Self-monitoring of blood glucose forms part of the treatment regime for many patients with diabetes mellitus. There is consensus about the usefulness of self-monitoring by patients who use insulin, not least because the monitoring can prevent hypoglycemic episodes (1) – (3). However, the usefulness has not been documented in patients who are not on insulin (4) – (8). Nevertheless, self-monitoring is often recommended to these patients (9) – (12).
Sales of antidiabetics are rising. In 2009 sales of blood glucose-lowering drugs reached NOK 458.6 million, 4.7 % up on 2008 (13). There are a number of studies that report on diabetes prevalence in the Norwegian population (14) – (16). By using data obtained from the Norwegian Prescription Database, Strøm et al. found that the prevalence for medicinally treated diabetes in 2004 was 2.6 % among men and 2.2 % among women (14). This is consistent with the prevalence estimated by Stene et al. in 2002, where data from a number of Norwegian population surveys were used to estimate the overall Norwegian diabetes prevalence, adjusted for gender and age, to 2.3 % (15). However, Stene et al. reported significant variation between the numeric outcomes of the different surveys and called for studies that would shed light on regional differences (15). More recent findings from the Nord-Trøndelag Health Study (HUNT III) indicate that the diabetes prevalence has soared in recent years, to 3.8 % in women and 4.9 % in men (16).
There has been a shortage of studies on the scope and use of blood glucose self-monitoring in this patient group, internationally as well as nationally. A Dutch study found significant geographic differences with respect to the time it took from a patient was put on antidiabetic drugs until strips were made available to them (17). We have previously published a study which demonstrated a national self-monitoring prevalence of approx. 2 %, and estimated that approx. 70 % of patients who are receiving medicinal treatment for diabetes carry out self-monitoring (18). Total sales of glucometer strips was approx. NOK 355 million in 2008. We found significant variation between patients with respect to the amount of strips they purchased; approx. 45 % of patients collected sufficient strips to carry out daily meter readings while 1 % collected a number of strips equivalent to more than ten readings per day. This one per cent of patients accounted for 8 % of the total cost of strips (18).
This article investigates regional differences, county by county, between the prevalence of patients on antidiabetics in Norway, and the regional differences in the use of glucometer strips.
Material and method
Data
In Norway, self-monitoring strips are usually prescribed by the patient’s GP, but because the strips are defined as medical equipment, they are not subject to registration in the Norwegian Prescription Database. We received data from The Norwegian Health Economics Administration (HELFO) on all glucometer strips sold through pharmacists or orthotists to non-institutionalized patients in 2008. The following variables were included: ID number (anonymous identification number replacing the person’s birth registration number), age group, sex, place of sale (pharmacist or orthotist), county, date of collection, product serial number, product name, quantity and the pharmacy’s retail price.
We also obtained data from the Norwegian Prescription Database, the Norwegian Institute of Public Health (19), on all ATC A10A drugs (insulins and analogues) and A10B drugs (blood glucose lowering drugs except insulin) sold in 2008, including the following variables: sex, age group, county, number of users, and number of users per 1 000 inhabitants, as well as the cost in Norwegian currency. Each county’s age demographics as at 1 January 2008 were obtained from Statistics Norway (SSB) (20). Strips and drugs purchased through hospitals and nursing homes are not included, either in the Norwegian Prescription Database or in the data provided by HELFO. Consequently, the study includes no data for the use of antidiabetics or glucometer strips by patients who have been admitted to hospital or a nursing home, for a shorter or longer period.
The use of strips and drugs
In order to compare the user prevalence in the various counties, we make use of CPFs (comparative prevalence figures), calculated using CMF formulas (comparative mortality figure) (21). CPFs are here used to compare the prevalence of use within a certain geographic area to the national average. If the CPF is below 1, the area has a lower prevalence than the national average, while a CPF above 1 means that the area has a higher prevalence than the national average. CPFs are adjusted to account for the fact that different counties have different age demographics, and this enables us to make a direct comparison with other counties and with the national average. It also enables us to calculate the confidence interval of adjusted values. The age demographics of each county have been obtained from Statistics Norway. In our case, each county’s CPF was calculated as:
CPF = expected number of patients/observed number of patients
Spearman’s rank correlation was used to investigate the degree of correlation between the proportion of strip users and the proportion of blood glucose-lowering drugs.
