Dementia and neuropsychiatric symptoms in nursing-home patients in Nord-Trøndelag County
Dementia is a syndrome that encompasses cognitive failure, change of behaviour and/or social functioning and failure to function in daily life. Approximately 70 000 persons suffer from dementia in Norway (1). The most frequently occurring forms are Alzheimer’s disease, vascular dementia, frontotemporal lobe dementia, Parkinson’s disease, dementia with Lewy bodies and alcohol-induced dementia.
Many patients with dementia experience anxiety, depression, hallucinations, delusions, aggression, aberrant motor behaviour, apathy or changes in appetite or sleeping habits. These symptoms are grouped under the designations of neuropsychiatric symptoms of dementia or behavioural and psychological symptoms of dementia. Cognitive failure and neuropsychiatric symptoms are a burden on the patient, the next of kin and the care personnel (2). Neuropsychiatric symptoms may lead to more use of coercion (3) and increased use of psychotropic drugs (4). Biological, psycho-social and environmental factors all have a bearing on the development of neuropsychiatric symptoms (5).
Previous studies have shown that approximately 80 % of Norwegian nursing-home patients suffer from dementia, and that approximately 70 % of the patients with dementia have clinically significant neuropsychiatric symptoms (6, 7). Corresponding figures have been reported from the Netherlands and the UK (8) – (10). Previous factor analyses have shown that neuropsychiatric symptoms can be grouped into four categories: psychotic symptoms, affective symptoms, symptoms of agitation and symptoms of apathy (11).
Nord-Trøndelag County encompasses 23 municipalities, with a mixture of urban and rural municipalities with coastal and inland settlements. We wished to study the prevalence of dementia in nursing homes in Nord-Trøndelag County and describe the prevalence of neuropsychiatric symptoms in patients with dementia. We also wished to identify sub-groups of neuropsychiatric symptoms, i.e. symptoms that may be relevant to understanding the causes of dementia and thus help improve treatment methods.
Material and methods
All patients in all of the 32 nursing homes in Nord-Trøndelag County were invited to participate in the study. The inclusion criterion was that the patient had been in the nursing home for at least two weeks. Of a total of 979 relevant patients, 259 were excluded because the patient or his/her next of kin refused (n = 179), or because of somatic illness (n = 24), death before the data collection started (n = 17), because the patient had been discharged from the nursing home (n = 1) or for unknown reasons (n = 20). Altogether 16 of the 720 patients included had not been assessed with the aid of the Clinical Dementia Rating Scale. A total of 704 patients were thus included in the study.
Data collection
The data collection took place from June 2010 to March 2011, and was based on standardised interviews with patients and health personnel in the nursing homes. Nine project nurses with extensive clinical experience were charged with the collection of data. They received two days of training in the use of the registration form, as well as a general introduction to the study. The registration comprised examination of neuropsychiatric symptoms, symptoms of depression, daily functioning, degree of dementia and somatic illness.
The Clinical Dementia Rating Scale ranks the degree of seriousness of the dementia illness in six categories (12). Each category is scored from 0 to 3, where 0 = no dementia, 0.5 = possible dementia, and 1, 2 or 3 denote mild, moderate and serious dementia respectively. The total score is calculated according to an algorithm that gives added weight to failing memory.
The Neuropsychiatric Inventory is a form for identification of 12 neuropsychiatric symptoms of dementia (13). Scores are entered for the frequency and degree of seriousness of each symptom over the last four weeks, and subsequently multiplied into a symptom score (0 – 12 points), where higher scores denote more serious symptoms. A symptom score of 4 or higher is defined as clinically significant (14). The Norwegian version of the Neuropsychiatric Inventory has been tested for reliability and validity (15). The prevalence of neuropsychiatric symptoms was compared to the prevalence reported by a previous study undertaken in four other Norwegian counties in 2004 – 05 (7).
