In recent years, increasing attention has been devoted to aspects of safety related to the management of emergency patients in Norwegian EDs. At the same time, many EDs have faced a situation in which the inflow of patients has exceeded capacity, and not everybody could be seen by a doctor immediately upon arrival to the ED. This situation has led to an increased interest in triage. «Triage» comes from French, and means «sorting, distinguishing, selecting, selection» (2). In the following, «triage» will be used instead of synonyms such as «assessment of level of urgency» or «prioritisation». Triage was initially used in a medical context during the Napoleonic wars, when wounded soldiers were sorted into three categories: «acute», «can wait» and «cannot be treated» (2). Today, triage is used on a routine basis in military situations, in disaster situations and in EDs (3).
Triage scales with five levels of urgency discriminate better between patients and have a better reliability than three- or four-level scales (4, 5). Internationally several five-level triage scales are in use in emergency departments. The most well-known scales that have been tested for reliability and validity internationally (6) include the Australasian Triage Scale (ATS) (7), the Canadian Emergency Department Triage and Acuity Scale (CTAS) (8), the Emergency Severity Index (ESI) (USA) (9) and the Manchester Triage Scale (MTS) (10). A five-level triage scale has also been developed and tested in Sweden, the Medical Emergency Triage and Treatment System (METTS) (11) (Table 1). An example of a flowchart from the Manchester Triage Scale is shown in Figure 1 (12). A five-level triage scale was used for the first time in Norway in 2004 (13). In 2007, the Norwegian Board of Health Supervision undertook an inspection in 27 Norwegian EDs and found that several EDs did not have a satisfactory system for prioritising patients, and this was claimed to potentially jeopardize the life and health of patients. (14).
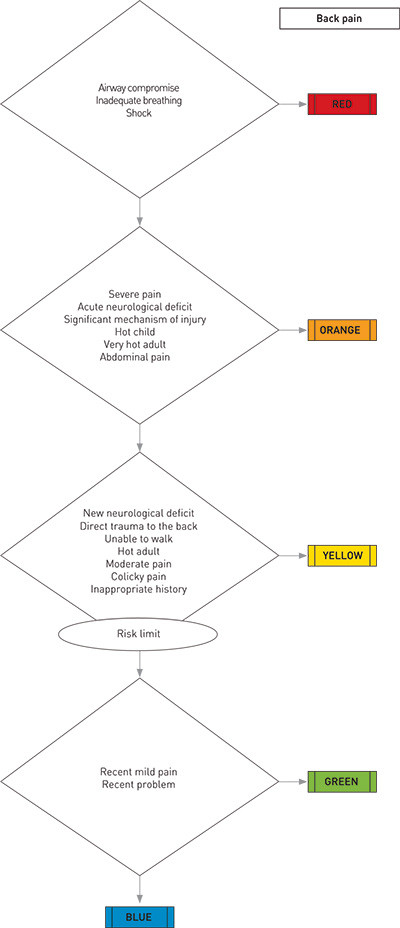
Table 1:
Content of the five-level triage scales that are used internationally
| Australasian Triage Scale (7) | Manchester Triage Scale (10) | Emergency Severity Index (9) | Canadian Emergency Department Triage and Acuity Scale (8) | Medical Emergency Triage and Treatment System (11) | |
| Levels of urgency and time before medical attention (min.) | |||||
| Level 1 | 0 | 0 | 0 | 0 | 0 |
| Level 2 | < 10 | < 10 | Not stated | < 15 | < 20 |
| level 3 | < 30 | < 60 | Not stated | < 30 | < 120 |
| level 4 | < 60 | < 120 | Not stated | < 60 | < 240 |
| level 5 | < 120 | < 240 | Not stated | < 120 | Not stated |
| Decision-making support | Clinical guidelines for each level of urgency | Flowcharts based on presenting complaint | Flowchart based on clinical presentation and expected resource use | List of presenting complaints and associated discriminators | Flowcharts based on presenting complaint and vital signs |
| Proposed goal indicators related to the level of urgency | Time from arrival to treatment Hospitalisation rate Mortality | Completeness Accuracy | Time from arrival to medical attention Length of stay Hospitalisation rate | Not stated | Not stated |
Despite the fact that more than half of all hospitalisations in Norway take place through the EDs (14), no studies of triage in Norwegian emergency departments have been undertaken. Existing knowledge is restricted to personal communication and the report from the Norwegian Board of Health Supervision (14). The purpose of this survey was therefore to describe the organisation of triage in Norwegian emergency departments (triage personnel, physical facilities, training and the use of goals) and to investigate the use of triage scales and systems/tools for decision-making support
Material and method
All the 53 Norwegian public emergency hospitals (15) and three private hospitals with emergency functions identified through Internet searches were included. Department managers were contacted by e-mail. Follow-up was made by e-mail after two weeks, and then by telephone after another two weeks until contact had been established in writing or orally with all institutions. The managers were asked to select the employee who had the best knowledge about the topic to participate.
