Norway has scattered settlement and a harsh climate with decentralised and differentiated maternity care. A total of 61 634 children were born here in 2008 – 89.6 % in gynaecology/obstetric departments, 9.6 % at low-risk units (fødestuer) or maternity departments with < 500 births/year, 0.7 % unplanned out-of-hospital and 0.1 % planned at home (1).
The quality requirements for maternity care entail centralisation (2, 3). This may have increased the need for an accompaniment service. In Report no. 12 (2008 – 2009) to the Norwegian Storting (parliament): En gledelig begivenhet [A joyous occasion], it was decided that with effect from 1 January 2010, the regional health authorities were to be responsible for an accompaniment service for pregnant women, with a transitional period of 1 – 2 years (2). The service used to be the responsibility of the municipal health service. In the guidelines Et trygt fødetilbud [A safe maternity option] the government’s limit for providing a qualified accompaniment service is defined as a travel period of 90 minutes from home address to the maternity institution (3).
Several levels of healthcare are affected when a pregnant woman reports a need for out-of-hospital birthing help. The Municipal Health Service Act lays down in Section 2- 1: «Everyone has the right to necessary medical aid in his municipality of residence or in the municipality where he is staying» (4). A pregnant woman who goes into labour has an automatic right to medical assistance in the municipality in which she is there and then.
Prehospital maternity care can be defined as the medical service that is offered from the time a pregnant/birthing woman reports a need for transportation, or maternity assistance, until she receives assistance at a maternity institution. The term «prehospital maternity care» includes assessing whether the woman is in active labour, assessing the need for accompaniment to a maternity institution and determining the mode of transport, degree of urgency and maternity assistance to women who have unplanned deliveries at home or during transportation.
In 1991, Daltveit et al. published an article on outcomes of deliveries during transportation in the period 1967 – 1988, based on data from the Medical Birth Registry (5). The survey revealed a perinatal mortality of 156 per 1 000 children born during transportation in the period 1967 – 71, i.e. mortality was seven times higher than for children who were not born during transportation. The perinatal mortality associated with deaths during transportation dropped sharply in the 1970s, and in the period 1986 – 1988 the figures were 16 and 13 per 1 000 for children born during transportation and not born during transportation, respectively. The authors concluded that it was the healthy, multiparous women who gave birth to healthy children and lived in rural municipalities who paid the price for the centralisation. The children who were born during transportation did not have a higher risk of perinatal mortality, and centralisation of maternity institutions did not have any demonstrable negative effect on perinatal outcomes.
A study of helicopter transportation of sick neonates in Sør-Trøndelag county in the period 1988 – 2001 showed the importance of the air ambulance service arriving early in order to be able to provide treatment. The average response time was 42 minutes, the average gestation period 38 weeks. Almost 5 % of the children had a birth weight of < 1 000 g and/or < 28 weeks’ gestation, 12 % died within one year (6).
In this study we have surveyed the organisation of and obtained data on prehospital maternity care in Norway in 2008. We believe that our survey represents new knowledge that may be useful when the new requirements regarding prehospital maternity care and accompaniment are implemented.
Material and method
We applied to the Medical Birth Registry and gained access to information on unplanned births outside maternity institutions in Norway in 2008. These are placed in four categories: unplanned home, during transportation, elsewhere (out-of-hospital, unspecified, e.g. doctor’s office or birth centre) and unknown.
The data from the Medical Birth Registry are anonymised, classified according to mother’s county of residence and the place where the child was born/«Place of birth». We have obtained the following clinical data about unplanned out-of-hospital births: singleton/multiple pregnancies, presentation, Apgar score and birth weight. For the mothers, we have obtained data on parity, gestation period and complications such as haemorrhage/tears.
The study also included a questionnaire sent to Norway’s 53 maternity institutions, the municipal midwifery service in Norway’s 431 municipalities and 19 EMDCs, with the exception of Svalbard. The maternity institutions and municipal midwives were asked whether they had a formally organised accompaniment service whereby they turned out when a need for prehospital maternity help was reported, and about how they met the need for accompaniment if the service was not formally organised (Appendix 1, Appendix 2). They were also asked what sort of equipment and aids they had with them if they turned out, and who determined the degree of urgency.
The EMDCs were asked to provide an overview of any agreements/current practice concerning support by a municipal or hospital midwife in the event of prehospital births, turnout time, criteria for choice of means of transport of the woman in labour and neonate, the midwife’s skill in determining the degree of urgency in line with the Norwegian index for emergency medical assistance, and the paramedic’s obstetrics skills (Appendix 3).
