Systematic screening for postnatal depression in combination with counselling sessions has been introduced in recent years at many child health centres in Norway. This is in line with national guidelines for the diagnosis and treatment of adults with depression in the primary and specialist health service (1), which recommend that: «There should be routines in place for identification of depression in pregnancy and after childbirth, and professional competence and resources to follow up on the families that are identified». However, it is not specified how this is to be done.
The Norwegian guidelines for antenatal care (2) also recommend that the health services identify pregnant women with symptoms of depression. These guidelines also say nothing explicit about how this should be done or what type of follow-up those identified should receive. The British (National Institute for Clinical Excellence, NICE) (3) and Swedish health authorities (4), on the other hand, have drawn up fairly clear guidelines on how this should be achieved.
This article provides an overview of the knowledge basis for recommendation of screening and follow-up of postnatal depression in new mothers.
Material and method
The article is based on a literature search in PubMed, PsychInfo and Cochrane from 2002 to May 2013, with the search words «postnatal/postpartum», «perinatal», «depression» and «screening» in different combinations. Only studies in English were included. The literature search returned 482 hits.
Relevant articles were selected based on the authors’ own research experience. In addition, international and national guidelines and related Norwegian reports were downloaded from the websites of the respective health authorities.
Depression and low mood associated with childbirth
Depression that affects women after childbirth is often labelled «postnatal depression» or «postpartum depression». Both of these terms indicate depression that occurs after childbirth. Postnatal depression is, however, not an independent diagnosis with its own diagnostic criteria, but represents a heterogeneous and complex group of depressive disorders.
The prevalence of depression in the postnatal period is often indicated to be somewhere between 10 % and 15 % (5). It is important to be aware that these figures are mainly based on self-reported questionnaire data, not on clinical interviews. The prevalence figures therefore do not reflect clinical depression based on diagnostic criteria, but indicate moderate to severe symptoms of depression based on a defined threshold point on a validated symptom scale.
It is, however, well documented that the period after childbirth is a risk period for women’s mental health (6). A large-scale Danish study indicates that the likelihood of needing psychiatric help is twice as high in the first three months after childbirth compared with one year later, and the risk of being affected by depression is three times as high in the first five months after childbirth compared to one year later (7). However, approximately one-third of all cases of postnatal depression arise during the pregnancy itself (8). The results of a large-scale American study of depressed mothers of infants showed that 40 % of those surveyed had become depressed in the postnatal period and 34 % during pregnancy, while 26 % had already been depressed before they became pregnant (9).
Postnatal depression must not be confused with the so-called baby blues: a temporary emotional lability that occurs in the first week after giving birth. This occurs in 50 – 80 % of all new mothers and lasts for a few days. Hormonal factors are considered to be the main reason for the baby blues (10), but lack of sleep before and during the birth can also contribute to the condition. This is so frequent that it is considered a normal occurrence.
Severe consequences
Depression in this period of life may have large ripple effects if the woman is not cared for. For the woman, it can lead to exacerbation of symptoms and a prolongation of the depression. In the most serious cases there may be a risk of suicide or infanticide (11). Approximately 20 % of all deaths in the postnatal period are due to suicide, which is therefore the second most common cause of death associated with pregnancy and childbirth (12).
When depression occurs in the period following childbirth, it can also affect the ability to care for the infant and possibly other children in the family, as well as the woman’s relationship with her partner (10). Infants are particularly vulnerable. The synaptic network in the brain is affected by the experiences that the infant has in these early years (13). It is well documented that depression in mothers is a key risk factor for both emotional and cognitive problems and difficulties with language and socialisation in children (14).
What may cause depression in the postpartum period?
Most studies indicate that psychiatric problems that occur in the period around childbirth are often problems that the woman also had previous tendencies toward (15). A birth is a key transitional period in life – great physical and emotional changes occur in a short space of time – and this makes women particularly vulnerable in this phase. Lack of sleep, problems with breastfeeding, the feeling of huge responsibility, having a child with a difficult temperament, and lack of social support are known factors that can lead to anxiety and low mood.
Despite relatively extensive research, there is currently not much support for the idea that hormonal factors help to trigger postnatal depression to any significant degree. However, approximately 5 – 10 % of all new mothers develop postpartum thyroiditis, which is often wrongly diagnosed as postnatal depression (16).