We used a questionnaire that had been developed for a similar study in Sweden (3). The questionnaire was revised and adapted for Norwegian conditions. Of a total of 27 questions, five pertained to demographic features of the emergency centre’s catchment area, the rest pertained to triage (see appendix). Three of the questions were open-ended, the remaining had pre-defined response categories, and some had a field for comments. Prior to implementation, the questionnaire was tested on nurses who were familiar with the topic. Some adjustments were made on the basis of their feedback, for example in the response categories and the order of questions.
The data collection was undertaken through telephone interviews, prior to which the questionnaires had been distributed to the respondents. Written recording of responses was undertaken consecutively during the interview. All interviews were undertaken from March to June 2010, by the first author.
Descriptive analyses were undertaken with the aid of SPSS version 17. Responses to open-ended questions as well as comments were categorised according to established guidelines for qualitative data (16).
The study was submitted to the Norwegian Social Science Data Services (NSD) and the Data Protection Officer, who both concluded that the study was not subject to notification to them. The respondents and the department managers signed a declaration of informed consent, and were informed that they could withdraw from the study at any time.
Results
Of the 56 hospitals that were asked, 45 participated (80 %). The response rate varied from 50 % in one of the health regions to 83 %, 89 % and 100 % in the three others. Seven university hospitals and 38 local hospitals participated. The reported volume of emergency patients in the EDs in 2009 varied from 810 to 42 000. Altogether 15 of 45 EDs reported to receive waiting-list patients as well as emergency patients.
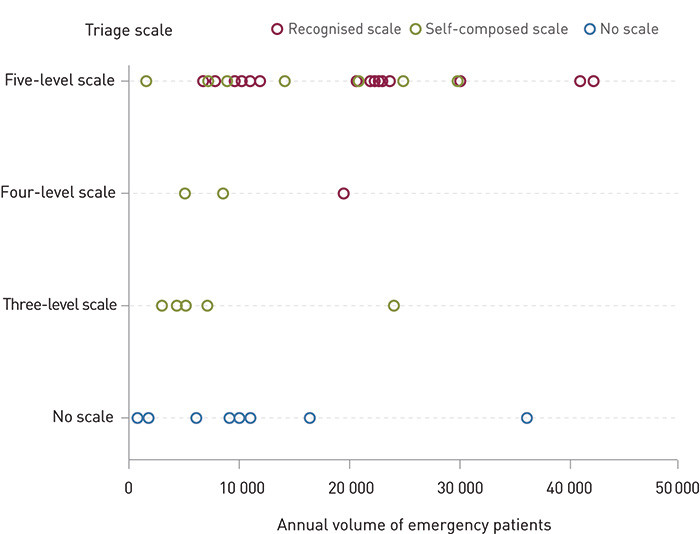
All the respondents reported that emergency patients underwent triage on the basis of a clinical assessment of signs and symptoms (Question 6 in the Appendix). Furthermore, a few reported using another basis for triage. 34 (76 %) reported to use a triage scale, 17 of which were self-composed. 17 of 45 EDs used an established five-level scale. Of these, two (one of which did not report patient volume) had deleted one level, i.e. down to four levels (Figure 2). The MTS, METTS and CTAS scales were used by eleven, five and one EDs respectively; none used the ATS or ESI scales. The self-composed triage scales used varying time frames to specify the maximum waiting time before receiving medical attention, and 12 of the 17 self-composed scales provided no time frame for one or more of the levels. The self-composed triage scales also provided varying decision-making support. Three of these 17 self-composed scales provided algorithms based on the Medical Index, eight of 17 had algorithms based on an assessment of ABCD and/or vital signs and/or signs and symptoms. Six of these 17 scales provided no decision-making support.
Altogether 24 of 45 EDs (53 %) had local guidelines describing which personnel should perform triage. 25 of 45 EDs reported that triage was performed by a nurse, while in 16 other EDs this task could be performed by a nurse (n = 16), an assistant nurse (n = 7), a doctor (n = 11) or a secretary (n = 1). Four EDs did not report who was performing triage. 14 and 15 of the respondents respectively reported to have designated triage personnel and triage area. Furthermore, 31 EDs (69 %) had defined goals with regard to triage, and 21 of these reported to undertake goal evaluation (Table 2).