The 503 informants were all asked to report the number of turnouts or estimated figures for 2008. The survey was carried out in the period autumn 2009 – spring 2010, with a written reminder to all informants and a verbal reminder to all maternity institutions that had not responded to the written reminder.
Results
The response to the questionnaire was 100 % for maternity institutions (n = 53), 73 % for municipal midwives (n = 313) and 84 % for EMDCs (n = 16).
Births
Table 1 shows a breakdown by county of unplanned out-of-hospital births in terms of number of births and the ratio of prehospital births to the total. There is no information as to how many of these births during transportation concerned transfers from a maternity unit to a higher level care unit. The results for the 429 unplanned prehospital deliveries (430 children) in 2008 and for their mothers are given in Figure 1. Of the in all 430 children, 26 (6 %) were born before the 37th week. Five of them had an Apgar score of < 7 after five minutes; one was a breech delivery at home and one was in «other lie» during transportation. One full-term baby had an Apgar score of < 7 after five minutes. This baby had a birth weight of > 4 000 g and a breech delivery at home. The material contained two reports of deaths 0 – 24 hours after birth – twins with birth weights of 400 – 600 g after a gestation period of 22 weeks and four days.
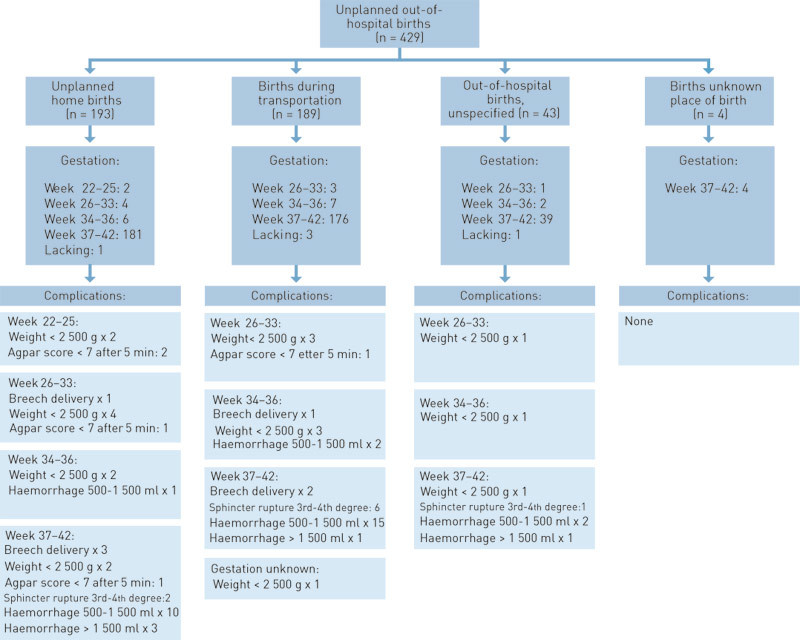
Table 1
Unplanned out-of-hospital births in 2008 by county. Number of babies born
| County | Total births | Home | Transportation | Other, unspecified | Unknown | Total | Percentage of total born ( %) |
| Østfold | 3 037 | 8 | 5 | 4 | 0 | 17 | 0.56 |
| Akershus | 6 299 | 19 | 9 | 4 | 2 | 34 | 0.54 |
| Oslo | 10 264 | 21 | 5 | 4 | 2 | 32 | 0.31 |
| Hedmark | 1 864 | 9 | 4 | 0 | 0 | 13 | 0.70 |
| Oppland | 1 927 | 4 | 10 | 3 | 0 | 17 | 0.88 |
| Buskerud | 3 046 | 13 | 5 | 2 | 0 | 20 | 0.66 |
| Vestfold | 2 535 | 4 | 6 | 0 | 0 | 10 | 0.39 |
| Telemark | 1 752 | 6 | 7 | 2 | 0 | 15 | 0.86 |
| Aust-Agder | 1 245 | 4 | 4 | 1 | 0 | 9 | 0.72 |
| Vest-Agder | 2 275 | 9 | 4 | 1 | 0 | 14 | 0.62 |
| Rogaland | 6 154 | 16 | 21 | 1 | 0 | 38 | 0.62 |
| Hordaland | 6 331 | 27 | 32 | 3 | 0 | 62 | 0.98 |
| Sogn og Fjordane | 1 260 | 3 | 8 | 4 | 0 | 15 | 1.19 |
| Møre og Romsdal | 2 829 | 14 | 14 | 1 | 0 | 29 | 1.03 |
| Sør-Trøndelag | 3 839 | 14 | 19 | 3 | 0 | 36 | 0.94 |
| Nord-Trøndelag | 1 496 | 6 | 13 | 0 | 0 | 19 | 1.27 |
| Nordland | 2 578 | 9 | 9 | 2 | 0 | 20 | 0.78 |
| Troms | 1 970 | 8 | 8 | 2 | 0 | 18 | 0.91 |
| Finnmark | 879 | 0 | 6 | 6 | 0 | 12 | 1.37 |
| Total | 61 580 | 194 | 189 | 43 | 4 | 430 | 0.70 |
In Oslo Municipality, where very few women need to travel more than an hour to a maternity institution, there were 32 unplanned out-of-hospital births, and in Akershus County there were 34. There were 44 unplanned prehospital births in the catchment area of the Bergen Health Trust, and 28 in that of the Stavanger Health Trust (1).
