The SCI units at Sunnaas Hospital, Haukeland University Hospital and St Olav’s Hospital are responsible for the treatment, rehabilitation and follow-up of SCI patients in Norway. In the longer term, the patient group encounters general practitioners and doctors at local hospitals. Therapy and follow-up require multi-disciplinary collaboration. Respiratory complications associated with spinal cord injury are the most important cause of morbidity and mortality in both the acute phase and a long-term perspective (1, 2). All disciplines involved must obtain knowledge of respiratory complications to ensure pulmonary expertise in the prevention of respiratory complications.
Respiratory complications associated with spinal cord injury have a strong bearing on the length of the patient’s stay in hospital and on treatment costs. Surgery related to cervical spinal cord injury tracheotomy, mechanical ventilation and treatment of pneumonia account for 60 % of the hospital costs of treating spinal cord injuries (3).
This paper discusses respiratory complications in the acute phase, ventilator treatment and weaning, secretion mobilisation, long-term mechanical ventilation (LTMV), electrophrenic ventilation, sleep-related respiratory disorders and follow-up of patients with spinal cord injury. Terms associated with mechanical ventilation are explained in Table 1.
Table 1
Terms and explanations
| Term |
Explanation |
| Mechanical ventilation (MV) |
The patient is dependent on BiPAP or a regular ventilator |
| Bilevel positive airway pressure (BiPAP) |
Type of ventilator that is used non-invasively. BiPAP is not regarded as life-sustaining treatment, but for patients who require mechanical ventilation for limited periods during the day (mostly during the night). BiPAP systems do not usually have an internal battery, and the alarm functions are somewhat limited compared with a regular ventilator. |
| Ventilator |
Pressure and/or volume-controlled ventilator has internal battery and extended alarm functions. The ventilator is connected to the patient via a mask/mouthpiece or tracheostomy tube. The treatment can be life-sustaining. |
| Non-invasive ventilation (NIV) |
Mechanical ventilation with BiPAP or regular ventilator connected to patient via a mask/mouthpiece |
| Invasive mechanical ventilation (invasive MV) |
Mechanical ventilation with a regular ventilator connected to the patient via tracheostomy tube |
| Long-term mechanical ventilation (LTMV) |
The patient is permanently dependent on mechanical ventilation via a mask/mouthpiece or tracheostomy tube, around the clock or for limited periods during the day (mostly during the night) |
Material and method
The review article is based on a literature search in PubMed. Articles were selected on the basis of the authors’ clinical experience of treating and following up respiratory complications in patients with spinal cord injuries.
Mortality and morbidity
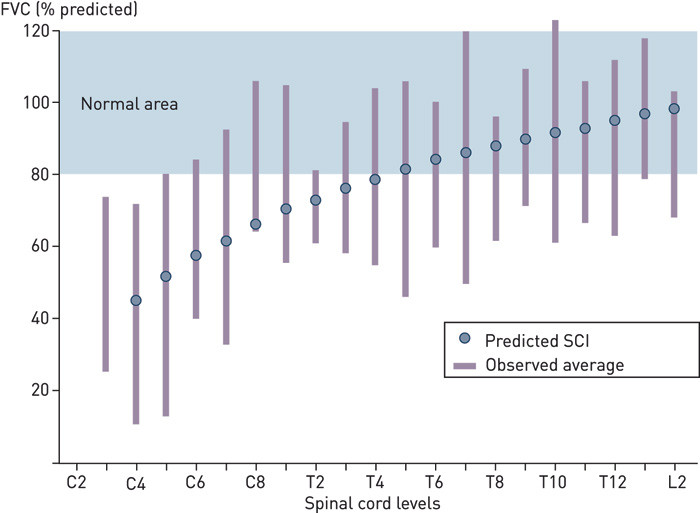
The extent of respiratory complications depends on the level of the spinal cord injury and the degree of motor impairment according to the classification of the American Spinal Injury Association (ASIA) (4). The effect on lung function is due to the paralysis of inspiratory and expiratory muscle groups with secondary respiratory failure, weakened cough strength and secretion stagnation. Lung function, measured in terms of forced vital capacity (FVC), is reduced depending on the level of the injury (Fig. 1): in patients with high tetraplegia and motor complete injury, FVC is on average 44 % of the expected capacity, and increases by 16 % in cases of incomplete injury (5). Total lung capacity and static lung volume are reduced according to the level of the cervical spinal cord injury (6). The decline in lung function over time with SCI is more rapid than might be expected for the patient’s age, irrespective of the level of the injury (7).
