Improved diagnostics and treatment have increased breast cancer survival (1). At the same time, new surgical methods, including breast-conserving operations and sentinel lymph node technology offer improved quality of life. Primary breast cancer treatment consists of surgery, radiotherapy, supplementary treatment with cytostatics (adjuvant therapy), endocrine therapy and treatment with monoclonal antibodies.
National guidelines for treatment of breast cancer were first published in 1981. The Norwegian Breast Cancer Group (NBCG) has gradually improved the treatment guidelines. Today breast cancer is classified by means of the TNM system, according to immunopathological criteria and genetic analysis. At the time of diagnosis, about 15 % of breast cancer tumours overexpress human epidermal growth factor receptor 2 (HER2), and are called HER2 positive. In metastatic breast cancer this percentage is higher (20 – 30 %). The HER2-positive tumours are aggressive and imply a poor prognosis (2).
In the year 2000, trastuzumab (Herceptin), a monoclonal antibody against HER2, was registered as a medicinal product in Norway. In combination with taxans and vinorelbine, trastuzumab produces high response rates in metastatic disease and increases the median survival time by about five months (2). In the case of localized disease, adjuvant trastuzumab has been shown to almost halve the risk of relapse (3, 4). The side effects profile for the majority of those treated is favourable, but some individuals develop serious heart failure (5). It is possible to minimize toxic heart failure by means of recommended regimes and regular heart check-ups.
The purpose of the article is to summarize knowledge in this field, particularly for the benefit of oncologists, cardiologists, nuclear medicine specialists and general practitioners.
Material and method
The article is based on a non-systematic review of articles found by means of a literature search. The major clinical trials have been reviewed. Norwegian and international guidelines for trastuzumab therapy have also been studied.
Anthracyclines and trastuzumab can cause heart failure
Anthracyclines in various combination therapies have been used in first-line treatment of breast cancer for more than 30 years. The dose-dependent cardiotoxic effect of anthracyclines has been known for a long time (6, 7) and is related to the ability of the substances to generate free radicals (8). The intention in introducing trastuzumab was specifically to attack the HER2 receptor-positive cancer cells. The cardiotoxic effects of trastuzumab were not known from the Phase II studies (9, 10). In 2001, a pivotal study was published on treatment of metastatic breast cancer with a combination of doxorubicin/cyclophosphamide plus trastuzumab or a placebo. The survival data in the trial were favourable for trastuzumab, with a median survival increase of 4.8 months within a two-year observation period. However, 27 % of the patients who received the combination of trastuzumab and doxorubicin/cyclophosphamide developed signs of heart failure. 16 % developed severe disabling heart failure (NYHA III-IV) (2), and fatal heart failure was reported. Heart failure as a side effect could thus be so serious in some individuals that it over-shadowed the favourable effects of trastuzumab (11). This observation led to broad-based research which has yielded information about the causes of heart failure development and how to prevent and treat this side effect.
The HER2 receptor belongs to the class of epidermal growth factor receptors which are found in most cell types to a greater or lesser extent. Cardiomyocytes are relatively abundantly equipped with HER2 receptors. When the heart is exposed to anthracyclines, signalling pathways that lead to the death of the cardiomyocytes are activated. Signalling from HER2/HER4 dimers is activated as a counter-measure, to keep the cardiomyocytes alive. This signal is blocked by trastuzumab, which may reinforce the cardiotoxic effect of anthracyclines (12).
How to prevent and treat heart failure induced by trastuzumab treatment
The aforementioned pivotal study showed that the combination doxorubicin/cyclophosphamide and trastuzumab must not be used simultaneously (2). According to the summary of product characteristics, if trastuzumab is administered first, anthracyclines should not be used until six months later, because the monoclonal antibodies have a long half-life in blood (13). However, this rule is gradually being relaxed.
