Norwegian doctors work longer weekly hours than most other professions (1, 2), but are also on the whole quite satisfied with their jobs (3). A comparison of Norwegian and German hospital doctors showed that the Norwegian doctors were more satisfied with their working hours than their German counterparts to a statistically significant extent (4). Hospital doctors tend to have regulated working hours which can easily be measured objectively, and a number of studies have used the working hours and shift schedules of hospital doctors as explanatory variables, with regard to patient safety (5) as well as in terms of the doctors′ own health and well-being (6, 7).
In contrast to the hospital doctors, the GPs tend to regulate their own working hours, and there is no information available with regard to their weekly working hours and schedules other than what the GPs themselves have reported. The introduction of the list-patient system in 2001 entailed a considerable standardization of the working conditions of the GPs, in which the main variable is the number of patients on their lists. We know exactly how many list patients the GP is expected to serve, but we know little about the amount of time the individual GP spends with his or her patients. In a previous study we have shown that the list-patient scheme has not had any impact on the job satisfaction of the GPs, which at the outset is significantly higher than that of the hospital doctors (8). The question remains, however, of whether the introduction of the list-patient scheme has had any effect on the weekly working hours of the GPs. Previous studies indicate varying answers. Grytten et al. showed that the amount of curative activity among Norwegian GPs decreased by 2.2 hours per week from 1998 to 2003, but this study did not report any information on total weekly hours, and the two samples were not very comparable (9). In a hearing statement in the context of a strategic plan for employment and mental health, the Norwegian Association of General Practice noted that the weekly working hours of GPs had increased by 6–7 hours to approximately 49 hours per week following the introduction of the list-patient scheme in 2001 (10), but the data on which this information is based remain unclear.
The purpose of this article is to describe the development of the total weekly working hours of GPs on the basis of data from 2000, 2002, 2004, 2006 and 2008, the proportion of that time which is spent on direct contact with patients, changes in the length of the patient lists, perceived workload, and to what extent the list-patient GPs would want a larger or a smaller workload.
Material and methods
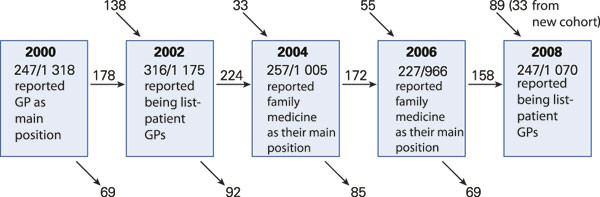
The data are taken from the reference panel of the Research Institute of the Norwegian Medical Association, a nearly representative sample of 1 600 doctors who have received a postal questionnaire bi-annually since 1994. This article draws on data from 2000, 2002, 2004, 2006 and 2008. As shown in Figure 1, there is a rather considerable attrition and renewal in the group of GPs between each round. This is because some respondents retire, withdraw from the panel or change their profession. In addition, not all panel members respond to the questionnaire in each round. In 2008, the panel was expanded by a random group of younger doctors who had received their authorizations after 2000, and of these, 33 reported that they were GPs. A total of 119 doctors, 32 women and 87 men, were GPs in 2000 and list-patient GPs in 2008, and constitute a «veterans’ group». To assess the representativeness of the sample with regard to age, gender and place of residence, as well as to estimate the response rate, we also used data from the NMA’s Internet-based statistics bank (11).
Questions concerning time use
Questions that were formulated in a fairly identical manner were used in all five survey rounds. In 2000, 2002 and 2004, we asked: «In an average working week, approximately how many hours do you spend on: Working with patients, meetings, paperwork, telephones, etc. combined?» The questions were structured so that the doctor should state the number of hours spent on each component, but also arrive at a total number of working hours by totalling them. With a view to improving precision, in 2006 the question was formulated in this manner: «During an average working week, including any secondary positions, approximately how many hours do you spend on: ...» The level of precision was further increased in 2008 by the addition of a qualifying description for each component of time used as well as an opportunity to report hours spent on updating professional skills or for other purposes. The entire question complex was presented as illustrated in Table 1.
