Several international studies show that a considerable proportion of health expenses are spent on treatment in the final phase of life, but the estimates vary greatly (1) – (6). Some of this variation occurs because the studies have different time frames, include different expenses and consider different groups of patients. A study by Polder and collaborators of expenses in the Netherlands shows that 11 % of all health expenses are devoted to patients in their final year of life (6), but do not include expenses for psychiatry. In their study from Finland, Häkkinen and collaborators include hospitals, psychiatry, drugs and other expenses, and conclude that 14 % of the expenses are devoted to patients in their final year of life, but they focus only on those aged over 65 (1). On the basis of data from Medicare, which largely include people aged 65 and above, studies from the USA show that 25 – 33 % of the expenses for this group are incurred by patients in their final year of life (7) – (10).
In Norway, we have a vibrant and important debate on treatment at the end of life (11) – (13), but we have little knowledge about the costs involved. The only Norwegian study available estimates these costs to be 18 – 26 % of the total (14), but the study is now more than 20 years old and based on estimates, since individual data were unavailable at the time. The literature is thus characterised by studies that are based on various components of expenditure for different periods of time in various sub-groups, and include results that are based on estimates. Using data from the Norwegian Patient Registry, many of these problems can be avoided. We can calculate hospital expenditure on the basis of individual data for the entire population, and we can estimate the real average hospital expenses for men and women who died in 2010 and for those who lived through the entire year.
Material and method
The results in this report are based on a data set in which information from the National Resident Registry identifying which persons died in 2010 and which survived, was linked to data from the Norwegian Patient Registry. The data set comprises 1 294 626 contacts with hospitals, distributed among 729 887 patients. For each of these individuals, we have information telling us whether he or she survived or died in 2010, and his or her use of hospital services in the form of outpatient or hospital treatment. The linkage of the registries was undertaken by the patient registry. Many individuals had more than one treatment episode, but with the aid of the personal identifier in the Norwegian Patient Registry we were able to total up costs at the individual level. The data set contained 27 341 patients who had died in 2010 and who had undergone outpatient or hospital treatment for which costs had been registered in the same year.
The average cost per person who died in each age group has been calculated by dividing the total hospital costs for persons who died in a given age group in 2010 by the total number of persons who died in Norway as a whole in the same age group. The average cost per person who survived 2010 has been calculated in the same manner. Our figures thus represent the average cost per person in the age group as a whole, not only the average cost for those who received treatment. Information on the number of deaths and survivors in various gender and age groups was retrieved from Statistics Norway. The calculation of costs was based on the assumption that a treatment sequence for various diagnostic groups has an average cost indicated by its DRG weight.
Results
Of those who died in 2010, altogether 27 341 (65 %) had visited a hospital for some form of cost-accounted outpatient or hospital treatment during the same year. The total costs for those who died amounted to NOK 4.2 billion, i.e. 10.6 % of the total hospital costs devoted to somatic outpatient or hospital treatment recorded by the DRG system. Figure 1 shows the proportion of hospital costs in various age groups that were devoted to persons who died in 2010. This proportion rises with age: Of all resources spent on people in their fifties in hospitals, 7 % were incurred by persons who died in the course of the year. For people in their seventies the corresponding proportion amounted to 13 %, for patients in their eighties it was 19 % and for those in their nineties it amounted to 29 %.
