Hyperkinetic disorder, or ADHD, is a neuro-psychiatric condition presenting with inattentiveness and concentration problems, impulsiveness and hyperactivity from a young age, causing difficulties for the patient in connection with, for example, education, work and leisure (2). The worldwide prevalence of this disorder is estimated at approximately 5 % in children and young people under the age of 18, and is higher among boys than among girls (3). Half the children with ADHD will continue to present symptoms as adults (4), and many suffer from additional mental disorders (5). Without treatment, the risk increases of later difficulties in working life (6), poor personal finances, problems in inter-human relationships and substance abuse (2).
In Norway, methylphenidate, racemic amphetamine and atomoxetine are prescribed for ADHD in children and young people aged 6 – 17 as part of a treatment programme, while dexamphetamine is prescribed only subject to approval exemption (7). Methylphenidate is recommended as the first choice (2) and is available in immediate-release and extended-release formulations. Immediate-release methylphenidate is prescribed in two or four daily doses, while extended-release methylphenidate and atomoxetine are both prescribed in a single daily dose. For a long period, only immediate-release methylphenidate was licensed for sale in Norway. Extended-release methylphenidate was approved for use in Norway in the autumn of 2002, and in the autumn of 2004 atomoxetine was approved for sale in this country (7). Racemic amphetamine has been available on the Norwegian market for many years as a pharmacist-produced medicine. From 1997 to 2005 the treatment of adult ADHD patients with drugs that stimulate the central nervous system was permissible subject to approval from a team of specialists and the regional chief medical officer. In the period from 1 May 2005 to 1 February 2011 medication used for treating ADHD in adults was approved for government-funded prescriptions (2, 8).
An ADHD diagnosis is based on either the DSM-IV or ICD-10 disorder classification systems. Any course of medication must be initiated under the supervision of a specialist in behavioural disorders in children. Methylphenidate and amphetamine stimulate the central nervous system. These drugs can only be prescribed by someone who holds a general requisition authorisation (specialist in behavioural disorders in children), or an individual requisition authorisation (GP). Such authorisation is available on application to the regional chief medical officer. Until 2005 follow-up treatment could only be provided under the guidance of a specialist, but since 1 May 2005 GPs have been able to continue the treatment unsupervised (2).
The prescription of ADHD medication in Norway has increased significantly since the 1990s (9), a development which is frequently debated in professional circles and in society generally. Based on national data from the Norwegian Prescription Database and the GP database we have analysed how the prescription rate for ADHD medication has developed in the years 2004 – 08.
Material and method
Data sources and extraction
The Norwegian Prescription Database (NorPD) at the Norwegian Institute of Public Health contains information about all prescription drugs sold by Norwegian pharmacies to individuals after 1 January 2004. The study included all prescriptions for the active substances (ATC code) methylphenidate (N06BA04), atomoxetine (N06BA09), racemic amphetamine (N06BA01) and dexamphetamine (N06BA02) sold in the period 2004 – 08. Prescription indications are not recorded in the Norwegian Prescription Database, and patients who have received treatment for, say, narcolepsy are therefore also included in the material. We included the following variables: the patient’s birth year and sex, any specialties the prescriber might have, the name of the medication, the prescribed volume in Defined Daily Dose (DDD) and the date of purchase. The DDD is the calculated average daily dose of the drug when used for its main indication.
We grouped the drugs into extended-release methylphenidate (Concerta, Equasym capsule, Ritalin capsule or depot tablet), immediate-release methylphenidate (Ritalin tablet, Equasym tablet), atomoxetine (Strattera) and amphetamine (both racemic amphetamine and dexamphetamine).
From a total of 559,327 prescriptions we excluded 1.9 % due to insufficient information about the patient, the prescriber or the volume. We also excluded six prescriptions for which the prescribed volume exceeded 1,000 DDD, leading us to believe they had been incorrectly recorded.
Prescribers
We obtained information about the identity of GPs from the GP database at the Norwegian Social Science Data Services, and about the identity of specialist consultants from the Norwegian Prescription Database. For every year between 2004 and 2008 we grouped the prescribers as GPs (registered in the GP database, irrespective of any specialty), paediatric psychiatrists (specialists in paediatric psychiatry who were not also GPs), psychiatrists (specialists in psychiatry who were not also GPs or paediatric psychiatrists), paediatricians (specialists in childhood diseases who were not also GPs, paediatric psychiatrists or psychiatrists), other specialists and non-specialists.
