Distal radius fractures are the most frequently occurring type of fracture in Norway, accounting for about 20 % of all fractures. Incidence rates indicate more than 15 000 of these fractures each year in Norway (1, 2). The injury mechanism is normally a fall onto an outstretched hand. A displaced fracture will typically result in a wrist deformity. There will be pain with movement, and tenderness on palpation of the distal radius.
Some patients end up with a delayed operation or a malunited fracture. This is often because good reduction is accepted without considering whether the fracture may be so unstable that it will move toward the position of initial injury. The higher energy of the trauma and the older the patient, the greater the comminution of the fracture. These are the most important predictive factors for loss of reduction during the course of treatment (3) – (6). Stability is assessed at the time of the injury indirectly from anatomical criteria such as change in radial tilt, inclination and/or shortening (7). The challenge is thus to determine at the first medical consultation which fractures should be operated.
Conservative treatment, with reduction of the fracture if needed, stabilising bandaging and subsequent follow-ups to check whether the fracture reduction has been maintained, has an important place in the treatment of non-displaced and slightly displaced distal radius fractures. For displaced fractures, there has been increasing use of operative treatment in the last couple of decades. This is due to the correlation between anatomical and functional result (8) – (12) and to extensive product development. Volar locking plates have become particularly popular, despite the scarcity of documentation before these plates were used on a large scale. The increased use of surgery on assumed unstable high-energy fractures in younger age groups has influenced the treatment of elderly, cognitively unimpaired patients with displaced fractures who are now receiving surgical treatment in increasing numbers.
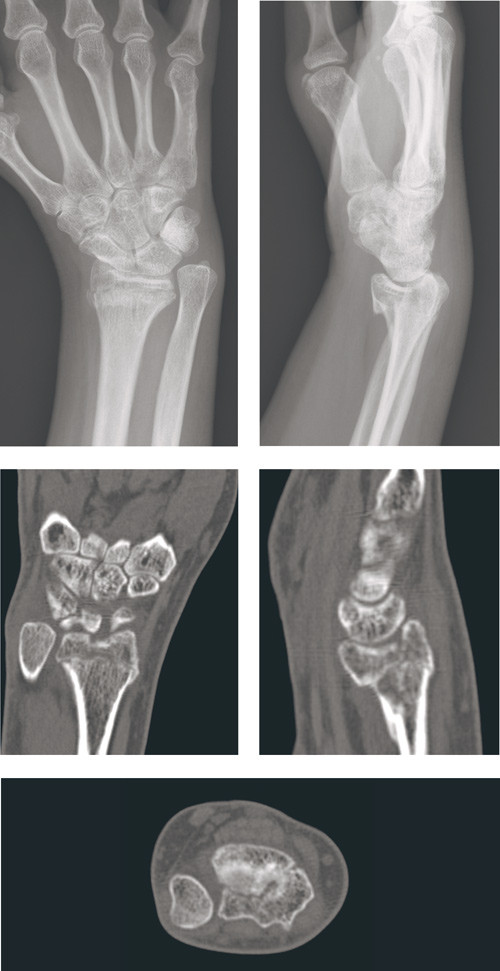
Despite growing emphasis on treatment of distal radius fractures, there is wide variation in practice. Many hospitals attempt to differentiate treatment. At other hospitals the options are more limited with respect to both which fractures are operated on and choice of treatment method. This may result in a poorer outcome for some patients than might be expected in view of the treatment options available today (Fig. 1). This situation is also illustrated by figures from the Norwegian System of Patient Injury Compensation that show distal radius fractures to be one of the most frequent causes of successful claims brought by patients (13). It is therefore important to ensure patients with such fractures optimal treatment. The purpose of this paper is to review the evidence for treatment of distal radius fractures.
Method
In 2005, the Board of the Norwegian Orthopaedic Association concluded that the high number of cases received by the Norwegian System of Compensation for Injuries to Patients where patients had lodged successful claims after treatment of distal radius fractures was noteworthy. In December of the same year, the Board therefore applied to the Norwegian Knowledge Centre for the Health Services for assistance in reviewing the evidence for treatment of these fractures, and in 2006 received a mandate from the General Assembly to appoint a consensus group consisting of doctors with a special interest in the subject. The goal was to establish guidelines for ensuring consistent, high quality treatment.