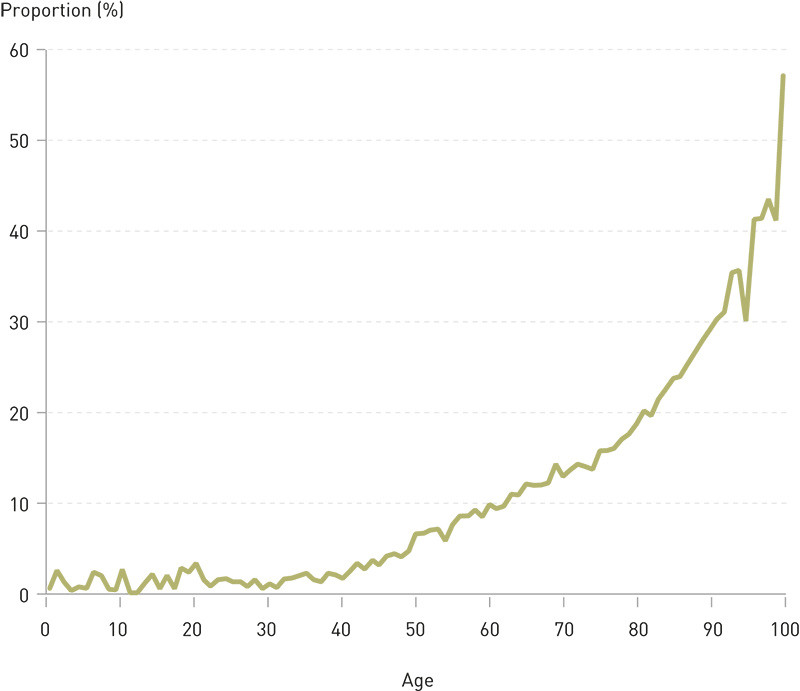
Figure 2 shows average hospital costs for outpatient and hospital treatment in various age groups over 50. For example, the diagram reveals that women aged 70 who died in 2010 on average received hospital treatment worth NOK 157 000 in that year, while the average for those who lived through the entire year amounted to NOK 16 000. The excess cost for those approaching the end of life thereby amounted to NOK 141 000, and the hospital expenses for women in their seventies who died in 2010 were close to ten times higher than for women who lived through all of 2010. The figure also shows that the costs for those who died decreased with age, while the costs for those who survived 2010 increased with age.
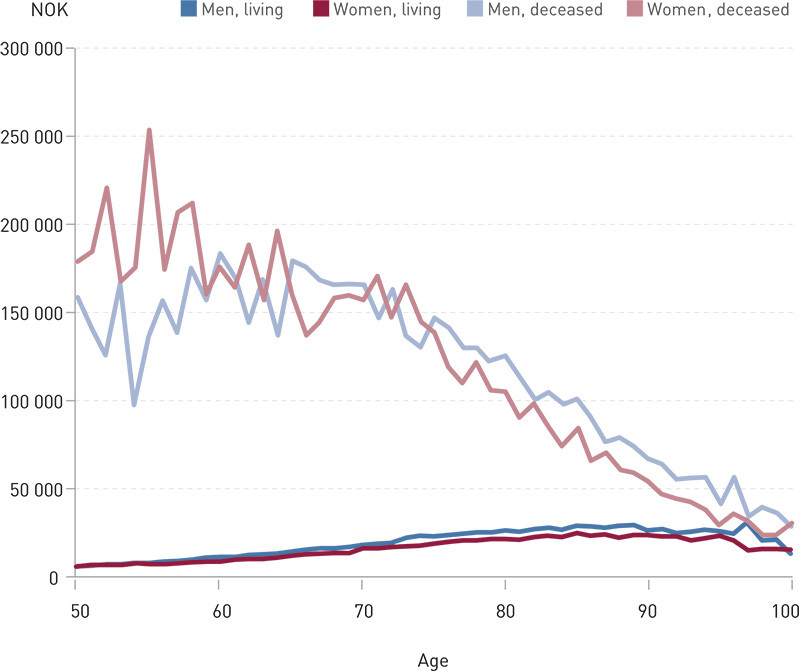
Figure 3 shows the monthly percentage distribution of the total hospital expenses for the last year for men and women in their eighties who died in December 2010. The data set contained 3 096 persons who died in December. Of these, altogether 102 persons were over 80 years of age, and for this group, a total of 868 cost-incurring hospital contacts had been recorded. Of all the expenses incurred during the last year before death, 30 % were incurred during the final month and more than 50 % during the final three months. This pattern could also be identified in other age groups (e-Table 1).