Table 1
Questions related to the working hours of GPs in the reference panel of the Norwegian Medical Association in 2008. In an average working week, including on-call work and any secondary positions, approximately how many hours do you spend on:
| Work with patients(all direct contact with individual patients or their relatives, including telephones, e-mail, etc.) |
|__| |__| |
hours per week |
| Meetings(team meetings, journal meetings, supervisory meetings, etc. |
|__| |__| |
hours per week |
| Paperwork, telephones (journals, certificates, case histories, etc.) |
|__| |__| |
hours per week |
| Updating professional skills |
|__| |__| |
hours per week |
| Other, please specify: |
|__| |__| |
hours per week |
| Total |
|__| |__| |
hours per week |
In 2004 and 2006 the doctors were requested to report whether they were specialists in family medicine. In 2002 and 2008 we also requested those who were list-patient GPs to state how many patients they had on their lists. In 2000, 2004 and 2008 the doctors were also asked: «State how often you perceive your workload as unacceptable.» The response alternatives were «never», «rarely», «sometimes», «quite often» and «very often». Finally, in 2008 we included the following question: «If you were in a position to choose and did not need to make any financial considerations, would you work fewer hours than you do today, work approximately the same number of hours as you do today, or would you work more hours than you do today?»
Analyses
We present data from those doctors who in each of the five survey rounds reported to be a general practitioner. We use average values to describe the central tendency and for group comparisons. A correlation analysis has been made using the length of the patient list and perceived workload as variables. Testing of statistical significance was done by assessing whether the 95 per cent confidence intervals overlapped, for proportions (percentages) and for interval variables (age, list length, hours per week). Women and men have mainly been analysed separately.
Estimation of the response rate
Unfortunately, we are unable to estimate the response rate for each survey round since we have no information on how many GPs who did not respond to each round. Instead, we have compared the proportion of responding GPs of all respondents with the proportion of employed members of the General Practice Association as a percentage of all employed doctors (Table 2).
Table 2
Representativeness of the sample with regard to proportion of GPs, gender and age
| Our respondents |
All working GPs |
||||||||
| Year |
Number of GPs/number of respondents |
Proportion of GPs (95 % CI) |
Age (years), average |
Proportion of women ( %) |
Number of members in the GP Assoc./all doctors |
Proportion of members in the GP Assoc. |
Age (years), average |
Proportion of women (%) |
|
| 2000 |
247/1 318 |
18.7 (16.7 –21.0) |
46.4 |
29.6 |
3 200/ 14 359 |
22.3 |
46.1 |
28.6 |
|
| 2002 |
316/1 175 |
26.9 (24.4 –29.5) |
48.0 |
28.6 |
3 702/ 16 161¹ |
22.9¹ |
46.3¹ |
30.0¹ |
|
| 2004 |
257/1 005 |
25.6 (22.9 –28.4) |
49.4 |
28.2 |
3 777/ 16 116 |
23.4 |
46.8 |
31.5 |
|
| 2006 |
227/966 |
23.5 (20.9 –26.3) |
50.9 |
28.8 |
3 877/ 17 568 |
22.1 |
47.1 |
33.4 |
|
| 2008 |
247/1 070 |
23.1 (20.6 –25.8) |
50.1 |
31.6 |
4 322/ 18 919 |
22.8 |
47.4 |
35.5 |
|
| [i] | |||||||||
[i] ¹ Figure refers to 2003
Results
In each of the rounds from 227 to 316 respondents reported that they have their main position in general practice or work as list-patient GPs (Fig. 1). In 2004, a total of 195 of 257 (76 per cent), and in 2006 a total of 172 of 227 (76 per cent) reported that they were specialists in family medicine. In 2000 and 2008, there were 247 general practitioners in the sample, whereof 199 held this kind of position at the time of the survey.
Response rate
The proportion of GPs among the respondents was lower than the proportion of members of the General Practice Association as a percentage of all working doctors in 2000, whereas the proportion was higher in 2002. In 2004, 2006 and 2008 this difference was not statistically significant (Table 2).