The consensus group accordingly drew up the questions requiring research:
Which patient groups benefit from surgical rather than conservative treatment?
Which types of surgery yield the best outcome?
The Knowledge Centre conducted a literature search in October 2007. Updated searches were conducted in April 2008, June 2009 and November 2009. The search terms used were forearm and wrist injuries and forearm, wrist, radius, Colles, Smith, chauffeur and/or die punch fracture. All searches were made in the databases the Cochrane Library, Cochrane Database of Systematic Reviews (CDSR), Database of Abstracts of Reviews of Effects (DARE Cochrane), the Health Technology Assessment (HTA) database, PreMedline, Medline and Embase. The inclusion criteria are shown in Table 1. Only articles in English, Finnish, German and the Scandinavian languages were included.
Table 1
Systematic reviews included. Participants in all studies were adult patients, mostly with unstable dorsally dislocated or intra-articular fractures
| First author, year of publication (reference) |
Treatments compared¹ |
Number of studies and patients |
Search |
Quality² |
| Handoll et al., 2007 (17) |
Percutaneous pinning versus conservative treatment Kapandji pinning versus transstyloid pinning |
13 randomised, controlled trials with 904 patients |
October 2007 |
High |
| Handoll et al., 2007 (18) |
External fixation versus conservative treatment |
15 randomised, controlled trials with 1 022 patients |
October 2007 |
High |
| Handoll et al., 2008 (19) |
Bridging external fixation versus conservative treatment Bridging versus non-bridging external fixation Adjuvant pinning of fracture fragment versus no pinning Dynamic versus static external fixation |
9 randomised, controlled trials with 510 patients |
November 2008 |
High |
| Handoll et al., 2008 (20) |
External fixation combined with bone graft or bone substitute versus only external fixation |
10 randomised, controlled trials with 874 patients |
November 2008 |
High |
| Cui et al, 2011 (21) |
Plates versus external fixation |
10 randomised, controlled trials with 738 patients |
December 2011 |
Moderate |
| [i] | ||||
[i] ¹ The comparisons are described in the results section of this article in the order in which they occur and are described in the cited articles
² Quality evaluation (low, moderate or high) is made in accordance with predefined criteria in the Cochrane Handbook (15)
The group evaluated 114 systematic reviews that fulfilled all the main criteria in Box 1, and on the basis of their quality decided to include only four systematic review articles (level 1 studies) of treatment of distal radius fractures. At the time of the searches performed by the Knowledge Centre, there were no systematic review articles on volar locking plates. In December 2011 the authors conducted a new search and then included a further systematic review. The present paper is thus a review of reviews, i.e. a summary of several systematic review articles (14).
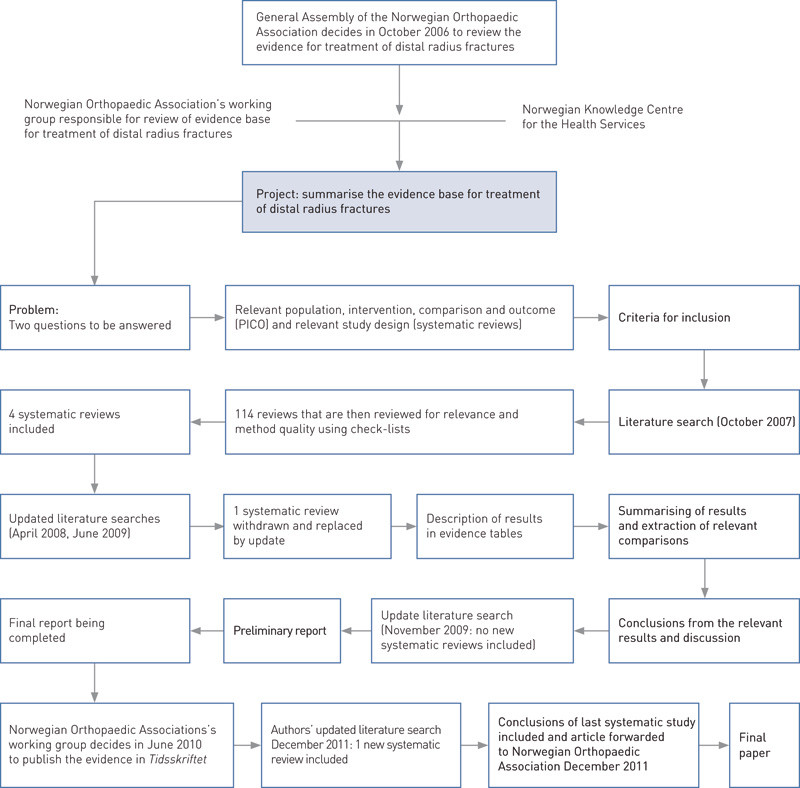
A flow chart for the work process and selection of the systematic review articles is shown in Fig. 2. The quality assessment was conducted with the aid of the Knowledge Centre's check-list for systematic review articles (14). This is an expanded version of the quality criteria for systematic review articles described in the Cochrane Handbook for Systematic Reviews of Interventions (15). The strength of the documentation for each outcome in the studies was assessed using the GRADE system (Grading of Recommendations of Assessment, Development and Evaluation) (16). According to the GRADE assessment, randomised, controlled trials are considered at the outset to be of high quality, while the results of non-randomised studies are considered to be of low quality. High quality also means that further research will not affect the strength of the outcome assessment.
