Use of manual techniques for perineal support in Norwegian maternity departments
The incidence of sphincter rupture during deliveries in Norway increased appreciably in the period 1967 – 2004, according to figures from the Medical Birth Registry (1). Risk factors for sphincter rupture, for example older birthing mothers, only offer partial explanations for this increase (1). In 2006, the Norwegian National Advisory Committee on Maternity Care therefore launched an action plan for reducing the occurrence of sphincter damage (2). One of the measures in the action plan was that more emphasis should be placed on the use of support techniques for protecting the perineum in the final stage of delivery.
The use of support techniques is controversial, partly because there is little research-based knowledge about the effectiveness of these methods (3) – (5). Some studies, from Norway among others, provide evidence that the use of manual support results in less ruptures (6) – (8), but the results of randomised, controlled studies seem to indicate that manual techniques have little or no effect (9) – (11). It is uncertain whether support techniques actually contribute to reducing sphincter rupture in number or severity and whether some manual techniques are better than others.
The modified Ritgen’s manoeuvre, also called the Finnish manoeuvre, has attracted a lot of attention in Norway in recent years. It is not known how extensively this or other methods are used. An important part of the procedure is active use of the other hand to control the speed of crowning.
The purpose of this survey was to gain more knowledge about the use of manual perineal support techniques at Norwegian maternity departments – in terms of how common it is to use such techniques, what techniques are used, and whether there have been changes in practice in recent years.
Material and method
We prepared a brief questionnaire with a total of five questions (Appendix 1). We obtained from the Directorate of Public Health a list of all the maternity departments in Norway with email addresses, which for the most part were the electronic mailboxes of each of the health enterprises.
We conducted a simple pilot test of the questionnaire by first sending it to the heads of the first ten maternity departments on the list (7 February 2011). This resulted in two minor adjustments to the questionnaire – the respondents were asked to specify which maternity department they represented, and it was stressed that we were only interested in written guidelines (Question 4). We then sent the questionnaire to the heads of all the other maternity departments in Norway (28 February 2011). We followed up with up to three reminders, including an offer that the questions could be answered orally over the phone.
Results
We received responses, one of them illegible, from 40 maternity departments. Some of the major hospitals have several maternity departments, and we received joint replies from some of these. We treat these as one department in our analysis. Thus we had answers from 39 of 47 maternity departments in Norway (83 %).
34 of 39 departments responded that most (> 90 %) of their midwives normally used manual techniques to protect the perineum during the final stage of delivery. The five remaining heads of department stated that many (71 – 90 %) of the midwives used manual techniques.
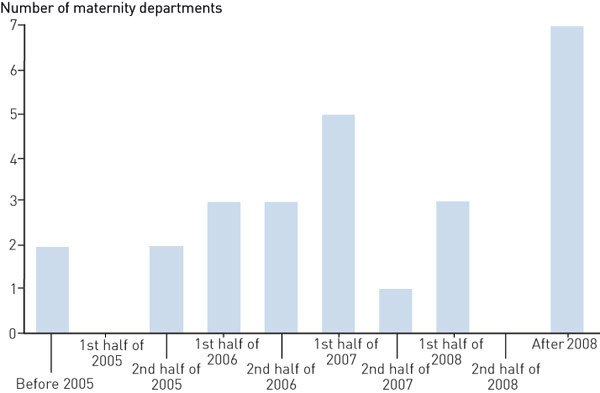
Twelve of 39 departments stated that there had been little or no change in practice. The other departments indicated that there had been some change, a major change, or a complete change in practice in recent years (Table 1). A number of the respondents had difficulty in pinpointing the time when any changes had taken place, but almost all thought it had happened in the course of the last five years (Fig. 1). Overall, almost two thirds of the departments stated that there had been a change in practice in the course of the last five years.
Table 1
Answers to questions on the use of manual perineal support during delivery at 39 Norwegian maternity departments
| How many staff in the department use manual support techniques? | |
| Proportion (%) | No. of departments (%) |
| Very few (< 10 %) | 0 |
| Few (10 – 30) | 0 |
| Some (31 – 70) | 0 |
| Many (71 – 90) | 5 (13) |
| Most of them (> 90 %) | 34 (87) |
| How much has practice changed in recent years? | |
| No. of departments (%) | |
| No change | 3 (8) |
| Little change | 9 (23) |
| Some change | 16 (41) |
| Great change | 10 (26) |
| Complete change | 1 (3) |
| What do the department guidelines say about use of manual support?¹ | |
| No. of departments (%) | |
| Avoid manual support | 0 |
| Ritgen’s manoeuvre | 3 (12) |
| Modified Ritgen’s manoeuvre | 12 (48) |
| Other manual support | 0 |
| Free choice of manual support | 10 (40) |
| [i] | |
[i] ¹ Answers from only 25 departments
Seventeen of the 39 maternity departments had written guidelines concerning the use of manual support techniques. A couple of the departments also referred to national guidelines. The use of manual techniques was recommended without exception during the final stage of delivery, but there was some variation in the type of manoeuvre recommended in the guidelines of the different departments (Table 1). Almost half recommended the modified Ritgen’s manoeuvre («the Finnish manoeuvre»). The Ritgen’s manoeuvre could also be used at some of these departments. Some departments reported only the Ritgen’s manoeuvre as the recommended method. In many departments, the choice of perineal support was left to the discretion of the individual midwife or obstetrician.
