High-dose therapy with autologous stem cell support for lymphoma in Norway 1987 – 2008
High-dose therapy with autologous stem cell support (HDT) is a very intensive, highly specialised and resource-intensive therapy. It has been a treatment option for lymphomas for 25 years. Based on results from prospective studies, it has progressed from being an experimental form of treatment to becoming an established treatment for a number of indications (1). In the first years (1987 – 95) it was performed only at the Norwegian Radium Hospital in clinical studies. Following recommendation by an expert group appointed by the Norwegian Board of Health Supervision, the treatment was regionalised in 1996 and has since been performed in all four health regions (on a national level has not been produced until now.
We have investigated how many lymphoma patients who have received HDT in Norway as a whole, by lymphoma type and by hospital, based on place of residence and time of diagnosis. We have also investigated survival following this treatment.
Method
This study is part of a national multicentre study in which a broad spectrum of late effects following HDT for lymphoma in Norway is being studied. All lymphoma patients above 18 years of age who have received the treatment up to and including 31 December 2008 are included. The patients are identified through each hospital’s records of all HDT therapies, cross-checked against reports from HDT meetings, the clinical quality register for lymphoma at the Norwegian Radium Hospital and radiotherapy registers. In addition, the data collected are double-checked through a retrospective review of patient notes. Where relevant, date of death has been obtained from Statistics Norway.
Data for population base by health region are retrieved from Statistics Norway’s annual population census and number of HDT therapies per 100 000 inhabitants is entered. Comparisons between the health regions were made based on the patients’ county of residence at the time of diagnosis.
Statistical analyses
Descriptive analyses are used to describe the patient material. For the survival analyses, observation time is calculated as the time from HDT until death or until 31 December 2011.
The lymphoma patients are divided into three groups: Hodgkin’s lymphoma, aggressive/very aggressive lymphomas (diffuse large B-cell lymphoma, transformed lymphoma, mature T-cell lymphomas, mantle cell lymphoma, Burkitt’s lymphoma and lymphoblastic lymphoma) and indolent lymphomas.
Survival is described using Kaplan-Meier curves, and univariate analysis with log-rank test is used to describe differences between groups. Early mortality is defined as death within 100 days following the high-dose therapy, and comparison between lymphoma groups is analysed using Pearson’s chi-square test. Statistical significance is defined as p < 0.05. The statistical analyses are conducted in SPSS 18.
Ethics
The project was approved in 2011 by the Norwegian Regional Ethics Committee South East (ref. 2011 – 1353).
Results
How many lymphoma patients received the treatment in the period 1987 – 2008?
A total of 726 adult lymphoma patients had received HDT in Norway at the end of 2008. Of these, 465 were men (64 %), and median age at treatment was 48 years (range 18 – 69 years). 230 patients (32 %) received HDT in first remission, while 488 (67 %) received the therapy for relapse or primary chemoresistant/progressive disease (eight unknown – 1 %). Altogether 108 patients (15 %) were treated in the period 1987 – 95 when the high-dose treatment consisted of total body irradiation and high-dose cyclophosphamide and was only performed at the Norwegian Radium Hospital. In the period 1995 – 2008 altogether 618 (85 %) received HDT with BEAM (carmustine (BCNU), etoposide, cytarabine (Ara-C) and melphalan) as a high-dose regimen. Median age for HDT in the first period was 39 years, and in the period 1996 – 2008 it was 50 years.
For the country as a whole, an average of 0.73 patients per 100 000 inhabitants per year were treated in the whole period (1987 – 2008). The annual treatment activity for the whole country gradually increased from 0.12 per 100 000 in 1987 to a peak in 2004 of 1.49 per 100 000 inhabitants (Fig. 1).
