Electroconvulsive therapy (ECT) normally has a rapid and beneficial effect and few acute side effects (1).
Moderate to serious depression often recurs. In a study on elderly patients who had been successfully treated with antidepressants for recurrent depression, the relapse rate in the course of three years of aftercare was 90 % in those who received a placebo, 64 % in those who received interpersonal psychotherapy plus a placebo, 43 % in those who were given nortriptyline and 20 % in those who received nortriptyline plus interpersonal psychotherapy (2).
In studies in recent decades, high relapse rates have also been found after electroconvulsive therapy. Sackeim and his colleagues found rates of 84 % with a placebo, 60 % with nortriptyline alone and 39 % with nortriptyline plus lithium within six months (3).
The purpose of this study was to investigate how large a percentage experienced a relapse after ECT treatment at Dikemark Hospital, how much time elapsed before the relapse, and what prophylactic steps were taken to prevent it.
Material and method
The study is based on a review of the ECT records and case notes of all patients who received electroconvulsive therapy in the period 1960 – 1995 at three psychiatric departments at Dikemark Hospital. 141 persons received a total of 241 series and 1 960 individual treatments. 124 of 141 patients (88 %) had an affective disorder as their primary diagnosis. Medicinal treatment had been tried for most of the patients before they received electroconvulsive therapy, and 52 (37 %) had received ECT treatment previously. This means that what is called «the first ECT series» in this article is not necessarily the first ECT treatment the patient received, but the first treatment the patient received at Dikemark Hospital. The ECT procedure, materials, efficacy and side effects have been described previously (1, 4).
Doctors have monitored discharged patients receiving aftercare since before 1960, and the rule was that those who experienced a relapse were readmitted to the same department at the hospital.
The observation period is defined as the time since completing the first ECT series at Dikemark up to and including 31 December 1995. A review of the material showed that five persons who received electroconvulsive therapy in the period 1960 – 1995 had had their first ECT series at the hospital before 1960. These five series have also been included in the material.
Relapse was defined as a recorded, definite recurrence of depressive symptoms, i.e. rehospitalisation or an evident decline in social functioning, a need to change antidepressant medication or administration of a further ECT series, in patients who had achieved improvement or remission within four weeks of an ECT treatment series.
Improvement was classified as follows:
Much improved (remission): regaining of premorbid functional level with full remission of symptoms, which led to the patient being discharged from the hospital within four weeks.
Improved: improvement of symptoms and functional level, but with residual symptoms as a result of which the patient could not be discharged from the hospital within the first four weeks.
Relapse figures are presented for the total material, for first and subsequent series and according to variables with assumed clinical relevance (first series): gender, age, diagnosis, indication (delusions/other), duration of index depression and hospitalisation, number of treatments in first ECT series, degree of improvement, how rapidly the improvement manifested itself, use of medication before electroconvulsive therapy and of medicinal prophylaxis subsequently.
The practice with regard to prophylactic medicinal treatment during the period was to start the patient on an antidepressant or lithium immediately after the ECT series. If the patient was already on an antidepressant or lithium, the general rule was that it was temporarily terminated, whereas patients often continued with medicines for somatic disorders and antipsychotics during the series.
Ethics
The study was approved by the Data Protection Officer at Oslo University Hospital.
Results
Relapse after initial series (n = 141)
The median observation period was nine years (spread: 3 months – 44 years). 86 of 120 (72 %) suffered a relapse, 38 (32 %) during the first two months and 56 (47 %) within the first six months. Eight persons (7 %) suffered a relapse in the next six months (Fig. 1). The average time before relapse was 13 months, the median time three months.
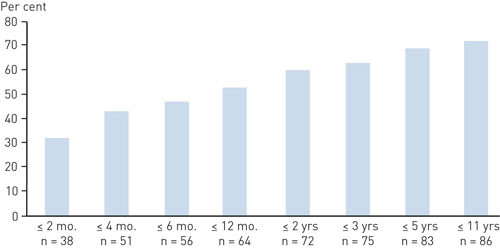
Sub-groups
None of the seven patients who recovered from their initial depressive episode suffered a relapse in the course of an average observation period of four years (median 5 years), compared with 56 of 71 (79 %) with recurrent depression (Table 1).