Maternity institutions
Five (9 %) of Norway’s 53 maternity institutions have a formal organised accompaniment service agreement (Fig. 2). Three of these are birth centres, in Finnmark, Nordland and Oppland counties, and two maternity departments, in Sogn og Fjordane and Hordaland counties. These maternity institutions state that they have continuous preparedness and that a midwife or if relevant A&E doctor provides the accompaniment service.
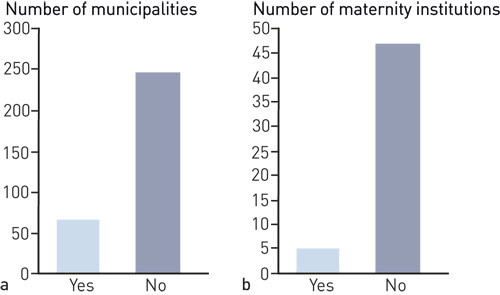
Of the 48 institutions without a formal agreement, 15 improvise in every case where there is a report of a woman in labour with a need for transportation. The improvised accompaniment service is evenly distributed across all types of maternity institutions and counties – two birth centres and one maternity department in Troms, one birth centre and one maternity department in Nordland, one maternity department in Oppland, one birth centre and two maternity departments in Hedmark, one maternity department in Sogn og Fjordane, one gynaecology and obstetrics department in Rogaland, one maternity department and a gynaecology and obstetrics department in Vest-Agder, a gynaecology and obstetrics department in Vestfold and one in Østfold.
There are 33 maternity institutions that report that they do not have an accompaniment service. Their reasons for this are partly that the municipalities meet this need (22 maternity institutions); five believe that it is not the institution’s responsibility, three maintain that there is no need for an accompaniment service, one says that there are not enough midwives at their institution. One institution has a need, but not budgetary cover, and one maintains that the running of the department has first priority. Midwives at maternity institutions state that they have attended 175 unplanned out-of-hospital births (41 % of all unplanned out-of-hospital births).
The Norwegian Index of Medical Emergencies (the Index) is a relatively unknown tool for midwives. Only nine (17 %) of the maternity institutions were familiar with this index and the concepts red (acute), yellow (urgent) and green (normal) trip which form the basis for all the EMDCs’ decisions concerning response, degree of urgency and means of transport.
Municipalities
Of the 313 municipalities that responded to the survey, 247 (79 %) reported that they did not have a formalised emergency and accompaniment service (Fig. 2). In 64 municipalities, patients have to travel 90 minutes or more to the nearest maternity institution. There was a travel time of less than 60 minutes to a maternity institution in 68 (46 %) of a total of 148 unplanned prehospital births with a municipal midwife present (Fig. 3). Of the 64 municipalities with travel time of ≥ 90 minutes, 31 have a formalised accompaniment service, and 26 describe this as a 24-hour service. Among other things, we asked who is accompanied by a midwife to a maternity institution, with three possible responses. The response of 19 of the 114 municipalities (36 %) that answered the question was that all patients are accompanied. The response of 77 was that they accompany as needed, and 18 that they had other criteria.
