Substitution treatment with methadone or buprenorphine is currently the most common treatment for heroin dependence (1). The treatment was established in Norway as drug-assisted rehabilitation (DAR) in 1997. The model has been evaluated a number of times (2) – (5). The Directorate of Health issued guidelines based on special regulations in 2010 (6), but the basic model is unchanged. Evaluation of indication, choice of drug type and setting of the optimal dosage are to be carried out by the specialist health service. The GPs have a central part to play in the treatment, but cannot initiate it independently. It presupposes cooperation with the municipal social services and the treatment should build on the use of patient care groups and interventions. This therefore entails certain requirements in terms of GPs’ participation and a certain restriction on their free choice of treatment.
Pharmaceutical maintenance treatment with methadone was developed in the US, with strict monitoring requirements and emphasis on specialised centres. Today the design of the treatment model varies internationally. The Norwegian model has a model for shared care involving cooperation between specialist interventions and GPs.
The introduction of the regular GP scheme in 2001 and amendments to the Municipal Health Services Act and the Specialist Health Services Act in 2002 as well as the drugs policy reforms of 2004 have given doctors a more important role in the treatment of drug and alcohol dependence. Norwegian doctors’ views on these changes and on drug-assisted rehabilitation were investigated using questionnaire surveys of a panel of doctors in 2000 and 2006 (7). The majority were positive about the reforms, and moreover 53 % had a positive view of substitution treatment, both in 2000 and 2006. In 2000, 45 % were negative about prescribing methadone/buprenorphine themselves, while this proportion was 33 % in 2006.
In January 2010, 5 383 patients were in drug-assisted rehabilitation. 3 500 (65 %) of these were being treated by GPs cooperating with DAR teams (8). One year later, 6 015 patients were in DAR treatment. 4 090 (68 %) of these received the DAR drug prescribed by their GP (9). A significant number of Norwegian doctors are therefore participating in a tripartite collaboration with the social services (the Norwegian Labour and Welfare Service – NAV) and the specialist health service. Some doctors have been very critical of drug-assisted rehabilitation (10). Others believe that GPs possess the competence to have greater responsibility within the model (11). There has been severe criticism from a criminological and legal angle of an authoritarian «methadone inspectorate» (12).
Drug-assisted rehabilitation today has become an integrated part of the health services, the experience base is broader and the debate is more refined. In this study we wished to investigate whether the changes have altered Norwegian GPs’ views of this form of treatment and how doctors with DAR experience evaluate the Norwegian model of shared responsibility and tripartite collaboration. This is important both for the further development of drug-assisted rehabilitation and for discussions on collaborative models for multidisciplinary health services.
Material and method
A sample of 3 770 GPs was drawn from the members’ register of the Norwegian Medical Association in November 2009. These encompassed all GP’s in the register at the time, minus a random sample of 500 who were used in another study. These doctors received an e-mail in June 2010 with a link to an electronic questionnaire (QuestBack) and information that the Norwegian Centre for Addiction Research at the University of Oslo (SERAF), the reference group for addiction medicine of the Norwegian Association of General Medicine (Norwegian Medical Association) and the Research Institute of the Norwegian Medical Association were behind the survey. Data collection lasted until 13 September 2010, with four reminders sent. The survey was approved by the Norwegian Social Science Data Services.
The questionnaire was in two parts. The first part contained questions about attitude to and opinions on drug-assisted rehabilitation. Those who had participated in this type of treatment completed Part 2 with 22 statements about the model, formulated on the basis of the debate in professional forums. The general evaluations were surveyed using a three-point value scale (negative-neutral-positive) and the specific opinions using a five-point Lickert scale from 1 (strongly disagree) to 5 (strongly agree). The survey was anonymous, but we asked about gender, age, list size, county and specialisation in general medicine as well as the number of DAR patients over all and at the time of responding.
The results are primarily presented in descriptive form. We use percentages and average values to describe tendencies and group comparisons and logistic regression to describe concurrent effects. The four dependent variables in the regression analyses were all on an ordinal scale from 1 – 5. The odds ratio represents the change in the association that takes place by moving one ordinal place on the scale, e.g. from 1 to 2. An odds ratio higher than 1.0 thereby indicates a significant association between the independent variable and greater support for the attitude statement in the model. Statistical significance is tested using the chi-squared or 95 % confidence interval. All the analyses were conducted using Predictive Analytics SoftWare Statistics (PASW), version 18.