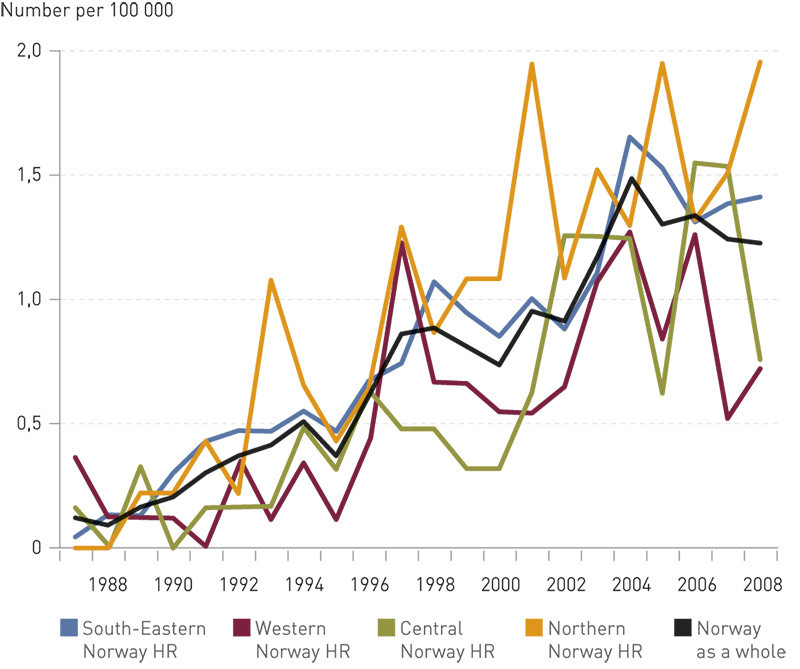
Where were they treated?
In the period 1987 – 95 an average of 12.0 patients per year received HDT at the Norwegian Radium Hospital. In the period 1996 – 2008 an average of 28.3 patients per year were treated there, while the University Hospital of North Norway treated 5.7, Haukeland University Hospital 5.8, St. Olavs Hospital 5.0 and Ullevål University Hospital 2.5.
Figure 1 shows the annual treatment activity per 100 000 inhabitants, based on the health region in which the patient was resident at the time of diagnosis. The average number of treatments annually per 100 000 inhabitants was highest for patients belonging to Northern Norway Health Region, with 0.94, while the corresponding figures for the other health regions were 0.80 for South-Eastern Norway Health Region, 0.58 for Central Norway Health Region and 0.55 for Western Norway Health Region.
Which types of lymphoma did they have?
Table 1 shows number of patients, age and gender distribution and the total diagnoses distributed among the various hospitals. Diffuse large B-cell lymphoma (23 %) and Hodgkin’s lymphoma (21 %) were the most frequently occurring lymphoma types, followed by T-cell lymphomas (13 %), transformed lymphomas (12 %) and indolent lymphomas (12 %).
Table 1
Number of lymphoma patients treated with high-dose therapy with autologous stem cell support (HDT) in Norway, by hospital. Up to and including 1995, HDT was only performed at the Norwegian Radium Hospital, except for two patients at the University Hospital of North Norway who received the treatment in 1995. Number (%) unless otherwise indicated.
| All, 1987 – 2008 n = 726 |
Oslo University Hospital, Norwegian Radium Hospital, 1987 – 95 n = 108 |
Oslo University Hospital, Norwegian Radium Hospital, 1996 – 2008 n = 368 |
Oslo University Hospital, Ullevål, 1996 – 2008 n = 32 |
Haukeland University Hospital, 1996 – 2008 n = 76 |
St. Olavs Hospital, 1996 – 2008 n = 65 |
University Hospital of North Norway, 1995 – 2008 n = 77 |
||||||||
| Age (years): Median (spread) |
48 (18 – 69) |
39 (18 – 60) |
50 (18 – 66) |
55 (23 – 66) |
48 (18 – 65) |
51 (19 – 67) |
50 (18 – 69) |
|||||||
| Age groups (years) |
||||||||||||||
| 18 – 20 |
16 |
(2) |
3 |
(3) |
34 |
(1) |
0 |
(0) |