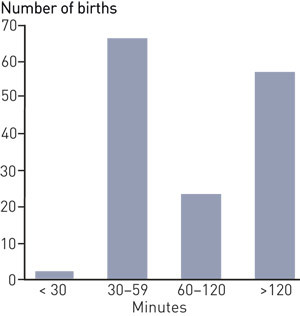
Half of the estimated 1 800 pregnant women who were examined before transportation without subsequently being accompanied by a midwife to a maternity institution were at least an hour away from the nearest birth centre/maternity department. In the 313 municipalities that answered the questionnaire, 55 municipal midwives answered that they had had to refuse an expressed need for accompaniment, largely because of lack of emergency preparedness and conflicts with other urgent matters. In 2008, municipal midwives assisted with 23 unplanned home births where the home was 1 – 2 hours away from the nearest maternity institution, and in the case of 57 births the home was more than two hours from a maternity institution.
Some areas have a well organised service with intermunicipal cooperation and a 24-hour support service. Examples of this are to be found in the northern Gudbrandsdalen valley, where the municipalities Dovre, Lesja, Lom, Sel, Skjåk and Vågå have a smoothly functioning intermunicipal midwife service for cases where the travel time to the nearest maternity institution ranges from one and a half to four hours. In northern Troms, the municipalities of Kvænangen, Kåfjord, Nordreisa and Skjervøy cooperate on the support service centred around Sonjatun birth centre in Nordreisa municipality. The travel distance from the individual municipality to Sonjaturn birth centre varies from half an hour to one and a half hours. The trip to the University Hospital of North Norway takes from half an hour to four hours. Eight municipalities with a formal agreement describe a midwife availability scheme linked to the patients' due dates. The municipal midwife is on call 3 – 7 days before the woman is due. This scheme does not make allowances for any premature, higher risk births.
The emergency medical dispatch centres (EMCDs)
The EMCDs register all turnouts, but 15 of 16 stated that it is a complex matter to extract suitable figures in order to give a precise response to our questions about volume. As a result, the responses include estimated figures. One of the EMCDs stated that they have an established procedure for when a municipal midwife is involved in a turnout. Another centre has written procedures on indications for turnout with a midwife from a maternity institution, with a requirement of five minutes’ response time. Half of the EMCDs confirmed that midwife’s assessment of urgency is in line with the guidelines in the Norwegian index for emergency medical assistance (Box 1) (7).
The Norwegian index for emergency medical assistance (7) has outlined criteria, advice, response, supplementary questions, advice to persons phoning in and tips to health personnel about complications graded as red response ACUTE, yellow response URGENT and green response NORMAL.
-
Examples:
-
Red response: The foster is not in a normal position and the waters have broken
-
Yellow response: after 37th week of pregnancy – primapara: less than 2 min between strong, regular contractions
-
Green response: Multipara with more than 5 min between contractions
-
Six of 16 EMCDs considered that their ambulance personnel have the necessary expertise to assist in deliveries during transportation. All the 16 EMCDs that responded to the questionnaire confirmed that there is an organised transport system for sick and premature babies.
Discussion
Our survey has shown acceptable results for unplanned out-of-hospital births in 2008. There were no deaths in the case of births after viable gestation periods. Of the unplanned out-of-hospital births, 93 % took place after a gestation period of ≥ 37 weeks. Only one of these babies had an Apgar score of < 7 after five minutes. There were two births after gestations of 22 – 25 weeks; eight took place in Weeks 26 – 33, and 15 in Weeks 34 – 36. There were four breech deliveries at home, one in which the baby had a birth weight of < 1 500 g and two with Apgar scores of < 7 after five minutes, and three breech deliveries during transportation where all the babies had a birth weight of > 2500 g and all had an Apgar score of > 7 after five minutes. Nine women suffered a sphincter tear.
Births during transportation are never to be recommended, but many of them are rapid and the results good. In the event of a short gestation or where there is a breech presentation or twins, birth outside an institution entails an additional risk. Moreover, the woman in labour, family members and medical personnel who are not specialists in maternity assistance and who experience such a birth often find them unsafe and frightening and maintain that each of these births is one too many. In areas with a harsh climate or particularly great distances, many people appear to find it advisable to travel to the assigned place of birth well before the birth.
We have found that there are various ways of dealing with emergencies, and the organisation is unclear and varies very considerably in Norway. The service is provided primarily by midwives and a good ambulance service (road, boat, helicopter and plane).
We believe a zero vision for unplanned prehospital births is unrealistic. However, in our view, the number of these out-of-hospital births can be reduced through systematic measures. Women in labour who are at more risk of complications should give birth at maternity institutions with the necessary expertise. It is often crucial that preterm births take place in a hospital with a neonatal department. The great majority of pregnant women who are at risk of preterm births are transported to the hospital with the baby in utero.
