In the Cause of Death Registry, «violent death» is defined as death from an external cause, such as injuries and poisonings resulting from accidents, self-harm (suicide) or homicide (2). To reduce the number of such deaths, it is essential to identify the factors that may determine the outcome after such an event. In Norway, some studies of seriously injured patients and people who have died from external causes have been undertaken, which in addition to an identification of those affected have included the mechanism and scope of their injuries. However, there are no unambiguous conclusions regarding the number of these deaths that could have been prevented (3) – (5). A study that not only focuses on descriptive data, such as the circumstances of the accident and the characteristics of those affected, but also investigates whether the injuries were survivable, will provide a better indication of the possible benefits of an increased focus on trauma treatment, early intervention by bystanders and preventive efforts. When the accident has taken place and has been reported, it is crucial that those injured are available for provision of help by the health services. The objective of this study was to assess the number of people who could have been saved by optimisation of their treatment.
Material and method
The study is a retrospective review of deaths from violent causes and accidents in Hordaland County during the years 2003 – 2004. Permission for use of the data and exemption from the duty of confidentiality were granted by the Regional Committee on Medical and Health Research Ethics, Norwegian Social Science Data Service, the Norwegian Directorate of Health and the Director of Public Prosecutions. Lists of people who had died in Hordaland County and whose cause of death was coded as V01-Y81 in the ICD-10 system were retrieved from the Cause of Death Registry. These codes are used for deaths from external causes. Inclusion and exclusion of patients are shown in Figure 1. Persons who died at Haukeland University Hospital after accidents that occurred in other counties were excluded, and so were people who had been resident in Hordaland, but had fallen victim to an accident that had occurred in another county. Patients with plain poisoning as their cause of death were excluded, while patients who succumbed to trauma, drowning, fire or hypothermia while intoxicated were included. Patients older than 64 years with simple fracture injuries sustained from a fall at ground level and who died from sequelae/other illnesses were also excluded. These exclusion criteria were applied in order to permit comparison with previous studies of traumatic deaths in Norway (3). Inclusion and exclusion were primarily based on ICD-10 codes in the Cause of Death Registry. Wherever there was room for doubt, we consulted the patient records.
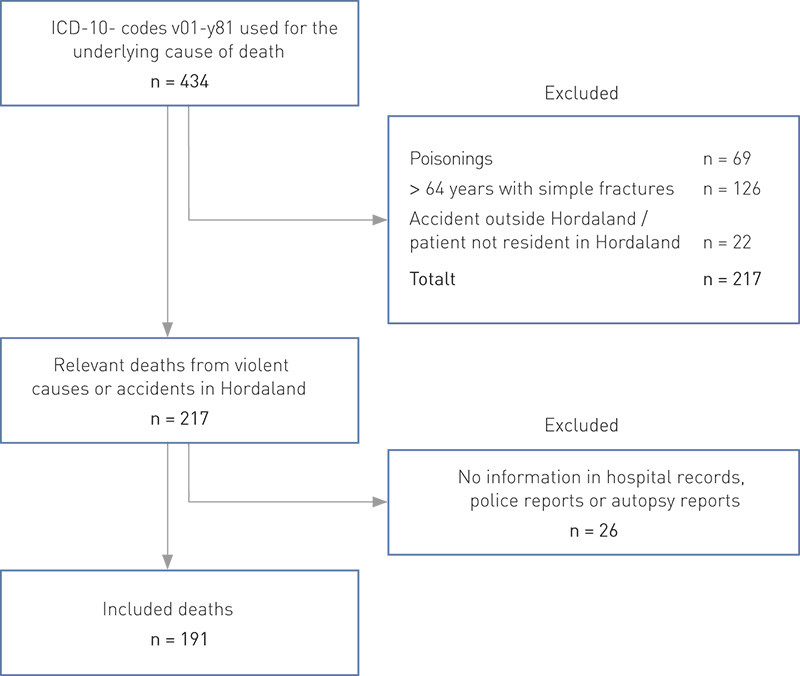
To find information, searches were made in record systems and forensic archives with the aid of personal ID numbers. In the cases where neither a forensic report nor a patient record was available, we collected police reports. No active searches were made in ambulance archives, but ambulance reports had in most cases been appended to the forensic autopsy reports and could be reviewed. For 26 patients, no forensic autopsy reports, hospital records or police reports were available. These patients were excluded from the study. After all exclusions, information on 191 deaths was available. Autopsy reports were available for 173 of the patients.