Statistics Norway generated unique, pseudonymous serial numbers for each of the patients registered in the Norwegian Prescription Database and each of the prescribers registered in the GP database. Population figures were obtained from Statistics Norway.
Ethics
The regional committee for medical and health research ethics (REK West) has approved the study. The Norwegian Data Protection Authority has authorised the linking of the databases, and the Norwegian Directorate of Health has granted exemption from the confidentiality rules.
Statistical analysis
The results are presented as the number of people per 1,000 inhabitants who collected at least one prescription for ADHD medication in the course of a year. New ADHD medication prescription users are people who collected at least one prescription in the course of one calendar year and who had not received such medication the year before. The qualifying period was set to one year to enable us to calculate the rate for 2005, since the Norwegian Prescription Database was first launched in 2004. One-year persistence and three-year persistence refer to the percentage of new users in 2005 who also collected at least one prescription for ADHD medication for a period of one and three consecutive years respectively. Children and young people (boys, girls) are defined as people under the age of 18; adults (men, women) are defined as people of 18 years of age or older.
The analyses were carried out using the SPSS Statistics 19.0 software.
Results
Prescription rate for ADHD medication
From 2004 to 2008 the number of people who collected prescriptions for ADHD medication increased steadily from 2.6 to 5.2 per 1,000 inhabitants, albeit there were major regional variations (tab 1). In 2004 the number varied from 1.5 per 1,000 inhabitants in Hordaland to 4.0 in Aust-Agder, and in 2008 from 3.3 in Oslo to 8.7 in Aust-Agder.
Table 1
The number of people per 1,000 inhabitants in Norway who collected at least one prescription for methylphenidate, atomoxetine, racemic amphetamine or dexamphetamine in 2004 and 2008; regional distribution
| Region |
2004 |
2008 |
| Akershus |
2.5 |
4.8 |
| Aust-Agder |
4.0 |
8.7 |
| Buskerud |
3.8 |
6.1 |
| Finnmark |
3.2 |
5.9 |
| Hedmark |
3.0 |
6.3 |
| Hordaland |
1.5 |
3.7 |
| Møre and Romsdal |
3.1 |
5.4 |
| Nordland |
3.2 |
7.3 |
| Nord-Trøndelag |
2.2 |
5.3 |
| Oppland |
2.0 |
4.3 |
| Oslo |
2.0 |
3.3 |
| Rogaland |
2.3 |
5.6 |
| Sogn and Fjordane |
3.2 |
4.6 |
| Sør-Trøndelag |
2.0 |
4.4 |
| Telemark |
3.3 |
6.2 |
| Troms |
1.8 |
4.1 |
| Vest-Agder |
3.7 |
6.1 |
| Vestfold |
3.2 |
6.6 |
| Østfold |
2.6 |
6.1 |
| Norway overall |
2.6 |
5.2 |
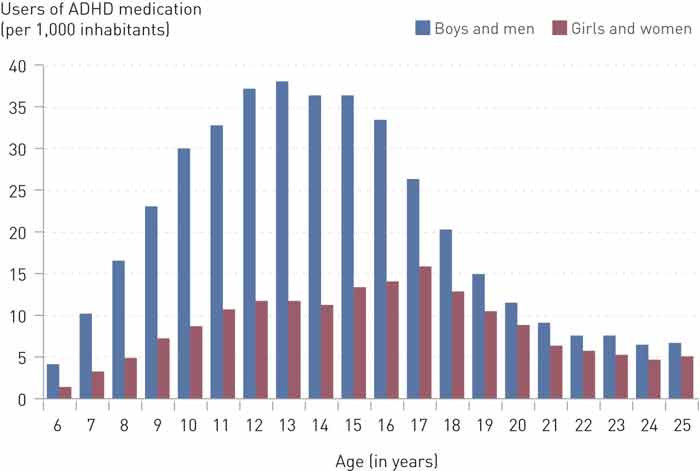
Figure 1 shows the number of people per 1,000 inhabitants aged 25 and younger who collected such prescriptions in 2008. For boys, the number increased with age until they reached 13 (38 per 1,000) and for girls, until they reached 17 (16 per 1,000); thereafter the numbers fell. The number of people who collected such prescriptions increased over the period in all age groups and among both males and females (tab 2). The absolute increase was strongest during the teenage years, while the relative increase was strongest among adults. Women make up an increasing proportion of the people who collect prescriptions for ADHD medication in all age groups, and the male to female ratio (boys and men : girls and women) fell from 3.4 to 2.0 over the period 2004 – 08.