In the acute phase, 36 – 83 % of patients with SCI are affected by respiratory complications (2, 8) – (10); with cervical injury, 80 % of all deaths are secondary to respiratory complications (2). In a prospective study of 261 patients with acute SCI, the most frequent respiratory complications were atelectasis (36 %), pneumonia (31 %) and respiratory failure (23 %), and a total of 67 % of the patients had respiratory complications in the acute phase (11). In a 50-year follow-up study from Western Norway (12), respiratory failure and ineffectual mucous mobilisation are stressed as significant complications, and respiratory causes of death were twice as frequent as expected on the basis of the age of the whole patient group. Long-term follow-up of patients treated at Sunnaas Hospital shows that respiratory complications are the most common cause of death in the patient group (13). Survival for the first one to two years after SCI has improved over the past 30 years (14), but there is still little difference in the survival rate three years after the injury (15).
Acute therapy and surveillance
Close surveillance of respiration is important with acute SCI at all levels. With acute tetraplegia, 75 – 80 % of the patients need invasive mechanical ventilation (invasive MV). The corresponding figure for injuries at levels caudally of C4 is 60 % (16, 17). A total of 65 % of patients with injuries at levels from T1 to T12 may have severe respiratory complications (8). Oedema or haemorrhaging in the spinal cord may cause the loss of up to one ASIA level in the course of the first few days. If C4 tetraplegia is temporarily exacerbated to C3, it will have significant consequences for respiration. With C5-C6 injuries, a 30 – 50 % reduction of vital capacity is described in the course of the first week after an injury. It is therefore recommended that vital capacity and arterial blood gases be measured during the initial assessment and at regular intervals until the patient is stable (8).
Patients with tetraplegia must be assessed with respect to their need for mechanical ventilation during the acute phase. With injury levels higher than C6, intensive surveillance is required initially. Tracheotomy is recommended early on for patients who are very likely to be dependent on long-term mechanical ventilation or slow weaning (8). Non-invasive ventilation (NIV) can be used in the acute phase (18, 19), but this practice requires specialist expertise that is not available at all hospitals (17).
Secretion mobilisation
Prevention of respiratory complications must start immediately, irrespective of the level of the spinal cord injury. Secretion stagnation due to weakness of the expiratory musculature is treated with lung physiotherapy (20), postural drainage, suction, manual cough support and mechanical insufflation and exsufflation (21). Mechanical insufflation-exsufflation employs a technical respiratory method (cough-assist device) whereby air is blown into the lungs and then suctioned out, rapidly and with great force. The high expiration flow causes secretions to be forced up into the upper airways. The cough device can be applied via a face mask or a tracheostomy tube (21, 22).
In manual cough assist, a helper presses the lower portion of the ribcage on both sides or presses their hand flat against the epigastrium while the patient tries to cough. This enhances the flow of air and produces a more effective cough. Another technique is «frog-breathing» (glossopharyngeal breathing), where the patient uses gulping swallowing movements to press small volumes of air (40 – 200 ml) down into the lungs and after 6 – 9 cycles breathes out, or coughs (23). In airstacking, a ventilator or bag with mouthpiece or mask is used to «stack» a number of inspirations, preferably 3 – 6, before the patient coughs. Other factors that may reduce the risk of infection in the acute phase are elevated bed head (45°), closed suction system, weekly replacement of circuit and good oral hygiene (24).
Ventilator management in the acute phase
Ventilator settings that apply larger tidal volumes to SCI patients than to other patients are recommended (25). In the acute phase, this helps to prevent atelectasis and pneumonia, because the patient has limited possibilities for changing position and because small tidal volumes will increase the risk of atelectasis. The recommended tidal volume is about 15 ml/kg of ideal body weight (25). In the event of manifest atelectasis, the tidal volume can be temporarily increased, normally in small steps of up to 100 ml per day, right up to 20 ml/kg. This is contingent on there being no acute lung damage or acute respiratory distress syndrome (ARDS). The airway pressure must be kept to below 40 cm H₂O in order to reduce the risk of barotrauma. A high tidal volume also helps to maintain the static flexibility of the chest wall, suppress the sense of dyspnoea and improve the speech function (26).