The Edinburgh Postnatal Depression Scale (EPDS)
In severe cases of depression it will often be evident that the woman needs help. In other cases it may not be so obvious, even to her close family or healthcare personnel. It is not unusual for new mothers to feel ashamed that they feel low and do not have the expected maternal feelings towards their infant. Many therefore try to conceal their problems and it can then be difficult for healthcare personnel to ascertain which women are struggling mentally after childbirth. This is what led British psychiatrist John Cox and his colleagues to develop the Edinburgh Postnatal Depression Scale (EPDS), to discover feeling of depression in women who had recently given birth (17).
Other well-tested depression scales (18) – (20) that are often used in the health services are not particularly designed with perinatal depression in mind, and are not validated in pregnant or postnatal women. What distinguishes the EPDS scale from other depression scales is that it does not survey physical symptoms such as tiredness, low energy or changes in sleep, appetite or libido. These symptoms can equally be consequences of the birth and caring for an infant. The scale consists of ten questions about how the person has been in the past seven days, and each response is ranked on a scale from 0 to 3. The total score varies from a minimum of 0 to a maximum of 30. A total score of 12 or more has proven to be an indication of clinical depression (21). It takes approximately five minutes to complete the form.
The scale has been translated into more than 60 languages and validated in a number of countries (22), including Norway (23). In the Norwegian validation study, different threshold values for EPDS scores were compared to DSM-IV criteria for «major depression» from a clinical diagnostic interview. A threshold value of 10 yielded a sensitivity of 100 % and a specificity of 87 %, which resulted in many false positives. A threshold value of 11 or more yielded a higher specificity (92 %), but also a significantly lower sensitivity (67 %) and thereby also a risk of overlooking women with depression.
A broad spectrum of interventions
The British and Swedish health authorities have recommendations for follow-up of postnatal depression. The recommendations vary according to the degree of severity, previous depressive episodes, and possible comorbidity (3, 4).
If the woman has a high depression score (EPDS score of 12 or more), a more thorough assessment should be conducted in order to reach a decision on the best treatment. According to the British guidelines, the woman’s GP must always be informed if there is suspicion of severe depression (3). Psychotherapy, drug treatment, and even hospital admission may be necessary in cases of severe depression. The latter particularly applies if the woman shows signs of lacking the ability to care for herself or the child, and if she has severe sleep disturbances, risky behaviour, or suicidal thoughts (24). In a large-scale American study 30 % of those who scored 13 or more on the Edinburgh scale had suicidal thoughts (9).
On the other hand, women with EPDS scores of 10 – 12 will not normally satisfy the formal criteria for a diagnosis of depression and should not generally be regarded as needing treatment. Nevertheless, the depressive symptoms may have a considerable effect on their level of functioning, and an EPDS score of 10 – 12 should, according to the British guidelines (3), be followed up with an interview. If the woman has had no previous episodes of anxiety or depression, help and support may consist of regular informal individual or group-based support.
For women who have a history of depression, it is recommended to commence with 4 – 6 hours of interpersonal or cognitive behavioural therapy, even if the depression is subclinical (EPDS score 10 – 12) (3). A Cochrane analysis concluded that both psychological and psychosocial interventions are effective for treating women with postnatal depression (25). If psychotherapy is indicated, according to the British guidelines this treatment should be offered within one month of the need being identified.
The Edinburgh method
Screening using the EPDS questionnaire in combination with counselling with the public health nurse constitutes the so-called Edinburgh method (21), which is now offered at many child health centres in Norway. The method entails EPDS screening of all postnatal women with a subsequent interview with the public health nurse about the woman’s mental health and, if required, an offer of a limited number of counselling sessions. According to the guidelines for use of the Edinburgh method, a woman with a total score of 12 or more should also be offered a new appointment as soon as possible for a more thorough assessment (21).
A high EPDS score on two occasions, plus an interview, a so-called two-step screening, generally provides a good picture of whether the signs of depression in the woman should result in further assessment and possible referral. This type of process will result in high specificity and thereby minimize the risk of obtaining many false positives (21).