Consumption of strips and drugs per user
In addition to looking at the number of users within each county, we have also looked at the amount of drugs and strips used per person. Each county’s average drug and strip consumption was adjusted for age by multiplying the county’s number of patients within each age group by the nation-wide proportion of patients in that age group. The adjusted number of users was then multiplied by the average consumption within this county’s relevant age group. The outcomes for each age group were then added up to find total average consumption adjusted for age.
Analyses were conducted in SPSS v.15 and Microsoft Excel v.14.1.2.
Results
Table 1 shows the prevalence of medicinally treated diabetes in Norway by sex and age group. The figures include everyone who has collected drugs from the ATC-group A10, i.e. anyone who uses insulin and/or other blood glucose-lowering drugs. A total of 139 098 individuals collected A10 class drugs in 2008, which gives a prevalence of medicinally treated diabetes of 2.9 %.
Table 1
Prevalence of medicinally treated diabetes in Norway in 2008
| Age group |
Number of people |
Prevalence (%) |
|||
| Women |
Men |
Women |
Men |
||
| < 30 |
4 141 |
3 796 |
0.5 |
0.4 |
|
| 30 –39 |
4 509 |
4 161 |
1.4 |
1.2 |
|
| 40 –49 |
6 386 |
9 034 |
1.9 |
2.6 |
|
| 50 –59 |
9 642 |
15 405 |
3.2 |
5.0 |
|
| 60 –69 |
13 910 |
21 094 |
5.7 |
8.7 |
|
| 70 –79 |
13 133 |
14 290 |
8.3 |
10.8 |
|
| 80+ |
11 577 |
8 020 |
7.7 |
9.8 |
|
| All ages |
63 298 |
75 800 |
2.6 |
3.2 |
|
Table 2 shows the number of patients per 1,000 inhabitans who used insulin, other blood glucose-lowering drugs (BGLD and glucometer strips in Norway in 2008, by county, in absolute figures. The prevalence of average national insulin use is 10.7 individuals/1,000 inhabitants, for other blood glucose-reducing drugs it is 22.1 individuals/1,000 inhabitants, and for strips 21.1 individuals/1,000 inhabitants.
Table 2
Sales of insulin, other blood glucose-lowering drugs (BGLD) and glucometer strips in 2008. Given as users /1 000 inhabitants, per county and overall for the whole country, sorted by prevalence of strip users in descending order.
|
|
Insulin |
BGLD |
Insulin and/or BGLD |
Strips |
Total population |
| Hedmark |
13.0 |
31.2 |
38.6 |
26.8 |
189 693 |
| Østfold |
12.7 |
26.6 |
34.9 |
25.8 |
267 011 |
| Nordland |
12.4 |
24.1 |
31.9 |
25.4 |
235 168 |
| Nord-Trøndelag |
12.7 |
27.7 |
35.0 |
25.2 |
130 257 |
| Finnmark |
11.1 |
27.1 |
32.6 |
24.6 |
72 445 |
| Oppland |
12.3 |
22.8 |
31.4 |
24.1 |
183 952 |
| Buskerud |
12.2 |
25.0 |
33.2 |
23.8 |
252 924 |
| Telemark |
12.6 |
23.6 |
32.1 |
22.7 |
167 138 |
| Sogn og Fjordane |
11.6 |
21.6 |
29.2 |
22.6 |
106 346 |
| Troms |
11.4 |
23.5 |
29.7 |
22.6 |
155 091 |
| Møre og Romsdal |
11.4 |
21.7 |
29.3 |
22.0 |
247 714 |
| Vestfold |
10.1 |
22.6 |
29.7 |
21.2 |
227 809 |
| Vest-Agder |
11.0 |
19.3 |
27.4 |
20.9 |
167 096 |
| Aust-Agder |
11.6 |
20.0 |
28.6 |
20.3 |
106 733 |
| Oslo |
8.9 |
21.1 |
26.9 |
19.3 |
567 944 |
| Sør-Trøndelag |
9.8 |
20.9 |
27.3 |
19.1 |
284 874 |
| Akershus |
9.4 |
19.5 |
25.8 |
18.2 |
523 100 |
| Hordaland |
9.9 |
20.2 |
26.9 |
18.2 |
466 166 |
| Rogaland |
9.2 |
17.6 |
24.0 |
17.0 |
416 614 |
| All counties |
10.7 |
22.1 |
29.2 |
21.1 |
4 768 075 |
Because the use of drugs and strips varies with age (18), the age demographics of any county will affect the number of users as well as the quantities used. Figure 1 shows age-adjusted 95 % confidence intervals for prevalence of strip and drug use by county, relative to the national average. The figure shows that there are statistically significant differences between counties when it comes to the use of both strips and drugs, even when adjusted for the counties’ age demographics. Hedmark has the highest prevalence of patients on antidiabetics, with 1.16 times the national average. Rogaland has the lowest age-adjusted prevalence (0.91 times the national average). This means that Hedmark has 27.5 % more patients who are treated medicinally for diabetes than Rogaland.