Table 2
The number of people per 1,000 inhabitants, specified by age and sex, who collected one prescription or more for methylphenidate, atomoxetine, racemic amphetamine or dexamphetamine in 2004 and 2008.
| Boys and men |
Girls and women |
||||||
| 2004 |
2008 |
2004 |
2008 |
||||
| Age (in years) |
(n = 9 156) |
(n = 16 500) |
(n = 2 721) |
(n = 8 121) |
|||
| < 6 |
0.5 |
0.3 |
0.1 |
0.1 |
|||
| 6 – 10 |
12.9 |
16.9 |
2.9 |
5.1 |
|||
| 11 – 15 |
24.1 |
36.0 |
5.8 |
11.7 |
|||
| 16 – 20 |
11.2 |
21.5 |
3.9 |
12.5 |
|||
| 21 – 25 |
3.2 |
7.5 |
1.1 |
5.4 |
|||
| 26 – 30 |
1.9 |
5.3 |
0.9 |
3.7 |
|||
| > 30 |
0.6 |
1.8 |
0.4 |
1.5 |
|||
| Total |
4.0 |
6.9 |
1.2 |
3.4 |
|||
The number of new people per 1,000 inhabitants who collected such prescriptions, remained largely unchanged throughout the period 2005 – 08 (tab 3), but fell slightly among boys. There were considerable differences between males and females in childhood, but this was less of a feature among teenagers and adults.
Table 3
The number of people per 1,000 inhabitants, specified by age and sex, who collected one prescription or more for methylphenidate, atomoxetine, racemic amphetamine or dexamphetamine in 2005 and 2008, and who had not collected a prescription the previous year.
| Boys and men |
Girls and women |
||||||
| 2005 |
2008 |
2005 |
2008 |
||||
| Age (in years) |
(n = 4 316) |
(n = 4 035) |
(n = 2 017) |
(n = 2 658) |
|||
| < 6 |
0.4 |
0.2 |
0.1 |
0.0 |
|||
| 6 – 10 |
7.5 |
6.6 |
2.2 |
2.4 |
|||
| 11 – 15 |
7.6 |
6.6 |
3.2 |
3.1 |
|||
| 16 – 20 |
3.8 |
3.5 |
3.0 |
3.8 |
|||
| 21 – 25 |
2.4 |
2.0 |
1.1 |
1.9 |
|||
| 26 – 30 |
1.6 |
1.5 |
0.9 |
1.5 |
|||
| > 30 |
0.5 |
0.6 |
0.3 |
0.5 |
|||
| Total |
1.9 |
1.7 |
0.9 |
1.1 |
|||
For new users who first collected prescriptions for ADHD medication in 2005, the one-year and three-year persistence was 76 % and 53 % respectively (males and females combined). Table 4 shows that the rate of persistence was highest among children, fell sharply among teenagers, but increased again in adulthood. More female than male teenagers and adults collected their prescriptions over an extended period of time.
Table 4
Sex and age specific percentages of people who collected one prescription or more for methylphenidate, atomoxetine, racemic amphetamine or dexamphetamine in 2005, and who also collected a prescription the next (2006) or three next (2006 – 08) consecutive years.
| Boys and men |
Girls and women |
||||
| Age (in years) |
One-year persistence (%) |
Three-year persistence (%) |
One-year persistence (%) |
Three-year persistence (%) |
|
| < 6 |
86.7 |
81.3 |
93.8 |
81.3 |
|
| 6 – 10 |
87.5 |
76.1 |
85.1 |
76.0 |
|
| 11 – 15 |
81.5 |
55.9 |
80.8 |
57.2 |
|
| 16 – 20 |
58.5 |
23.4 |
65.8 |
32.1 |
|
| 21 – 25 |
60.3 |
33.2 |
66.0 |
43.3 |
|
| 26 – 30 |
65.7 |
39.4 |
75.6 |
45.8 |
|
| > 30 |
71.4 |
44.7 |
74.9 |
51.8 |
|
| Total |
76.2 |
53.4 |
75.6 |
52.1 |
|
Choice of medication
Table 5 shows the percentage distribution of the various ADHD drugs purchased in 2004 and 2008. From 2004 to 2008 the proportion of extended-release methylphenidate rose, while the proportion of immediate-release methylphenidate fell both among children/young people and adults. In 2008 immediate-release and extended-release methylphenidate constituted 35 % and 51 % respectively of the prescription volume (in DDD) collected by adults and 11 % and 83 % of the volume collected by children and young people (not shown in the table). The number of people who collected prescriptions for atomoxetine, increased sharply from 12.7 to 21.1 per 1,000 adults and from 4.9 to 18.4 per 1,000 children/young people in the period 2004 to 2005; thereafter it remained stable. In relative terms, amphetamine constituted a smaller proportion in 2008 (tab 5), but the number of people who collected prescriptions for amphetamine increased between 2004 and 2008.