Results
Of the 3 770 GPs invited, 243 used the unsubscribe link. 120 questionnaires were returned due to invalid e-mail addresses. The real percentage of responses was 34 (1 165/3 407). Of these, 411 (35 %) were women and 750 (65 %) were men (non-respondent = 4). The respondents had worked an average of 16.2 years as GPs. The majority were specialists or in specialist training in general medicine. The average number of patients on their lists was 1 191.
883 doctors (76 %) had experience of systematic treatment and follow-up of patients with substance abuse problems generally. 321 (28 %) had not referred a patient for specialist substance abuse treatment in the past year, while 766 (66 %) had done this «a few times». Only 72 (6 %) had made referrals monthly or more frequently. 683 (59 %) of the respondents had at some time participated in DAR treatment. These are referred to as DAR doctors in this article. 149 (22 %) of the DAR doctors had no DAR patients at the time of responding. The remaining 534 (78 %) had a total of 2 028 DAR patients. At the time of the survey this represented approximately 53 % of all DAR patients being treated by GPs, calculated as the median of the number at the beginning and end of the year. 445 (65 %) of DAR doctors had fewer than six DAR patients, 215 had six to ten DAR patients and 23 doctors had more than ten DAR patients. Five doctors had more than 20 DAR patients, whereof three had 30 or more. One doctor had 70 patients and one 85. The average was just under four DAR patients per doctor.
The representativeness of the sample in terms of age, gender, county of work and specialisation in general medicine is presented in Table 1. The respondents and DAR doctors differed little from the GP group as a whole, with the exception of a certain geographical skewing and a somewhat high proportion of specialists in general medicine. The DAR doctors did not stand out from the respondents overall except for a somewhat higher participation from the Eastern Norway health region.
Table 1
Representativeness of the sample in terms of gender, age, region and specialty
| Our respondents |
All GPs in November 2009 |
|||
| All |
Doctors with DAR experience |
|||
| Number |
1 165 |
683 |
4 205 |
|
| Proportion of women, percentage (95 % CI) |
35.4 (32.6 – 38.0) |
30.6 (27.1 – 34.1) |
37.1 |
|
| [Unanswered 4] |
[Unanswered 0] |
|||
| Age, percentage (95 % CI) |
||||
| ≤ 40 years |
31.4 (28.5 – 33.9) |
31.2 (27.7 – 34.7) |
29.9 |
|
| 41 – 55 years |
39.0 (36.1 – 41.7) |
39.3 (35.6 – 42.9) |
39.0 |
|
| > 55 years |
29.6 (26.9 – 32.1) |
29.5 (26.1 – 32.9) |
31.1 |
|
| [Unanswered 4] |
[Unanswered 1] |
|||
| County, percentage (95 % CI) |
||||
| Østfold, Akershus, Oslo, Hedmark, Oppland |
35.1 (30.5 – 39.4) |
44.5 (40.8 – 48.3) |
32.0 |
|
| Buskerud, Vestfold, Telemark, Aust- and Vest-Agder |
9.1 (5.3 – 12.9) |
18.8 (15.9 – 21.7) |
15.2 |
|
| Rogaland, Hordaland, Sogn og Fjordane |
21.8 (16.7 – 26.9) |
17.2 (14.5 – 18.9) |
19.7 |
|
| Møre og Romsdal, Sør-Trøndelag, Nord-Trøndelag |
13.4 (8.0 – 18.8) |
12.3 (9.8 – 14.8) |
14.0 |
|
| Nordland, Troms, Finnmark |
10.8 (5.4 – 16.2) |
9.9 (7.7 – 12.1) |
11.1 |
|
| [Unanswered 9] |
[Unanswered 3] |
|||
| Specialist in general medicine, percentage (95 % CI) |
||||
| Non-specialist |
5.9 (4.3 – 6.9) |
5.4 (3.7 – 7.1) |
– |
|
| In specialist training |
27.9 (25.2 – 30.4) |
28.7 (25.3 – 32.1) |
– |
|
| Specialist |
66.1 (63.1 – 68.5) |
65.9 (62.3 – 69.5) |
56.4 |
|
| [Unanswered 5] |
[Unanswered 0] |
|||
Attitudes to DAR
The attitudes to substitution treatment (DAR) varied: 155 (13 %) were negative, 395 (34 %) were neutral, while 607 (53 %) described a positive attitude. 414 (36 %) «would not think of prescribing methadone or buprenorphine themselves». 572 (49 %) were positive towards participating in such treatment, while 172 (15 %) were unsure.