For each individual patient, we registered information on their age, gender, type of event, place of injury, scope of injury, time of injury, time elapsing from injury to death, influence of medical drugs/intoxicating substances, the type of health personnel who treated the patient, whether cardiopulmonary resuscitation had been provided prior to the arrival of health personnel, and the patient’s clinical status (Glasgow Coma Scale, respiration rate, blood pressure and oxygen saturation (spO₂)), pre-hospital and upon arrival at the hospital.
Two experienced forensic pathologists jointly reviewed the available information for each individual patient and assessed whether the injuries were survivable. This assessment was based on forensic medical experience of examining patients who were dead or severely injured. The assessment of whether the injured patients were available for treatment was based on the time when the injury was reported to the police or the health services. The response time has not been taken into account, and the assessment assumes that the response time was not decisive for the outcome. Those patients who were alive when the accident was reported were counted as available for treatment, unless they had died before being extracted (for example from a car wreck) or unless later examination showed that the patient most likely had no cerebral circulation at the time of reporting. Assessments of whether the patient was alive when the accident was discovered were made post-hoc on the basis of documentation including information in hospital records. In most cases, the records stated that the patient was dead at the time of reporting, or this was evident on the basis of information on common post-mortem changes such as reduced temperature, post-mortem lividity, rigor mortis and decomposition. In a few cases, the time of death could be somewhat uncertain on the basis of ambulance and/or hospital records. In such cases, the discovery of major injuries revealed by the autopsy, for example a severed spinal cord or large contusions to the brain, were interpreted as evidence that the patient had died immediately after the accident.
Results
Altogether 191 deaths were included in the study. Of these, 48 were women and 143 were men, with an average age of 50.7 years (Figure 2). A total of 173 persons were autopsied. The mechanisms of injury are shown in Table 1. Injuries from falls are categorised as blunt force, and elderly patients accounted for a major proportion of this group.
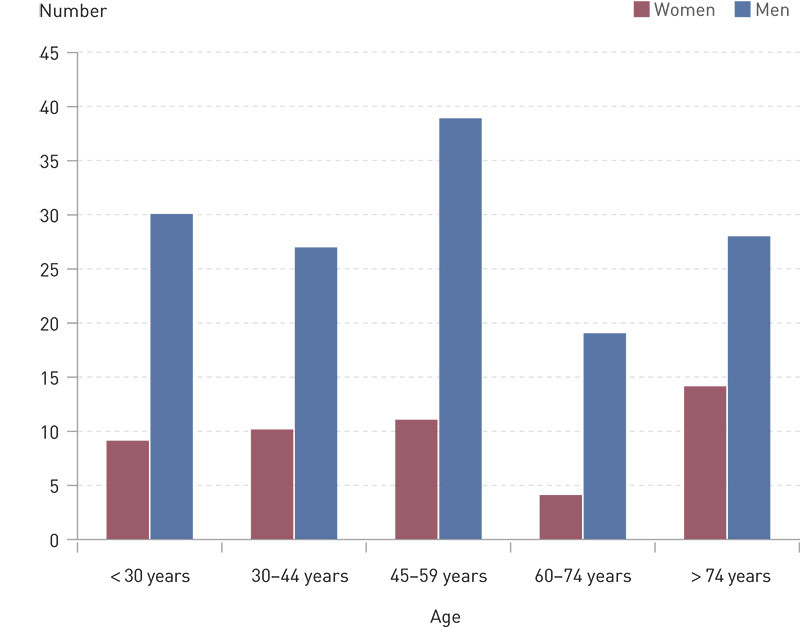
Table 1
Mechanisms of injury for deaths from violent causes and accidents in Hordaland County 2003 – 2004
| Type of event |
Number |
| Blunt force injury |
43 |
| Strangulation/asphyxiation |
42 |
| Traffic accident |
38 |
| Drowning |
31 |
| Gunshot injury |
11 |
| Sharp force injury |
8 |
| Fire |
7 |
| Hypothermia/asphyxiation as a result of an improper recumbent position |
6 |
| Other transport-related accident |
5 |
Analyses of intoxicants, with a broad screening of blood, urine or aqueous humour, were undertaken in all cases when an autopsy had been conducted and material was available (n = 173). No analyses for intoxicants were undertaken in those 18 persons who had not been autopsied. Altogether 45 persons had a detectable amount of alcohol in their bloodstream. This finding of alcohol was not registered in those cases in which it was clear that the alcohol content was caused by decomposition processes. Benzodiazepines were detected in ten of the patients, five had narcotic substances in their bloodstream, and combinations of both types of substances were found in 25 patients. The remaining 88 patients had no intoxicating substances in their bloodstream. In other words, intoxicating substances were found in more than half of all patients exposed to accidents, suicides and homicides.