Inclusion criteria for systematic reviews on the treatment of distal radius fractures. All the main criteria had to be present for a review to be included
Study design
Systematic reviews
Population
Adults (aged over 18)
All types of distal radius fracture
Interventions
Conservative treatment
Surgical treatment
Comparisons
Surgical versus conservative treatment
Between different surgical methods
Outcome
Function
Pain
Quality of life
Radiological/anatomical findings
Instability
Malunion
Complications
Arthrosis (radiocarpal, radio-ulnar)
Follow-up time
At least 12 months for malunion and radiological findings
At least 6 months for early mechanical failure
Results
Of the 115 papers that were considered, four systematic reviews were considered to be of high quality (17) – (20). One systematic review (21) included only randomised, controlled trials, but was of moderate quality because the search strategy was only partly specified. It was included nonetheless, since it was the only paper on plate osteosynthesis and volar locking plates. The studies included are shown in Table 1.
The primary studies in all reviews were small, with few exceptions. It was therefore appropriate to only describe outcomes and their strength of evidence from comparisons with 100 or more subjects or from smaller studies with statistically significant outcomes or which discussed important aspects of treatment.
Surgical treatment methods compared with conservative treatment
Percutaneous pinning compared with conservative treatment. In one Cochrane review (17), percutaneous pinning was compared with conservative treatment of unstable, mainly dorsally displaced fractures. For some of the outcomes, a pooled estimate was calculated using meta-analysis. In five of the included randomised, controlled trials, with a total of 347 patients, different functional outcomes were examined, and the result in all five was significantly better after pin fixation than after conservative treatment. The strength of evidence was moderate.
Anatomical outcomes were assessed in three small randomised, controlled trials with a total of 135 patients. There was no basis for pooling the results in meta-analyses, and significant differences between pinning and plaster casting were not shown in any of the studies – with the exception of one small study with 50 patients, where the anatomical score was better with pinning. There were also fewer complications associated with pinning. The strength of evidence for both outcomes was low. No conclusions were reached as to which patients and which fractures should be treated or which pinning method was best.
External fixation compared with conservative treatment. In one Cochrane review (18), external fixation was compared with conservative treatment of unstable, mainly dorsally displaced fractures. Ten of the randomised, controlled trials included, with a total of 651 patients, showed that external fixation maintained the reduction significantly better than conservative treatment. Six randomised, controlled trials with a total of 352 patients showed that external fixation prevents secondary displacement and malunion significantly better than plaster cast immobilisation. The estimate of effect in the meta-analysis showed low strength of evidence for both outcomes.
Patients with various functional outcomes were assessed in 13 randomised, controlled trials with a total of 730 patients. The results were not pooled in a meta-analysis, and the quality of the outcome assessment was moderate or low. These trials reported better functional scores for patients treated with external fixation, but there was a high drop-out rate in some studies, and when sensitivity analyses were applied, the results became non-significant. External fixation is associated with numerous complications, even though they are described as minor, for example pin infections. For more serious complications, such as complex regional pain syndrome, no statistically significant difference was found. No conclusion was reached as to which patients and which fractures should be treated with external fixation either.
Comparison of different types of surgical treatment methods
Comparison of different types of pinning. One Cochrane review compared different types of pinning of unstable, dorsally displaced fractures (17). The studies were small, and there was no basis for pooling the results in a meta-analysis.