Table 2:
Organisation of triage in 45 Norwegian EDs
| All EDs (n = 45) | |
| Uses designated triage personnel | 14 |
| Performs only triage | 7 |
| Also performs other tasks | 7 |
| Facilities | |
| Designated triage area¹ | 15 |
| Examination room ¹ | 27 |
| Corridor¹ | 15 |
| Internal triage training | 24 |
| Theoretical teaching¹ | 15 |
| Peer training¹ | 22 |
| Has goals for triage | 31 |
| Evaluates goals | 21 |
| Electronically | 9 |
| Manual measurements/other | 12 |
| [i] | |
[i] ¹ Multiple responses allowed
The EDs required varying degrees of experience and qualifications from their triage personnel. Among the EDs that used nurses and assistant nurses for triage, one reported to require two years’ experience as a nurse, two required one year of ED experience , and another two required two years of ED experience. The remaining EDs had not ticked any of the alternatives (Question 21 of the Appendix). This also applied to those EDs that used doctors for triage. None reported to require postgraduate training. 24 EDs (53 %) reported to require internal triage training for nurses and assistant nurses (Table 2).
There was a tendency for established five-level scales to be used more frequently in EDs with large patient volumes (Figure 2). The same applied to use of especially designated triage personnel and triage area and evaluation of goals (data not shown).
Discussion
Ensuring that the sickest patients receive treatment at the correct time is one of the key remits of an ED. Triage is used to identify these patients. In this study, all EDs reported to triage their patients, and approximately three of four used a triage scale. Many used self-composed scales. Only 17 emergency departments used internationally recognised five-level triage scales.
More than half of the self-composed scales had only three or four levels. These have been shown to discriminate less well between patients and to have a poorer reliability than five-level scales (4, 5). The self-composed scales specified varying times before medical attention should take place, and in some cases no time interval was provided. During the inspections undertaken by the Norwegian Board of Health Supervision in 2007, nurses and doctors had differing views on levels of urgency and the time when the patient should receive medical attention (14). We believe that this may result in delayed medical assessment or unnecessary use of resources. The use of a recognised triage scale with time-specific levels of urgency and a shared nomenclature could prevent this from happening.
Nor did some of the self-composed scales provide any decision-making support. This may lead to differing assessments of the level of urgency, depending on the person who undertakes the assessment. An erroneous decision may lead to undertriage, which at worst may delay treatment and harm the patient (17). Decision-making support of various kinds, such as in the recognised five-level scales (Table 1), may help triage personnel make more consistent decisions (18). Better discrimination between patients, better reliability, shared nomenclature and built-in decision-making support speak in favour of using recognised five-level scales instead of self-composed ones in Norway as elsewhere. It is essential, however, that these scales be tested also in our country.
We found that triage was organised differently in the various EDs. Goal evaluation is a critical aspect? of this organisation. 31 EDs had defined goals, but only 21 of these reported that these goals were being evaluated. Only nine EDs possessed electronic statistics tools for undertaking such evaluations. Existing ICT systems in Norwegian hospitals include few good applications for use in EDs (19), and such applications are essential for evaluation of goals.
Only half of the EDs had guidelines identifying the personnel that should perform triage. The health authorities in some other countries have issued guidelines stating who should perform this task (4, 5). Norwegian health authorities have not issued any guidelines other than stating that triage should be undertaken in a systematic manner (13, 14). This study shows that in Norway, triage is primarily undertaken by nurses. This is in line with international experience (3, 7) – (10, 20) – (23).
Moreover, we found that only half of the EDs reported to impose requirements for triage training. It has been shown that factual knowledge rather than experience has the best effect on triage decision-making (24), and triage training should comprise factual knowledge, for example about the triage scale being used and assessment skills (25). We believe that all triage nurses ought to undertake such training.
Designated physical premises for triage, such as a triage area or a triage room, were uncommon. Several EDs sometimes used the corridor, which could prolong the triage process, affect the decision and at worst result in undertriage (26, 27). In addition, this may violate the right to confidentiality. When new EDs are being planned, inclusion of designated triage premises should be considered.
There was a tendency towards a correlation between the EDs’ reported patient volume and their use of a triage scale and their organisation of triage. One may ask whether triage is necessary in EDs with small patient volumes. However, even these EDs have peak times, and we therefore believe that it is important for them to use recognised triage scales and organise their triage. A precondition for triage to function at peak times is that the personnel is accustomed to practising it. In their recommendation to undertake triage in a systematic manner, the health authorities do not distinguish between small and large patient volumes (13, 14). EDs with small patient volumes tend to have fewer doctors, and in Norway these are often tied up with tasks outside the department. Use of triage may help identify serious conditions that the patients are developing while in the ED, and ensure timely alert of adequate medical competence.