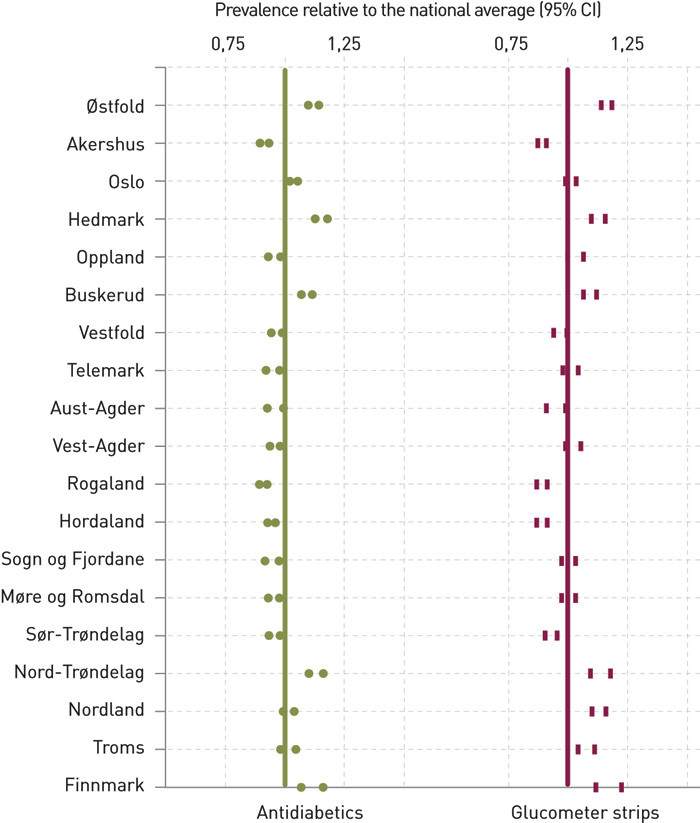
Finnmark has the highest prevalence of strip use after adjusting for age (1.17 times higher than the average), while Akershus, Rogaland and Hordaland are at the bottom of the list with 0.89 times the national average. This means that there are 31.5 % more patients using glucometer strips in the counties with the highest prevalence compared to the counties with the lowest prevalence.
The correlation between the number of individuals who use glucometer strips and the number of individuals on antidiabetics varies from 0.68 in Hordaland to 0.80 in Nordland; nationally the correlation is 0.73. Spearman’s rank correlation gives a rho of 0.83, 95 % KI 0.60 – 0.94, p = 0.001, and shows a clear correlation between use of medication and use of strips within each county.
Just like the number of users per county varies, there are also differences between counties when it comes to the money spent on drugs per user and the number of strips collected per user. On average, a total of NOK 3,300 was spent on antidiabetic drugs per user in 2008. Finnmark has the lowest consumption, with NOK 2 971 per user, whereas Vestfold has the highest consumption, with NOK 3,675 per user, i.e. 23.7 % more. The figures have been adjusted for the age demographics of each county. If all the country’s diabetes patients consumed drugs at the rate of those in Vestfold, the national bill for diabetes drugs would be NOK 95.4 million higher than if all patients consumed drugs at the rate of those in Finnmark.