Table 1
Number of patients suffering relapses after the first ECT series at Dikemark Hospital in the period 1960 – 1995 grouped by variables with assumed clinical relevance (n = 120 of 141)¹. Median and average time to relapse is given for sub-groups with more than four patients
| Number of patients |
Number improved |
Number with relapses |
Time to relapse (months) |
||||
| ≤ 2 mo. |
≤ 6 mo. |
Total |
Average |
Median |
|||
| Gender |
|||||||
| Women |
104 |
87 |
29 |
44 |
67 |
14 |
3 |
| Men |
37 |
33 |
9 |
12 |
19 |
9 |
4 |
| Age (years) |
|||||||
| 20 – 39 |
2 |
1 |
1 |
1 |
1 |
||
| 40 –49 |
8 |
6 |
0 |
1 |
4 |
32 |
30 |
| 50 –59 |
17 |
15 |
7 |
9 |
12 |
19 |
2 |
| 60 –69 |
47 |
39 |
12 |
18 |
28 |
13 |
4 |
| 70 –79 |
49 |
42 |
15 |
18 |
31 |
11 |
3 |
| 80 –89 |
18 |
17 |
3 |
9 |
10 |
3 |
3 |
| Diagnosis |
|||||||
| First-time depression |
10 |
7 |
0 |
0 |
0 |
||
| Recurrent depression |
81 |
71 |
24 |
34 |
56 |
15 |
3 |
| Bipolar depression |
31 |
28 |
9 |
16 |
21 |
10 |
3 |
| Organic depression² |
9 |
5 |
2 |
2 |
2 |
||
| Schizophrenia with depression |
5 |
5 |
2 |
3 |
4 |
12 |
4 |
| Schizoaffective disorder with depression |
3 |
3 |
1 |
1 |
2 |
||
| Dysthymia |
2 |
1 |
0 |
0 |
1 |
||
| Total |
141 |
120 |
38 (32 %) |
56 (47 %) |
86 (72 %) |
13 |
3 |
| Use of medicines before ECT treatment |
|||||||
| No antidepressants |
12 |
9 |
4 |
5 |
7 |
10 |
2 |
| One class of antidepressants |
62 |
56 |
18 |
26 |
42 |
16 |
3 |
| 2 –4 classes of antidepressants |
67 |
55 |
16 |
25 |
37 |
10 |
3 |
| Degree of improvement |
|||||||
| Improved |
59 |
24 |
32 |
43 |
11 |
2 |
|
| Much improved (remission) |
61 |
14 |
24 |
43 |
13 |
4 |
|
| Duration of hospitalisation (months) |
|||||||
| ≤ 6 |
73 |
67 |
14 |
18 |
44 |
18 |
8 |
| > 6 |
68 |
53 |
24 |
38 |
42 |
6 |
2 |
| Number of ECT treatments |
|||||||
| ≤ 5 |
18 |
12 |
7 |
8 |
9 |
9 |
2 |
| 6 –9 |
72 |
65 |
21 |
30 |
48 |
12 |
4 |
| ≥ 10 |
51 |
43 |
10 |
18 |
29 |
15 |
3 |
| Indications |
|||||||
| Delusions |
61 |
55 |
16 |
22 |
42 |
18 |
4 |
| Others |
80 |
65 |
22 |
34 |
44 |
8 |
3 |
| Duration of index depressions (mo.) |
|||||||
| ≤ 6 |
73 |
63 |
17 |
27 |
44 |
16 |
4 |
| > 6 |
68 |
57 |
21 |
29 |
42 |
10 |
3 |
| Improvement speed (d) (n = 92) ³ |
|||||||
| ≤ 3 |
55 |
9 |
17 |
34 |
16 |
7 |
|
| > 3 |
37 |
14 |
18 |
25 |
12 |
2 |
|
| Use of medicines after ECT treatment |
|||||||
| No antidepressants |
30 |
21 |
9 |
14 |
16 |
9 |
2 |
| Anti-depressants alone |
33 |
31 |
11 |
15 |
25 |
15 |
3 |
| Anti-depressants + lithium and/or neuroleptic |
55 |
47 |
10 |
13 |
27 |
17 |
7 |
| Others ⁴ |
23 |
21 |
8 |
14 |
18 |
6 |
3 |
| [i] | |||||||
[i] ¹ Five persons who received ECT treatment in the period 1960 –1995 had had their first ECT series at Dikemark Hospital before 1960. These five series have been included in the material.