4 |
(5) |
3 |
(5) |
2 |
(3) |
| 20 – 29 |
101 |
(14) |
23 |
(21) |
49 |
(13) |
4 |
(13) |
11 |
(15) |
8 |
(12) |
6 |
(8) |
| 30 – 39 |
123 |
(17) |
30 |
(28) |
60 |
(16) |
1 |
(3) |
10 |
(13) |
6 |
(9) |
16 |
(21) |
| 40 – 49 |
154 |
(21) |
38 |
(35) |
68 |
(19) |
4 |
(13) |
18 |
(24) |
14 |
(22) |
12 |
(16) |
| 50 – 59 |
202 |
(28) |
13 |
(12) |
106 |
(30) |
15 |
(47) |
21 |
(28) |
21 |
(32) |
26 |
(34) |
| 60 – 69 |
130 |
(18) |
1 |
(1) |
81 |
(22) |
8 |
(25) |
12 |
(16) |
13 |
(20) |
15 |
(20) |
| Gender |
||||||||||||||
| Men |
465 |
(64) |
76 |
(70) |
237 |
(64) |
23 |
(72) |
40 |
(53) |
41 |
(63) |
48 |
(62) |
| Women |
261 |
(36) |
32 |
(30) |
131 |
(36) |
9 |
(28) |
36 |
(47) |
24 |
(37) |
29 |
(38) |
| Lymphoma group |
||||||||||||||
| Diffuse large B-cell lymphoma |
164 |
(23) |
13 |
(12) |
80 |
(22) |
12 |
(38) |
23 |
(30) |
11 |
(18) |
25 |
(33) |
| Hodgkin’s lymphoma |
152 |
(21) |
18 |
(17) |
91 |
(25) |
3 |
(9) |
13 |
(17) |
12 |
(18) |
15 |
(20) |
| T-cell lymphomas |
91 |
(13) |
7 |
(7) |
49 |
(13) |
5 |
(16) |
8 |
(11) |
8 |
(12) |
14 |
(18) |
| Transformed lymphomas |
87 |
(12) |
9 |
(8) |
47 |
(13) |
5 |
(16) |
6 |
(8) |
14 |
(22) |
6 |
(8) |
| Follicular lymphoma |
85 |
(12) |
28 |
(26) |
44 |
(12) |
1 |
(3) |
5 |
(7) |
2 |
(3) |
5 |
(7) |
| Mantle cell lymphoma |
68 |
(9) |
1 |
(1) |
37 |
(10) |
4 |
(13) |
12 |
(16) |
7 |
(11) |
7 |
(9) |
| Lymphoblastic lymphoma |
48 |
(7) |
23 |
(21) |
17 |
(5) |
1 |
(3) |
2 |
(3) |
4 |
(6) |
1 |
(1) |
| Burkitt’s lymphoma |
18 |
(3) |
9 |
(8) |
3 |
(0,8) |
0 |
2 |
(3) |
3 |
(5) |
1 |
(1) |
|
| Other/unspecified |
13 |
(2) |
0 |
0 |
1 |
(3) |
5 |
(7) |
4 |
(6) |
3 |
(4) |
||
Survival
Early mortality, defined as death within 100 days, was 6 % for all lymphoma types collectively, 9 % for aggressive/very aggressive lymphomas, 4 % for indolent lymphomas and 1 % for Hodgkin’s lymphoma. Altogether 411 (58 %) of the 726 patients were alive as of 31 December 2011, with five-year and ten-year overall survival of 64 % (95 % CI 60 – 67 %) and 55 % (95 % CI 51 – 59 %) respectively. Those who were treated for Hodgkin’s lymphoma had the highest survival rate, followed by patients with indolent lymphomas, thereafter patients with aggressive/very aggressive lymphomas (p = 0.01) (Fig. 2).