The use of strips also varies between counties, even if we adjust for age. The national average is 1.75 strips per user per day. People in Østfold, Hedmark, Oppland, Nord-Trøndelag, Nordland, Troms and Finnmark all use less than the national average, while people in Akershus, Oslo, Buskerud, Telemark, Vestfold, Aust-Agder and Vest-Agder use more than the average. The average consumption is lowest in Finnmark, where they use 1.39 strips per user per day, and highest in Vest-Agder where the corresponding figure is two strips per day. Their expenditure is therefore 44 % higher. In a year, the difference between the counties with the highest and lowest consumption amounts to approx. 223 strips per user. If all of the country’s diabetes patients used the same number of strips as those in Vest-Agder, the national spend on strips would have been NOK 133.5 million higher than if all diabetes patients had the same consumption as those in Finnmark.
Discussion
The figures in this study only describe purchases of strips and medication, not the real scope of their use. It is quite possible that a considerable number of strips bought are never used, and that patients keep a store of strips «just in case », or they may change their meter and therefore throw away a quantity of unused strips. These eventualities would give rise to an overestimation of the strip consumption per person. However, the relationship between used/purchased strips should not vary to any major extent between counties, and the difference in consumption is therefore relevant, even if the level may be slightly high. It is not very likely that the prevalence figures are affected by this, as we may legitimately presume that people who have bought strips will have taken a meter reading at one point or another, even if they do not do so regularly. There may be some degree of uncertainty with regard to the number of users of glucometer strips, as the data from HELFO provide no information about the individual patients’ county of residence, only the county where the purchase was made. The same user may therefore have been counted repeatedly if this individual has picked up strips from pharmacies in more than one county.
This study has found that the average prevalence of antidiabetics in 2008 was 2.9 %. The prevalence in the various age and sex groups (tab 1), is higher than that described by Strøm et al., who used the Norwegian Prescription Database’s figures from 2004 and the first half of 2005 (14). Our figures are also somewhat higher than Stene et al.’s estimate of diabetes prevalence, except in the highest age group, 80+, where they found a prevalence of 12.4 % (women) and 11.5 % (men), compared to our figures of 7.7 % and 9.8 % respectively (15). Stene reports the prevalence of all patients with diabetes, including those who are not being treated medicinally. It is possible that a greater proportion of the oldest diabetes patients is treated by diet alone. T
his, combined with the fact that a considerable proportion of patients in this age group are nursing home residents and therefore not included in our statistical material, may go some way towards explaining why our oldest age group differs from the figures presented by Stene et al. Because their prevalence figures include all patients with diabetes, we had expected their figures to be higher than ours for all age groups. When this is not the case, our figures suggest that there has been a real rise in the prevalence of diabetes. This is consistent with the findings presented by Midthjell et al. in the HUNT III study (16), which reported an even higher prevalence than us. Their data also include all diabetes patients, including those whose treatment is solely dietary, and this may provide some of the explanation why their figures are even higher than ours. It is also worth noting that our study ranks Nord-Trøndelag (where Midthjell collected his data) as the county with the highest prevalence of medicinally treated diabetes. Despite the fact that the prevalence figures for patients over 40 years of age are different for men and women, we have chosen not to adjust our county-wise comparisons for sex, as the proportion of women to men in each county differs only to a minimal degree (22).
We found statistically significant differences between counties both with respect to the prevalence of use of antidiabetics and with respect to self-monitoring. Despite some variation in the relationship between the number of strip users and the number of drug users (17 % difference between the highest and lowest ranking county in terms of strip users), Figure 1 shows that the purchase of strips correlates reasonably well with the variations in drug use. This suggests that there is a real difference between the counties with respect to the prevalence of medicinally treated diabetes. The health surveys to which Stene et al. refer also finds regional differences in diabetes prevalence, both for established and previously undiagnosed diabetes (15).
Diabetes prevalence varies with ethnicity (23) – (26), but because our data includes no information about ethnicity, we have been unable to establish whether this contributes to the differences we have observed.
We may ask whether or not regional differences of 30 – 40 % are significant. It is not entirely uncommon to observe regional health differences of these proportions. According to Statistics Norway, sickness absence varies from 6.2 % in Rogaland to 8.8 % in Troms, a difference of 42 % (27). The percentage of smokers varies from 16 % in Oslo to 31 % in Finnmark, a difference of close to 100 % (28). The «Health in Norway » report from 2001 reported that the consumption of sedatives and sleeping pills in Finnmark is less than half the consumption in Østfold (not adjusted for age). The report lists factors such as demography (age), the population-to-pharmacy ratio, the population-to-physician ratio, the population-to-hospital ration and access to health services as possible explanations, but also says that the differences may be linked to different therapy traditions and attitudes to medication (29). We have adjusted for age differences between counties, but other variables will also be relevant to our findings.