Some of the respondents answered the question concerning recommended manual techniques even though there were no written guidelines in the department, usually because there were informal recommendations concerning the use of manual support. We chose to include these answers.
Discussion
This survey shows that techniques to protect the perineum against tearing during delivery are used by the great majority of midwives at Norwegian maternity departments. This is a result of changes in practice in recent years, according to the responses from the heads of 39 of 47 departments.
We chose to prepare a very short questionnaire in the hope of getting as many answers as possible. We were very successful in this respect, since we received responses from 83 % of the maternity departments. On the other hand, the questionnaire was so short that the amount of information we received from each department was limited.
We did not carry out any formal validation of the questionnaire, but it was adjusted after pilot testing. There is a certain risk that misunderstandings may have arisen as a result of weaknesses in the questionnaire. One major weakness is that all the answers were subjective, since we asked the heads of department to give their «impression» of practice at their maternity department. We do not know whether the heads of department have a realistic impression of what is going on in the delivery rooms. A better option might have been to ask all Norwegian midwives about their use of manual techniques to protect the perineum.
At the same time as the use of support techniques at Norwegian maternity departments appears to have increased, the incidence of sphincter rupture has decreased (12). It is difficult to know whether there is a causal relationship. Our survey is not appropriate for saying anything about this.
Theoretical considerations indicate that active support results in more controlled expulsion and slower emergence of the head. This reduces the pressure on the sphincter, which in turn reduces the risk of tearing. On the other hand, it is conceivable that the risk of rupture increases, for example if the deflection of the head during emergence results in an unfavourable head diameter so that the emerging head occupies more space than if it were flexed, as it usually is (13).
Several controlled studies have been performed where active manual techniques have been compared with more passive approaches (9) – (11). The results of these studies do not provide any unambiguous answer to whether the use of support techniques affects the risk of sphincter rupture. Nor can the possibility that support techniques do more harm than good be excluded. In one of the randomised studies, the frequency of third degree ruptures was several times as high in birthing mothers where manual manoeuvres had been used than in the others (10). In this study, a comparison has been made between the Ritgen manoeuvre and a passive approach without touching of the perineum (hands poised). The results of two other relevant randomised studies we know of had conflicting results with respect to the effect on the frequency of serious ruptures, but neither of the findings was statistically significant (9, 11).
Our study indicates that there has been a widespread introduction of support techniques among midwives at Norwegian maternity departments in recent years. The big question is whether this has contributed to the decline in the number of sphincter ruptures, which has taken place concurrently. The introduction of routine use of the modified Ritgen’s manoeuvre («Finnish manoeuvre») has been evaluated at five Norwegian maternity departments, where a dramatic decline has been reported in rupture frequency when a comparison is made between the incidence before and after the introduction of the intervention (6, 7). But an observed change from one time to another is seldom sufficient to allow the effects of a measure to be estimated – there may be a number of other reasons for the observed decline in the incidence of ruptures during this period. The strong focus on sphincter ruptures may have led to a number of changes that may have affected the frequency of ruptures. Without a control group, it is very difficult to assess how effective a measure has been. Simple before-and-after comparisons can be very misleading (14).
The results of our questionnaire survey indicate that it is no longer possible to perform a comparative study of a hands-on versus a more passive approach in Norway, since support techniques have now become standard procedure at the great majority of Norwegian maternity departments. This is positive for the women giving birth – provided that the use of these techniques reduces the risk of sphincter rupture – but negative with respect to the possibility of ascertaining whether it actually does so. A few years ago, the maternity departments could have been randomised to introduce routine use of hands-on or otherwise, but it is difficult to imagine today’s midwives taking part in an experiment where half of the maternity departments are randomised to re-introduce old methods.
In the absence of a robust evaluation, a thorough investigation should be made of the relationships between changes in the incidence of ruptures in recent years and measures that were introduced during the same period – using interrupted time series analysis. Such a study could contribute to substantiating any causal relationships.
We would like to thank the heads of department who took the time to answer the questionnaire, Ingeborg Strømseng Sjetne for help in formulating the questionnaire and Kjetil Olsen, who computerised the answers. The authors are engaged in a project, the aim of which is to estimate the effects of measures to prevent sphincter rupture that have been introduced in Norway in the last few years.
Tabell
Main points |
|
- 2.
Nasjonalt råd for fødselsomsorg. Sfinkterskader ved fødsel bør reduseres i Norge. Nasjonal handlingsplan. Oslo: Sosial- og helsedirektoratet, 2006.
- 5.
Lukasse M, Grimsrud E. Varig reduksjon av sfinkterskader – hvordan skal vi få det til? Tidsskrift for jordmødre 2009; nr. 5.
- 10.
Mayerhofer K, Bodner-Adler B, Bodner K et al. Traditional care of the perineum during birth. A prospective, randomized, multicenter study of 1,076 women. J Reprod Med 2002; 47: 477 – 82. [PubMed]
- 12.
Sterk økning i obstetriske sfinkterskader. Fødselsnytt 2010; nr. 2: 3. www.fhi.no/dav/17e444f118.pdf (22.9.2011).