RGPs are obligated to accept accident and emergency (A&E) duty (1). The agreements allow for exemption under certain preconditions, while studies show that far more doctors than those who are formally exempted have resigned from A&E duty (2, 3). The Ministry of Health and Care Services has therefore proposed a stricter enforcement of the RGPs’ A&E duty (4).
A&E work is strenuous. It is often performed under difficult circumstances, with an increased risk of making errors (5). Sometimes the doctor will face dramatic emergencies that he or she is poorly prepared to deal with (6). However, most presenting complaints are the same as those encountered in regular general practice (7, 8), and it has therefore been argued that among doctors, the RGPs are best qualified to undertake A&E work (4, 9, 10).
In a previous study we have investigated which doctors received reimbursement from National Insurance for A&E work in 2004 (2). The RGPs received 51.8 % of all the reimbursements, and we found that older doctors, women doctors and doctors with long lists had low incomes from on-call work. The incomes from on-call work were higher in rural municipalities than in centrally located ones. In 2006 we undertook a questionnaire-based survey of the RGPs’ participation in the A&E scheme. Among the 78 % who responded, 50 % participated fully in the A&E scheme and 15 % participated to a limited extent, while 35 % did not participate at all (3). Here too, the participation decreased in proportion to the doctors’ age, and it was lower among women RGPs and in large and centrally located municipalities. In this study, the characteristics of the lists had little significance.
Questionnaire-based surveys are fraught with some uncertainty due to missing responses. In our study, doctors with long lists were underrepresented. We therefore wished to use a complete registry material to analyse what kind of RGPs participate in the A&E scheme. Compared to previous studies, we could also include other explanatory variables, such as the organisation of their practices and the type of salary, as well as the RGPs’ immigrant status and duration of residence in Norway. This material also gives us an opportunity to investigate the number of patient contacts for each individual A&E doctor.
Material and method
The material includes all electronic billing cards from A&E doctors in Norway in 2008 (11). The material is near-complete; the degree of coverage in a corresponding material has been estimated as approaching 98 % in 2009 (12).
By linking this file to registries in the Regular GP Database and Statistics Norway (SSB) we have obtained further information on the patients’ RGP, so that the material also comprises all Norwegian RGPs. By comparing pseudonymous registry numbers we were able to identify those of the RGPs who were also A&E doctors. Locums who are not included in the RGP database were defined as other on-call doctors. We have the following information on the A&E doctors: gender, age, immigrant status, time of residence in Norway. With regard to the RGPs, we also have the following variables: type of salary (fixed salary or private practice), type of practice (single-doctor or group practice), municipality (centrality), list capacity (open or closed) and list length.
An immigrant is defined as a person who was born abroad and whose parents were both born abroad, and who at some point in time has immigrated to Norway.
Centrality is defined as the geographical location of a municipality in relation to a centre where high-order functions are located (central functions). Centrality is calculated on a scale from 0 to 3, where 0 denotes the least central municipalities and 3 the most central ones
The RGPs’ lists are considered as open when the difference between the list ceiling and the list length exceeds 20. We calculated the difference between the list ceiling and the list length throughout the year, and defined the list as open if this difference exceeded 20.
A contact with the emergency services was defined as a consultation (fee code 2ad, 2ak, 2fk), a house call (11ad, 11ak), a telephone contact (1bd, 1bk, 1g) or a simple contact (1ad, 1ak, 1h).
We estimated the proportion of the RGPs who performed A&E duty, divided into various sub-groups. Duty participation was defined as delivery of at least one billing card for A&E service by an RGP during the year. For the same groups, but only for those who had actually been on A&E duty, we also estimated the number of patient contacts over the year. The same groups were then used as explanatory variables in a multivariate logistic regression analysis, in which the dependent variable was whether the RGPs had undertaken A&E duty or not. All the variables describing the RGPs and their lists are simultaneously included in the model, and have been adjusted for each other. The explanatory variables included were gender, age group, immigrant status, with short and long duration of residence (dichotomised at the median value of 11 years), type of salary (private practice or fixed salary), type of practice (group or single-doctor practice), centrality, list capacity (open or closed list) and list length (four groups).
