An epiphrenic oesophageal diverticulum develops as the result of increased pressure in the oesophageal wall (pulsion diverticulum). The diverticulum is located in the distal 10 cm of the oesophagus, with herniation of mucosa and submucosa through the muscularis propria, usually towards the right in the mediastinum (1). The median size of diverticula varies from 4 cm to 7 cm (range 1 – 14 cm) in different datasets (1). Up to 15 % of patients have two or more diverticula. Oesophageal motility disorders such as non-specific dysmotility, diffuse oesophageal spasm, achalasia and increased pressure in the lower oesophageal sphincter occur in 75 – 100 % of patients (1).
Oesophageal diverticula are detected in < 1 % of upper endoscopies and are assumed to cause 1 – 3 % of all cases of dysphagia (2). Radiological studies indicate that the prevalence of epiphrenic diverticula in the general population is 0.015 % in the USA (3) and 0.04 – 0.15 % in Japan (4). In a more selective dataset from Europe, epiphrenic diverticula were found in 2 % of patients who were examined for swallowing disorders (5). The estimated annual incidence in the USA is about 1 per 500 000 individuals (6). The fact that epiphrenic diverticulum is a rare condition is also reflected in the small datasets in published material, ranging from 3 – 35 patients.
Between 37 and 63 % of diverticula are reported to cause symptoms (1). The most common are dysphagia, regurgitation, pain on swallowing food and weight loss (1). Diverticula that cause mild or no symptoms seldom progress to a symptomatic disease (6). In cases of large, symptomatic diverticula, there is increased risk of complications related to the diverticulum, such as aspiration pneumonia. Conservative treatment targets reflux, if any. In some cases, balloon dilation may be attempted in cases of achalasia with stenosis and increased pressure in the lower oesophageal sphincter (6).
The original surgical procedure was left-side thoracotomy with dissecting free and resection of the diverticulum (1, 2). In cases of concomitant achalasia or increased pressure in the lower oesophageal sphincter it is increasingly common to perform myotomy of the oesophagus on the opposite side of the diverticulum and an antireflux operation, normally with partial fundoplication, to counteract acidic and alkaline gastro-oesophageal reflux (1).
Surgery is increasingly performed in a minimally invasive manner, and most frequently by means of laparoscopy (1). A dataset of 133 patients who underwent surgery in the period 1995 – 2008 (7) revealed that two had died during the operation. Post-operative morbidity was reported in 21 %, including leakage from the oesophagus in 15 % of the patients.
The main purpose of this study was to evaluate the post-surgery results for patients who had undergone surgery for epiphrenic oesophageal diverticulum in the period 2002 – 2012 at Oslo University Hospital, Ullevål.
Material and method
Selection
During the period May 2002 to September 2012, nine patients underwent surgery for epiphrenic oesophageal diverticulum at Oslo University Hospital, Ullevål. The patients were identified by searching on the diagnosis oesophageal diverticulum (K22.5) in the electronic patient records system. We also included two patients who were transferred to the hospital after operations at other hospitals in Ullevål's catchment area.
Patients treated with stents or venting gastrostomy were not included in the dataset. The heads of the surgical departments in Ullevål's catchment area were contacted by telephone for information on whether other patients had undergone surgery.
Variables
Data on pre- and post-operative clinical course were obtained retrospectively from patient records and registered anonymously in a database. We entered the patient’s age at the time of the operation, pre-operative symptoms (symptoms present (yes/no) and frequency of regurgitation), duration of symptoms, pre-operative tests, surgical method, post-operative complications and time in hospital.
Surviving patients as of December 2012 (n = 10) were invited in writing to take part in a retrospective survey. This included an outpatient check-up, at which 24-hour pH measurement was offered on indication to two patients. The patients were offered manometry, which seven accepted.