Only five maternity institutions (9 %) have a formal agreement for an accompaniment service. The maternity institutions gave many and mixed reasons for not having agreements for an accompaniment service in 2008. Of the 53 institutions, 33 do not participate in an accompaniment service. Nevertheless, 45 of the maternity institutions have a special delivery equipment bag ready for use in the event of a birth during transportation.
In our study, the maternity institutions estimate that midwives have turned out and attended 175 prehospital births. The municipal midwives have reported their presence at 148 unplanned out-of-hospital births. This puts the presence of midwives at 323 of 429 unplanned prehospital births (75 %). This may be part of the reason why the unplanned out-of-hospital births had such good results nonetheless.
It has been difficult to obtain reliable information on unplanned out-of-hospital births, accompaniment and ambulance transportation of women in labour. Since 2009, all Norwegian maternity institutions are required as a trial arrangement under the Medical Births Registry to register all planned home births with transfer to a maternity institution, all transfers from birth centres to hospital and all births during transportation. We believe such a scheme should be permanent, in order to provide reliable data on such births.
Most women in labour appear to travel to the maternity institution on their own, without organised transport through EMDCs. Others contact a midwife or GP at their place of residence for an assessment before deciding whether to travel. This assessment provides a necessary clarification of whether the woman actually is in labour and accordingly should travel to the planned birth place, an assessment of the need for and means of transport, degree of urgency and need for qualified accompaniment.
Six of 16 EMCDs considered that their ambulance personnel have the necessary expertise to assist in deliveries during transportation. At first glance, we find this response somewhat surprising, in light of our experience with ambulance personnel’s limited knowledge and experience of providing birthing assistance. One possible explanation may be that we did not define «necessary expertise» in the questionnaire, and that this can be interpreted in various ways. The basic training for ambulance personnel provides an introduction to the normal course of a delivery and in the assistant function, but they get little (or no) practical experience during their paramedic training or later in their jobs. A report about the prehospital services establishes that paramedic training does not provide the necessary expertise in observation, assessment and treatment of women in labour and neonates (8). The report concludes, paradoxically enough, that where there is no established accompaniment service, the health authorities must compensate for this with special training for ambulance personnel.
The EMDCs confirm that there is an organised transport scheme in all regions for sick and premature babies. As a result of the Storting decision, the regional health authorities assumed responsibility for the accompaniment service from 1 January 2010 (2). The guidelines Et trygt fødetilbud [A safe maternity service] retain the limit of one and a half hours for a formalised accompaniment service for women in labour (3). We have not found documentation for why the limit was set at one and a half hours. Figures from municipal midwives document that in almost half of the unplanned deliveries they have been involved in, the travel time to the maternity institution was less than an hour. Distance is just one of a number of reasons for 430 unplanned out-of-hospital births. Other possible explanations are precipitated labour/delivery, late departure for the maternity unit despite regular labour pains for a period, language problems that may give rise to misunderstandings concerning the need for hospitalisation or lack of systematic guidance.
All the regional health authorities were instructed to make a plan for pregnancy, birthing and maternity care by the end of 2010 (2). The Western Norway Regional Health Authority’s regional plan concludes that municipalities with at least an hour and a half’s travel to a maternity institution must establish an agreement on on-call duty and an accompaniment service. The plan launches a proposal that the municipal A&E service should be responsible for emergency preparedness in municipalities with low birth rates (9). The North Norway Regional Health Authority stresses that even though there are few births during transportation in the region and that this must be taken into account in determining the resources used for accompaniment service, it is important that pregnant women feel looked after and safe as the birth approaches (10). The South-East Regional Health Authority states in its draft regional plan that the health enterprises should have responsibility for emergency preparedness for births during transportation and that affected health enterprises should draw up agreements for an accompaniment service in collaboration with the municipalities (11). In its planning work, the Central Norway Regional Health Authority has estimated that establishing an accompaniment service in municipalities whose inhabitants have to travel for more than one and a half hours to the nearest maternity institution will cost over NOK 7 million annually (12).