Age and gender
Table 2 also shows the representativeness of the sample with regard to age and gender. Average age for the GPs who responded in 2008 was 50.1 years (95 per cent CI: 49.0 – 51.3 years), with 47.6 years (95 per cent CI: 45.5 – 49.7 years) for women and 51.3 years (95 per cent CI: 50.0 – 52.7 years) for men. The average age of all working doctors in Norway in late 2008 was 47.4 years, meaning that our sample is approximately 2.5 years older on average.
The proportion of women in the sample varied around 30 per cent, but increased to 31.6 per cent (95 per cent CI: 25.9 – 37.8) after the panel was expanded by a group of younger doctors in 2008, which is not significantly different from the proportion of women among all working general practitioners in Norway (35.5 per cent in 2008).
Place of residence
There was no statistically significant difference between the place of residence of the respondents in 2008, distributed among the five health regions, compared to the place of residence of all Norwegian GPs (data not shown).
Total working hours
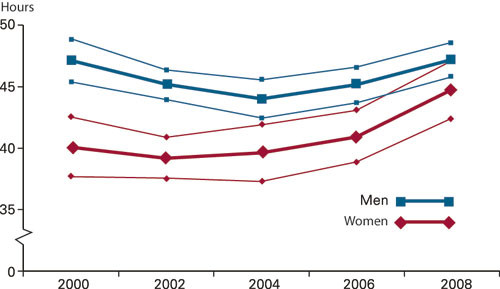
Figure 2 shows the changes in the average number of weekly working hours with a 95 per cent confidence interval over the entire period for women and men. As can be seen, women were at a significantly lower level than the men in 2000, 2002, 2004 and 2006, but not in 2008. In 2000, a total of 45 of 72 (62.5 per cent) women GPs worked 37.5 hours per week or more, and in 2008 there were 63 of 77 (81.8 per cent) (the change is not statistically significant). The equivalent figures for male GPs were 148 of 173 (85.5 per cent) in 2000 and 153 of 169 (90.5 per cent) in 2008 (the change is not statistically significant).
Working-time components
Table 3 shows all working-time components for women and men GPs in 2008. Their internal distribution was approximately identical to previous years, except that in those rounds we did not explicitly include the question of time spent on updating professional skills (data not shown). The proportion of total weekly hours spent on work with patients was very stable, varying from 70 per cent to 72 per cent, and there was no gender difference.
Table 3
Reporting of different working-time components among GPs in the reference panel of the NMA in 2008, hours per week
| No. of resp. |
Average |
Lowest |
Highest |
||
| Work with patients |
Women |
78 |
31,23 |
13 |
72 |
| Men |
169 |
32,82 |
0 |
60 |
|
| Both |
247 |
32,32 |
0 |
72 |
|
| Meetings |
Women |
78 |
3,57 |
0 |
17 |
| Men |
168 |
4,28 |
0 |
40 |
|
| Both |
246 |
4,06 |
0 |
40 |
|
| Paper work and telephones |
Women |
78 |
7,22 |
1 |
20 |
| Men |
167 |
7,14 |
0 |
30 |
|
| Both |
245 |
7,16 |
0 |
30 |
|
| Updating professional skills |
Women |
74 |
2,45 |
0 |
25 |
| Men |
162 |
2,80 |
0 |
19 |
|
| Both |
236 |
2,69 |
0 |
25 |
|
| Other |
Women |
7 |
4,43 |
0 |
15 |
| Men |
20 |
5,35 |
0 |
36 |
|
| Both |
27 |
5,11 |
0 |
36 |
|
| Total |
Women |
77 |
44,73 |
21 |
90 |
| Men |
169 |
47,17 |
14 |
77 |
|
| Both |
246 |
46,41 |
14 |
90 |
|
List length
In 2002, the average length of the patient lists (n=312) was 1 275 (95 per cent CI: 1 231 – 1 319), with 1 155 (1 079 – 1 230) for women and 1 325 (1 272 – 1 377) for men. The shortest list amounted to 150 patients, and the longest to 2 600. Equivalent figures for 2008 (n = 243) were 1 236 for all GPs, with 1 144 (1 068 – 1 219) for women and 1 278 (1 222 – 1 334) for men. The shortest list had 480 patients, the longest had 2 500. The average difference between women and men in terms of list length decreased from 170 to 134.