They answered written questions about symptoms, quality of life and their evaluation of the results of their treatment. Questions about symptoms concerned whether they had a particular symptom or not; for regurgitation, whether the symptom presented less often (daily or weekly) than prior to surgery. Data on symptoms and evaluation of the results of the treatment are reported here.
Swallowing function was assessed using modified Ogilvie’s score, on a scale from 0 to 4 (8). 0 points means that the patient can eat any kind of food, 1 point some solid food, 2 points pureed and liquid food, 3 points liquid food, 4 points complete blockage.
Diagnostics and treatment
Pre-operatively, we perform a CT scan, X-ray of the oesophagus-ventricle-duodenum and/or gastroscopy to determine the size of the diverticulum, its level and orientation in the mediastinum and whether there is a hiatus hernia. Manometry can determine whether the patient requires myotomy of the lower oesophageal sphincter and/or an operation to counteract gastro-oesophageal reflux.
The pre-operative tests for previously operated patients consisted of gastroscopy (n = 9), computed tomography (n = 7), X-ray oesophagus-ventricle-duodenum (n = 5), oesophagus manometry (n = 4) and 24-hour pH measurement in the oesophagus (n = 2). Two patients were diagnosed as having achalasia.
Various surgical methods were used (Table 1). Where the diverticulum was excised, it was dissected free and then excised, after which the m. propria was adjusted over the excision site. Also performed on some patients were Heller myotomy (9) and Dor fundoplication (9).
Table 1
Surgical method for epiphrenic oesophageal diverticulum in 11 patients who underwent surgery in the period 2002 – 2012
| Procedure |
Number of patients |
| Diverticulum excised |
9 |
| By means of thoracotomy |
6 |
| By means of thoracoscopy |
1 |
| By means of laparoscopy with simultaneous myotomy and fundoplication |
1 |
| By means of thoracotomy with oesophageal and ventricular resection |
1 |
| Diverticulum retained |
2 |
| By means of laparoscopy with myotomy and fundoplication |
2 |
Ethical considerations
The study was submitted to the South-East Norway Regional Ethics Committee, which regarded it as a quality control study not subject to the submission requirement. It was then approved by the Data Protection Officer at Oslo University Hospital, Ullevål.
Written consent was obtained for participation in the retrospective survey. Written consent for publication of the article was also obtained from all patients who had undergone surgery and were alive, and from relatives of one deceased patient.
Results
Selection
The median age was 60 (range 53 – 77). Nine of 11 had undergone surgery at Oslo University Hospital, Ullevål. Two patients were transferred to our department because of complications due to leakage from the oesophagus. In response to questioning, heads of surgical departments did not report any more patients who had undergone surgery for epiphrenic diverticula in the catchment area of our hospital during the study period. The median duration of the symptoms prior to operation was three years (range 1 – 12 years).
Surgery
Nine patients had diverticula excised (Table 1). One of them had achalasia and underwent myotomy and fundoplication in addition. One patient had undergone a partial diverticulum resection some years previously. The operation was complicated by leakage from the oesophagus. The patient underwent uncomplicated excision of the diverticulum with open oesophageal and ventricular resection. This patient died before the retrospective survey was conducted. Two patients with achalasia and dysmotility of the distal oesophagus, respectively, had small epiphrenic diverticula that were not excised. Myotomy and fundoplication were performed on these patients.
Post-operative time in hospital was a median of 16.5 days (range 5 – 45 days). For the eight patients without serious complications, it was ten days (5 – 16 days). The median longest diameter of an extirpated diverticulum (Fig. 1) was 5 cm (range 3.5 – 9 cm). The neck of the diverticulum at the oesophagus was a median of 3 cm (range 1.5 – 5 cm).