A randomised, controlled study of almost 4 000 British women (26) supports the beneficial effect of the Edinburgh method, which has also been seen in earlier studies (27, 28). A recent report by the Norwegian Knowledge Centre for the Health Services concludes that screening combined with various follow-up measures in the postnatal period reduces the incidence of depressive symptoms from 10 % to 6 % (29).
It is important to be aware that these studies have been conducted in countries where public health nurses and GPs work together in cross-disciplinary health centres, often also with a psychologist (30). In Norway, public health nurses usually have a more independent responsibility for follow-up after the screening. However, it is not certain that this is of any significance for the beneficial effect of the Edinburgh method. The results from a Norwegian study indicate that public health nurses have both the possibility and the competence to prevent and treat mild to moderate postnatal depression (31).
Preconditions for screening
The purpose of screening is to discover illness at an early stage. The World Health Organization has defined preconditions that must be in place before starting new screening programmes (32). The health problem must have a certain level of prevalence. An effective, documented treatment for the condition must exist, and it must be possible to offer help to those who test positive for it.
The screening instrument must have good measurability, must not entail unnecessary discomfort, and recognised procedures for further diagnostics must exist. Introduction of screening also presupposes knowledge and agreement on the distribution of normal values in the population and on the cut-off point for a positive test.
Discussion
Several international studies have demonstrated a positive effect of the Edinburgh method, and a number of countries recommend screening for postnatal depression with associated low-threshold interventions. Based on the WHO guidelines there should, in general, be a basis for screening for depression among postnatal women. The condition is common and potentially harmful for the child, and early intervention is beneficial. A suitable screening instrument and effective treatment methods exist (33). Very few of the women who have completed the form have reported adverse effects (34).
However, introduction of general screening also requires an assessment of how a method works on a national level – and this includes a cost-benefit analysis of treatment versus non-treatment. At the current time no studies have been conducted on resource expenditure in Norway. We also lack user surveys of how the test is being received by Norwegian women.
Both the British and Swedish guidelines recommend screening for postnatal depression (3, 4). In Sweden, use of the EPDS scale is recommended, while in the UK «the Whooley questions» are recommended (two questions about depression, which are supplemented by one further question if the patient has answered «yes» to the first two). However, the UK National Screening Committee has had reservations regarding a routine assessment of this type (35). This is mainly due to limitations associated with cost-benefit analyses, in view of the high proportion of false positives when using screening tools of this nature.
A so-called two-step screening has been recommended in order to avoid an unnecessarily high percentage of false positives (21), but this has currently been insufficiently tested. What constitutes an acceptable percentage of false positives is a value question and a matter for discretionary judgement. Discussion is therefore required as to whether the percentage of false positives or false negatives in a screening programme is acceptable; in other words there must be agreement on the cut-off point for a positive test.
Screening of women for depression in connection with pregnancy and childbirth was recently assessed by the Norwegian National Council for Priority Setting in Health Care. The council concluded with the recommendation that screening for postnatal depression should not be introduced on a national basis at the present time (36). In view of how antenatal and maternity care are organised in Norway, it is also our assessment that several further questions should be addressed before it is possible to make a general recommendation on screening and follow-up using the Edinburgh method on a national basis. Firstly, in our opinion clarification is needed on when it is most appropriate to undertake screening (during pregnancy and/or in connection with infant health checks). Then clear guidelines need to be set regarding how screening should be conducted and by whom (public health nurse, doctor etc.).
Antenatal checks are normally undertaken by the GP in collaboration with the midwife. A user survey showed that 85 % of pregnant women primarily went to their GP for antenatal check-ups, while 69 % had also seen a midwife at a child health centre at least once for a check-up (37). Most new mothers attend an infant health check at a child health centre from the sixth week after the birth (95 – 98 %).
Recent research indicates that six weeks after the birth is an appropriate time to screen for postnatal depression (7). If screening is performed too early, that is, in the very first weeks after the birth, too many responses would reflect how the woman feels on the day of screening, but there are normal fluctuations in mental state associated with a new period of transition and adaptation (see baby blues). In light of this, there is much to be said for the six-week check-up at the child health centre being both the right time and place, but approximately one-third of women could presumably also be identified in connection with antenatal checks (8).