Our view is that emergency preparedness agreements for an accompaniment service based on A&E doctors is a systematised ad hoc solution. We believe that neither women in labour nor A&E doctors will be satisfied with such agreements, because most general practitioners have little obstetrics experience. Midwives are specialists in assisting at births, and the best qualified when it comes to determining how far labour has progressed and whether there is a need for accompaniment. A&E doctors and paramedics are qualified to assist a midwife and must be prepared in emergencies to provide maternity assistance in the absence of a midwife. The proposed requirements regarding an accompaniment service in Storting Report no. 12 will undoubtedly increase the costs of an accompaniment service. We are of the opinion that a discussion is needed of whether it is right to guarantee a qualified midwife service, including qualified accompaniment, according to need throughout Norway. An intermunicipal midwife service is probably the only possible means of providing reasonable coverage.
The regional health authorities have extensive obligations in this respect, and the work should have been started long ago.
Conclusion
Prehospital maternity care in Norway is organised in very disparate ways and formalised to only a limited extent. Responsibility for the accompaniment service and necessary emergency preparedness for pregnant women and women in labour was transferred to the regional health authorities with effect from 1 January 2010. Thus the regional health authorities have the primary responsibility for organisation and arrangements. Twenty-four hour on-call preparedness and an accompaniment service with qualified personnel shall be established when the maternity unit is more than one and a half hours away. In 2008, 79 % of Norwegian municipalities lacked a formalised accompaniment service. There was a midwife in attendance at 75 % of unplanned out-of-hospital births. It is important that the interface between a turnout service from the maternity institution and the municipal accompaniment service is optimised. It is vital that the regional health authorities make agreements with the municipalities and thereby ensure optimal utilisation of local resources, primarily municipal midwives, and thereby a good accompaniment service.
We should like to thank informants who answered questions about prehospital maternity care. Thanks also to Bo Conneryd for data processing and to the Medical Birth Registry for data from 2008. The Western Norway Regional Health Authority’s Regional Centre for Emergency Medical Research and Development, the Lærdal Foundation for Acute Medicine, the Norwegian Association of Midwives and Stavanger University Hospital have provided financial support for the study.
- 1.
Årsrapport 2008. Medisinsk fødselsregister. http://mfr-nesstar.uib.no/mfr/ (20.2.2011).
- 2.
St.meld. nr. 12 (2008 – 2009). En gledelig begivenhet.
- 3.
Et trygt fødetilbud. Helsedirektoratet 2010. IS-1877. www.helsedirektoratet.no/publikasjoner/veiledere/t_trygt_f_detilbud__kvalitetskrav_til_f_dselsomsorgen_780084 (20.2.2011).
- 4.
Lov om helsetjenesten i kommunene. Helse- og omsorgsdepartementet 1984. http://www.lovdata.no/all/hl-19821119-066.html#2-1 (4.3.2011).
- 5.
Daltveit AK, Irgens LM, Vollset SE. Risikoforhold ved transportfødsler i Norge 1967 – 88. Tidsskr Nor Lægeforen 1991; 111: 1217 – 21. [PubMed]
- 7.
Norsk indeks for medisinsk nødhjelp. Lærdal Medical AS 2009. Oslo: Den norske legeforening, 2009.
- 8.
En helhetlig gjennomgang av de prehospitale tjenestene med hovedvekt på AMK-sentralene og ambulansetjenesten. Rapport fra arbeidsgruppe nedsatt av Helse- og omsorgsdepartementet. Mars 2009. http://earlywarner.no/filer/rapport%20om%20prehospitale%20tjenester.pdf (20.2.2011).
- 9.
Regional plan for svangerskaps-, fødsels- og barselomsorga i Helse Vest. 2010. http://www.helse-vest.no/aktuelt/rapporter/Documents/Regionale%20rapportar/Regional%20rapport%20Regional%20plan%20svangerskap-fodsel-barselomsorg%20nov2010.pdf (20.2.2011).
- 10.
Regional plan for en helhetlig svangerskaps-, fødsels- og barselomsorg i Helse Nord. 2010. www.helse-nord.no/getfile.php/RHF/Rapporter/Regional_plan_for_svangerskap_fodsel_og_barsel_Helse_Nord.pdf (20.2.2011).
- 11.
Regional plan for svangerskaps-, fødsels- og barselomsorg i Helse Sør-Øst 2011 – 2014. Sak 072 – 2010. Hamar: Helse Sør-Øst, 2010.
- 12.
Helse Midt-Norge RHF. Styresak nr. 88/10: Regional plan for svangerskaps-, fødsels- og barselsomsorgen 2011–2014. https://ekstranett.helse-midt.no/1001/Sakspapirer/sak%2088-10%20Regional%20plan%20for%20svangerskaps,%20f%C3%B8dsels%20og%20barselomsorgen%202011-2014.pdf (20.2.2011).