas one-third of those who had an uncontrolled use of substances in 2009 had the same status in 2011. There was a considerable stability in the groups who were under medical treatment by a GP and among those who were drug-fee. Ten of the eleven patients who were drug-free in 2009 continued to be drug-free in 2011.
Over 18 months, another five persons had died. Of all those 23 who died after discharge from OMT, altogether 13 cases were described as overdose-related. The mortality rate during the period 31 December 2009 – 30 June 2011 among discharged patients for whom information is available for 2011 amounted to four deaths per 100 person-years.
Discussion
Those who terminated their OMT in our study constitute a heterogeneous group, and the reasons for their discharge were varied. Their mortality was high. After the cessation of OMT there was considerable instability with regard to situational status over time, but there were many who returned to periods of maintenance treatment.
Our study showed that 77 % of the discharges from OMT during the observation period were undertaken voluntarily. The introduction of the reform of the care system for substance users in 2004 established a clear distinction. Before 2004, the proportion of involuntary discharges amounted to 44 %, after 2004 this proportion declined to 8 %.
Of the surviving patients who were discharged, nearly half were back in maintenance treatment in June 2011, either in the form of OMT or with another substitution medication administered by a GP. In other words, nearly one-half alternated between being in and outside of OMT.
In our material approximately one in ten of those who had terminated their OMT were considered to be drug-free or in medication-free treatment in June 2011. This indicates that a small number of OMT patients do well without substitution treatment over time. Those who succeed in achieving a drug-free life after OMT are characterised by having ceased to use substances, a desired and planned tapering off of medication and a network consisting of drug-free friends/family members (14).
Untreated opioid-addicted persons have a high mortality rate. International studies have estimated this rate at between 2 % and 4 % per year (15, 16). In Norway, the mortality rate was found to be 2.4 % per year for those who were on a waiting-list for OMT and a mortality rate of 1.4 % for those who were undergoing treatment (5).
In this study, the mortality rate for those who had terminated their OMT amounted to 4 % per year during the period 2009 – 2011. Most deaths affected the group described as substance users in 2009. Terminated OMT and continued substance use outside of OMT appears to be a combination resulting in a high risk of death. The observed mortality rate is somewhat higher than a previously documented national estimate of mortality after OMT (3.4 % per year), based on data from 1998 – 2003 (5). More than 50 % overdoses as a cause of death following termination of treatment, as observed in this study, concurs with the national estimate (12).
In a Swedish study of 38 patients who had remained under stable methadone treatment for more than ten years, it was found that those who were involuntarily discharged from the treatment had a poorer outcome than those who tapered their medication voluntarily, in terms of substance use and perceived quality of life (14). Thirteen patients attempted to taper their methadone treatment voluntarily in the course of 15 years. Seven did this successfully and lived a reportedly opiate-free life (14). Most of these had stable family and social conditions when they terminated their OMT. The proportion of drug-free patients in Vest-Agder county was somewhat lower than in the Swedish study, but viewed as a whole, these studies indicate that only a small proportion of those who terminate their OMT succeed in maintaining a drug-free life in the long term.
According to the Swedish study, characteristics of those who succeeded in maintaining a drug-free life without OMT medication include many years of stable OMT, establishment of drug-free networks and a desire to taper their medication (14). Only one in ten of those who terminated their OMT in Vest-Agder county lived a drug-free life, compared to one in three of those who remained in OMT over the last year. This is in line with a Cochrane summary showing the benefits of OMT compared to no treatment with regard to overcoming addiction problems (17).
A large group failed to report for OMT (n = 28). Of those who died (n = 23), these non-planned and patient-initiated discharges accounted for a full 39 %. Of those who survived, a large proportion were back in OMT or under medication administered by a GP during the observation in mid-2011.
A recent study from Norway shows that crime as an expression of negative behaviour during the treatment increased gradually over the 100 days prior to the termination of the treatment (18). Hence, it is essential for clinicians to be aware of negative development features, such as increasing substance use and problematic behaviour in the form of crime, and initiate special measures to prevent a premature termination of the treatment sequence. We believe that it is important to establish routines ensuring that new treatment options can be provided at the earliest possible time, thus to reduce the death risk of those who terminate their treatment. Similarly, it will be relevant to assess whether the dosage of OMT medication is adequate or whether a better treatment effect can be achieved by switching to another form of medication (19).