Child health centres, with the public health nurse and health centre doctor, have an important role in identifying physical, mental, and developmental problems in children, while the GP is responsible for the diagnosis and treatment of mothers. Based on earlier empirical evidence, women with subclinical symptoms (EPDS score 10 – 12) and with no previous mental illness will benefit from a limited number of counselling sessions with experienced child health centre personnel (26, 38).
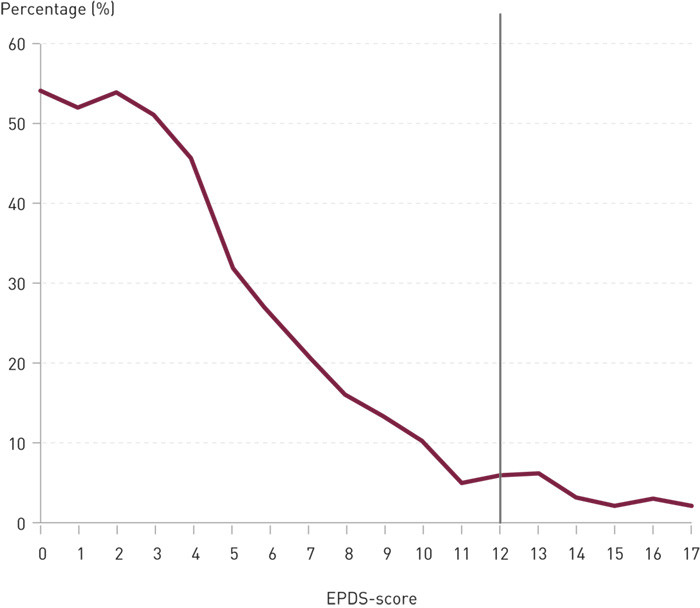
Very few new mothers with symptoms of depression are seriously ill (Fig 1) (23) in the sense that they will need treatment by a doctor, and they can therefore be helped at a lower level of care. If the problems are long-lasting or the case concerns clinical depression, the woman’s GP should be involved.
However, the report by the Norwegian Board of Health Supervision based on scrutiny of child health centre activities (39) points to large deficiencies in communication between child health centres and GPs in many parts of Norway, and that there is a widespread lack of routines in place for collaboration with GPs. Seven months after EPDS screening was introduced in the Søndre Nordstrand district of Oslo, the district GPs still had no referrals from any child health centre for follow-up of women with depression, despite the fact that the district has almost 600 births per year (unpublished data based on a questionnaire sent to GPs).
We do not know whether this can be attributed to the child health centres’ belief that they can deal with women with depressive symptoms without their GPs’ help, whether they ask the women to contact their GP themselves, or whether there are other reasons. Perhaps it is an expression of poor communication between the child health centre and the GP. The GP often has knowledge of the woman’s previous medical history and family relationships, which may be important in making a wider assessment of her state of health, and which the child health centre doctor usually lacks.
Public health nurses require training and supervision to be able to follow up with counselling sessions for mothers. This requires a quality-assured training plan and qualified supervisors with knowledge of mental health, developmental psychology, and mother-child interaction. However, there are too few specialists with this type of competence on a national basis.
Summary
Screening for postnatal depression may be an appropriate measure. However, more knowledge is required on the efficacy of alternative models for follow-up. We would recommend that a good comparative effectiveness study be conducted in Norway, possibly supplemented by economic data-gathering to enable a health economic analysis. Introduction of screening also presupposes agreement on the cut-off point for a positive test.
MAIN MESSAGE
Several international studies have demonstrated a positive effect of the Edinburgh method of screening for postnatal depression
However, introduction of screening is contingent on an assessment of how well a method works on a national basis
More knowledge is needed on the effect of various models for follow-up of postnatal depression in Norway
- 1.
Helsedirektoratet. Nasjonale retningslinjer for diagnostisering og behandling av voksne med depresjon i primær- og spesialisthelsetjenesten. IS-1561. Oslo: Helsedirektoratet, 2009. www.helsedirektoratet.no/publikasjoner/nasjonale-retningslinjer-for-diagnostisering-og-behandling-av-voksne-med-depresjon-i-primer--og-spesialisthelsetjenesten/Publikasjoner/nasjonale-retningslinjer-for-diagnostisering-og-behandling-av-voksne-med-depresjon.pdf (31.5.2013).