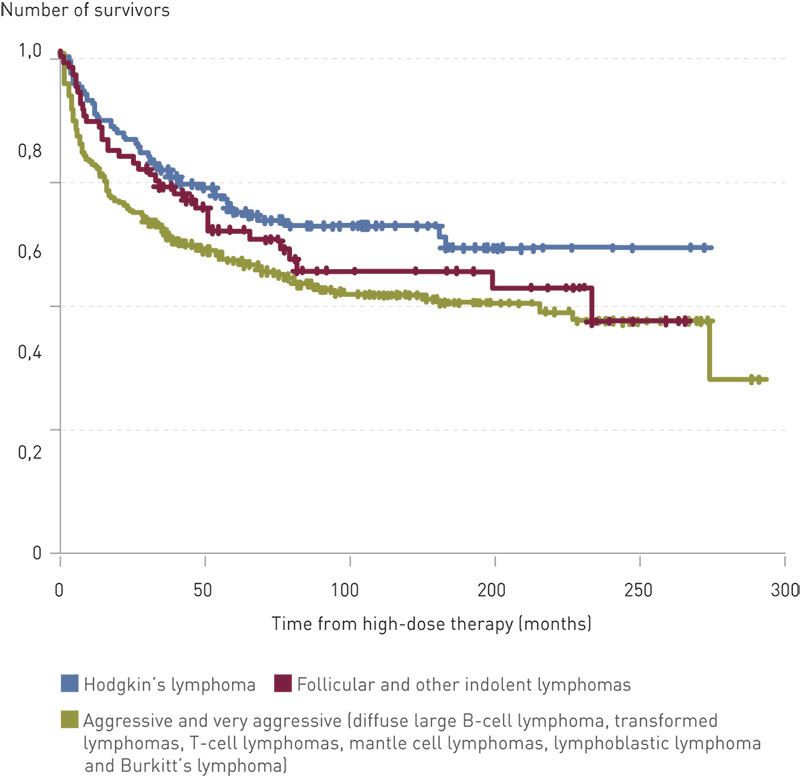
Discussion
There was a steady increase in the number of patients who received HDT for lymphoma from 1987 until a maximum was reached in 2004. In the last few years the figure has remained relatively stable, or perhaps shown a slight decrease. This may be attributed in part to the fact that primary treatment for several lymphoma types has substantially improved in the past 10 – 15 years, which is reflected in the Cancer Registry of Norway’s survival figures for lymphoma (5). The main reason for this is most likely the introduction of rituximab (anti-CD20 antibody), which has resulted in fewer and later relapses of all types of B-cell lymphomas (6). The primary treatment of Burkitt’s lymphoma over these 25 years has improved greatly, so that these patients now seldom need HDT (7). In addition, most of the indications related to lymphoma have been tested over time. In some clinical situations no benefit has been shown for HDT compared to less toxic cancer treatment (1). In refining the treatment, emphasis is now being placed on improved induction therapy to increase the remission rates before the HDT, in order for more people to undergo this treatment and hopefully reduce later relapse (1).
In the first few years the patient selection was stringent, and only young and otherwise healthy patients were considered for HDT. With increasing experience, improved supportive therapy, and last but not least, progress such as stem-cell harvesting from blood rather than bone marrow, it has been possible to achieve reduced treatment-related morbidity and mortality, as well as lower costs (8). The therapy is thereby also relevant for older patients with more comorbidity, and HDT is currently offered to more elderly patients than in the first few years, as illustrated by the figures for the two periods – those treated in the period 1987 – 95 were 11 years younger (median) than those treated in the period 1996 – 2008.
Overall the Radium Hospital of Norway has performed HDT on the greatest number of lymphoma patients. It was the only treating hospital in the period 1987 – 95 and had 60 % of all HDT patients following the regionalisation in 1996.
For Norway as a whole, the number of HDT therapies for lymphoma has been 0.73 per 100 000, which is comparable to the treatment activity in Western Europe and the rest of Scandinavia (9). When adjusted for the population base, the highest number of lymphoma patients who have received HDT are resident in the Northern Norway Health Region, followed by the South-Eastern Norway Health Region, the Western Norway Health Region and the Central Norway Health Region. Our data do not explain what these differences can be attributed to. One reason may be that it is a matter of discussion whether and when in the course of the disease HDT should be offered for particular lymphoma types, for example transformed lymphomas and follicular lymphomas, in relation to other treatment options. This gives more scope for clinical discretion and local tradition. In addition, participation in international studies may be a contributory factor.