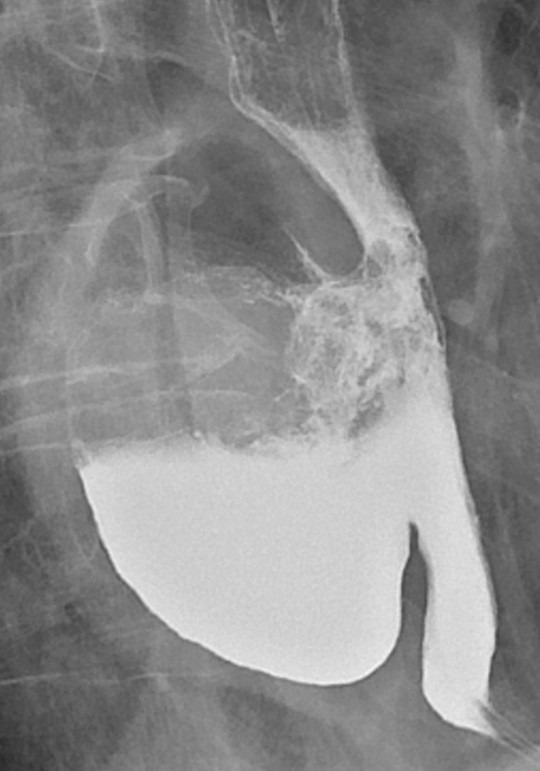
Complications
There were no fatalities as a result of the treatment. Three patients suffered severe complications in the form of leakage from the row of metal sutures in the oesophagus. Two of three developed leakage after resection of a solitary diverticulum. Thoracotomy and thoracic debridement were performed on these two, and temporary installation of a full-coverage oesophageal stent.
One of these patients experienced sequelae in the form of a fistula from the oesophagus to the mediastinum. The fistula was excised a year later. The third patient was found to have minimal leakage of contrast medium from the oesophagus. The patient was kept fasting and given antibiotics, and the leakage healed in the course of a week without stenting.
Symptoms and findings
The survey was conducted a median of 27.5 months (range 2 – 105 months) after the operation. The symptom of pain in connection with swallowing had been eliminated post-operatively, and the number of patients with dysphagia and regurgitation was considerably reduced (Table 2). One patient had mild dysphagia (Ogilvie’s score 1) after myotomy and fundoplication for achalasia. Three patients still had regurgitation, but reduced from daily to weekly episodes. These patients had pre-operative achalasia (n = 2) and low pressure in the lower oesophageal sphincter (n = 1).
Table 2
Pre- and postoperative symptoms in the ten patients who completed the questionnaire in the retrospective survey. Patients reported whether the symptom occurred or not. Dysphagia is defined here as an Ogilvie score of 1.
| Symptom |
Pre-operative |
Post-operative |
|
| Dysphagia |
9 |
1 |
|
| Regurgitation |
7 |
3 |
|
| Pain on swallowing food |
5 |
0 |
|
| Gastro-oesophageal reflux |
Unknown |
2 |
Post-operative manometry was conducted on seven patients a median time of 17 months (range 7 – 94 months) after the operation. Two of the patients also had 24-hour pH measurement. These results were considered in relation to the procedure used and pre-operative findings (Table 3). Patients upon whom myotomy and fundoplication had been performed had better motility in the oesophagus after the surgery than pre-operatively. Two patients had symptomatic gastro-oesophageal reflux at the time of the retrospective survey. The other three patients who underwent excision had normal manometry and no recorded problems.
Table 3
Results of pre- and post-operative manometry conducted on seven surveyed patients. In addition, the degree of reflux revealed by 24-hour pH measurement is given (two patients, pre- and post-operatively). Duration of gastro-oesophageal acid reflux to the oesophagus as a percentage of time per 24 hours with pH
| Patient |
Pre-operative |
Procedure |
Post-operative |
| 1 |
Moderate dysmotility, no reflux |
Myotomy/fundoplication |
Improved motility |
| 2 |
Achalasia |
Myotomy/fundoplication |
Normalisation of lower oesophageal sphincter pressure |
| 3 |
Not carried out |
Excision |
Low pressure in lower oesophageal sphincter Limited reflux (9 %) |
| 4 |
Normal manometry, no reflux |
Excision |
Non-specific dysmotility, significant reflux (28 %) |
| 5 |
Not carried out |
Excision |
Normal |
| 6 |
Not carried out |
Excision |
Normal |
| 7 |
Not carried out |
Excision |
Normal |
The ten patients in the survey reported that they were completely recovered (n = 5) or improved (n = 5) after the operation. One of the patients who had undergone reoperation for leakage and subsequently oesophageal mediastinal fistula refused to undergo further surgery.