Based on the scope of injury, it was estimated that 26 patients had injuries that were survivable, and 165 patients had injuries that were not survivable. At the time of reporting, 33 patients were available for treatment, whereas 158 patients were not.
Eighteen patients (9.4 %) had sustained injuries that were survivable and were also available for treatment (Table 2). All of these 18 patients had traffic accidents or falls as their mechanism of injury. All 18 patients had sustained contusions and died from their injuries or sequelae such as organ failure, infections or embolisms (Table 3). Of these 18 patients, 11 were in the age group 70 years or older, while this age group accounted for 41 of 191 persons in the material. Injuries from falls were clearly predominant among these 11 patients. In 12 of 18 cases, it had been recorded that following a comprehensive assessment, no further treatment had been initiated, or life-saving treatment had been discontinued. None of the victims of suicide or homicide had injuries that were survivable while also being available for treatment. In the entire material, first aid had only very rarely been given before the arrival of health personnel.
Table 2
Patients with potentially survivable injuries who were available for treatment
| Survivable injuries |
Non-survivable injuries |
Total |
|
| Available for treatment |
18 |
15 |
33 |
| Not available for treatment |
8 |
150 |
158 |
| Total |
26 |
165 |
191 |
Table 3
Scope of injury/cause of death for patients who were available for treatment and had sustained survivable injuries (n = 18)
| Scope of injury/cause of death |
Number |
| Contusion: thorax, abdomen and pelvis |
5 |
| Contusion: major head injuries |
7 |
| Sequelae (infections, embolisms, organ failure) from contusions |
6 |
| Total |
18 |
Discussion
Identification of those who die and from what causes is essential for drawing any conclusions regarding how trauma treatment can be optimised and what kinds of preventive efforts should be prioritised. Hordaland is a medium-sized county with dispersed settlement as well as urban areas. The county accounts for approximately one-tenth of the Norwegian population (4, 5). A study on the basis of the list of deaths from violent causes or injuries in Hordaland County in 2003 – 2004, issued by the Cause of Death Registry, may therefore be representative for this type of death in Norway. In our material, some of the patients who died from such causes had injuries that were deemed to be survivable while also being available for treatment at the time when the accident was reported. These are the persons who could theoretically have been saved. They had some features in common that distinguished them from the large group for which intervention was deemed possible. A large proportion of them were older than 75 years, and all had died after falls or traffic accidents. In Finland, a country which is comparable to Norway, Korhonen and collaborators have also shown that the number of deaths caused by falls has increased among older people since 1971 (6). Many of the patients who were deemed as having been possible to save were older than 75 years, and the decision to discontinue their treatment had been made after a comprehensive assessment. Many previous studies have pointed out a trend towards a higher percentage of elderly people among those who die from violent causes or accidents (7, 8). It is interesting to note that many of those patients whom we deemed it possible to save were exactly such elderly people who had sustained fall injuries inside or outside their home. In some elderly patients, sequelae may also result in a larger scope of injury than is seen among healthy young people. This indicates that reducing the tendency of older people to fall may prevent deaths (6, 9). If we consider all deaths caused by falls among elderly people, this will account for a large proportion, since prevention will also have an effect in cases where the injuries primarily were non-survivable. This will most likely apply to a large proportion of the patients whom we chose to exclude from the study, for example people over 64 years with simple fractures (Figure 1).
The death certificates documented that for some of the patients with potentially survivable injuries no life-saving treatment, such as respirator or surgery, had been initiated, or active treatment had been discontinued after a comprehensive assessment. Age and co-morbidity play a role, and it is difficult to conclude that more of these 12 patients could have been saved by optimising their initial trauma treatment. This notwithstanding, it is clear that rapid intervention after accidents must always be recommended (10, 11).
Assessment of the mechanism of death-related injury from violent causes or accidents will frequently be complicated by the fact that there are no witnesses to the event itself. In addition to investigations at the site of the accident, examinations of the injured/deceased person will therefore often yield the most reliable information. The quality of this study is increased by a high autopsy rate, especially with regard to assessments of the mechanism and scope of injury; this has also been focused on in other studies (3, 8, 12, 13). Some studies similar to ours have chosen to exclude persons who have died from hanging, strangulation, drowning or fire (8, 14). These account for a large group in our study, and a direct comparison is therefore difficult. We can nevertheless see similar tendencies in terms of the age and gender distribution and in the fact that a large proportion of the victims die at the scene of the accident (3, 6) – (8, 14).