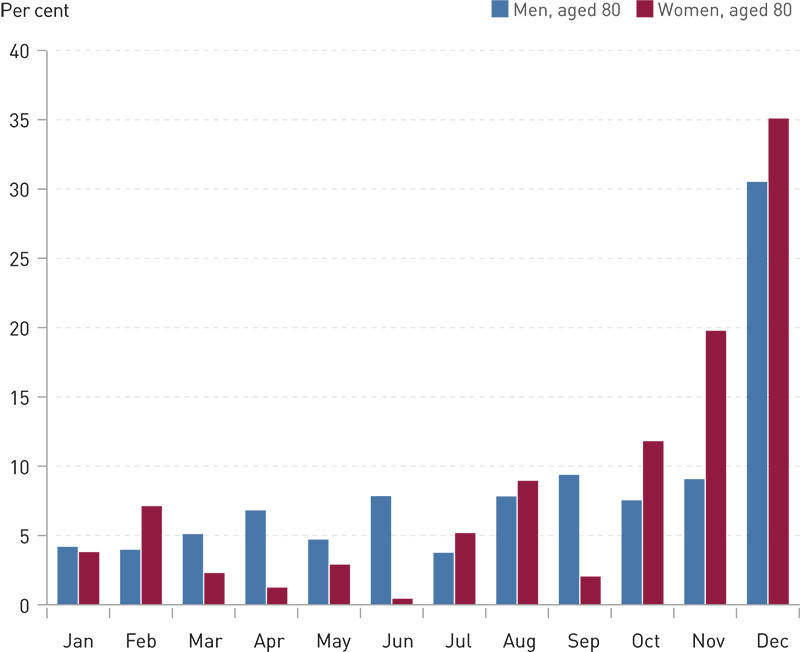
Table 1
Percentage distribution of costs for hospital treatment during the last 12 months prior to death for all persons in their sixties, seventies and eighties who died in December 2010 and were treated in hospital in 2010
| Month prior to death |
||||||||||||
| Jan |
Feb |
Mar |
Apr |
May |
Jun |
Jul |
Aug |
Sep |
Oct |
Nov |
Dec |
|
| Men |
||||||||||||
| In their eighties |
4 |
4 |
5 |
7 |
5 |
8 |
4 |
8 |
9 |
7 |
9 |
30 |
| In their seventies |
5 |
6 |
7 |
2 |
3 |
9 |
5 |
5 |
4 |
8 |
21 |
25 |
| In their sixties |
0 |
0 |
1 |
6 |
6 |
8 |
4 |
2 |
2 |
19 |
5 |
47 |
| Women |
||||||||||||
| In their eighties |
4 |
7 |
2 |
1 |
3 |
0 |
5 |
9 |
2 |
12 |
20 |
35 |
| In their seventies |
6 |
3 |
3 |
3 |
6 |
1 |
3 |
7 |
9 |
16 |
25 |
18 |
| In their sixties |
2 |
3 |
11 |
9 |
5 |
7 |
5 |
3 |
6 |
10 |
10 |
28 |
Discussion
The results show that the total expenses associated with hospital treatment of persons who died in 2010 amount to 10.6 % of total hospital expenditure, but that the average expenditure per person decreased with age (Figure 2). Hospital expenses for women in their eighties who died in 2010 were on average more than NOK 50 000 (33 %) lower than for seventy-year-olds who died in the same year. Corresponding figures for men were a decrease of NOK 40 000 (24 %). The figure also shows that more resources were spent on women than men who passed away at a relatively young age (under 60 years of age), while more was spent on men who passed away at an older age (over 80 years of age).
There are several reasons why expenses vary with gender and age. First, studies show that those who die at an early age often succumb to diseases or injuries that require more hospital resources than those who die in old age (15). For example, many die from cancer at a relatively young age, especially women, whereas people in older age groups more frequently die of a myocardial infarction (16).
International research in this area indicates that one cannot explain the entire difference between the age groups in terms of the prevalence of diseases or events; some of it may also be due to the fact that identical diseases are not treated as aggressively in older age groups (17) – (19). There may be sound medical reasons for this, since elderly patients are unable to sustain the same tough treatment as younger patients, although the literature indicates that elements of age discrimination may also be involved (16, 18). Further studies are required to clarify this.
The variations between consecutive age cohorts illustrate the impact of historical and institutional issues. For example, health and expenses may be influenced by retirement or by having been born into an age cohort that has experienced particular events or epidemics. In addition to random variations, such issues illustrate why the expenses do not follow a straight decline, but vary around a decreasing trend at different age levels.
A potential problem associated with investigating hospital expenses for those who died in a particular year as opposed to those who lived through the entire year is that one fails to capture all death-related hospital expenses: If the costs associated with the cause of death are spread over several years, the investigation will be biased if only hospital expenses in the current year are included. In the data set, this applied in particular to those who died early in 2010, where the hospital expenses most likely had increased from late 2009. A key issue is the extent to which the costs were incurred at the very end of life, or whether they were more evenly distributed over a short or long period prior to death. This is illustrated in Figure 3, which shows two clear trends: First, expenses increased slowly towards the time of death. In analyses of data from the UK, a slight increase could be found as far back as 15 years before death (3). This could indicate that the definition of death-related expenses ought to be expanded. Second, the analysis of our material shows that even though the costs increased long before the time of death, this increase was minor compared to the increase in expenditure during the last few months. Hospital expenses accrued during the final month accounted for 30 % of all costs over the year for persons who died in December. Among patients in their eighties, the final three months prior to death accounted for 50 % of the total cost. We found a similar pattern for the other high-age groups. We may therefore assert that even though hospital expenses start increasing for some time prior to death, the bulk of the cost is incurred during a short period at the very end of life.