Experiences as a DAR doctor
The group with experience as DAR doctors were asked what it was like to be a doctor for DAR patients. 252 (37 %) responded that it was positive, 261 (38 %) were neutral, while 167 (25 %) considered it negative. The DAR doctors’ scores for the specific statements in Part 2 are presented in Figure 1. The majority value collaboration in this field, and the tripartite model has strong support in this sample. Few want sole responsibility for treatment and very few consider the specialist health services to be a hindrance. The doctors in the sample for the most part support the monitoring of treatment and the restrictions on doctors’ autonomy. Few DAR doctors find that the patient care groups take up too much time or are often badly managed. The statement that drug-assisted rehabilitation is mainly about harm reduction divides the respondents into two groups with the emphasis on «partly agree» and «partly disagree». The same applies to the question of whether doctors find the specialist health services helpful.
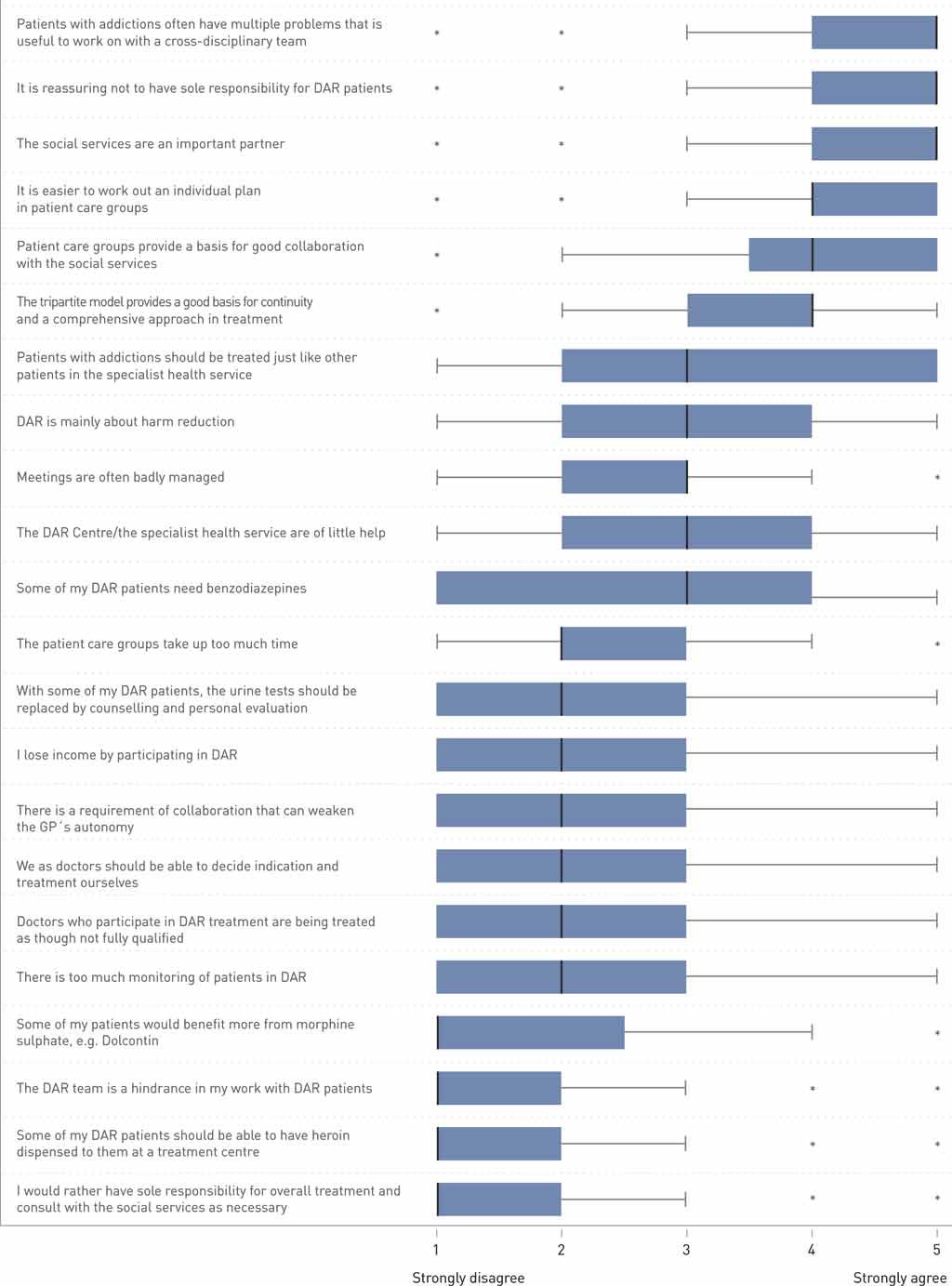
Table 2 shows the effect of list size, specialist status, health region, age and gender on four different DAR-related factors. The value placed on participation in drug-assisted rehabilitation is generally independent of gender, list size, experience of substance abuse treatment and specialist status. Younger doctors tend to have a more negative attitude to the model, whereas those who have had many DAR patients are more positive. The collaboration with the specialist health services is considered to be more positive in Central Norway and in the counties that previously comprised Health Region South. Those with many DAR patients and those working in North and Central Norway disagree to a greater extent that drug-assisted rehabilitation is mainly about harm reduction. There is somewhat greater support for the statement that some DAR patients need benzodiazepines among those who have had many DAR patients and those working in North Norway. An increasing number of DAR patients on a doctor’s list is associated with increased satisfaction with being a DAR doctor and greater open-mindedness about prescribing benzodiazepines, but less agreement that drug-assisted rehabilitation is mainly about harm reduction.