² Patients with primary diagnosis of organic brain disorder such as various types of senile dementia with depression
³ Data available for 92 of 120 improved
⁴ Others are lithium and neuroleptic alone and in combination
In the age group 40 – 49, the median time to relapse was 30 months. The median among those over 50 was 2 – 4 months (Table 1).
24 of 61 (39 %) of those who achieved remission and 32 of 59 (54 %) of those who responded without achieving remission suffered a relapse within six months.
Patients with a hospital stay of six months or less prior to ECT treatment had a median time to relapse of eight months, compared with two months in the case of hospital stays in excess of six months. Of patients with a hospital stay of over six months, 24 of 53 (45 %) experienced relapse within two months, while 14 of 67 (21 %) with a shorter stay suffered an equally rapid relapse.
Those with five or fewer ECT treatments had a median time to relapse of two months, while those with 6 – 9 treatments went a median of four months before suffering a relapse. Of those who showed signs of improvement within three days, the median time to relapse was seven months (Table 1).
There was no evident connection between the percentage of relapses and gender, medication prior to electroconvulsive therapy, indication or duration of index depression.
Prophylactic use of medicines after the initial series
After the first ECT series, 78 (65 %) of the 120 who improved were recorded as receiving a prophylactic antidepressant, 27 (23 %) of them in combination with a neuroleptic and seven (6 %) in combination with lithium. Thirteen (11 %) received both a neuroleptic and lithium. Three (3 %) received only lithium, 15 (13 %) received a neuroleptic alone and three a combination. 21 (18 %) did not receive medicinal prophylaxis.
81 % of those who received an antidepressant alone and 76 % of those who received no prophylaxis suffered a relapse. Three of seven (43 %) suffered a relapse when using an antidepressant and lithium in combination. Without prophylaxis, the median time to relapse was two months, whereas it was three months when an antidepressant was used and seven months when an antidepressant combined with lithium and/or a neuroleptic was used (Table 1).
Results of all ECT series (n = 241)
46 patients received a second ECT series and 24 of these a third. One received as many as ten series. Of the 87 of in all 100 follow-up series where an improvement was observed, 58 (67 %) relapses were recorded within six months. Of a total of 207 series with improvement, 114 relapses (55 %) were observed within six months (Table 2).
Table 2
Relapse in patients who were improved or much improved after the first and subsequent ECT series administered at Dikemark Hospital in the period 1960 –95 (n = 241)¹
| ECT series no. |
Series No. |
Series with improvement No. ( %) |
Relapse before 6 months No. ( %) |
Relapses total No. ( %) |
| Series 1 |
141 |
120 (85) |
56 (47) |
86 (72) |
| Series 2 –10 |
100² |
87 (87) |
58 (67) |
75 (86) |
| All series |
241² |
207 (86) |
114 (55) |
161 (78) |
| [i] | ||||
[i] ¹ Five persons who received ECT treatment in the period 1960 –1995 had had their first ECT series at Dikemark Hospital before 1960. These five series have been included in the material.
² Response to treatment could not be assessed in one patient
Discussion
After an initial improvement following electroconvulsive therapy, the study shows that there is a high degree of relapse, mostly during the first six months. This is in line with the results of other studies (3). In the case of three patients, a relapse did not occur until after 5 – 11 years, which influenced the average time to relapse.
The findings support the assumption that the sub-diagnosis of affective disorder is positively associated with the risk of relapse. In the small group with first-time depression, seven of ten improved after electroconvulsive therapy and none relapsed, whereas relapse was frequent in cases of recurrent depression and bipolar depression. It appears that age may be of significance when it comes to time to relapse (Table 1). Only one of six 40-year-olds suffered a relapse in the course of the first six months, even though none of them had first-time depression (data not shown).