Table 5
Percentage distribution of ADHD medication collected in 2004 and 2008. The figures are based on the number of children/young people and adults who collected at least one prescription for methylphenidate, atomoxetine or amphetamine (racemic amphetamine and/or dexamphetamine).
| Children and young people (under 18) |
Adults (18 or older) |
||||
| Medication |
2004 (n = 8 662) |
2008 (n = 13 991) |
2004 (n = 3 215) |
2008 (n = 10 630) |
|
| Extended-release methylphenidate |
49.6 |
52.7 |
17.2 |
30.5 |
|
| Immediate-release methylphenidate |
16.2 |
6.7 |
46.0 |
29.7 |
|
| Extended and immediate release methylphenidate |
25.9 |
25.6 |
12.3 |
19.9 |
|
| Amphetamine |
2.3 |
0.9 |
9.4 |
5.4 |
|
| Amphetamine and methylphenidate |
1.1 |
0.5 |
2.4 |
2.0 |
|
| Atomoxetine |
1.9 |
8.1 |
9.9 |
9.3 |
|
| Atomoxetine, amphetamine and methylphenidate |
3.0 |
5.5 |
2.8 |
3.2 |
|
Prescribers
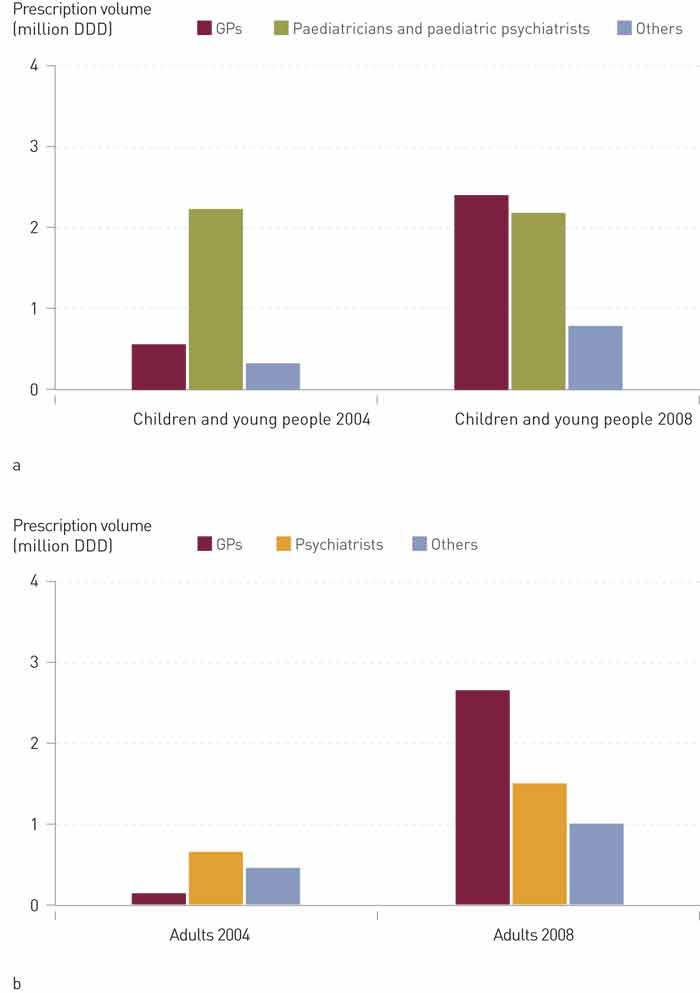
Figure 2 shows that in 2004, paediatric psychiatrists and paediatricians prescribed most of the medication for children and young people, while the majority of adults received their prescriptions from psychiatrists. The GPs’ contribution to the total prescribed volume purchased increased from 17 % in 2004 to 48 % in 2008. The GPs made up 59 % (1,254 of 2,141) of the prescribers of ADHD medication in 2004 and 82 % (3,238 of 3,963) in 2008. These GPs constituted 32 % of the total Norwegian GP population in 2004, and 79 % in 2008.