Discussion
Most patients in the dataset reported symptomatic improvement following surgical treatment of epiphrenic diverticula, but three developed serious complications in the form of leakage from the row of metal sutures in the oesophagus.
An overview based on 13 studies with 224 patients who had an epiphrenic diverticulum excised, shows lethality of 4 % on average and leakage in the closure line of 12.5 % of the patients (6). There was no lethality in our dataset, but a high leakage percentage (3 of 11 patients). Two patients had be treated with a combination of sanation of infection in the pleural cavity and temporary stenting of the oesophagus to stop the leakage.
All those surveyed reported full or partial regression of symptoms. However, patients with achalasia (n = 2) and low pressure in the lower oesophageal sphincter (n = 1) continued to experience a good deal of discomfort from dysphagia and/or regurgitation. In seven studies where a total of 168 patients underwent operation for a solitary epiphrenic diverticulum, 72 – 93 % experienced excellent or good symptomatic results (1).
Oesophageal dysmotility and increased pressure in the lower oesophageal sphincter are viewed as the most important aetiological factors behind the development of epiphrenic diverticula (1, 6). The patient in this dataset found in the retrospective survey to have low pressure in the lower oesophageal sphincter and distressed by considerable regurgitation and slight reflux would probably have benefited from an antireflux procedure at the same time. Concurrent myotomy also appears to provide protection against recurrence of a diverticulum (10), while myotomy on the opposite side of an extirpated diverticulum reduces the risk of leakage compared with excision without myotomy (6).
Despite excellent results after diverticulum excision for seven patients with an apparently normal lower oesophageal sphincter in this dataset, it seems rational also to perform myotomy on these patients. Although there are no prospective randomised studies comparing open and laparoscopic excision of epiphrenic diverticula, a number of authors (1, 6, 7) recommend that symptomatic, small diverticula be removed by means of laparoscopic procedure. Laparoscopy is also suitable for myotomy and fundoplication.
We included only patients who had undergone surgery, so the review says nothing about how the patients’ symptoms would have developed in the absence of surgery, or what complications might be expected in those who did not undergo surgery. However, a literature review showed progression to disease requiring treatment in 2.8 % of patients who are asymptomatic or only have mild symptoms, and a risk of progression in 92 % of those with symptomatic disease (6).
Conclusion
Most of the 11 patients who underwent surgery for epiphrenic oesophageal diverticulum and were treated at Oslo University Hospital, Ullevål, over a period of 10 years experienced symptomatic improvement, but three developed serious complications in the form of leakage from the oesophagus.
MAIN POINTS
During the period 2002 – 2012, 11 patients who had undergone surgery for epiphrenic oesophageal diverticulum were treated at Oslo University Hospital, Ullevål.
Most experienced symptomatic improvement.
Serious complications were noted for three patients
- 3.
Wheeler D. Diverticula of the foregut. Radiology 1947; 49: 476 – 82. [PubMed]
- 5.
Schima W, Schober E, Stacher G et al. Association of midoesophageal diverticula with oesophageal motor disorders. Videofluoroscopy and manometry. Acta Radiol 1997; 38: 108 – 14. [PubMed]
- 10.
Plackett TP, Meghoo CA, Febinger DL. Recurrent epiphrenic diverticulum after transabdominal diverticulectomy: report of a case and review of the literature. Hawaii Med J 2009; 68: 13 – 5. [PubMed]