The study is included in the project Immigrant Health in Norway at the Research Group for General Practice, Department of Public Health and Primary Health Care, University of Bergen. The project employs data from the Norwegian Health Economics Administration (HELFO), the Regular GP Database, Statistics Norway and the Norwegian Prescription Database. The project has been granted a concession by The Data Inspectorate and is approved by the Regional Committee for Medical and Health Research Ethics. The Norwegian Labour and Welfare Administration (NAV) and the Directorate of Health have granted exemptions from the duty of confidentiality. The registry linkages were established by the Norwegian Prescription Database. The pseudonymised data file was adapted for analysis by the Norwegian Social Science Data Services (NSD).
Results
In 2008, the A&E services had a total of 1 715 279 patient contacts. For 86.2 % of these contacts the duty doctor could be identified. Altogether 2 174 RGPs (53.1 % of all RGPs) accounted for 46.7 % of the identifiable contacts, and 2 138 other duty doctors catered to the rest. The RGPs who were on duty were older than other doctors who were on call, and included a smaller proportion of women. Immigrants accounted for slightly more than 20 % of both groups (Table 1).
Table 1:
Comparison of duty doctors who are regular general practitioners and other duty doctors. The figures in brackets are the 25th and 75th percentiles.
| Regular general practitioner |
Other duty doctor |
|
| Proportion of women (%) |
33.2 |
44.6 |
| Age (years) |
44.2 (36.0 – 51.5) |
33.9 (29.0 – 35.0) |
| Proportion of immigrants (%) |
23.0 |
21.3 |
| Number of contacts per duty doctor |
317 (81 – 390) |
369 (71 – 387) |
| Total |
2 174 |
2 138 |
In the bivariate analysis an equally large proportion of the male and female RGPs performed A&E duty. Their participation decreased in proportion to the RGPs’ age, to increasing centrality and increasing list length. RGPs with fixed salaries had a somewhat higher rate of participation than RGPs in private practice, and RGPs in group practices had a somewhat higher rate of participation than their colleagues in single-doctor practices. RGPs with an open list had a somewhat higher rate of participation than RGPs with a closed list. Immigrant doctors with a short time of residence in Norway had a particularly high rate of participation (Table 2).
Table 2:
Proportion of regular general practitioners who perform A&E duty and the number of patient contacts per duty doctor. The figures in brackets are the 25th and 75th percentiles.
| Regular general practitioner |
Number |
Proportion (%) of doctors who perform A&E duty |
Average number of contacts per duty doctor |
| Man |
2 724 |
53 |
374 (99 – 444) |
| Woman |
1 373 |
53 |
206 (56 – 274) |
| Age < 40 |
1 093 |
79 |
312 (92 – 407) |
| Age 40 – 49 |
1 045 |
63 |
352 (93 – 397) |
| Age 50 – 59 |
1 405 |
41 |
285 (62 – 365) |
| Age > 59 |
554 |
14 |
327 (25 – 286) |
| Norwegian |
3 278 |
51 |
289 (70 – 359) |
| Immigrant, time of residence ≤ 11 years |
383 |
81 |
393 (115 – 532) |
| Immigrant, time of residence > 11 years |
378 |
49 |
449 (118 – 521) |
| Private practice |
3 808 |
52 |
318 (80 – 390) |
| Fixed salary |
285 |
63 |
310 (81 – 369) |
| Group practice |
3 447 |
54 |
316 (81 – 389) |
| Single-doctor practice |
613 |
46 |
324 (75 – 385) |
| Centrality 0 |
645 |
77 |
245 (96 – 310) |
| Centrality 1 |
319 |
68 |
287 (83 – 395) |
| Centrality 2 |
943 |
55 |
335 (87 – 403) |
| Centrality 3 |
2 115 |
42 |
353 (65 – 426) |
| Closed list |
2 599 |
50 |
290 (72 – 355) |
| Open list (at least 20 free slots) |
1 498 |
59 |
357 (90 – 452) |
| List length < 1 100 |
1 681 |
62 |
304 (86 – 368) |
| List length 1 100 – 1400 |
1 298 |
53 |
312 (73 – 398) |
| List length 1 401 – 1 700 |
764 |
43 |
336 (81 – 406) |
| List length > 1 700 |
354 |
34 |
416 (60 – 471) |
The multivariate analysis confirmed that the rate of participation in A&E duty decreased in proportion to increasing age among the RGPs, but this analysis also showed that female RGPs were underrepresented on the A&E duty roster. This is shown also in Figure 1. The multivariate analysis also revealed a decreasing rate of participation in A&E duty in proportion to increasing centrality and list length. Type of salary and open/closed list were of no significant importance, but the RGPs in single-doctor practices were somewhat underrepresented compared to doctors in group practices. The multivariate analysis confirmed that immigrant RGPs with a short time of residence in Norway were overrepresented on the A&E roster (Table 3). We found no significant differences between immigrant doctors from various parts of the world.