The patient group had a high degree of medication resistance, which may have contributed to relapses. Almost half had used two or more classes of antidepressants before the ECT series, but this does not appear to have influenced the relapse rate or the median time to relapse. Sackeim et al. found a higher relapse rate among those who had received appropriate pre-ECT pharmacotherapy than among those who had not received it – 64 % compared with 32 % (5).
The high relapse occurrence may be related to the fact that 18 % of the patients who improved did not receive prophylactic medicines after the first ECT series, and that most of those who received secondary prophylaxis received antidepressants that had already proved ineffective against depression before the ECT treatment (data not shown). Those who received a combination of an antidepressant and lithium and/or a neuroleptic exhibited a lower relapse rate and longer median time to relapse than those who received an antidepressant alone.
The relapse percentage for the 100 follow-up ECT series that 46 patients received was somewhat higher. The explanation may be that 93 of these series concerned recurrent or bipolar depression (data not shown).
What can be done to maintain remission over time? In a recent overview it is found that psychotherapy alone or in combination with antidepressants or electroconvulsive therapy may have a positive supplementary effect, but that this is not a robust strategy for preventing relapse (6).
Many clinics now administer maintenance ECT to extend the remission period and reduce the need for rehospitalisation when medicinal treatment has failed to prevent relapse (7). In a controlled retrospective study, it was found after two years that 93 % had suffered no serious relapse with maintenance ECT in addition to a combination of medicines, compared with 52 % without maintenance ECT. After five years, the figures were 73 % and 18 % (8).
Lisanby et al. propose that prophylactic antidepressant medicinal treatment be started already during the ECT series, and that four ECT treatments be given during the first month after the series, since the risk of relapse is greatest then (9). Thereafter patients should be examined weekly to determine the treatment frequency for the next six months. This approach should be tested with a randomised, controlled trial.
Strengths and weaknesses
Strengths and weaknesses have been discussed previously (1) and are summed up briefly here. The material consists of a selected patient group and is based on retrospectively obtained case notes. Although patients were as a rule monitored during aftercare and rehospitalised in the same department on relapse, it is not certain that all relapses were recorded. The information in the patients’ records was not good enough to enable assessment of whether antidepressants were administered in an optimal dose over an appropriate period of time, or to establish the degree of compliance of this treatment. Lack of compliance may be part of the explanation for the high relapse frequency.
Multivariable analyses were not performed or tested for possible confounding factors. The sub-groups in the material were small, which makes comparisons uncertain. The strength of the study is its naturalistic form and the fact that it spans a long period of time.
Conclusion
Recurrence of serious depression after successful electroconvulsive therapy is usual, and today’s practice for preventing relapse is not good enough. This invites prospective studies of secondary prevention in depressive patients who receive ECT treatment.
I would like to thank Stein Opjordsmoen Ilner at Oslo University Hospital for sound advice. Table 1 is only available in the electronic document published on Tidsskriftet's website.
Tabell
| Main points |
|
- 1.
Moksnes KM, Opjordsmoen S. Elektrokonvulsiv terapi – virkning og bivirkninger. Tidsskr Nor Legeforen 2010; 130: 2460-4.
- 4.
Moksnes KM, Vatnaland T, Eri B et al. Elektrokonvulsiv terapi i Ullevål sektor i Oslo 1988–2002. Tidsskr Nor Lægeforen 2006; 126: 1750–3.
- 6.
McClintock SM, Brandon AR, Husain MM et al. A systematic review of the combined use of electroconvulsive therapy and psychotherapy for depression. J ECT 2011; 27: 236 – 43. [PubMed]
- 7.
Odeberg H, Rodriguez-Silva B, Salander P et al. Individualized continuation electroconvulsive therapy and medication as a bridge to relapse prevention after an index course of electroconvulsive therapy in severe mood disorders: a naturalistic 3-year cohort study. J ECT 2008; 24: 183 – 90. [PubMed] [CrossRef]
- 9.
Lisanby SH, Sampson S, Husain MM et al. Toward individualized post-electroconvulsive therapy care: piloting the Symptom-Titrated, Algorithm-Based Longitudinal ECT (STABLE) intervention. J ECT 2008; 24: 179 – 82. [PubMed]