There is a slightly larger discrepancy between counties with respect to the consumption of strips per person (43.9 %) compared to the consumption of drugs per person (23.7 %). This may be because it is difficult to set a «correct» frequency for self-monitoring by diabetes patients, and both national and international guidelines are vague on frequency recommendations (10, 11, 30). From pharmacies we know it is normal for prescriptions to state the amount of strips to be dispensed as «one year’s supply», and that doctors tend to leave the decision about frequency of readings and type of meter to the patient or the pharmacy staff. Since no upper limit has been set for the total number of strips that may be collected, patients may collect virtually unlimited numbers. Earlier studies among Norwegian diabetes patients indicate that a considerable proportion of patients are self-taught in the skills of glucose monitoring, and that very few have the quality of their readings checked (31, 32). International studies have shown that self-monitoring of blood glucose in patients who are not using insulin, may lower their quality of life (3, 33). This indicates that GPs should consider whether it is strictly necessary for patients to perform self-monitoring of blood glucose. It is important that those patients who have self-monitoring recommended to them are explained the measurements’ objective, and the GP and the patient should agree on an appropriate frequency regime. GPs should be clearer as to whether they wish to take responsibility for teaching their patients how to use the glucometer and then follow up with quality controls of readings, or whether they wish to delegate this job to other health personnel, such as at diabetes outpatients clinics or pharmacy personnel.
We would like to thank Senior Consultant David Scott Lauritzen at HELFO for making the data on sales of glucometer strips available for our study; and Kari Nerhus at NOKLUS for her initiatives and assistance at the planning stage.
Tabell
| Main message |
|
- 1.
Patel A. Diabetes in focus. 2. utg. London: Pharmaceutical Press; 2003.
- 2.
Tests of glycemia in diabetes. Diabetes Care 2000; 23 (suppl 1): S80 – 2.
- 3.
Franciosi M, Pellegrini F, De Berardis G et al. The impact of blood glucose self-monitoring on metabolic control and quality of life in type 2 diabetic patients: an urgent need for better educational strategies. Diabetes Care 2001; 24: 1870 – 7.
- 4.
Towfigh A, Romanova M, Weinreb JE et al. Self-monitoring of blood glucose levels in patients with type 2 diabetes mellitus not taking insulin: a meta-analysis. Am J Manag Care 2008; 14: 468 – 75.
- 5.
Welschen LM, Bloemendal E, Nijpels G et al. Self-monitoring of blood glucose in patients with type 2 diabetes who are not using insulin: a systematic review. Diabetes Care 2005; 28: 1510 – 7.
- 6.
Davidson MB. Counterpoint: Self-monitoring of blood glucose in type 2 diabetic patients not receiving insulin: a waste of money. Diabetes Care 2005; 28: 1531 – 3.
- 7.
Martin S, Schneider B, Heinemann L et al. Self-monitoring of blood glucose in type 2 diabetes and long-term outcome: an epidemiological cohort study. Diabetologia 2006; 49: 271 – 8.
- 8.
Klonoff DC, Bergenstal R, Blonde L et al. Consensus report of the coalition for clinical research-self-monitoring of blood glucose. J Diabetes Sci Technol 2008; 2: 1030 – 53.
- 9.
Bergenstal RM, Gavin JR 3rd. The role of self-monitoring of blood glucose in the care of people with diabetes: report of a global consensus conference. Am J Med 2005; 118 (suppl 9A): 1S-6S.
- 10.
Claudi T. red. Nasjonale faglige retningslinjer: diabetes – forebygging, diagnostikk og behandling. Oslo: Helsedirektoratet, 2009.
- 11.
Standards of medical care in diabetes–2011. Diabetes Care 2011; 34 (suppl 1): S11 – 61.
- 12.
Austin MM, Haas L, Johnson T et al. Self-monitoring of blood glucose: benefits and utilization. Diabetes Educ 2006; 32: 835 – 6, 844 – 7.
- 13.
Apotekforeningen. Apotek og drugs 2010 – bransjestatistikk om apotekenes virksomhet og rammevilkår. Oslo: Apotekforeningen, 2010.
- 14.