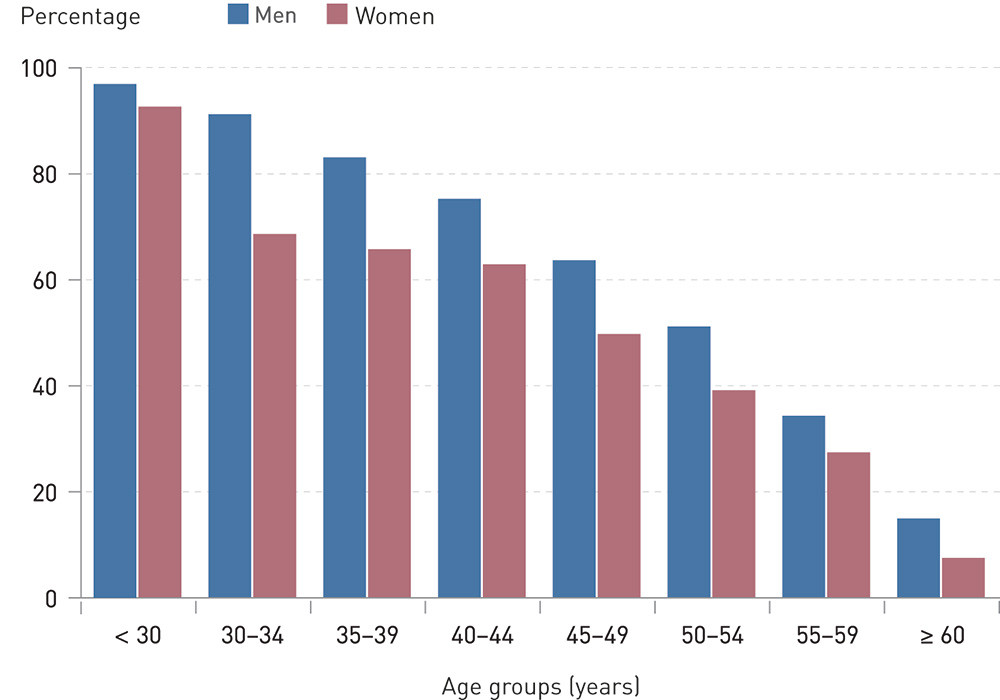
Table 3:
The regular general practitioners’ participation in A&E duty, multivariate analysis (logistic regression). All the variables describing the RGPs and their lists are included in the model and adjusted for each other
| Regular general practitioner |
Odds ratio |
95 % confidence interval |
| Man |
Reference |
|
| Woman |
0.49 |
0.42 – 0.59 |
| Age < 40 |
Reference |
|
| Age 40 – 49 |
0.49 |
0.40 – 0.61 |
| Age 50 – 59 |
0.18 |
0.15 – 0.23 |
| Age > 59 |
0.03 |
0.02 – 0.04 |
| Norwegian |
Reference |
|
| Immigrant, time of residence ≤ 11 years |
1.71 |
1.26 – 2.33 |
| Immigrant, time of residence > 11 years |
1.02 |
0.79 – 1.31 |
| Private practice |
Reference |
|
| Fixed salary |
1.00 |
0.72 – 1.40 |
| Group practice |
Reference |
|
| Single-doctor practice |
0.74 |
0.59 – 0.92 |
| Centrality 3 |
Reference |
|
| Centrality 2 |
1.74 |
1.45 – 2.08 |
| Centrality 1 |
3.41 |
2.51 – 4.65 |
| Centrality 0 |
5.13 |
3.93 – 6.70 |
| Closed list |
Reference |
|
| Open list (at least 20 free slots) |
1.01 |
0.85 – 1.20 |
| List length 1 100 – 1 400 |
Reference |
|
| List length < 1 100 |
1.18 |
0.98 – 1.42 |
| List length > 1 400 |
0.80 |
0.65 – 0.99 |
| List length > 1 700 |
0.64 |
0.48 – 0.84 |
Discussion
In general, the material covers nearly all contact with the A&E services in 2008, although the duty doctor could not be identified for 13.8 % of the contacts. This is partly because some casualty clinics pay fixed salaries and submit their bills using the clinic’s or the municipality’s enterprise registration number. There is little reason to believe, however, that this will have a significant impact on our comparison of RGPs who perform A&E duty with those who do not.