Workload
In 2000, a total of 38.1 per cent (94/247) of the GPs reported that they quite often or very often perceived their workload as unacceptable. In 2004, this proportion amounted to 33.3 per cent (80/240) (17 respondents did not reply to the question), while in 2008, it had been reduced to 25.5 per cent (63/247). The difference between 2000 and 2008 is statistically significant. There was no statistically significant gender difference in the perceptions of unacceptable workloads, and there was no correlation between such perceptions and the length of the patient lists (data not shown).
Desire for a change in workload
Of 245 respondents, 165 (67 per cent) reported that they had a desire to work less than they do today, whereas 79 (32 per cent) would like to have the same workload as they had. Only one woman GP wanted to work more. Two respondents did not reply to the question.
Discussion
The study shows that the total average working hours for general practitioners has increased by approximately one hour per week from 2000 to 2008, and that the women GPs account for this increase. For them, the weekly working time increased by five hours, while the working hours of their male colleagues remained approximately unchanged during this period.
It may appear that one main reason for this increase is found in the observation that many women change from working part-time (less than 37.5 hours per week) to full-time employment (37.5 hours per week or more). If so, this is concurrent with the development among the population as a whole in which women devote more time to work than previously, even though we can observe a reduction among mothers of small children (12). During the relevant period, the average age of the women veterans increased from 43 to 51 years (data not shown), which is likely to imply that the time required for care of small children is reduced, with concomitant opportunities for working longer hours and having a longer list of patients.
Doctors in general work long hours (1, 2, 6, 7). GPs are likely to work longer hours than most other groups of professions in Norway, even though a comparison must be made with some reservations. For example, in 2005 a total of 6 per cent of the population as a whole worked more than 48 hours per week (13), whereas in our sample this proportion amounted to 28 per cent in 2004 (69/250). In 2008, employed Norwegians had a contractual working week of 34.3 hours on average (14), while our 246 GPs in the same year had an average working week of 46.4 hours. In a survey of general practitioners in 11 countries undertaken in 2009, the Norwegian Knowledge Centre for the Health Services found that a group of 774 Norwegian GPs (response rate: 56 per cent) who were asked: «How many hours per week do you work as a list-patient GP?» reported an average of 40.4 hours, compared to 37.8 hours in Sweden and 48.6 hours in France (15), for example. This six-hour difference between this survey and our study may have been caused by inclusion of medical work other than just list-patient activity in the doctors‘ responses.
The strength of our study is found in its basis in repeated measurements of the same GPs in 2000, 2002, 2004, 2006 and 2008. This enables us to assess the extent to which the introduction of the list-patient scheme in 2001 has had an impact on the doctors‘ weekly working hours. However, the study also has some weaknesses. Being cohort-based, the GPs who respond at any given time will not be fully representative of all GPs. On the other hand, the differences are minor, and the disadvantages are to a large extent counterbalanced by the advantage of having access to repeated measurements. The age of the respondents also reflects the fact that the panel comprises two cohorts, one of which consists of doctors who received their authorizations prior to 2000, where most of those aged 70 or above gradually will disappear, and a second cohort of doctors who received their authorizations after 2000. Over an eight-year period some doctors will also work intermittently in functions other than that of a GP. We have also estimated the weekly working hours with the aid of general linear modelling (GLM), with repeated measurements for those who responded to all five rounds (data not shown), and found approximately the same values as those emerging from the independent measurements presented above.