Lawton’s physical self-maintenance scale measures the patient’s ability to cope with six activities of daily life (ADL). Total scores range from 0 to 30, and a higher score indicates a poorer ability to function (16). The General Medical Health Rating Scale is a four-point scale for scoring of the degree of somatic illness. The scores were dichotomised into serious somatic illness (the two top scores) and good somatic health (the two lowest scores) (17).
Ethics and data protection
Depending on the patient’s ability to provide consent, the patient him-/herself or the next of kin provided consent for participation in the study. The study was approved by the Central Norway Regional Committee for Medical and Health Research Ethics.
Statistical analysis
The analyses were undertaken with the aid of Statistical Product and Service Solutions (SPSS), version 18.0. The data were described through frequency distributions of categorical variables, mean values and standard deviations for continuous variables with a normal distribution, and the median value and inter-quartile range (IQR) for non-normally distributed continuous variables. Continuous data were compared using Student’s t-test if they were normally distributed or with the Mann-Whitney U-test if they were non-normally distributed, while categorical variables were compared by cross-tabulation.
We undertook an exploratory factor analysis, in which the extraction factors were decided by an eigenvalue > 1 and inspection of the pattern formed by the eigenvalues (scree plot). The criterion for adequate adaptation of the factor analysis was a significant finding by Bartlett’s test of sphericity and the Kayser-Meyer-Olkins (KMO) measure for adequate sample size > 0.7. The factor analysis was undertaken using oblique (direct oblimin) rotation.
Results
Demographic variables for all the patients are listed in Table 1. When assessed with the Clinical Dementia Rating scale, altogether 575 patients (82 %) had dementia. These patients suffered more frequently from serious somatic diseases and had a higher degree of functional failure, but a significantly lower use of drugs than patients without dementia (Table 1).
Table 1
Demographic data and findings for 704 nursing-home patients in Nord-Trøndelag County examined for dementia in 2010 – 11 with the aid of the Clinical Dementia Rating scale. P-values denote the differences between patients with and without dementia. Figures are in real numbers ( %), unless stated otherwise.
| All (N = 704) |
With dementia (n = 575) |
Withoutdementia (n = 129) |
P-value |
|
| Age in years, average (standard deviation) |
84.5 (8.3) |
84.7 (8.1) |
84.1 (8.9) |
|
| ADL score, average (standard deviation) |
17.9 (5.7) |
18.8 (5.4) |
13.5 (4.7) |
< 0.001¹ |
| Number of drugs, average (standard deviation) |
6.7 (3.6) |
6.3 (3.3) |
8.3 (4.5) |
< 0.001¹ |
| Women |
500 (71) |
409 (71) |
91 (71) |
|
| Marital status |
||||
| Unmarried |
67 (10) |
50 (9) |
17 (13) |
|
| Married |
170 (25) |
146 (26) |
24 (19) |
|
| Widow/-er |
428 (62) |
347 (62) |
81 (63) |
|
| Divorced/separated |
26 (4) |
21 (4) |
5 (4) |
|
| Serious somatic disease |
359 (50) |
302 (53) |
47 (37) |
0,001² |