One randomised, controlled trial with 12 patients compared Kapanji pinning with transstyloid fixation. There were no significant differences for any of the outcomes measured, but a tendency to a higher incidence of complications with Kapandji pinning.
Comparison of different types of external fixation. One Cochrane review compared different types of external fixation of unstable or potentially unstable fractures (19). Two of the included randomised, controlled trials compared bridging external fixation with pinning and plaster cast immobilisation. No significant differences in function or deformity were found. One randomised, controlled trial showed no statistically significant difference in complications. One randomised, controlled trial in which bridging external fixation was used showed adjuvant pinning of the fracture fragment resulted in a significantly better radiological and functional result than external fixation alone.
In three randomised, controlled trials, non-bridging was compared with bridging external fixation. In one of these studies, no statistically significant functional differences were found, while in another significantly improved grip strength, wrist flexion and radiological outcome were found for non-bridging external fixation. In the third trial, a statistically significantly superior functional and radiological result was found for a bridging external fixator compared with non-bridging. There was no difference in the complication frequency. In two of the trials there were no differences between static and dynamic external fixators. The trials were small, and too different for the results to be pooled in meta-analyses. The quality of the outcomes was therefore regarded as low.
Bone graft or bone substitute as part of surgical treatment. There is one systematic review (20) of trials that evaluate the use of bone graft or bone substitute as adjuvant treatment to for example, external fixation of distal radius fractures. The adjuvant treatment did not result in any statistically significant improvement in the result.
Plate osteosynthesis compared with external fixation. We found one systematic review (21) in which plate osteosynthesis was compared with external fixation of unstable distal radius fractures. The review included intra-articular fractures. Three of the ten included trials also considered volar locking plates. The overall result was that functional variables such as grip strength, key grip strength, pronation and supination were significantly superior in the plate group after six and twelve weeks. Later the results were relatively similar.
Meta-analysis revealed no heterogeneity between the functional outcomes of the trials. DASH scoring (Disabilities of the Arm, Shoulder and Hand), which is the most widely used, was higher in the plate group after both three months and one year, but heterogeneity was found between the studies. Significantly fewer complications were found with plating than with external fixation. There was no difference between the treatment groups if pin infections were excluded. Nor was there any difference in radiological measurements after one year.
Sensitivity analyses showed that the complication outcome was the only one with high quality. There was no evidence pointing to a choice of one treatment method or another on the basis of age group or gender. A randomised, controlled trial also revealed higher Gartland-Werley functional scores for the simple intra-articular fractures in the plate group after 24 months.
Discussion
Many papers have been published on the treatment of distal radius fractures , but the quality of the studies is variable. A general problem is that they often include very heterogeneous groups. The patients may range from 18 to 100 years of age without differentiation between younger and older patient groups. This is consistent with current practice at centres like Haukeland University Hospital and Oslo University Hospital, where more emphasis is placed on biological than on chronological age in cognitively healthy patients.
There are also many different classification systems for distal radius fractures, and the fractures are grouped somewhat differently. Several of the classification systems are not sufficiently reproducible, either (22, 23). Different measuring methods are used for outcomes in some of the comparisons. Grading systems commonly used for functional testing frequently include anatomical and clinical outcomes, and modified versions of existing grading systems are often used. According to the authors of the reviews, this meant that the results could not be pooled.
Heterogeneity reduces the strength of the outcomes and conclusions are difficult to draw. This is the reason why none of the included studies was able to provide an unambiguous answer to our question of which patient groups benefit from surgical rather than conservative treatment.
A large percentage of patients with distal radius fractures can be treated conservatively (18). This applies to those with fractures with little or no displacement. The challenge lies in deciding which fractures require surgery (3) – (7). The review does not point to any change in the anatomical limits for instability that will better capture those fractures that displace during the course of treatment than those referred to in the introduction to this paper (3) – (6).
When it comes to the question of which types of surgical treatment result in the best outcome for unstable, displaced fractures, there is some documentation. Both pinning combined with stabilising bandaging (17) and external fixation (18) give better outcomes than conservative treatment. However, there is no documentation regarding their relative efficacy. Nor are there any differences between different types of external fixation (19).