Early mortality varied from 1 % for Hodgkin’s lymphoma to 9 % for aggressive/very aggressive lymphomas. This corresponds to previously published studies, in which treatment-related mortality of 1 – 10 % for Hodgkin’s lymphoma (8, 10, 11) and 4 – 10 % for non-Hodgkin’s lymphoma (8, 12, 13) was reported. Since we do not have complete details on causes of death for the whole population, in this study we have defined early mortality as death within 100 days following HDT, irrespective of cause of death. This will therefore also include early lymphoma-related mortality in addition to direct, treatment-related mortality.
We found a five-year overall survival rate of 64 % following HDT for all lymphomas combined. In an American single-centre study published in 2012, five-year survival for Hodgkin’s lymphoma and non-Hodgkin’s lymphoma of 59 % and 62 %, respectively, was found (14). In other studies of specific lymphoma types, three-year survival varies between 55 % and 80 % (11) – (13, 15, 16). More than half of the lymphoma patients are alive ten years after the HDT. Most of the patients had relapsed lymphoma or a disease that was resistant to conventional treatment, so that the prognosis was poor without HDT. In our opinion, it has been a life-saving treatment for most of these patients.
Altogether 411 lymphoma patients were alive following HDT at the start of 2011, and these represent a group of cancer survivors who have undergone very intensive treatment. A significant proportion of these have also had several rounds of chemotherapy and/or radiotherapy before receiving HDT. According to national guidelines, these patients should be followed up with regular controls (17). We know from earlier studies, both Norwegian and international, that certain groups of lymphoma patients have an elevated risk of developing late effects after treatment, such as hormonal dysfunctions, cardiovascular diseases, second cancers and chronic fatigue (18) – (21). The prevalence of and risk factors for late effects have not been specifically investigated in lymphoma patients who have received HDT. This is now being investigated in a national follow-up study in which all the 411 patients who are alive following HDT are also being offered a comprehensive medical control.
MAIN POINTS
The annual number of patients receiving HDT increased from the start-up in 1987 until 2004
The use of HDT was highest for lymphoma patients belonging to Northern Norway Health Region
Many lymphoma patients have been cured of an otherwise deadly disease with the help of HDT
- 1.
Smeland KB, Kiserud CE, Lauritzen GF et al. Høydosebehandling med autolog stamcellestøtte ved lymfom – fra utprøvende til standard behandling. Tidsskr Nor Legeforen 2013; 133: 1735 – 9.
- 2.
Hammerstrøm J, Aasland IL, Telhaug R et al. Høydosebehandling med stamcellestøtte i Midt-Norge. Tidsskr Nor Lægeforen 2004; 124: 2498 – 500. [PubMed]
- 3.
Liseth K, Abrahamsen JF, Ekanger R et al. Overlevelse etter høydosebehandling med autolog stamcellestøtte. Tidsskr Nor Lægeforen 2004; 124: 1374 – 5. [PubMed]
- 4.
Cancer in Norway 2010 – cancer incidence, mortality, survival and prevalence in Norway 2012. Oslo: Kreftregisteret, 2012.
- 12.
Dreyling M, Lenz G, Hoster E et al. Early consolidation by myeloablative radiochemotherapy followed by autologous stem cell transplantation in first remission significantly prolongs progression-free survival in mantle-cell lymphoma: results of a prospective randomized trial of the European MCL Network. Blood 2005; 105: 2677 – 84. [PubMed] [CrossRef]
- 14.
Sweetenham JW, Santini G, Qian W et al. High-dose therapy and autologous stem-cell transplantation versus conventional-dose consolidation/maintenance therapy as postremission therapy for adult patients with lymphoblastic lymphoma: results of a randomized trial of the European Group for Blood and Marrow Transplantation and the United Kingdom Lymphoma Group. J Clin Oncol 2001; 19: 2927 – 36. [PubMed]
- 15.
Schaaf M, Reiser M, Borchmann P et al. High-dose therapy with autologous stem cell transplantation versus chemotherapy or immuno-chemotherapy for follicular lymphoma in adults. Cochrane Database Syst Rev 2012; 1: CD007678. [PubMed]
- 16.
Nasjonalt handlingsprogram med retningslinjer for diagnostikk, behandling og oppfølging av maligne lymfomer nr. 987-82-8081-113-4/2012. Oslo: Norsk lymfomgruppe, 2012.