Since OMT is a form of treatment which is based on collaboration between the specialist health services, the social services and the GP, it is essential for all parties to be aware of the risk that may be associated with termination of the treatment and seek jointly to achieve the shared goal: to retain the patient in treatment. In our opinion, it is therefore somewhat disconcerting that nearly one in four GPs do not have a positive view of OMT or have no experience of prescribing OMT medication (3). Even though the main objective of OMT is retention in treatment and rehabilitation, provisions could also be made for a small group – the long-term stably drug-free patients who have a supportive social framework – to attempt to taper their medication in collaboration with the therapists, if they have the desire to do so.
Strengths and weaknesses of the evaluation
This study of a total cohort of OMT patients from the period 1998 – 2009 provides a holistic overview and a systematic summary of treatment results at the department on the basis of all patient records. However, a retrospective review of patient records such as this one will only capture information that the clinicians have become aware of and entered in the hospital’s records. This may cause a bias towards «negative» events that have entailed contact with the hospital, compared to the cases where the patient lives a life without any need for renewed contact with the unit.
The estimates of death, imprisonment and psychiatric treatment will be conservative, since no registry studies or other verification of the information have been undertaken beyond the review of patient records from the OMT department of Vest-Agder county.
Those who terminate their OMT are likely to constitute a group with special challenges related to substance use and co-morbidity when compared to those who remain in the treatment programme over time. In this study we have no specific measures for this possible selection bias.
Patient characteristics and findings from Vest-Agder county largely reflect the national results published in annual status reports and nationwide registry-based studies. The descriptions in our study are therefore deemed to provide a good estimate of reasons for discharge and situational status after OMT in many other regions of Norway.
Lessons for further clinical practice
This study indicates that the group that terminates OMT is predominantly composed of persons who continue to have periods of uncontrolled substance use and a high risk of death.
Even though the majority of those who start OMT stay in this treatment for a long period, a considerable proportion fail to persevere with it. An investigation should therefore be undertaken to reveal possible factors in this treatment option that could help reduce attrition.
A large proportion of those who terminate their OMT later return to make new attempts with OMT or another form of maintenance treatment. Close collaboration with the GPs will therefore be essential for providing follow-up to this group. Provisions should be made to undertake the transitions between different periods or forms of treatment in a unified perspective on patient pathways and continuum of care.
Patients who terminate their OMT should have easy access to readmission without any procedures that may cause unnecessary delay, thus to reduce the risk of complications and death.
MAIN MESSAGE
One in five patients who started their OMT in the period 1998 – 2009 terminated their treatment
The majority of those who terminated the treatment went through periods of uncontrolled substance use and a high mortality risk
- 1.
Waal H, Bussesund K, Clausen T et al. Statusrapport 2012: LAR som det vil bli fremover? Oslo: SERAF, Universitetet i Oslo, 2013.
- 2.
Waal H, Clausen T, Håseth A et al. Statusrapport 2011 – LAR i helseforetakene. Oslo: SERAF, Universitetet Oslo, 2012.
- 3.
Waal H, Brekke M, Clausen T et al. Fastlegers syn på legemiddelassistert rehabilitering. Tidsskr Nor Legeforen 2012; 132: 1861 – 6. [PubMed]
- 4.
Hansen MB, Kornør H, Waal H. Statusrapport for pasienter i legemiddelassistert rehabilitering 2002 – 2003. Oslo: SKR, Universitetet i Oslo, 2004.
- 9.
Helsedirektoratet. Nasjonal retningslinje for legemiddelassistert rehabilitering ved opioidavhengighet. Oslo: Helsebiblioteket, 2010. www.helsebiblioteket.no/Retningslinjer/LAR/Forord (3.5.2013).
- 13.
Moen S, Hansen MB, Waal H. Legemiddelassistert rehabilitering – en livslang behandling? Oslo: SKR, Universitetet i Oslo, 2004.
- 17.