Many of the variables that describe the RGPs are interdependent. Women RGPs tend to be younger than their male counterparts, and their lists are shorter. In non-central regions the RGPs have shorter lists and more often work on a fixed salary. Open lists are shorter than closed lists. Such circumstances may explain the differences between the results of the bivariate and the multivariate analyses. When young RGPs perform A&E duty significantly more often than their older colleagues and women RGPs are significantly younger than their male colleagues, women and men may come out with the same rate of participation in a bivariate analysis. In a stratified (Figure 1) or a multivariate (Table 3) analysis, however, this difference becomes apparent.
This study largely confirms our findings from a study of social insurance reimbursements in 2004 and a survey in 2006, although the rate of participation in A&E duty among RGPs appears to have decreased even further (2, 3). The correlations between participation and the gender and age of the RGPs is unchanged, but we find an even more pronounced correlation with centrality, in that an RGP in a rural community is five times more likely to perform A&E duty than an RGP in a centrally located municipality. This is not necessarily a problem, since the availability of other duty doctors is much better in centrally located municipalities, although it is questionable whether other doctors are equally well qualified for this work (4, 9, 10).
In the survey there was no significant correlation between list length or list capacity and the rate of participation in A&E services (3). This may be related to the fact that relatively few doctors with long lists responded to this survey. In this material, however, we find a clear correlation, in that the longer their lists, the less RGPs participate in A&E services. The same finding emerged from the study of social insurance reimbursements (2).
The bivariate analysis indicated that RGPs with open lists are more frequently on on-call duty. Godager & Lurås have previously shown that RGPs who have too few patients tend to accept more municipal assignments than RGPs whose lists are full (14). However, this finding could not be corroborated by the multivariate analysis. This may be because open lists are more common in rural communities, where the rate of participation in A&E duty is higher. The bivariate analysis could also indicate that RGPs with fixed salaries participate more frequently in A&E duty. This finding, however, may be related to the fact that RGPs with fixed salaries tend to be found in rural regions. In the multivariate analysis, this correlation disappeared. The analyses confirm, on the other hand, that RGPs in group practices are more frequent participants in A&E duty than RGPs in single-doctor practices. Of all the groups, immigrant RGPs with a short time of residence in Norway have the highest rate of participation, whereas immigrants with a long time of residence are indistinguishable from their Norwegian colleagues with regard to their rates of participation. Many immigrant doctors who perform A&E duty on a regular basis have a consistently high number of patient contacts.
Women RGPs who perform A&E duty have significantly fewer patient contacts while on duty than their male colleagues. This is most likely an effect of their less frequent duty periods, but could also be an effect of them spending more time with each individual contact. There is a weak tendency for women doctors to use the time-based fee somewhat more frequently than male doctors (15). We have no figures for the number of duty periods filled by each individual doctor, but a higher number of duty periods is a likely explanation of why the immigrant RGPs have a significantly higher number of patient contacts than their Norwegian colleagues, as well as of why RGPs with an open list have more patient contacts than RGPs with a closed list (14).
RGPs who perform A&E duty in centrally located regions have a higher number of patient contacts than their colleagues in rural municipalities. This is most likely due to the larger patient population served by centrally located casualty clinics. A&E duty in rural regions involves a greater amount of passive waiting, but also more time-consuming house calls (16). RGPs with long lists are rarely involved in A&E duty, although those who actually perform A&E duty also tend to work more than other doctors on call. It is a fair assumption that this is caused by an exceptionally strong eagerness and capacity to work among these doctors.