Spinal cord injuries seldom result in equal affection of the respiratory muscles on both sides, and we recommend controlled rather than assisted mechanical ventilation. Assisted mechanical ventilation can result in less expansion of declive lung sections and increase the tendency to atelectasis in the more poorly functioning hemithorax (25). To avoid spontaneous triggering, we recommend that the patient be kept lightly hyperventilated: pH 7.45 – 7.50 and pCO₂ 4.0 – 4.5 kPa and oxygen must be adequate with pO₂ > 9 kPa.
Weaning
Respiratory musculature atrophies rapidly with inactivity, and the patient’s strength must be gradually built up again during weaning. A vital capacity of less than 15 ml/kg of ideal body weight, reduced cough power, previous pulmonary disease, smoking and age > 45 years are unfavourable factors with respect to weaning (27). The general strategy for weaning patients with SCI is to gradually increase the length of two ventilator-free intervals per day. The patient must be monitored by means of frequent arterial blood gas tests or a combination of pulsoxymetry and end-tidal capnometry. This weaning method has proved definitely better than using synchronised alternately mandatory and spontaneous ventilation (SIMV), which is a ventilator mode (25).
Weaning by means of ventilator-free intervals requires that the patient have spontaneous respiratory activity, stable respiration and circulation, no current infection or sedation, appropriate nutrition and can cooperate on the training. The patient should not be dependent on oxygen therapy with FiO₂ higher than 25 % (8, 25) Transition to non-invasive ventilation will depend on adequate swallowing function, low tendency to aspiration and effective secretion mobilisation methods. This method results in cost savings and has a number of benefits compared with invasive mechanical ventilation (18).
Respiratory muscle training in connection with SCI has not shown an improvement in expiratory muscle strength, vital capacity or residual volume. Nor has it resulted in an improved quality of life or a reduction in the number of respiratory complications.
Long-term mechanical ventilation
In Norway, intensive care doctors have traditionally employed invasive mechanical ventilation. In a number of institutions today, pulmonary specialists monitor patients with both invasive and non-invasive mechanical ventilation. Long-term mechanical ventilation subsequent to SCI is indicated where there is restrictive ventilation reduction (vital capacity 60 – 50 %) and hypoventilation (pCO₂ > 6 kPa). Hypoventilation may develop several years after the SCI (Table 2), with recurrent lower airway infections, atelectasis, poor cough function, poor sleep quality and dyspnoea. The patient then needs long-term mechanical ventilation around the clock or during parts of the day. Non-invasive mechanical ventilation has a number of advantages over invasive mechanical ventilation: better quality of life and speech function, fewer infections, and cost savings (29). BiPAP (bilevel positive airway pressure) does not make air-stacking possible, and patients must have other methods of mobilising secretion. Today’s ventilators can be programmed in both pressure- and volume-controlled mode. This is practical in non-invasive mechanical ventilation if the patient alternates between using a mask connection at night and a mouthpiece during the day, or if the patient has a tracheostomy tube with a cuffless cannula during the day and a cannula with a cuff at night.
Table 2
Significance of the injury level for acute and chronic respiratory problems. + = always, (+) = varying degree, = never
| Affected respiration muscles |
Mechanical ventilation |
Secretion stagnation |
||||||
| Injury level |
Inspiratory |
Expiratory |
Acute |
Chronic |
Acute/ chronic |
Comment |
||
| C1-C3 |
+ |
+ |
+ |
+ |
+ |
Most frequently permanent invasive mechanical ventilation |
||
| C4-C5 |
(+) |
+ |
+ |
(+) |
+ |
Most patients are weaned from the ventilator.Non-invasive ventilation is often relevant during course |
||
| C5-C6 |
+ |
(+) |
(+) |
+ |
50 % need mechanical ventilation in acute phase with ASIA-A (8).Almost 100 % are weaned.Non-invasive ventilation may be relevant in a long-term perspective. |
|||
A high spinal cord injury (C1-C3) entails invasive mechanical ventilation (Table 2). Volume-controlled mechanical ventilation has traditionally been the first choice for adult patients with a tracheotomy. It may be simpler to achieve sufficient air leakage for speech function with volume-controlled rather than pressure-controlled mechanical ventilation (30). However, other studies show improved speech function with pressure-controlled mechanical ventilation because leakage compensation results in a stronger flow of air past the vocal cords (30). In addition, pressure-controlled mechanical ventilation eliminates the challenge of compensating for the leakage associated with cuffless ventilation. The faculty of speech is of great importance for the quality of life of these patients, and depends on both cannula adjustment and ventilator settings. The diameter of the tracheal cannula must be adjusted to the desired degree of leakage. The best results are yielded by a long inspiration time with moderate air flow and the use of positive end-expiratory pressure (PEEP) that ensures sufficient air leakage past the vocal cords during expiration, providing constant vocal volume during the entire respiratory cycle (30).