Adjuvant treatment with bone graft or bone substitute does not improve the results (20). Existing evidence indicates that plate osteosynthesis provides a better functional outcome than external fixation (21). This is supported by other literature (24, 25) A systematic review of low quality (25), which included both the old plate type and the newer, volar locking plates, found better DASH scores, supination and restoration of volar tilt in the plate group, while there was a tendency for external fixation to give better grip strength. Once studies of lower quality than randomised, controlled trials had been excluded, subgroup analyses showed that only the volar locking plates gave better results than external fixation. However, there are no studies of long-term results.
The review article of Cui et al. (21) showed fewer complications with plate osteosynthesis than with external fixation, but that the difference disappears if pin infections are disregarded. Complications have also been reported with the new, volar locking plates (24, 26). There are also fewer complications with these than with external fixation (24). The complications are partly attributable to poor surgical technique, because implants may be incorrectly placed, causing damage to tendons or cartilage. The complications may also be attributable to the method itself. For example, many distal radius fractures may be accompanied by damage to ligaments in the capus (27) and stabilising structures of distal radio-ulnar joint (28).
We have so far no overview of consequences of the short-term or lack of immobilisation used with the newer volar locking plates for these ligament injuries. In addition, cost-benefit analyses may necessitate the introduction of surgical methods that also take into account use of resources in terms of operation time, implant cost, post-operative follow-up and risk of complications. We do not yet know whether these analyses favour the new volar locking plates.
The studies tend not to differentiate between younger and older patient groups. They accordingly provide no answers as to how best to treat young patients with displaced extra- or intra-articular fractures, or how best to treat older patients with osteoporotic bones. The review of the evidence provides little new data on how much residual displacement is tolerated. Thus there is a need for good studies that show where the anatomical limits for functional impairment are, and whether there are patient groups that may tolerate a larger residual displacement than others.
Limitations of the evidence-based method
There are limitations inherent in using evidence-based practice for establishing treatment guidelines. One important factor is the time it takes before a systematic review of randomised trials is available after a new method is introduced. A systematic review will often not include the treatment methods currently in use to a sufficient degree. This also the case when it comes to treatment of distal radius fractures.
An example is the large-scale use of volar locking plates for the past ten years. When these plates were first introduced, there was no documentation of its use. Even after several years of use, there is only one systematic review article of more than moderate quality that includes this type of treatment (21). Since October 2008, the Cochrane database has contained a protocol for a review with the title Internal fixation and comparisons of different fixation methods for treating distal radial fractures in adults (29), which is very relevant to our subject. Four years later, the report has still not been completed.
The length of time before systematic reviews are available adds to the tendency for the individual surgeon to choose a method based on personal preference and experience rather than available evidence-based literature. However, it should be mentioned that evaluation of operations and the treatment of distal radius fractures has gained greater attention as a result of the focus applied by the Norwegian Orthopaedic Association. Distal radius fractures are no longer merely a task for house doctors. This is an exciting field for highly specialised orthopaedic specialists and hand surgeons. It is to be hoped that the increased attention will be reflected in the treatment results and in fewer claims for damages.
Need for further research
Despite the many papers on distal radius fractures, there is still a great need for further research. It is important initially to identify research topics and prioritise among them. It would be desirable to assess the outcomes in the various age and fracture groups. This has not been done in any of the systematic reviews included in this review.
There are a number of different classification systems for distal radius fractures. Unfortunately they are all of limited practical use when it comes to selecting the optimal treatment. We need research on criteria that predict with greater certainty which fractures will re-displace, given conservative treatment, and which should therefore receive surgical treatment. The relationship between fracture position and function is well known, but what are the limits for an acceptable position? And what follow-up should be employed to ensure healing in a satisfactory position? We continue to see a substantial number of fractures that heal in malunion that causes symptoms.
Rather than yet more small, single-centre studies that do not satisfy the requirements for high quality evidence, good prospective randomised, controlled, multi-centre trials are needed. There is also a need to establish registers and analyse register data to capture changes in the incidence of complications when new methods are introduced.
The emphasis in this article is on the treatment of distal radius fractures. It is important nonetheless to be aware of the importance of preventing these fractures. This offers considerable scope for research. Which measures work, how can resources be used most efficiently to prevent distal radius fractures, and can distal radius fractures provide an indirect measure of bone density and be a predictor of other types of fractures?
New treatment guidelines?
The evidence base for treatment of distal radius fractures was intended for use in preparing guidelines for treatment. Many questions remain unanswered, and good prospective, randomised multi-centre trials are needed to provide the best possible foundation for recommending treatments for patients.