Self-reported working hours may obviously deviate from the actual number of hours worked. We are unable to say whether the respondents in our sample have a tendency to overestimate or underestimate their own working hours (16), or whether there are any gender-based differences in the patterns of self-reporting. As noted above, the level of precision in the phrasing of the questions pertaining to the various components of the working hours was increased in 2006 (secondary positions are mentioned explicitly) and even further in 2008 (special reference to on-call work). We may assume, however, that most respondents have previously included these components, mainly because the phrasing of the questions has consistently focused on eliciting the total number of hours worked per week. For example, the time spent on «updating professional skills», a question which was not included until 2008, corresponds to a similar reduction in the time spent on «paperwork» in 2006 (data not shown). The relatively stable reporting of total working hours and the proportion of time spent directly working with patients indicate that the doctors on the whole have included secondary positions and on-call work in their reporting.
Certain background variables that are likely to have an effect on working hours, such as local variations in the patients? need to see a doctor (9, 17) or the doctors? need to take care of their own children (1), are not reflected in our data material.
It is conceivable that longer patient lists would result in higher workloads, but this does not appear to be the case for our women GPs, since the proportion who perceives their workloads as unacceptable decreases, while the length of the patient lists remains approximately stable. It is also conceivable that some of the doctors increase their working hours but keep the same patient list, and thereby reduce their perceived workloads. Shorter lists may allow more time for each patient as well as more time for other activities. This could possibly explain some of the reduction in the perception of unacceptable workloads in our sample. However, we believe that the key explanation must be that the list-patient scheme has provided each individual doctor with a better opportunity to manage his or her workload.
Tabell
| Main message |
|
- 1.
Abrahamsen B. Female professionals working hours in the welfare state services. Ergonomia IJE&HF 2007; 29: 193 – 7.
- 2.
Aasland OG. Konsekvenser av arbeidstid – en litteraturgjennomgang. Oslo: Legeforeningens forskningsinstitutt, 2008.
- 3.
Nylenna M, Aasland OG. Jobbtilfredshet blant norske leger. Tidsskr Nor Lægeforen 2010; 130: 1028-31. [PubMed]
- 6.
Rosta J, Gerber A. Excessive working hours and health complaints among hospital physicians: a study based on a national sample of hospital physicians in Germany. Ger Med Sci 2007; 5: Doc09.
- 9.
Grytten J, Skau I, Sørensen RJ et al. Fastlegereformen. En analyse av fastlegenes arbeidsbelastning og tjenestetilbud. Forskningsrapport 11/2003. Sandvika: Handelshøyskolen BI, 2003.
- 10.
Norsk forening for allmennmedisin. Strategiplan for arbeid og psykisk helse 2007 – 2012. Høringsuttalelse 25.5.2007. www.legeforeningen.no/id/121772.0 (26.3.2009).
- 11.
Den norske legeforening. Legestatistikk. www.legeforeningen.no/id/18 (13.8.2010).
- 12.
Kitterød RH. Han jobber, hun jobber, de jobber. Arbeidstid blant par av små barnsforeldre. Oslo: Statistics Norway, 2005.
- 13.
Aagestad C, Eiken T. Arbeidsmiljøet i Norge og EU – en sammenlikning. Oslo: Nasjonal overvåking av arbeidsmiljø og helse, 2007.
- 14.
Statistisk sentralbyrå. Statistisk årbok 2009. Tabell 209. www.ssb.no/aarbok/tab/tab-209.html (13.8.2010).
- 15.
Holmboe O, Bjertnæs ØA, Bukholm G et al. Commonwealth Fund-undersøkelsen i 2009 blant allmennleger: Resultater fra en komparativ undersøkelse i 11 land. Oslo: Nasjonalt kunnskapssenter for helsetjenesten, 2009.
- 16.
Hofoss D, Gjerberg E. Legers arbeidstid. Tidsskr Nor Lægeforen 1994; 114: 3059 – 63. [PubMed]
- 17.
Skogsholm A, Hasvold T. Er fastlegesystemet mer krevende for kvinnelige enn for mannlige leger? Tidsskr Nor Lægeforen 1999; 119: 3417 – 20. [PubMed]