Discussion
The study suggests that the number of Norwegians treated with ADHD medication was doubled in the period 2004 – 08, and that the number of women receiving treatment increased more over the period than the number of men. There were considerable geographical differences. It appears that more boys than girls used these drugs, whereas the gender difference would level out among adults. Extended-release methylphenidate was the most frequently collected ADHD drug. GPs prescribed half of the medication volume collected in 2008.
It is likely that the increased use of medication against ADHD from 2004 to 2008 was caused by raised awareness of the diagnosis. The approval and reimbursement arrangement introduced for the drug treatment of adults in 2005, was in line with these developments. Figures from the Norwegian Prescription Database’s website indicate that the trend continued in the period 2009 – 11 (10). A similar trend is also evident in the USA (11), where methylphenidate and atomoxetine have now been approved for adults.
If we look at childhood prescription rates in other countries, we find that for the 7 – 15 age group, the rates recorded in Finland, Denmark and Sweden were 6.4, 9.3 and 9.6 per 1,000 inhabitants in 2007, while the rate in Norway was 18.1. In Iceland, the rate was as high as 47.0 per 1,000 inhabitants (12), while the Netherlands recorded a rate of 21.0 for the 6 – 17 age group (13).
The number of new users remained stable throughout the 2005 – 08 period. The prescription rate may have increased because the number of new users was lower before 2005 and/or because the treatment period has been extended. It is reasonable to believe that children and young people who benefit from ADHD medication will continue the treatment as adults, but the follow-up period is too short within this study to enable us to document the treatment period of individuals. A number of studies have shown that the use of extended-release methylphenidate predicts longer treatment periods (14, 15), and our study has demonstrated an increase in the prescription rate for extended-release methylphenidate.
The considerable differences between male and female children and young people in this study may indicate that girls suffering from ADHD go through large parts of their statutory education before they are diagnosed and receive treatment (16). One possible explanation is that girls suffer from attention deficiency to a greater extent than boys. To other people, this type of problem is not as evident as hyperactivity and impulsiveness (17). Parents, teachers and doctors may not recognise that girls with an attention deficiency disorder suffer from ADHD, but interpret their symptoms as evidence of other behavioural problems, emotional problems or learning difficulties (18) – (20). On the other hand, the Attention-Deficit Hyperactivity Disorder Observational Research in Europe (the ADORE study) showed that there were few or no differences between males and females with respect to ADHD symptoms, nor the symptom debut age in boys and girls (5).
We have no explanation as to why women continue using ADHD medication over a longer period of time than men, but this may be associated with the fact that women also use other psycho-pharmaceuticals to a greater extent than men (21). In line with an English study (16) we found that many stopped taking their medication as teenagers or young adults, even though there is reason to believe that their condition continued. This may be interpreted as an indication that this age group is under-treated.
Choice of medication
Extended-release methylphenidate was approved for use in Norway in the autumn of 2002 and in the course of only a few years became the most extensively used ADHD drug. The increase may be explained by the fact that extended-release medication is simpler to administer than immediate-release medications, and the drug thus meets a need in relation to schools, educational institutions and the workplace.
The results of this study indicate that immediate-release methylphenidate is rarely taken on a regular basis by children and young people, but that this medication is used initially to titrate up to an appropriate treatment dose, or it is used as required to supplement extended-release methylphenidate. This is supported by the finding that most people who took immediate-release methylphenidate, also received extended-release methylphenidate in the course of the same year. Even if one in three young people who use ADHD medication collected immediate-release methylphenidate in 2008, this medication constituted only a tenth of the overall prescription volume for children and young people.
The sharp introductory increase in atomoxetine prescriptions may be caused by the fact that it is simpler to prescribe, since it is not subject to the granting of a special requisition authority or to the rigorous rules that apply for the prescription of narcotic substances. Another explanation may be that the medication is used for test purposes when other medication has been contraindicated, produced side effects or therapy failure. Furthermore, atomoxetine is easy to administer, while extended-release methylphenidate was already available when atomoxetine was launched on the market. The increase may also be due to the fact that new drugs are often more aggressively promoted during their first years on the market.