As a whole, this means that the figures probably capture a considerable proportion of the hospital expenses associated with the disease that caused death, but that the sum would have been greater if we could have obtained an overview of all death-related hospital expenses over several years. At the same time, by extending the time frame we would also run the risk of including treatment expenses that were unrelated to the end of life. For example, not all costs of treatment in January will necessarily be related to the cause of death if the patient dies in December. The correct interpretation of the figures is therefore «hospital expenses associated with persons who died in 2010», and that this represents a cautious, but not unrealistic, estimate of «hospital expenses towards the end of life».
The observation that large hospital costs are incurred by patients towards the end of their lives has major implications for the extrapolation of health expenditure. Assuming an increase in life expectancy, a traditional extrapolation of hospital expenses involves multiplication of the current average cost in various age groups with the number of people expected in these age groups in the future (20, 21). A problem associated with this method is that it fails to distinguish between expenses associated with the period prior to death, irrespective of age, and the expenses that follow from age alone. Today’s average expenses for people in their seventies include the costs of the many who die at age 70. If life expectancy rises, the proportion of people who die at age 70 will decrease, and the age-related average expenses for people in their seventies will thus also decrease. A more correct extrapolation of expenditure levels should take this into account.
A possible limitation of the analyses can be found in the use of DRG weights as a measure of expenses. In reality, some patients will cost more and others less than the DRG rate. If it costs more to treat a patient in her final year of life than another patient with an identical diagnosis and DRG category, the use of DRG rates will underestimate the costs associated with the end of life. There is also the possibility of an opposite bias: That the treatment of patients with the same diagnosis costs less when the patient is in her final year of life and unable to sustain similarly aggressive treatment. In this case, the DRG rates will overestimate the costs.
The finding that approximately 10 % of all hospital expenses were devoted to patients who died in the course of the year should be treated with some caution in the context of prioritisation. This requires another approach, investigating the extent to which the quality and length of life increase for those patients who receive hospital treatment in what could potentially be their last year of life. While some of these patients will die, many others will have a longer and better life as a result of the treatment. Moreover, many of those who die will have an enhanced quality of life as a result of hospital treatment in the period preceding their death. We have only investigated one half of this assessment, the costs, and can conclude that the costs associated with patients who die in the course of a year account for approximately 10 % of all hospital costs and vary somewhat according to gender and a lot according to age.
We would like to express our gratitude for the useful comments provided by the peer reviewers and the editors of the Journal of the Norwegian Medical Association, as well as colleagues such as Oddvar M. Kaarbøe, who pointed out the potential problems associated with using the DRG rates as a measure of costs. We would also like to thank the Ministry of Finance, the Research Council of Norway and The Commonwealth Fund for their financial support.
MAIN MESSAGE
More than 10 % of total hospital expenses for somatic outpatient and hospital treatment in 2010 were spent on patients who died within the same year.
Hospital expenses associated with patients in their final year of life increased considerably during the three months prior to their death.
The average expenses for hospital treatment of persons who died in 2010 declined with increasing age.
- 4.
Steinmann L, Telser H, Zweifel P. Aging and future health care expenditure: a consistent approach. Forum Health Econ Policy 2007; 10: 1 – 26.
- 5.
Zweifel P, Felder S, Meiers M. Ageing of population and health care expenditure: a red herring? Health Econ 1999; 8: 485 – 96. [PubMed]
- 11.
Kirkevold M, Brodtkorb K, Ranhoff A. Geriatrisk sykepleie: god omsorg til den gamle pasienten. Oslo: Gyldendal Akademisk, 2008.
- 12.
Kaasa S, Haugen DF, Rosland JH. Palliativ medisin–forskning og undervisning i et nytt fagfelt. Tidsskr Nor Lægeforen 2006; 126: 333 – 6. [PubMed]
- 13.
Sørbye L, Steindal S. Omsorg for døende og deres pårørende – hva har endret seg i løpet av en 30 års periode? Omsorg – Nordisk tidsskrift i palliativ medisin 2009; 21: 37 – 42.