Mattick RP, Breen C, Kimber J et al. Methadone maintenance therapy versus no opioid replacement therapy for opioid dependence. Cochrane Database Syst Rev 2009; nr. 3: CD002209. [PubMed]
Clausen og medarbeidere konkluderer med at det går dårlig med dem som avbryter LAR-behandling (1). For å unngå at pasienter dropper ut av LAR, mener jeg man trenger leger som tar pasienten seriøst og at pasienten ikke blir straffet for ærlighet med reaksjoner som strengere henteordning og hyppigere urinprøver. Dette er ekstremt viktig hvis man skal løse problema. Folk må bli behandlet med respekt, uansett. Ivar Skeie, som har forsket på LAR, fant i sitt doktorgradsarbeid at selv de som sprekker har godt av LAR (2).
Litteratur
1) Clausen T, Åsland R, Kristensen Ø. Pasienter som avbryter LAR-behandling – hvordan går det med dem? Tidsskr Nor Legeforen 2014; 134:1146 – 9.
2) Universitetet i Oslo. Disputas: Ivar Skeie - Rus- og avhengighetsmedisin. http://www.med.uio.no/klinmed/forskning/aktuelt/arrangementer/disputaser/2012/skeie-ivar.html (17.6.14)
Vi er enige i at en god relasjon mellom leger i LAR og pasientene er sentral i LAR-behandling. Det er riktig som påpekt; personer som er i LAR-behandling har lavere risiko for både død, sykelighet og kriminalitet sammenlignet med de som er utenfor LAR (1). Det er derfor sentralt at personer som er avhengige av opioider skal tilbys behandling raskt og uten forsinkende byråkrati, og behandlingen må tilrettelegges slik at pasientene ønsker og klarer å være i behandling. Dersom pasienter utskrives fra LAR, vil de aller fleste leve med høy risiko for tilbakefall til ukontrollert rusbruk, og økt dødelighet (2).
Urinprøvekontroll i LAR er en måte å følge opp behandlingen på, omtrent på samme måte som man måler blodsukker ved diabetes eller INR ved behandling med Marevan. Prøveresultatene brukes til å optimalisere behandlingstilbudet, og gjennom dialog med pasientene, til å motivere for adferdsendring, slik at bedre rusmestring oppnås. Pasienter i LAR skal selvsagt ikke straffes, heller ikke når de har tilbakefall i sin ruslidelse. I sårbare perioder skal ruspasientene tilbys ekstra oppfølging og eventuelt styrking av behandlingstilbudet.
Men, LAR-pasienter er ikke helt som diabetespasienter. De får en medisin som er attraktiv som rusmiddel hos personer utenfor LAR. LAR-pasienter som fortsetter å ruse seg mens de er i LAR, vil kunne fristes til å selge eller bytte bort deler av sine LAR-medisiner. Medisiner på avveie kan forårsake overdosedødsfall hos personer som bruker disse medisinene som rusmiddel utenfor behandling.
Leger i LAR har en kombinert rolle der de både skal bistå sine LAR-pasienter i rehabiliteringsprosessen, og styrke deres behandlingstilbud i perioder med forverring i sykdomstilstanden. I tillegg har leger i LAR et ansvar for å påse at medisinene de forskriver, brukes på rett måte.
I situasjoner med mye rusadferd hos en LAR-pasient, er det legens plikt å påse at LAR-medisiner ikke kommer på avveie, og med det styrke kontrollen med medisinutleveringen. Dette betyr regelmessig observerte inntak av medisin og liten grad av "ta-med-hjem" doser. Når rusmiddelbruken kommer under bedre kontroll, og LAR virker stabiliserende, kan man gradvis gi pasienten større ansvar for å oppbevare egne medisiner igjen. Medisineringsregimene i LAR er en balansegang der det gjelder å finne fram til riktig dose der pasienten føler seg frisk uten abstinensplager, motivere for god rusmestring og samtidig gjøre sikkerhetsvurderinger underveis.
Litteratur
1) Skeie I, Clausen T, Bukten A. Legemiddelassistert rehabilitering - viktig behandling med dilemmaer. Tidsskr Nor Legeforen 2014; 134; 1156-8
2) Clausen T, Åsland R, Kristensen Ø. Pasienter som avbryter LAR-behandling - hvordan går det med dem? Tidsskr Nor Legeforen 2014; 134:1146-9.