A Cochrane article concludes that there are no major differences between using passive humidification (humidifier filter) and active humidification (heating elements and water vapour) in mechanical ventilation (31). However, there may be a lesser risk of pneumonia and greater risk of cannula occlusion when a humidifier filter is used compared with active humidification (31). Experience shows that passive humidification is not effective enough with a cuffless cannula. Active humidification by adding water vapour to the respirator cycle is then necessary.
The situation in Norway
The prevalence of spinal cord injuries in Hordaland and Sogn og Fjordane counties was 36.5 per 100 000 inhabitants in 2002; the proportion of men to women was 4.7 : 1 (12). In Norway, there will be 90 – 100 persons each year with traumatic SCI who need therapy and rehabilitation, and an additional 70 – 100 with non-traumatic spinal cord injuries (personal communication, Erik Sigurdsen, responsible for the Norwegian Spinal Cord Injury Registry). At the end of 2007, 23 SCI patients (16 men and 7 women) were receiving long-term mechanical ventilation in Norway (32). The number at the end of 2010 was 36 (25 men and 11 women), with an average age of 52. A total of seven patients had invasive mechanical ventilation; the remainder had non-invasive mechanical ventilation. Most of them lived in their own home or in a serviced housing unit. On the basis of the prevalence of spinal cord injuries (12), about 15 % of all patients with SCI in Norway have long-term mechanical ventilation. Lower airway infections in non-ventilated SCI patients entail a considerable risk of respiratory failure and death (13), and today’s use of long-term mechanical ventilation is probably too low. There may be many reasons for this. General practitioners, internal medicine specialists, neurologists, rehabilitation teams and pulmonary specialists often do not recognise that recurrent pneumonia and atelectasis are secondary to ventilation reduction and hypoventilation due to extrapulmonary restrictive disease; consequently their patients are not referred for pulmonary examination and follow-up. Pulmonary expertise in the field of long-term mechanical ventilation varies from hospital to hospital (32).
Electrophrenic respiration
Pacemaker implantation has long been an alternative means of treating patients with SCI at the level above C3-C5 and an intact phrenic nerve. The improved quality of life attributable to increased mobility and being non-ventilator dependent has been stressed as an advantage (33, 34). However, implantation is resource-intensive and there is considerable perioperative risk. As far as the authors are aware, pacemaker implantation has been attempted on very few patients in Norway, and with varying result.
Laparoscopic implantation of pacemaker electrodes directly into the diaphragm is a considerably simpler surgical option than pacemaker implantation to the phrenic nerve. An account of experience with the first 88 patients with up to ten years of treatment was published in 2009 (35). Internationally, over 300 patients have been treated with laparoscopic implantation of pacemaker electrodes, and the method is being tested in Norway.
Sleep-related respiratory disorders
The prevalence of sleep-related respiratory disorders is higher in SCI patients than in the general population. The prevalence of obstructive sleep apnoea syndrome (OSAS) in the adult general population is 2 – 4 % (36). A number of studies of SCI patients have shown that the syndrome occurs in 25 – 45 % of those with long-term follow-up (37) – (39). In a longitudinal study of patients with SCI above T12, the syndrome was diagnosed in 75 % (40). The cognitive effects of a disrupted sleeping pattern, with impaired attention and powers of concentration, may affect the results of therapy in the rehabilitation of SCI patients (41). The threshold for a supplementary sleep assessment by means of nocturnal polygraphy should be low. The reason for the higher prevalence of obstructive sleep apnoea syndrome in SCI patients has not been determined. Possible explanations are overweight as a result of immobilisation, supine position when sleeping, use of sedatives and spasmolytics and changes in upper airway resistance as a result of reduced lung volume (42).