Göransson and collaborators discussed whether poor organisation of triage could be partly caused by the fact that doctors rarely have any obligations to the ED apart from being on duty on behalf of the parent department (3). In some countries there is a major interest on the part of the doctors, and the recognised scales have been developed in collaboration between emergency doctors and nurses or their organisations (7) – (10).
Strengths and weaknesses
Our lack of information about the respondents represents a limitation of our study. The first author conducted the telephone interviews, and this provided an opportunity to clarify misunderstandings or unclear responses during the process. The questionnaire was distributed to the respondents in advance, so that they could prepare for the telephone call. The specific information requested was of a fairly simple nature (see the Appendix), and information that the respondent did not possess could be collected from others. The reported number of emergency patients in the ED is based on the respondents’ answers, and is thus fraught with some uncertainty.
The high response rate indicates that the findings are representative. However, the response rates varied from one health region to another, and there is also a possibility that participation by the EDs that dropped out (n = 11) might have altered the results to some extent. Without being solicited, several of these reported that the reason for their non-participation was that they never performed triage. Hence, there is reason to believe that other EDs than those found in this population fail to use recognised triage scales.
Concluding comments
The use of triage scales and organisation of triage varied between Norwegian EDs. Norwegian health authorities claim that the responsibility for triage rests with the management of the health trust (14), and do not want to introduce a nationwide model (13), in contrast to what is seen in certain other countries (7, 8). As long as the health authorities provide no guidelines concerning triage, practices should be based on international research and trends that indicate use of recognised five-level scales, triage training and use of goals. We believe this could help improve quality in the management of ED patients, but wish to underscore that this is obviously not synonymous with quality, and that many other factors may also have an effect.
The article is based on the first author’s thesis for the master’s degree at the Oslo and Akershus University College of Applied Sciences, 2010 (1).
MAIN MESSAGE
All emergency departments reported to assess patients with regard to level of urgency.
Many emergency departments used self-composed triage scales.
There was considerable variation in how the triage was organised.
Several emergency departments did not evaluate goals for triage.
- 1.
Engebretsen S. Triage in Norwegian emergency departments. Masteroppgave. Oslo: Institutt for sykepleie, Høgskolen i Oslo og Akershus, 2010.
- 6.
Statens beredning för medicinsk utvärdering (SBU). Triage och flödesprocesser på akutmottagningen. En systematisk litteraturöversikt. Rapport 197. Stockholm: SBU, 2010.
- 7.
Australasian College for Emergency Medicine. Guidelines on the implementation of the Australasian Triage Scale in emergency departments. www.acem.org.au/infocentre.aspx?docId=59 (25.11.2009).
- 8.
Canadian Association of Emergency Physicians (CAEP). Canadian Triage and Acuity Scale. http://caep.ca/resources/ctas (1.1.2013).
- 9.
Gilboy N, Tanabe P, Travers DA et al. Emergency Severity Index, version 4: Implementation handbook. Rockville, MD: Agency for Healthcare Research and Quality, 2005.
- 10.
Manchester Triage Group. Emergency Triage. 2. utg. Oxford: Blackwell Publishing, 2006.
- 12.
Manchester Triage Group. Akuttmedisinsk triage. Oslo: Unipub, 2011.
- 13.
Fonn M. Triage når det haster. Sykepleien 2009; 7: 36 – 42.
- 14.
Helsetilsynet. Mens vi venter... – forsvarlig pasientbehandling i akuttmottakene? Rapport 2/2008. Oslo: Lobo Media, 2008.
- 15.
Helsedirektoratet. Offentlige sykehus i Norge. www.regjeringen.no/nb/dep/hod/tema/sykehus/sykehus-i-norge-3.html?id=467556 (1.1.2013).
- 16.
Malterud K. Kvalitative metoder i medisinsk forskning. 2. utg. Oslo: Universitetsforlaget, 2003.
- 19.
Antonsen T, Alsaker M, Bach G. IKT støtte i akuttmottak. Kartlegging og analyse. Rapport fra KITH. Trondheim: KITH, 2009.
- 20.
Purnell LD. A survey of emergency department triage in 185 hospitals: physical facilities, fast-track systems, patient-classification systems, waiting times, and qualification, training, and skills of triage personnel. J Emerg Nurs 1991; 17: 402 – 7. [PubMed]
- 21.
Purnell L. A survey of the qualifications, special training, and levels of personnel working emergency department triage. J Nurs Staff Dev 1993; 9: 223 – 6. [PubMed]
- 22.
Gerdtz MF, Bucknall TK. Australian triage nurses’ decision-making and scope of practice. Aust J Adv Nurs 2000; 18: 24 – 33. [PubMed]