- 2.
Sosial- og helsedirektoratet. Retningslinjer for svangerskapsomsorgen. IS-1179. Oslo: Sosial- og helsedirektoratet, 2005. www.helsedirektoratet.no/publikasjoner/nasjonal-faglig-retningslinje-for-svangerskapsomsorgen-fullversjon/Publikasjoner/nasjonal-faglig-retningslinje-for-svangerskapsomsorgen-fullversjon.pdf (31.5.2013).
- 3.
Antenatal and postnatal mental health: clinical management and service guidance (CG 45). London: National institute for health and clinical excellence, 2007. www.nice.org.uk/nicemedia/live/11004/30433/30433.pdf (31.5.2013).
- 4.
Nationella riktlinjer för vård vid depression och ångestsyndrom 2010. Stockholm: Socialstyrelsen, 2010. www.socialstyrelsen.se/lists/artikelkatalog/attachments/17948/2010-3-4.pdf (31.5.2013).
- 5.
O'Hara MW, Swain AM. Rates and risk of postpartum depression – a meta-analysis. Int Rev Psychiatry 1996; 8: 37 – 54. [CrossRef]
- 6.
Eberhard-Gran M, Slinning K. Nedstemthet og depresjon i forbindelse med fødsel. Oslo: Folkehelseinstituttet, 2007.
- 10.
Boyce P. Personality dysfunction, marital problems and postnatal depression. I: Cox J, Holden J, red. Postnatal psychiatry. London: Gaskell, 1994.
- 13.
Rutter M, Beckett C, Castle J et al. Effects of profound early institutional deprivation: an overview of findings from a UK longitudinal study of Romanian adoptees. Eur J Dev Psychol 2007; 4: 332 – 50. [CrossRef]
- 18.
Bedford A, Foulds G. Delusions, symptoms, states. State of anxiety and depression (manual). Windsor: National Foundation for Educational Research, 1978.
- 19.
Goldberg D. The Detection of psychiatric Illness by Questionnaire. Maudsley Monograph, 21. Oxford: Oxford University Press, 1972.
- 21.
Cox J, Holden J. Postnatal Mental Health. A guide to the Edinburgh Postnatal Depression Scale. London: Gaskell, 2003.
- 24.
Boath E, Henshaw C. The treatment of postnatal depression: a comprehensive literature review. J Reprod Infant Psychol 2001; 19: 215 – 48. [CrossRef]
- 25.
Dennis CL, Dowswell T. Psychosocial and psychological interventions for preventing postpartum depression. Cochrane Database Syst Rev 2013; 2: CD001134. [PubMed]
- 29.
Kunnskapssenteret. Depresjonsscreening av gravide og barselkvinner. Nr 1 – 2013. Oslo: Kunnskapssenteret, 2013. www.kunnskapssenteret.no/Publikasjoner/Depresjonsscreening+av+gravide+og+barselkvinner.17323.cms?threepagenor=1 (31.5.2013).
- 32.
Wilson JMG, Junger G. Principles and practice of screening for disease. Genève: World Health Organization, 1968.
- 33.
Buist AE, Barnett BEW, Milgrom J et al. To screen or not to screen–that is the question in postnatal depression. Med J Aust 2002; 177 (suppl): S101 – 5. [PubMed]
- 35.
NSC. UK National Screening Committee. www.screening.nhs.uk (29.11.2013).
- 36.
Depresjonsscreening av kvinner ved svangerskap og barsel. www.kvalitetogprioritering.no/saker/depresjonsscreening-av-kvinner-ved-svangerskap-og-barsel (29.11.2013).
- 37.
TNS Gallup 2003. Tilfredshet med svangerskapsomsorgen i Norge. Rapport fra brukerundersøkelse. Oslo: Sosial- og helsedirektoratet, 2003.
- 39.
Styre for å styrke. Rapport fra tilsyn med helsestasjonsvirksomheten. Rapport fra Helsetilsynet 1/2012. www.helsetilsynet.no/upload/Publikasjoner/rapporter2012/helsetilsynetrapport1_2012.pdf (29.11.2013).