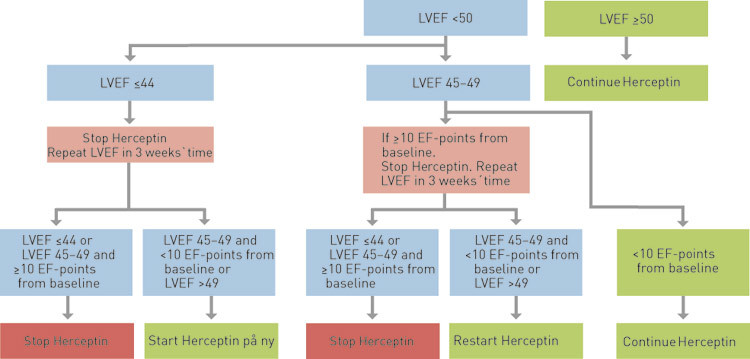
Recommendations for regular monitoring of the heart function of patients who have been given trastuzumab were developed on the basis of several large studies (14). An analogous algorithm is recommended by the Norwegian Breast Cancer Group (NBCG) (Fig. 1) (15). The check-ups include history of illness, clinical examination and echocardiography or nuclear medicine determination (GTSPECT or MUGA) of the ejection fraction. The nuclear medicine methods and echocardiography are regarded as more or less equivalent methods of examining the ejection fraction (14). Echocardiography can also provide information about other pathological conditions, for example whether the patient already has a reduced ejection fraction due to valve disease or previous infarction. In asymptomatic patients, the factor that determines whether treatment should be continued or discontinued is the ejection fraction. However, there are also descriptions in the literature of cases of clinically severe diastolic heart failure with a preserved ejection fraction (16).
Information is available on the risk of heart failure under many different treatment protocols (16). In the HERA trial, surgery was followed by at least four chemotherapy courses, including anthracyclines and then trastuzumab for 12 months. This gave a 1.9 % risk of developing symptomatic heart failure, while 5.1 % had to discontinue trastuzumab therapy because of heart problems (17). The patient in question had not suffered myocardial infarction, valve defect or cardiomyopathy before.
In practice, risk profile and risk assessment will often be different in patients with recidivist or metastatic disease. Patients with recidivism are older and have been treated with cytostatics before. It has been documented that a high age, hypertension and a high body mass index (BMI) are risk factors predisposing subjects to develop heart failure under anthracycline treatment (7). The risk of developing heart failure in connection with trastuzumab treatment is exacerbated by previous coronary disease, valve disease, diabetes or anthracycline treatment (18). Patients with metastases can have long-term treatment with trastuzumab. In one such cohort, a change in the ejection fraction was observed in 28 % of those studied. In the same study, trastuzumab treatment was temporarily stopped for 15 % of the patients, but could be resumed under close surveillance for most of them. Only 3 % of the patients had to terminate trastuzumab treatment (18).
The myocardial injury markers troponin T and troponin I show an early rise after each injection of trastuzumab in those patients who gradually develop heart failure (19). Using troponins to monitor breast cancer patients is not recommended today, however.
If the injection fraction falls to less than 44 %, trastuzumab treatment must immediately be interrupted (14, 18). Similarly, a break should be taken if the ejection fraction has fallen more than 10 %, and measurement shows 45 – 49 %. The ejection fraction of many patients will then gradually improve and heart failure symptoms will regress (14, 18, 20, 21). Long-term follow-up of the patients who developed heart failure shows that about 80 % regain their previous cardiac function (22, 23). The United Kingdom National Cancer Research Institute recommends administering betablockers and ACE inhibitors in response to signs of developing heart failure (14). There is no international consensus on this, however, unless the patients have symptoms of heart failure. Studies show that patients who are treated with betablocker or ACE inhibitor are less at risk of developing heart failure (24, 25). Prophylactic treatment is therefore assumed to be effective, but is not recommended for normotensive patients for fear of masking symptoms. It is recommended that ACE inhibitor form part of the treatment regime for hypertonics (14).