| Regular use of drugs |
659 (94) |
540 (94) |
119 (92) |
|
| Regular use of psychotropic drugs |
440 (63) |
355 (62) |
85 (66) |
|
| Clinical Dementia Rating (form) |
||||
| 0 |
33 (26) |
|||
| 0,5 |
96 (74) |
|||
| 1 |
125 (22) |
|||
| 2 |
164 (29) |
|||
| 3 |
286 (50) |
|||
| [i] | ||||
[i] ¹ T-test
² Chi-square test
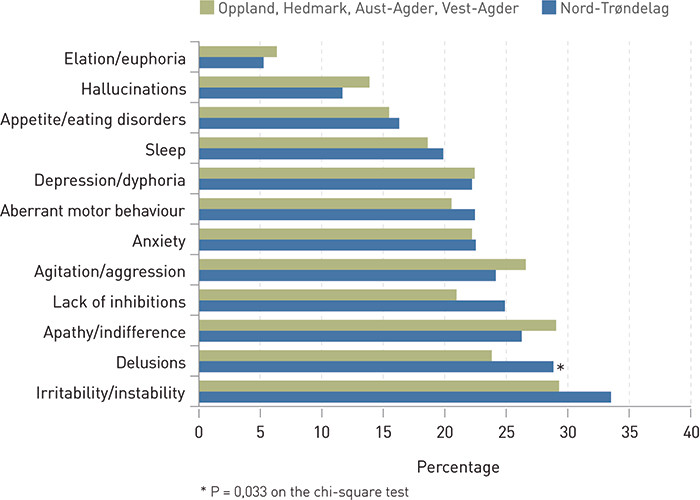
The proportion of patients who had clinically significant neuropsychiatric symptoms is shown in Figure 1, and compared to corresponding data in a study of Norwegian nursing homes from 2004 – 05 (7). Of all the patients with dementia, 75 % had one or more clinically significant neuropsychiatric symptoms. The three most frequently occurring symptoms were delusions, apathy and irritability. With the exception of delusions, which were more common in our study (p =0.033), there were no differences in the prevalence of individual symptoms between our study and the study from 2004 – 05.
In a factor analysis of the neuropsychiatric inventory, undertaken as a principal-component extraction analysis of the sub-symptoms in the inventory, four factors were identified (Table 2). For the model, Bartlett’s test of sphericity was significant (p < 0.001) and the Kayser-Meyer-Olkins measure of adequate sample size was 0.82, i.e. above 0.7, which is common in corresponding studies.
Table 2
Principal-component extraction analysis (PCA) of the neuropsychiatric inventory for 704 nursing-home patients in Nord-Trøndelag County, examined for dementia and neuropsychiatric symptoms in 2010 – 11. Figures in bold denote symptoms with factor loading above 0.5.
| Factor 1 |
Factor 2 |
Factor 3 |
Factor 4 |
|
| Agitation |
Apathy |
Psychosis |
Affective symptoms |
|
| Delusion |
0.08 |
–0.16 |
0.64 |
–0.37 |
| Hallucination |
–0.01 |
–0.17 |
0.73 |
–0.16 |
| Agitation |
0.67 |
0.14 |
0.20 |
–0.12 |
| Depression |
0.13 |
0.20 |
–0.14 |
–0.80 |
| Anxiety |
0.22 |
0.00 |
0.20 |
–0.74 |
| Elation |
0.64 |
–0.16 |
0.17 |
–0.03 |
| Apathy |
–0.04 |
0.72 |
–0.05 |
–0.21 |
| Lack of inhibitions |
0.80 |
0.21 |
0.10 |
0.08 |
| Irritability |
0.70 |
0.11 |
0.15 |
–0.15 |
| Motor unrest |
–0.06 |
0.34 |
0.68 |
0.10 |
| Nocturnal unrest |
0.24 |
0.02 |
0.53 |
0.14 |
| Appetite |
0.07 |
0.74 |
0.00 |
–0.04 |
Agitation (Factor 1) encompassed agitation, elation, irritability and lack of inhibitions. Apathy (Factor 2) encompassed symptoms of apathy as well as appetite and eating disorders. Psychosis (Factor 3) encompassed delusions, hallucinations, aberrant motor behaviour and sleeping disorders. Affective symptoms (Factor 4) encompassed depression and anxiety. We also estimated the correlations between the factors. Agitation and psychosis had the highest positive correlation, while agitation and affective symptoms had the highest negative correlation.
Discussion
This study shows that there is a high prevalence of dementia among nursing-home patients in Nord-Trøndelag County. Many of the patients suffering from dementia also had one or more additional neuropsychiatric symptoms. The prevalence of dementia and neuropsychiatric symptoms was comparable to the prevalence in a previous study undertaken in four Norwegian counties in 2004 – 05 (7).