Despite the limited documentation with respect to choice of treatment for different patient groups and fracture types, we know a good deal about treatment of distal radius fractures. We should use this knowledge as a basis for establishing treatment guidelines to reduce the variation in treatment practice and the number of claims for damages from patients.
We should like to thank the following personnel at the Knowledge Centre: researcher/project manager Katrine B. Frønsdal, researcher/project participant Bjørn Anton Graff, research manager/project manager Inger Natvik Norderhaug and research librarians Sari Ormstad and Ingrid Harboe for their assistance in our review of the evidence. Thanks are also due to Leiv M. Hove, Torstein Husby, Knut Melhuus, Adalsteinn Odinsson, Magne Røkkum, Knut Skoglund and John H. Williksen, all members of the consensus group, for their contribution to our review of the evidence.
MAIN POINTS
Pins and stabilising bandaging or external fixation yield a better outcome for treatment of unstable distal radius fractures than conservative treatment
Plate osteosynthesis yields better short-term results for unstable distal radius fractures than external fixation
Recent studies indicate that volar locking plates may be the reason for improved results in the plate group, but this must be confirmed by sound prospective randomised, controlled multi-centre trials
- 1.
Hove LM. Distal radius fractures. A study of occurrence, treatment and complications. Doktoravhandling. Bergen: Universitetet i Bergen, 1994: 1 – 160.
- 3.
Lafontaine M, Delince P, Hardy D et al. L’instabilité des fractures de l’extrémité inférieure du radius: à propos d’une série de 167 cas. Acta Orthop Belg 1989; 55: 203 – 16. [PubMed]
- 9.
McQueen M, Caspers J. Colles fracture: does the anatomical result affect the final function? J Bone Joint Surg Br 1988; 70: 649 – 51. [PubMed]
- 10.
Fernandez DL. Correction of post-traumatic wrist deformity in adults by osteotomy, bone-grafting, and internal fixation. J Bone Joint Surg Am 1982; 64: 1164 – 78. [PubMed]
- 11.
McQueen MM, Michie M, Court-Brown CM. Hand and wrist function after external fixation of unstable distal radial fractures. Clin Orthop Relat Res 1992; 285: 200 – 4. [PubMed]
- 12.
McQueen MM, Hajducka C, Court-Brown CM. Redisplaced unstable fractures of the distal radius: a prospective randomised comparison of four methods of treatment. J Bone Joint Surg Br 1996; 78: 404 – 9. [PubMed]
- 13.
Husby T, Walløe A, Willumstad Thomsen M. Behandler vi distale radiusfrakturer dårlig? Abstrakt i Vitenskapelige forhandlinger ved Kirurgisk høstmøte 2006. Oslo: Norsk kirurgisk forening, Den norske legeforening, 2006: 39.
- 14.
Kunnskapssenteret. Slik oppsummerer vi forskning. Håndbok for Nasjonalt kunnskapssenter for helsetjenesten, 2011. www.kunnskapssenteret.no/Verkt%C3%B8y/Slik+oppsummerer+vi+forskning.2139.cms (30.4.2012).
- 15.
Cochrane Handbook for Systematic Reviews of Interventions. www.cochrane-handbook.org/ (14.1.2012).
- 17.
Handoll HH, Vaghela MV, Madhok R. Percutaneous pinning for treating distal radial fractures in adults. Cochrane Database Syst Rev 2007; nr. 3: CD006080. [PubMed]
- 18.
Handoll HH, Huntley JS, Madhok R. External fixation versus conservative treatment for distal radial fractures in adults. Cochrane Database Syst Rev 2007; nr. 3: CD006194. [PubMed]
- 19.
Handoll HH, Huntley JS, Madhok R. Different methods of external fixation for treating distal radial fractures in adults. Cochrane Database Syst Rev 2008; nr. 1: CD006522. [PubMed]
- 20.
Handoll HH, Watts AC. Bone grafts and bone substitutes for treating distal radial fractures in adults. Cochrane Database Syst Rev 2008; nr. 2: CD006836. [PubMed]
- 29.
Handoll HH, Watts AC. Internal fixation and comparisons of different fixation methods for treating distal radial fractures in adults. Cochrane Database Syst Rev 2008; nr. 4: CD006951.