It is characteristic of suicides and homicides that they often lead to a swift fatal outcome. In our material, none of these persons had injuries that were survivable while also being found alive. Prevention of suicides is essential to reduce the number of such deaths (15, 16).
In nearly half of the persons who died, intoxicants were detected by biochemical testing; this could be seen in victims of accidents, suicides and homicides. The use of intoxicants is thus an important negative factor with regard to deaths from violent causes or accidents, even though in some persons the serum concentration was too low to conclude that they had been under the influence of intoxicants at the time of death. Others have also found that the use of intoxicants was associated with fatal head injuries (17) and suicides (18).
Two experienced forensic pathologists have assessed whether the registered injuries could have been survivable. In a large majority of the cases (86 %), the victims had sustained injuries that were deemed to be non-survivable. We may ask whether forensic pathologists assess injuries in the same way as trauma surgeons/anaesthesiologists. The difference in assessment is unlikely to be very large, since forensic pathologists also assess injuries on critically injured patients. Assessment of the injuries after the fact may in some cases present difficulties in obtaining a correct description of the scope of injury. Since the assessment of the various deaths was done in parallel, it was easier to ensure that the assessments did not vary over time.
Previous studies have shown that a large proportion of the victims die at the scene of the accident (3), and this is clearly reflected in our material, in which 93 % of the patients were not available for treatment. The reason was that in a large number of cases, the injury was not discovered before the patient was already dead.
The material shows that once an accident has taken place and has been discovered, few of those who die would have been likely to be saved. This shows that primarily it is preventive efforts that can reduce the number of deaths from violent causes and accidents. Increased attention to the proclivity of older people to fall and prevention of suicides and the use of intoxicants can save lives.
The article is based on a thesis at the second-degree level at the Faculty of Medicine and Dentistry, University of Bergen, 2010 (1).
MAIN MESSAGE
Altogether 18 of 191 patients were deemed to have sustained survivable injuries while also being accessible for treatment.
Half of those who died had intoxicating substances in their bloodstream.
An optimalisation of the trauma treatment or earlier intervention after the time of injury is unlikely to have resulted in fewer deaths.
- 1.
Bakkane Bendixen A, Schrøder Hansen I. Voldsomme dødsfall i Hordaland 2003 og 2004. Hovudoppgåve. Bergen: Det medisinsk- odontologiske fakultet, Universitetet i Bergen, 2010.
- 2.
Folkehelseinstituttet. Beskrivelse av dødsfall som inngår i gruppen «ulykker og voldsom død». www.fhi.no/eway/default.aspx?pid=239&trg=Content_6508&Main_6157=6261:0:25,5944:1:0:0:0:0&MainContent_6261=6508:0:25,5946:1:0:0:0:0&Content_6508=6430:65172:1:6411:1:0:0 (23.4.2013).
- 4.
Hordaland fylkeskommune. Hordalending nummer 500.000 kom til verda i natt. www.hordaland.no/aktuelt/arkiv-nyhende/2013/mars/hordalending-nummer-500000-kom-til-verda-i-natt/?hl=hordalending nummer (29.4.2013).
- 5.
Statistisk sentralbyrå. Folkemengd etter alder, kjønn, sivilstand og statsborgarskap, 1. januar 2013. www.ssb.no/befolkning/statistikker/folkemengde (23.4.2013).
- 7.
Hansen KS, Morild I, Engesaeter LB et al. Epidemiology of severely and fatally injured patients in western part of Norway. Scand J Surg 2004; 93: 198 – 203. [PubMed]
- 11.
Hammell CL, Henning JD. Prehospital management of severe traumatic brain injury. BMJ 2009; 338: b1683.
- 13.
Alfsen GC, Mæhlen J. Obduksjonens betydning for registrering av dødsårsak. Tidsskr Nor Legeforen 2012; 132: 147 – 51. [PubMed]
- 15.
Folkehelseinstituttet. Forebygging av selvmord – faktaark, www.fhi.no/artikler/?id=49751 (23.4. 2013).
- 16.
Nasjonal faglig retningslinje for forebygging av selvmord i psykisk helsevern. Oslo: Helsedirektoratet, 2008.
- 17.
Cryan J, Catháin NO, Curtis M et al. The contribution of alcohol to fatal traumatic head injuries in the forensic setting. Ir Med J 2010; 103: 303 – 5. [PubMed]
- 18.
Lilleng P, Morild I. Selvmord blant alkoholikere. Nord Med 1994; 109: 32 – 3. [PubMed]