There were no statistically significant differences between the two studies, with the exception of the prevalence of delusions. It is possible that the prevalence of neuropsychiatric symptoms varies more between the wards of an individual nursing home or between different nursing homes in the same county than within a sample of patients from different counties, but we have not undertaken any such analysis. The statistically significant difference in the prevalence of delusions is small, however, and should not be given undue weight. The similarity in the prevalence of neuropsychiatric symptoms in the two studies may indicate that the frequency of such symptoms is independent of external factors, such as the organisation of the nursing-home services and the use of medications, and rather a characteristic of the dementia illness itself.
The factor analysis of neuropsychiatric symptoms in our study identified four factors: psychosis, agitation, affective symptoms and apathy. Another longitudinal Norwegian study of nursing homes found that the same four factors were the most stable ones (11). The stable pattern in the factor structure revealed by these studies, across geographical regions and time periods of data collection, indicates that certain sub-groups of patients with dementia have recognisable patterns of neuropsychiatric symptoms. This is corroborated by international studies that have made similar findings (18). The subdivision of neuropsychiatric symptoms into such factors is useful as an outcome measure in studies and for evaluation of the causes of symptoms and the effects of drug therapies.
One of the strengths of this study is its inclusion of a large number of patients over several nursing homes. The size of the cohort indicates that it is representative for nursing-home patients in Nord-Trøndelag County. The use of standardised registration forms which have been validated in Norwegian and are widely used in international research is also a crucial element. In addition, the study employed a limited number of data collectors, all of whom had been trained in the use of the registration instruments prior to the start of the data collection.
The lack of a verified dementia diagnosis is a limitation, although previous studies have shown that dementia diagnosed with the aid of the clinical dementia rating scale is a valid substitute for diagnosis by clinical examination (19, 20). The fact that a relatively high number of patients refused to participate or were excluded for other reasons represents a further limitation.
Conclusion
There is a high prevalence of dementia among nursing-home patients in Nord-Trøndelag County, and many of the patients suffering from dementia have one or more additional neuropsychiatric symptoms, of which delusions, apathy and irritability occur most frequently. The high prevalence of dementia and neuropsychiatric symptoms is of significance for the clinical practice, running and planning of nursing homes, and shows that health personnel need to be competent in the field of dementia and neuropsychiatric symptoms.
The study is part of the health and memory project in Nord-Trøndelag County, which is undertaken as a collaboration between HUNT, Norwegian University of Science and Technology, The Norwegian Institute of Public Health, Central Norway Regional Health Authority, Northern Norway Regional Health Authority, Nord-Trøndelag Health Enterprise, The County Governor of Nord-Trøndelag, Nord-Trøndelag division of the Norwegian Association of Local and Regional Authorities and the Research Centre for Old-Age Psychiatry, Innlandet Hospital Trust.
Tabell
| Main message |
|
- 1.
Engedal K, Haugen PK. Demens, fakta og utfordringer. Oslo: Nasjonalt kompetansesenter for aldersdemens, 2004.
- 4.
Bartels SJ, Horn SD, Smout RJ et al. Agitation and depression in frail nursing home elderly patients with dementia: treatment characteristics and service use. Am J Geriatr Psychiatry 2003; 11: 231 – 8. [PubMed]
- 5.
Rongve A, Auning E, Ehrt U et al. Psykose ved Parkinsons sykdom. Tidsskr Nor Legeforen 2012; 132: 155-8. [PubMed]
- 12.
Berg L. Clinical Dementia Rating (CDR). Psychopharmacol Bull 1988; 24: 637 – 9. [PubMed]
- 17.
Lyketsos CG, Galik E, Steele C et al. The General Medical Health Rating: a bedside global rating of medical comorbidity in patients with dementia. J Am Geriatr Soc 1999; 47: 487 – 91. [PubMed]
- 19.
Engedal K. The prevalence of dementia in a sample of elderly Norwegians. Int J Geriatr Psychiatry 1993; 8: 565 – 70. [CrossRef]