Discussion
Trastuzumab treatment of patients with HER2-positive tumours is an important advance in treatment of breast cancer which requires caution and interdisciplinary collaboration. Pre-existing cardiac disease must be identified before starting cytostatics, with a view to possibly using a different regime, and patients must be under constant surveillance. Experience shows that any previous myocardial damage, even transient, predisposes patients to develop this type of heart failure. This applies, for example, to post partum cardiomyopathy, or previously suffered viral myocarditis with a transient low ejection fraction. Cardiologists increasingly have patients who have been treated with trastuzumab referred to them for examination. The cardiologist can concentrate on measuring the ejection fraction and assessing the heart's global pump function. The algorithm for controlling the stopping and restarting of trastuzumab treatment is very intricate, however, approaching the limits of accuracy of the methods. A special challenge is therefore posed when patients are treated at two hospitals with different monitoring methods, for example MUGA and echocardiography, as the two methods yield slightly different measurement data.
Even in recommended doses, anthracyclines may have cardiotoxic effects that manifest themselves 5 – 20 years after dosage. It is not known whether trastuzumab could result in these long-term side effects, but it is possible. Some patients with metastatic disease receive trastuzumab treatment regularly for more than five years. What effect long-term treatment and a cumulative dose will have on the heart has not been established, and the challenge is increasing in pace with increased long-term use of trastuzumab.
Conclusion
The introduction of trastuzumab in standard treatment of HER2-positive breast cancer represents a major advance, both in adjuvant chemotherapy and in treatment of metastatic disease. The development of heart failure during treatment with trastuzumab is a serious complication. The phenomenon is seen in approximately 5 % of patients receiving adjuvant chemotherapy if there are no risk factors for heart failure (17, 20). The complication is more frequent in cases of metastatic disease.
It is important that predisposed patients are identified and that the patient group is monitored, with determination of the ejection fraction every three months. Monitoring may take the form of echocardiography performed by a cardiologist or by nuclear medicine examination (MUGA). If the ejection fraction falls to less than 44 %, trastuzumab treatment must be interrupted. A break should also be taken at values of 45 – 49 % if the ejection fraction has fallen more than 10 %. Conventional treatment of heart failure and ventricular dysfunction with ACE inhibitor and betablocker can be initiated in the event of symptoms or if the ejection fraction fails to improve.
We should like to thank Janne Beheim, Cand. Pharm., of Roche for literature references and useful discussions on the beneficial and side effects of trastuzumab.
Tabell
| Main points |
|
- 6.
Von Hoff DD, Layard MW, Basa P et al. Risk factors for doxorubicin-induced congestive heart failure. Ann Intern Med 1979; 91: 710 – 7. [PubMed]
- 8.
Tveteraas IH, Lundgren S, Bruserud Ø, et al. Antibiotika med cytostatisk effekt. I: Dahl O, Lehne G, Baksaas I et al, red. Medikamentell kreftbehandling Cytostatikahåndboken 7. utg. Oslo: Farmakologisk institutt, Det medisinske fakultet, Universitetet i Oslo, 2009.
- 9.
Baselga J, Tripathy D, Mendelsohn J et al. Phase II study of weekly intravenous recombinant humanized anti-p185HER2 monoclonal antibody in patients with HER2/neu-overexpressing metastatic breast cancer. J Clin Oncol 1996; 14: 737 – 44. [PubMed]
- 10.
Pegram MD, Lipton A, Hayes DF et al. Phase II study of receptor-enhanced chemosensitivity using recombinant humanized anti-p185HER2/neu monoclonal antibody plus cisplatin in patients with HER2/neu-overexpressing metastatic breast cancer refractory to chemotherapy treatment. J Clin Oncol 1998; 16: 2659 – 71. [PubMed]
- 13.
Felleskatalogen over farmasøytiske spesialpreparater. Produktomtale: Herceptin. Oslo: felleskatalogen.no, 2010.
- 15.
Norsk Bryst Cancer Gruppe (NBCG). www.nbcg.no/adjuvant_behandling/5.kontroll.av.hj.57 – 1.pd (11.10.2011).
- 23.
Russell SD, Blackwell KL, Lawrence J et al. Independent adjudication of symptomatic heart failure with the use of doxorubicin and cyclophosphamide followed by trastuzumab adjuvant therapy: a combined review of cardiac data from the National Surgical Adjuvant breast and Bowel Project B-31 and the North Central Cancer Treatment Group N9831 clinical trials. J Clin Oncol 2010; 28: 3416 – 21. [PubMed] [CrossRef]