Table 2
Factors influencing attitudes to drug-assisted rehabilitation (DAR) among Norwegian doctors. Ordinal logistic regression in four separate models with identical covariants. Odds ratio (95 % CI). The variables «list size» and «number of DAR patients last year» are continuous. The ratios shown in bold are significantly different from the reference variables (= 1)
| Experience of DAR¹ |
DAR centre² |
DAR and harm reduction³ |
DAR and benzodiazepines⁴ |
|
| Gender |
||||
| Female |
0.79 [0.57 – 1.10] |
1.08 [0.79 – 1.47] |
1.12 [0.82 – 1.53] |
0.96 [0.70 – 1.32] |
| Male (ref.) |
1 |
1 |
1 |
1 |
| Age |
||||
| 40 or below |
0.58 [0.36 – 0,93] |
1.28 [0.81 – 2.03] |
1.02 [0.64 – 1.63] |
0.71 [0.45 – 1.13] |
| 41 – 55 |
0.76 [0.53 – 1.09] |
0.93 [0.67 – 1.31] |
0.92 [0.65 – 1.29] |
1.04 [0.74 – 1.45] |
| 55 or above (ref.) |
1 |
1 |
1 |
1 |
| List size |
0.99 [0.99 – 1.00] |
1.00 [0.99 – 1.00] |
0.99 [0.99 – 1.00] |
0.99 [0.99 – 1.00] |
| Number of DAR patients last year |
1.13 [1.07 – 1.19] |
1.00 [0.98 – 1.03] |
0.97 [0.94 – 0.99] |
1.07 [1.02 – 1.11] |
| Referral to specialist substance abuse treatment last year |
||||
| Never |
1.34 [0.69 – 2.60] |
0.68 [0.37 – 1.25] |
0.58 [0.31 – 1.07] |
0.69 [0.37 – 1.30] |
| A few times |
1.22 [0.69 – 2.17] |
0.81 [0.48 – 1.39] |
0.58 [0.34 – 1.00] |
0.66 [0.38 – 1.15] |
| Monthly or more (ref.) |
1 |
1 |
1 |
1 |
| Specialist status |
||||
| Non-specialist |
0.82 [0.43 – 1.57] |
1.23 [0.66 – 2.30] |
1.11 [0.59 – 2.10] |
0.91 [0.49 – 1.69] |
| In specialist training |
0.88 [0.57 – 1.36] |
0.73 [0.48 – 1.11] |
1.25 [0.82 – 1.89] |
0.96 [0.63 – 1.46] |
| Specialist (ref.) |
1 |
1 |
1 |
1 |
| Health region |
||||
| Northern |
1.54 [0.84 – 2.80] |
0.76 [0.43 – 1.34] |
0.46 [0.26 – 0.82] |
1.97 [1.11 – 3.48] |
| Central |
1.10 [0.63 – 1.91] |
0.47 [0.28 – 0.81] |
0.42 [0.25 – 0.72] |
0.60 [0.35 – 1.03] |
| Eastern |
0.91 [0.56 – 1.41] |
1.06 [0.70 – 1.60] |
0.90 [0.59 – 1.36] |
1.29 [0.85 – 1.96] |
| Southern |
0.94 [0.57 – 1.56] |
0.40 [0.25 – 0.65] |
0.69 [0.43 – 1.11] |
0.92 [0.57 – 1.49] |
| Western (ref.) |
1 |
1 |
1 |
1 |
| [i] | ||||
[i] ¹ Question asked: How do you find being a DAR doctor?