Prescribers
GPs constituted an increasing proportion of prescribers during the study period, and their prescriptions represented most of the total volume increase. This reflects a development which sees specialists set the diagnosis and commence the drug treatment, only to refer the patient back to his/her GP for further follow-up. One explanation for this development may be the changes to the regulations that were introduced in 2005, although it is possible that GPs would have become increasingly responsible for the treatment of ADHD anyway. The same trend was found in Nordland county over the period 1999 – 2004 (22), but the increase accelerated in the period 2004 – 08. The contribution from non-specialists who are not GPs, increased considerably from 2004 to 2008. This can probably be explained by the fact that doctors training to become psychiatrists or paediatric psychiatrists to a greater extent than previously are involved with the diagnostic stages and the initial treatment of ADHD.
Strengths and weaknesses
This study is based on data obtained from a quality-assured register that includes records of all ADHD medication sold to the entire population from 2004 to 2008. We do not know how much of the medication sold was actually used. Furthermore, the register holds no information about the individual patient’s indication; narcolepsy is the only alternative indication for these drugs, and the prevalence is low. The register holds no information about the daily doses prescribed for individual patients. DDD is an unreliable measurement of the maintenance dose since this depends on weight and is different in children and adults. DDD was used in order to analyse the physicians’ prescription volume.
Data obtained from the GP database enabled us to identify prescriptions made by GPs. The other prescribers were grouped according to their specialties as recorded in the Norwegian Prescription Database, as we had no information about their places of work. This may have given rise to a certain level of incorrect classification.
Implications
The considerable differences between the prescribing of ADHD medication to boys and girls, suggest that girls are diagnosed too late, and that they have completed much of their statutory education before they receive treatment. This demonstrates a need for increased competence with respect to ADHD, particularly in girls, both generally and among professionals. At the same time, it appears that many patients stop taking their medication in their teens and in early adulthood, indicating possible under-treatment. There is reason to look closer into the basis for treatment through clinical studies.
GPs now play a prominent part in the treatment of ADHD, which means there is a need to bolster their competency to ensure that the patient group receives a sufficiently high standard of care. A SINTEF report from 2008 argues that GPs should increase their contribution at the diagnostic stages and that specialist consultants should contribute more to annual check-ups and whenever a change in medication is required (23). The report points out the need to map the patients’ pathways and the standard of coordination between first and second line health services for ADHD patients.
The article is based on a student thesis submitted at the University of Bergen (1).
Tabell
| Main messages |
|
- 1.
Lillemoen PKS. Legemiddelbruk mot ADHD 2004 – 2008. Særoppgåve i medisin. Bergen: Det medisinske fakultet, Universitetet i Bergen, 2011.
- 2.
Veileder i diagnostikk and behandling av ADHD, IS-1244. 2005, revidert 2007. Oslo: Sosial- and helsedirektoratet, 2007.
- 7.
Statens Legemiddelverk. Søkebase for legemidler. www.legemiddelverket.no/custom/Preparatsok/prepSearch____80333.aspx (31.3.2012)
- 8.
Statens Legemiddelverk. Vedtak om endring av refusjonsberettiget bruk for metylfenidat. 2010. www.legemiddelverket.no/upload/VEDTAK%20M.pdf (31.3.2012)
- 9.
Legemiddelforbruket i Norge 2006 – 2010. Oslo: Folkehelseinstituttet, 2011. www.legemiddelforbruk.no/ (31.3.2012)
- 10.
Nasjonalt reseptbasert legemiddelregister. www.reseptregisteret.no/ (31.3.2012).
- 15.
Kemner JE, Lage MJ. Impact of metylphenidate formulation on treatment patterns and hospitalizations: a retrospective analysis. Ann Gen Psychiatry 2006; 5: 5.
- 22.
Åsheim H, Nilsen KB, Johansen K et al. Forskrivning av sentralstimulerende legemidler ved ADHD i Nordland. Tidsskr Nor Lægeforen 2007; 127: 2360–2. [PubMed]
- 23.
Ådnanes M, Andersson HW. Evaluering av Veileder i diagnostikk and behandling av ADHD and regelverk for legers rett til å rekvirere sentralstimulerende legemidler. Delrapport 3 Legers erfaringer. Trondheim: SINTEF rapport 2008.