Discharge and follow-up
The degree of respiratory failure in SCI patients determines the need for respiratory aids. Safety, nursing and care requirements are substantial if, after the conclusion of rehabilitation, the patient is dependent on round-the-clock invasive mechanical ventilation. Tetraplegic patients with non-invasive mechanical ventilation often also require assistance and follow-up in putting on and taking off a mask. Adapting the home, nursing home or workplace for medical aids and adaptive equipment is part of the multidisciplinary therapy plan, and good interaction is required between first- and second-line services. Checklists for documenting transfer of expertise, written treatment procedures and emergency procedures have been developed by the Norwegian Centre of Excellence in Home Mechanical Ventilation and can be downloaded from the centre’s website (43).
Training nursing personnel to care for SCI patients often entails a combination of theoretical instruction and observation in hospitals, and in some cases (larger urban municipalities) also in specially adapted municipal residential and service units. The municipality is responsible for nursing and care, but the specialist health service is responsible for training and follow-up and has the financial and service-related responsibility for respiratory aids and consumables.
Tabell
| Main points |
|
- 2.
Lemons VR, Wagner FC Jr. Respiratory complications after cervical spinal cord injury. Spine (Phila Pa 1976) 1994; 19: 2315 – 20. [PubMed]
- 6.
Anke A, Aksnes AK, Stanghelle JK et al. Lung volumes in tetraplegic patients according to cervical spinal cord injury level. Scand J Rehabil Med 1993; 25: 73 – 7. [PubMed]
- 8.
Berlly M, Shem K. Respiratory management during the first five days after spinal cord injury. J Spinal Cord Med 2007; 30: 309 – 18. [PubMed]
- 15.
Shavelle RM, DeVivo MJ, Strauss DJ et al. Long-term survival of persons ventilator dependent after spinal cord injury. J Spinal Cord Med 2006; 29: 511 – 9. [PubMed]
- 16.
Velmahos GC, Toutouzas K, Chan L et al. Intubation after cervical spinal cord injury: to be done selectively or routinely? Am Surg 2003; 69: 891 – 4. [PubMed]
- 17.
Wing PC. Early acute management in adults with spinal cord injury: a clinical practice guideline for health-care professionals. J Spinal Cord Med 2008; 31: 403 – 79. [PubMed]
- 19.
Bach JR. Prevention of respiratory complications of spinal cord injury: a challenge to «model» spinal cord injury units. J Spinal Cord Med 2006; 29: 3 – 4. [PubMed]
- 21.
Homnick DN. Mechanical insufflation-exsufflation for airway mucus clearance. Respir Care 2007; 52: 1296 – 305, discussion 1306 – 7. [PubMed]
- 24.
Dodek P, Keenan S, Cook D et al. Evidence-based clinical practice guideline for the prevention of ventilator-associated pneumonia. Ann Intern Med 2004; 141: 305 – 13. [PubMed]
- 25.
Cosortium for Spinal Cord Medicine. Respiratory management following spinal cord injury: a clinical practice guideline for health-care professionals. J Spinal Cord Med 2005; 28: 259 – 93. [PubMed]
- 27.
Berlly MH, Wilmot CB. Acute abdominal emergencies during the first four weeks after spinal cord injury. Arch Phys Med Rehabil 1984; 65: 687 – 90. [PubMed]
- 31.
Kelly M, Gillies D, Todd DA et al. Heated humidification versus heat and moisture exchangers for ventilated adults and children. Cochrane Database Syst Rev 2010; nr. 4: CD004711. [PubMed]
- 32.
Tollefsen E, Gulsvik A, Bakke P et al. Prevalens av hjemmerespiratorbehandling i Norge. Tidsskr Nor Legeforen 2009; 129: 2094-7. [PubMed]
- 37.
Ayas NT, Epstein LJ, Lieberman SL et al. Predictors of loud snoring in persons with spinal cord injury. J Spinal Cord Med 2001; 24: 30 – 4. [PubMed]
- 43.
Helse Bergen. Nasjonalt register for langtids mekanisk ventilasjon (LTMV). www.helse-bergen.no/omoss/avdelinger/heimerespiratorbehandling/Sider/Nasjonalt_register.aspx (21.7.2011).