² Statement made: The DAR centre/specialist health service are of little help
³ Statement made: Drug-assisted rehabilitation is mainly about harm reduction
⁴ Statement made: Some of my DAR patients need benzodiazepines
Discussion
A majority of this sample of Norwegian GPs accept the DAR model, as the surveys of 2000 and 2006 also showed (7). The proportion who are negative towards it is low, while around a third are neutral. A significant minority still have reservations about being the prescribing doctor for the treatment. This proportion was 33 % in 2006, and is at the same level in this survey.
Some have stated that the DAR model is too cumbersome (10) or that the GPs can take on a greater share of the responsibility in the cross-disciplinary collaboration (11). The survey provides little support for this. The majority see a need for cross-disciplinary integration and few wish to take on the sole responsibility. The typical DAR doctor finds it reassuring to work within a collaborative structure with shared responsibility. Very few believe that the role of the specialist health services is an obstacle to treatment, and almost all consider the social services to be important. These considerations are consistent with the bulk of the evaluatory literature, which recommends collaboration between specialist and primary care (13) – (15). The survey shows that doctors take a sober view of what is achieved through drug-assisted rehabilitation, and many judge that the achievement is largely harm reduction, i.e. that the rehabilitation effect is small. However, the evaluations are mainly positive. The implication is that many doctors accept harm reduction as a relevant goal.
Much of the criticism of drug-assisted rehabilitation is linked to the heavy emphasis on monitoring and management of the treatment at the specialist level (10, 12, 16). This has little support among the DAR doctors. The majority do not think that the monitoring is too strict. Urine-test monitoring is well supported. However, a significant minority believe that urine tests could be replaced by counselling and personal contact, and some also believe that it should be possible to prescribe benzodiazepines. Almost no-one supports the proposals by the Stoltenberg Committee for trials of heroin-assisted treatment (17).
In the surveys of 2000 and 2006, gender, age and political orientation were significant for the evaluation of drug-assisted rehabilitation. In this survey political views are not included, and demographic conditions are of little significance. A certain polarity can be detected between younger and more restrictive doctors on the one hand and more DAR-experienced and liberal doctors on the other. The typical doctor has treated approximately five DAR patients and is most satisfied with the guidelines, while those who have most experience appear to want fine-tuning and relaxation of the model. This could be a basis for debate as to whether some doctors, possibly with special training, might have a more independent role.
Opinions about certain aspects of drug-assisted rehabilitation vary among health regions. It is regarded most positively in South and Central Norway, where there is more active collaboration between GPs and the specialist health services (8, 9). This can be viewed as supporting the development of drug-assisted rehabilitation as a collaboration between GPs and a specialist health service with responsibility for follow-up. Similar experiences have been described in Scotland, Australia (18) the US (13, 19) and Canada (20).Also, experience from Ireland, for example, shows that GPs who provide substitution treatment without specialist support may have moderate results (21). However, French experience of GPs issuing prescriptions without any training requirements or any particular guidelines is judged as positive, although the evaluation is mostly not based on systematic surveys. All in all, knowledge of GPs’ experience is somewhat limited. This Norwegian survey is therefore an important contribution.
Despite four reminders, survey participation was relatively low. This is a common experience with questionnaire surveys sent to doctors (22), in particular to GPs (22, 23). A number of international studies have lower participation (24) – (26). Selection bias cannot be ruled out, but the findings are supported by previous representative panels of Norwegian GPs (7). Moreover, the selection is representative of Norwegian GPs in terms of gender, age and list size. Furthermore, the findings correspond to a 2002 survey conducted by the Norwegian General Practitioners’ Association. (27).
There is an over-representation of DAR doctors in the study. This is regarded as favourable, in that the main purpose is to investigate the experience that doctors have of participating in DAR treatment. It is worth noting that the DAR doctors who responded to the survey have treated over half of all DAR patients to whom prescriptions have been issued by GPs. The responses therefore represent a majority of DAR-active doctors. It is possible that doctors with negative experiences of drug-assisted rehabilitation have not wished to participate. However, it is judged to be equally probable that doctors with clear opinions, both positive and negative, are more easily motivated to participate, while doctors with less interest and no clear standpoints may have failed to respond. Moreover, the DAR doctors are representative of the doctors who participated, and the latter in their turn are representative of Norway’s GPs in terms of age, gender and list size, and do not distinguish themselves particularly when it comes to workload and geographical affiliation.