Strøm H, Engeland A, Eriksen E et al. Hvor mange og hvem behandles medikamentelt for diabetes mellitus? Tidsskr Nor Lægeforen 2006; 126: 768 – 70.
- 15.
Stene LC, Midthjell K, Jenum AK et al. Hvor mange har diabetes mellitus i Norge? Tidsskr Nor Lægeforen 2004; 124: 1511 – 4.
- 16.
Midthjell K, Lee CMY, Langhammer A et al. Obesity and type 2 diabetes still increase while other cardiovascular disease risk factors decline. The HUNT study, Norway. Abstract. Obes Rev 2010; 11 (suppl): 58.
- 17.
Storimans MJ, Klungel OH, Talsma H et al. Regional influences on the dispensing of glucose test strips in Dutch community pharmacies. Pharm World Sci 2006; 28: 26 – 32.
- 18.
Kjome RL, Granas AG, Nerhus K et al. The prevalence of self-monitoring of blood glucose and costs of glucometer strips in a nationwide cohort. Diabetes Technol Ther 2010; 12: 701 – 5.
- 19.
Reseptregisteret (NorPD). Nasjonalt folkehelseinstitutt. www.reseptregisteret.no (8.8.2011).
- 20.
Statisktisk sentralbyrå. Folkemengd, etter alder og fylke. Absolutte tal. 1. januar 2008. www.ssb.no/utlstat/arkiv/tab-2008-02-21-01.html. (10.8.2011).
- 21.
Higham J, Flowers J, Hall P. INphoRM Standardisation. Measures of disease frequency. INphoRM series. Cambridge, Eastern Region Public Health Observatory, Institute of Public Health. Sist oppdatert 19.5.2005. www.erpho.org.uk/Download/Public/12267/1/INPHORM%206%20FINAL.pdf (15.8.2011).
- 22.
Statistisk Sentralbyrå. Befolkningsstatistikk. Folkemengd, etter kjønn and alder. www.ssb.no/befolkning/ (30.8.2011).
- 23.
Ziemer DC, Kolm P, Weintraub WS et al. Glucose-independent, black-white differences in hemoglobin A1c levels: a cross-sectional analysis of 2 studies. Ann Intern Med 2010; 152: 770 – 7.
- 24.
Jørgensen ME, Bjerregaard P, Borch-Johnsen K et al. New diagnostic criteria for diabetes: is the change from glucose to HbA1c possible in all populations? J Clin Endocrinol Metab 2010; 95: E333 – 6.
- 25.
Cowie CC, Rust KF, Byrd-Holt DD et al. Prevalence of diabetes and high risk for diabetes using A1C criteria in the U.S. population in 1988 – 2006. Diabetes Care 2010; 33: 562 – 8.
- 26.
Getaneh A, Andres R, Brillon DJ et al. The A1c Criterion for Diabetes Diagnosis among Hispanic and Non-Hispanic Populations. Endocr Pract 2011; 17: 210 – 7 .
- 27.
Statistisk sentralbyrå. Sykefravær, egen- og legemeldt, 2. kvartal 2011. www.ssb.no/emner/06/02/sykefratot/ (30.8.2011).
- 28.
Statistisk sentralbyrå. Røykevaner 2010. www.ssb.no/emner/03/01/royk/ (30.8.2011).
- 29.
Helsetilstand og behandlingstilbud belyst ved befolkningsundersøkelser. Oslo: Statistisk sentralbyrå, 2001. www.ssb.no/emner/03/00/sa41/sa41.pdf (30.8.2011).
- 30.
International Diabetes Federation – Clinical guidelines taskforce. Chapter 8: Self-monitoring. Global guideline for type 2 diabetes. 2005.
- 31.
Kjome RLS, Granas AG, Nerhus K et al. Quality assessment of patients' self-monitoring of blood glucose in community pharmacies. Pharmacy Practice 2010; 8: 62 – 9.
- 32.
Skeie S, Thue G, Nerhus K et al. Instruments for self-monitoring of blood glucose: comparisons of testing quality achieved by patients and a technician. Clin Chem 2002; 48: 994 – 1003.
- 33.
O’Kane MJ, Bunting B, Copeland M et al. Efficacy of self monitoring of blood glucose in patients with newly diagnosed type 2 diabetes (ESMON study): randomised controlled trial. BMJ 2008; 336: 1174 – 7.