Choosing not to take A&E duty or choosing to accept extra duty periods may be based on different motives. A&E duty is in principle mandatory for RGPs and doctors in training, although many RGPs have been given an exemption or have assigned their duty periods to other doctors. A&E work can be strenuous and entails an increased risk of making errors (5, 6). This work is undertaken outside of normal working hours and may be a strain on family life. On the other hand, it can provide a welcome amount of extra income, especially for young doctors who are at the start of their careers.
This study confirms and corroborates previous analyses of the participation of RGPs in A&E duty. RGPs in rural regions participate significantly more often than doctors in centrally located municipalities. It may seem as though long lists cause the RGPs to participate less frequently in A&E duty, but this problem is not of a large magnitude. Women account for an increasing proportion of RGPs, and it is thus likely that the rate of participation among the RGPs will decrease even further. On the other hand, the immigrants are providing a significant contribution to the maintenance of the A&E scheme.
In 2011, the project «Immigrant health in Norway» was granted financial support from the Directorate of Health (Department of Minority Health and Rehabilitation) for preparation of the data.
Tabell
| Main message |
|
- 1.
Forskrift om fastlegeordning i kommunene. www.lovdata.no/for/sf/ho/xo-20000414-0328.html (29.3.2012).
- 2.
Sandvik H, Hunskår S. Hvilke leger mottar trygderefusjon for legevaktarbeid? Tidsskr Nor Lægeforen 2007; 127: 1347-50. [PubMed]
- 3.
Sandvik H, Zakariassen E, Hunskår S. Fastlegenes deltakelse i legevakt. Tidsskr Nor Lægeforen 2007; 127: 2513-6. [PubMed]
- 4.
Høringsnotat om revidert fastlegeforskift m.m. Helse- og omsorgsdepartementet 22.12.2011. www.regjeringen.no/pages/36634101/fastlegeforskrift.pdf (29.3.2012).
- 5.
Bratland SZ, Hunskår S. Medisinsk-faglige vurderinger i tilsynssaker mot allmennleger. Tidsskr Nor Lægeforen 2006; 126: 166 – 9. [PubMed]
- 7.
Brügger EA, Jøsendal O. Registrering av aktivitet under legevakt. Tidsskr Nor Lægeforen 2001; 121: 2730 – 1. [PubMed]
- 8.
Nossen JP. Hva foregår på legekontorene? Konsultasjonsstatistikk for 2006. NAV-rapport nr. 4 2007. Oslo: Arbeids- og velferdsdirektoratet, 2007.
- 9.
Nasjonalt kompetansesenter for legevaktmedisin. ... er hjelpa nærmast! Forslag til Nasjonal handlingsplan for legevakt. Rapport nr. 1 – 2009. Bergen: Nasjonalt kompetansesenter for legevaktmedisin, Unifob helse, 2009. www.unifobhelse.no/upload/Handlingsplan.pdf (29.3.2012).
- 10.
Arbeidsgruppe ’Godt legevaktsarbeid’. Faglige og organisatoriske krav til legevakt. Videreutvikling av legevaktsbaser og interkommunalt legevaktsamarbeid. Rapport. Oslo: Den norske legeforening, 2008.
- 11.
Sandvik H, Hunskår S, Diaz E. Fastlegepasienters bruk av legevakt. Tidsskr Nor Legeforen 2012; 132: 2272-6.
- 12.
Analyserapport. Fastleger, legevakt og avtalespesialister. Aktivitetsstatistikk 2009. Oslo: Helseøkonomiforvaltningen, 2011. www.helfo.no/statistikk/Documents/Analyserapport%20Aktivitetsstatistikk%202009.pdf (29.3.2012).
- 13.
Standard for kommuneklassifisering 1994. Statistisk sentralbyrå 1994. www.ssb.no/kommuner/komklasse94.html (29.3.2012).
- 15.
Sandvik H, Hunskår S. Arbeidsstil hos fastleger og andre leger på legevakt. Tidsskr Nor Legeforen 2010; 130: 135–8. [PubMed]
- 16.
Sandvik H, Hunskår S. Årsstatistikk fra legevakt 2010. Rapport nr. 3 – 2011. Bergen: Nasjonalt kompetansesenter for legevaktmedisin, Uni helse, 2010.