The conclusion is that the DAR model is well adapted to the health-care situation in Norway. There was little opposition to the use of a collaborative model although this does to some extent restrict the autonomy of the individual GP.
Tabell
| Main message |
|
- 1.
WHO. Guidelines for the psychosocially assisted pharmacological treatment of opioid dependence. Genève: WHO, 2009.
- 2.
Gurrik T, Haga W, Hole R et al. MAR I Norge – utvikling, utfordringer og perspektiver. Oslo: MARIO, 2002.
- 3.
Hansen MB, Kornør H, Waal H. SKR-rapport nr. 7/2004. Bidrag til evaluering av Legemiddelassistert rehabilitering i Norge. Oslo: Seksjon for kliniske rusmiddelproblemer, Universitetet i Oslo, 2004.
- 4.
Vindedal B, Steen L-E, Larsen B et al. Evaluering av legemiddelassistert rehabilitering. Rapport til Sosial- og helsedirektoratet. Oslo: Sosial- og helsedirektoratet, 2004.
- 6.
Helsedirektoratet. Nasjonal retningslinje for legemiddelassistert rehabilitering ved opioid avhengighet. Oslo: Helsedirektoratet, 2010.
- 7.
Aasland OG, Spilhaug G, Johannesen A. Fastlegers syn på legemiddelassistert rehabilitering og rusreformen. Tidsskr Nor Legeforen 2009; 129: 97–100. [PubMed]
- 8.
Waal H, Clausen T, Håseth A et al. Statusrapport 2009. Siste år med gamle retningslinjer. Oslo: Senter for rus- og avhengighetsforskning, 2010.
- 9.
Waal H, Clausen T, Håseth A et al. Statusrapport 2010. Første år med nye retningslinjer. Oslo: Senter for rus og avhengighetsforskning, 2011.
- 10.
Haraldsen M. Behandling av opioidavhengige i allmennpraksis. Tidsskr Nor Lægeforen 2007; 18: 2706–7.
- 11.
Skeie I, Brekke M, Lindbæk M et al. Allmennleger kan ta ansvar for legemiddelassistert rehabilitering. Tidsskr Nor Legeforen 2007; 127: 296–7. [PubMed]
- 12.
Christie N, Syse A. Når Metadontilsynet forsvarer sine skanser. Aftenposten 1.1.2002.
- 14.
Kahan M, Wilson L, Midmer D et al. Short-term outcomes in patients attending a primary care-based addiction shared care program. Can Fam Physician 2009; 55: 1108 – 9, e5. [PubMed]
- 16.
Frantzsen E. Metadonmakt. Møte mellom narkotikamisbrukere og norsk metadonpolitikk. Oslo: Universitetsforlaget, 2001.
- 17.
Stoltenbergutvalget. Rapport om narkotika. Oslo: Helse- og omsorgsdepartementet, 2010.
- 20.
Kates N, McPherson-Doe C, George L. Integrating mental health services within primary care settings: the Hamilton Family Health Team. J Ambul Care Manage 2011; 34: 174 – 82. [PubMed]
- 21.
Cullen W, Bury G, Barry J et al. Drug users attending general practice in Eastern Regional Health Authority (ERHA) area. Ir Med J 2000; 93: 214 – 7. [PubMed]
- 22.
Flanigan T, McFarlane E, Cook S. Conducting survey research among physicians and other medical professionals. A review of current litterature. Alexandria, VA: Proceedings of the Survey Research Methods Section, American Statistical Association, 2008: 4136 – 47.
- 23.
Aasland OG, Falkum E. Legekårsundersøkelsen. Tidsskr Nor Lægeforen 1994; 114: 3054 – 8.
- 24.
Bestmann B, Rohde V, Wellmann A et al. Zufriedenheit von Ärztinnen und Ärzten. Dtsch Arztebl 2004; 101: 28 – 32.
- 26.
Shanafelt TD, Balch CM, Bechamps GJ et al. Burnout and career satisfaction among American surgeons. Ann Surg 2009; 250: 463 – 71. [PubMed]
- 27.
Steinert S, Maartman-Moe K. Allmennlegens rolle i behandlingen av narkomane – legemiddelassistert rehabilitering. Tromsø/Oslo: Alment praktiserende lægers forening, Den norske legeforening, 2002.